Do you know why many vets call Addison’s disease in dogs “the great pretender”? It’s because this concerning condition can have very vague signs that look like a lot of other diseases or sometimes like nothing in particular. Integrative veterinarian Dr. Julie Buzby invites emergency veterinarian Dr. Kathryn Williams to the blog to take an in-depth look at the symptoms, risk-factors, diagnosis, treatment, and prognosis of Addison’s disease in dogs.

When people have visions of emergency cases, they may think of horrific wounds, CPR, and emergency surgical procedures. But in reality, the vast majority of my patients in the emergency room are there for vomiting and diarrhea. The list of potential causes for GI symptoms is long—pancreatitis, parasites, intestinal blockage, indigestion from eating something new, and many other things. Many times finding the cause is pretty straightforward. But, there are always cases like my patient’s that remind us vets to stay on our toes.
A Border Collie mix has a stomach ache (Or so I thought)
Annie was a 6-year-old female spayed Border Collie mix who presented for an emergency vet visit. Her parents reported that she had profuse vomiting and diarrhea overnight and seemed very lethargic. While going over her history, it quickly became evident that her parents took excellent care of her. She was up to date on vaccines, preventatives, and had no other health issues.
However, her dad sheepishly mentioned that she got a hold of a piece of bacon while they were out on a walk the day before. He had tried to get it out of her mouth but was unsuccessful.
On her exam, you could tell Annie did not feel well. She was very quiet and just wanted to lay on the ground. Her gums were tacky (sticky) and when I tented her skin, it stayed where I left it instead of snapping back into place. This meant she was severely dehydrated. Her belly was tense and uncomfortable on palpation. That wasn’t surprising given her history of vomiting and diarrhea.
At this point, I was fairly certain this was either a severely upset stomach or a more serious condition called pancreatitis in dogs that was triggered by the bacon. I often treat vomiting and diarrhea as an outpatient case. But Annie was so lethargic that I recommended we keep her in the hospital for fluids and supportive care.

I also wanted to do X-rays in case she’d managed to snag something in addition to the bacon that was causing a blockage in her intestines. Plus, I thought it would be good to run blood work to check her red blood cells, white blood cells, blood sugar, electrolytes, and the health of her organs including her liver and kidneys.
Canine addison’s disease: The great pretender is revealed
I started my patient on IV fluids at a fairly aggressive rate while I waited for the laboratory results. When I got the results, her X-rays were perfect, and her blood work was, well, boring. In fact, a little too boring for a dog who was acting so sick. Interestingly, the only abnormality at all was that the levels of one of her white blood cells, the eosinophils, were high. These cells can become elevated with allergies, parasites, and, yes, Addison’s disease!
I called the owner and recommended we do an in-hospital screening test for Addison’s disease called a baseline cortisol. Of course, her parents agreed. I did let them know that this test only helps me eliminate Addison’s disease from the list of possible causes. Reaching a definitive diagnosis requires another specialized diagnostic test.
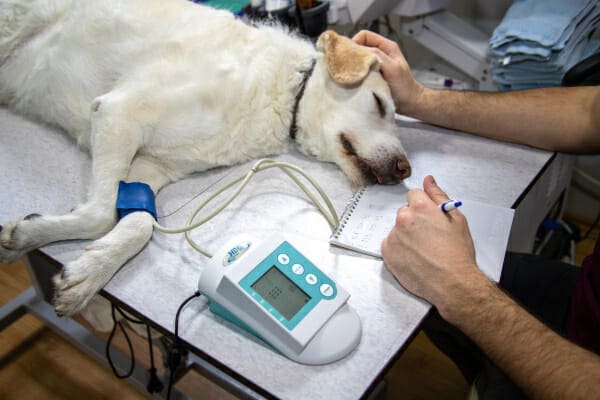
After several minutes of waiting (and me staring down the machine to encourage it to go faster), I had the result. Her baseline cortisol was extremely low. Therefore, Addison’s disease was moving higher on my mental list of culprits.
What is Addison’s disease in dogs?
As you may have gathered, patients with Addison’s disease have low cortisol levels (and often also low aldosterone levels, which we address soon). In fact, “low cortisol” is included right in the technical name for Addison’s disease which is hypoadrenocorticism. “Hypo” means low, “adreno” refers to the adrenal glands, and “corticism” refers to cortisol production.
To understand this disease a bit better, you need to first understand a bit about the adrenal glands and their function.
The paired adrenal glands, located next to the kidneys, are responsible for producing different hormones. These include glucocorticoids, such as cortisol, and mineralocorticoids, such as aldosterone.

The role of cortisol in the body
You may have heard of cortisol, the “stress hormone,” that helps your body get ready to burn fat and sugar in “fight or flight” scenarios. Like anything in the body, too much or too little cortisol is a bad thing. If the dog produces excessive cortisol, he or she has Cushing’s disease in dogs. On the other hand, dogs who produce too little cortisol have Addison’s disease.
The role of aldosterone in the body
One of the other main products of the adrenal glands, aldosterone, helps regulate important electrolytes in the body such as sodium and potassium. This hormone is equally important during times of stress because it causes the body to control electrolytes (mainly sodium) that would normally help the body retain water. This serves to stabilize blood pressure in case of injury.
As a result of their low cortisol and low aldosterone, dogs with Addison’s disease cannot physically respond to stress in an appropriate manner. This can trigger a crisis when they go through a stressful period.
Atypical Addison’s disease in dogs
Some dogs are deficient in both cortisol and aldosterone. This is the “classic” or “typical” form of Addison’s disease. However, other dogs only have low cortisol. Their aldosterone levels are still normal. In that case, we say the dog has “atypical” Addison’s disease.
What causes Addison’s disease in dogs?
Auto-immune destruction of the adrenal glands (i.e. destruction by the dog’s own immune system) is the most common cause of Addison’s disease. In rarer cases, a tumor or damage to the pituitary gland (i.e. the structure in the brain that sends the signals to the adrenal gland to stimulate them to produce cortisol) can cause Addison’s disease.
Additionally, medications that treat Cushing’s disease such as trilostane and mitotane may overcorrect the body’s excessive steroid production. This can lead to low cortisol levels. For this reason, and others, routine appointments for Cushing’s disease monitoring are so important for dogs taking those medications.
Who is at risk for Addison’s disease?
Hypoadrenocorticism is most common in young to middle-aged female dogs. In fact, over 80% of dogs diagnosed with Addison’s disease are less than 7 years old, and 70% are female.
Any breed or mixed breed of dog can develop Addison’s disease. However, it is more common in the following breeds:
- Portuguese Water Dogs
- Bearded Collies
- Standard Poodles
- Nova Scotia Duck Tolling Retrievers
- Leonbergers
- Great Danes
- Labrador Retrievers
- West Highland White Terriers
- Rottweilers
- Great Pyrenees
- Pomeranians
- Cairn Terriers
- American Cocker Spaniels

What are the symptoms of Addison’s disease?
There is a reason this disease is infamously known as “the great pretender.” Addison’s disease in dogs has notoriously vague symptoms that can look like a host of other diseases. To make things more difficult, the symptoms can wax and wane, which can make it seem as if the patient has recovered even though the disease is still present.
Signs of Addison’s disease in dogs can include:
- Anorexia (i.e. lack of appetite)
- A lethargic dog
- Weakness
- Collapse
- Shaking/trembling – including back legs trembling
- Mental depression
- Weight loss
- Poor body condition (Check out Dr. Buzby’s blog Your Dog’s Body Condition Score (BCS) to learn how to assess your dog’s body condition)
- Vomiting
- Diarrhea, sometimes with blood
- Increased thirst and urination
- Abdominal pain
- Dehydration
- Melena (i.e. digested blood in the stool)
- Weak pulses
- Prolonged capillary refill time
- Slow heart rate (To discover how to take your dog’s heart rate and other vial signs, read Dr. Buzby’s blog Keeping a “Pulse” on Your Dog’s Vital Signs)
- Low body temperature
- Shock (i.e. a state of low blood pressure where the body isn’t getting enough oxygenated blood to meet demands)
How is Addison’s disease diagnosed?
As you learned in Annie’s story, sometimes a vet will perform a basal (i.e. resting) cortisol level if he or she suspects Addison’s disease. A basal cortisol level less than or equal to 2 mcg/dL is suspicious for Addison’s disease.
The next step would be to perform an ACTH stimulation test to definitively confirm the diagnosis. (This test is further explained in an article published in the Journal of Veterinary Internal Medicine on the use of basal serum cortisol concentration as a screening test for hypoadrenocorticisim in dogs.)
For an ACTH stimulation test, first the vet will draw blood to establish the baseline level of cortisol. Then, the vet will inject a synthetic hormone, Cortrosyn, into the vein and draw a second blood sample an hour later.
The Cortrosyn mimics ACTH, the hormone produced and released by the brain to tell the adrenal glands that they need to produce more cortisol in a time of stress. In a healthy adrenal gland, the body will react accordingly and increase cortisol. Addisonian adrenal glands, however, will not respond sufficiently and cortisol levels will remain low.
It is important to run these tests prior to starting treatment, however, because the assay will read most steroids as cortisol. Dexamethasone is the only steroid that the test does not detect so your vet can safely give it prior to an ACTH stimulation test if needed.
Dogs who have the “typical” form of Addison’s disease are also deficient in aldosterone. Since aldosterone normally excretes potassium and conserves sodium, dogs who lack aldosterone will have high blood potassium and low blood sodium. This typically shows up on routine bloodwork. Thus, diagnosing this aspect of Addison’s disease does not usually require specialized testing.
What is the treatment for Addison’s disease in dogs?
For a patient like Annie, who presents in a crisis, Addison’s disease can be life threatening. The initial focus of treatment is to stabilize the patient.
Dogs with Addison’s are often in shock and have low blood pressure, making fluid therapy a critical part of treatment. This will replace the fluid lost through vomiting and diarrhea and also help bring blood pressure back to normal. Often these dogs need hospitalization and IV fluids. They cannot physically drink enough water to make up for what they lost.
Dogs who have low aldosterone also often have dangerously high levels of potassium in the blood. Sometimes fluid therapy is enough to correct electrolyte imbalances. In other cases, the dog may need additional medications such as sodium bicarbonate, insulin and dextrose (a type of sugar), or calcium to help bring the blood potassium back to normal.
Also, Addisonian dogs often need some sort of IV steroids since their cortisol is so low. There are several steroid options available. If the vet is treating presumed Addison’s based on a single baseline cortisol level, they need to remember to either run the ACTH stimulation test prior to giving steroids or to use dexamethasone, which is less likely to interfere with an ACTH simulation test.

Long-term therapy for Addison’s disease in dogs
As you can imagine, medical treatment for Addison’s disease is lifelong as the adrenal glands are unlikely to start working correctly again. Dogs will typical Addison’s will need aldosterone and cortisol supplementation.
These dogs may receive an injection of Desoxycorticosterone pivalate (also known as DOCP, Percorten, or Zycortal) every 25 to 30 days. This is a mineralocorticoid that helps regulate sodium and potassium by taking the place of the body’s normal aldosterone production.
In other cases, your vet may decide to put your dog on oral fludrocortisone instead of DOCP. This medication has mineralocorticoid activity like DOCP and also some glucocorticoid activity (i.e. ability to replace cortisol).
When treating typical Addison’s, all dogs on DOCP and approximately 50% of dogs on fludrocortisone also will need cortisol supplementation. Often, your vet will prescribe steroids such as prednisone for dogs to replace cortisol in the body. The goal is to taper these synthetic steroids to the lowest effective dose.
During times of stress such as travel or boarding, your dog may need more steroids (i.e. cortisol replacement) than during day-to-day life. Your vet can help you figure out how much you can or should increase your dog’s prednisone during those times of stress.
Dogs with atypical Addison’s have normal mineralocorticoid levels, so they only need cortisol supplementation. The same guidelines apply to them in terms of getting to the lowest effective dose of prednisone and increasing it during times of stress.
What does the future look like for dogs with Addison’s disease?
The good news is that, overall, dogs with Addison’s disease tend to do very well on the appropriate therapy. However, it can sometimes take months to get their sodium, potassium, and cortisol at the correct levels.
Dog parents need to be prepared financially and mentally for repeated trips to the vet for monitoring tests, rechecks, and DOCP injections (if that is how the vet decided to do mineralocorticoid replacement). Additionally, they need to be committed to lifelong medications such as fludrocortisone (if that was the mineralocorticoid replacement choice) and prednisone.
Parents of Addisonian dogs also should be on the lookout for return of the clinical signs of Addison’s disease. This may indicate that the mineralocorticoid and/or glucocorticoid levels are becoming too low again. It is important to stay in close contact with the vet and promptly report any changes. Dog parents should be extra aware of situations that might be stressful for their dog and follow the vet’s guidelines for increasing the prednisone dose during those times.
Despite all this, dogs with Addison’s can live a very happy and normal life. So if your dog was recently diagnosed with Addison’s, don’t lose heart. There can still be many happy days in your future!

Back to my patient who had Addison’s
You might be wondering what happened to Annie, and I am pleased to report that, like many dogs with Addison’s disease, her story has a happy ending.
Annie’s parents gave me permission to perform the ACTH Stim test to confirm that she had Addison’s disease. It would take a couple of days to get the results back from the lab. In the meantime, I went ahead and started treatment for Addison’s disease because I knew it would do more harm to wait than to move forward with treatment before an official diagnosis. My patient responded well to treatment in the hospital with fluids, steroids, and supportive care.
A couple days later, I got Annie’s ACTH stimulations results. Both her pre- and post-ACTH cortisol levels were low. Annie was definitively an Addisonian. When I called her dad, he happily reported that Annie was thriving after treatment and enjoying the remainder of her vacation. In fact, she was back to her normal self!
I braced myself to deliver the news that she had Addison’s disease and would need lifelong medication and careful monitoring. Thankfully, Annie’s parents weren’t phased by this news.
In fact, they had been reading up on Addison’s disease while they waited for the results, and proactively scheduled an appointment with their regular vet. That way they could establish a game plan for longer term management when they got home from vacation.
Annie was a lucky pup to have proactive parents who took her to the emergency room when she was sick and took her diagnosis in stride. I am honored to have been part of giving her a new leash on life!
Have you faced an Addison’s disease diagnosis with your own dog?
Please share his or her story.


Hi,
I had a 8 year old havanese girl. she was my absolute best friend and my guiding light. A month ago she passed away due to Addisons Crisis.
She never had any signs, always an energetic happy pup until the day she passed. She threw up once – took her to the vet. Labs showed her potassium/sodium levels were off. They put her on an IV drip for fluids & pain killers. I do not believe they gave her any steroids…or any other medication. Should they have? After 2 hours of being admitted at the vet, she passed away. They said she went into shock, then into cardiac arrest. It was the worst day of my life. And worst month of my life. I feel I failed her. And did the vet give her proper treatment? Was there a medication they could have give her? How come Annie lived and my sweet girl did not? Did the vet miss any steps?
Dear Lauren,
I am sorry for the tragic loss of your beloved pup. I can only imagine how much you miss her and understand your grief. It is normal to ponder all the “what ifs” but please don’t let them become a heavy burden to bear. It sounds like things progressed very quickly and I am certain the vet did everything they could to give your girl the best chance at survival. Believe me when I say your vet has probably lost many hours of sleep over your girl’s passing and has replayed every choice and action that was taken over and over in their mind as well. It is normal to want something or someone to blame when a tragedy occurs, but sometimes life is just cruel and doesn’t go the way we hoped. With time, I pray your heart can begin to heal and you can find peace. May your sweet girl’s memory stay with you always and continue to be a blessing in your life. ♥
Pet Loss Support: Groups & Resources for Comfort
Hello, my best boy, George was just diagnosed with Addison’s over the weekend and I’m devastated by the news. He’s a standard poodle, and just turned one on the third. Life doesn’t seem fair! I’m glad I took him in on the first day he was sick and didn’t go into a first crises. I took him so quickly because he was exhibiting the same signs as our other Standard after he had a bowel obstruction earlier in the year. I wasn’t taking any chances! Thankful for our vet who figured it out within a few days and even met us on the weekend on her day off to give him his first shot. I’m still processing all of this! Reading non stop, and praying that it’s just a temporary suppression of his adrenal glands that will miraculously resolve. Thanks for hearing me out. I’m sad, devastated and looking for some reassurance that it’ll all be OK. I’m also worried I’ll never be able to leave the house or take my kids on vacation again.
Hi Aly,
I understand your concern for George and am glad you were able to get a diagnosis so quickly. Try not to let worry take over. It is very possible to get this under control and well managed. How are things today? Hoping George is feeling well and has adjusted to this new treatment routine. Feel free to leave an update if you have a chance. Best wishes to you and your sweet boy.
I have an 8 year old whoodle. On her 8th birthday 12/1/23 she was diagnosed with Addisons. Just as mentioned, the disease is the “great pretender”. She was having issues for almost a full year. Her vet was treating her for arthritis & I even took her to a holistic vet who recommended water therapy. Nothing seemed to help and just before her birthday, she became very lethargic and stopped eating. She went from 50 pounds to 37 pounds. Her birthday fell on a Friday and her vet is closed on Fridays so I took her to urgent care for pets. Luckily the vet there suspected Addisons, ran tests and confirmed it. She stayed overnight and was treated with an IV, prednisone and a DOCP injection. She bounced back in about 2 weeks. She has responded really well. The only downfall, she is now 57 pounds but she acts like a puppy and we are so happy this was a treatable disease. It is expensive but our Sully is well worth it. Nice to hear all the comments.
Hi Peggy,
I can only imagine how stressful it must have been to spend a year searching for answers for your sweet girl. What a blessing the urgent care vet was able to make the diagnosis and start the necessary treatment. I am glad to hear your girl has responded so well to the medications and is back living her best life. Thank you for sharing your experience with us. Wishing you and Sully all the best and keep up the good work!
When our Bull mastiff x Bull Arab Sakura was around 6years old I noticed her not eating all her food but drinking water more than usual. I didn’t think too much of it until I noticed her back legs swaying and she took herself under a tree to probably take her resting place. I immediately thought she had a tick somewhere and took her straight to emergency. The vet took one look at her and said that he is 99% sure it’s Addison’s disease not a tick bite and put her on a drip right away. He did a blood test and kept her overnight for monitoring. He confirmed Addison’s with me and said if we had waited another few of hours she would have been dead. Fast forward to now she will be 12 on Christmas Day and has been getting around like a brand new puppy. I’ll tell you what, our crazy cute beautiful dog is a trooper, at the start of her beautiful life at just 4 weeks she was off her mum as her 14 siblings were draining their mother so much she was not doing so well. When we took her to her new home my husband who’s been around a lot of farm animals noticed very early signs of Parvovirus and took her for treatment right away at 4weeks old! meanwhile the vet did not think it was Parvovirus but treated anyway at the request of my husband. After testing Parvovirus was confirmed. The vet was shocked with the results and commended my husband for noticing it so soon. He nursed her to health and she loves him so much for it. She’s had two litters herself and got mastitis from the first litter at 2years old. Now dealing with Addison’s we give her monthly zycortal injections and cortisol tablets daily and she’s loving life. I think she doesn’t realise she’s old coz she jumps around like a newborn puppy like she’s happy to be alive.
Hi Sarah,
I am glad your girl is doing so well since starting treatment for Addison’s disease. She sounds like such an amazing pup, and it is obvious she is a big part of your lives. Thank you for sharing her story with us. This will definitely offer hope to others as they face this difficult diagnosis with their own dogs. Praying your sweet girl has many happy years ahead. Give her a hug for me and keep up the good work!
My sweet 8 yr old Cocker mix Harper had glaucoma diagnosed and her left eye removed in April.. While recovering from her surgery she suddenly quit eating and drinking. Took her to our Vet and was hospitalized for a couple days and diagnosed with Addisons Disease. Ugh! Poor thing.. We have her on monthly steroid and daily prednisone.. my concern is it’s very likely she will go blind in her right eye per her Opthamologist.. We are over 7K already between surgery/hospital/vet visits.. she has become incontinent and has had 2 UTII’s… she has her good days bad days when we will give her extra prednisone.. How do I keep her from a crisis when her other eye goes? Any suggestions?
Hi Lori,
I am sorry Harper has been through so much in the last several months. It sounds like you are already doing everything you can to ensure she remains happy and healthy. I don’t know of any other recommendations I can give to prevent a future crisis. Hoping the steroids will help keep the eye inflammation to a minimum and possibly prevent an issue with the right eye. Feel free to keep us updated on how things are going. Praying for continued success and wishing you both the best of luck.
Greetings Dr Buzby and all the fellow dog lovers.
I am writing to you becausw I feel a bit desperate since my biggest love, who’s yet to turn six, is being prepped for surgery today.
She was suspeced to have Addison’s but numbers didn’t add up because all her vital signs were excellent except of the Leucocites. After we ran out of ideas of what could it be, another vet appeared with a suggestion to mesaure cortisol and that’s when we found out for sure. But there is a catch, she doesn’t respond to any treatment and the vets have decided that our best bet is to do a surgery on her and see if there is anything else inside the body that causes obstruction, that hasn’t been seen on the Ecography (done with 4 different vets, nobody saw any anomaly).
At this time I just pray to God for the vets to find something, anything when they operate my doggie because otherwise I’m afraid that this could be the end for her.
Does anyone know if there is any chance for survival if she doesn’t respond to any treatment? Please pray for my beauty, she is way too young to die.
Dear Dejan,
My heart goes out to you as you facet this unknown situation with your beloved pup. How did the surgery go? Were they able to get some answers? Hoping your sweet girl is still with you and is making steady improvements. Praying for a miracle. ♥
My 13 yo Airedale has Secondary Addison’s. It began when she was 4 but because local vet was looking at all the wrong possibilities, no definitive diagnosis was made until she was 6. The new vet was somewhat puzzled but immediately picked up on extremely low blood sugar. commenting that it was not a disease but a symptom. Since secondary can sometimes evade ACTH test, she contacted the head of endochronology dept at Michigan State and w his imput was able to get a definitive answer. It has proven tricky to manage at times. A botched ccl sugery nearly did her in when the procedure used was old one and only for dogs 40 lb or less…she was 75 lb. add to that I brought home a dog that was in shock fm not enough dexamethazone during surgery (same day) Despite my ignorance she is still with me despite being loaded w arthritis. Sorry for long txt but I needed to share her story. Hope it saves some other pet parent fm my mistakes.
Jean and Casey
Dear Jean,
I am sorry your senior girl is dealing with this difficult diagnosis. What a blessing your vet was able to pick up on these vague symptoms and keep digging until they found an answer. I hope your girl will continue to respond favorably to treatment and wish you many happy years ahead. Bless you and your pup!
Hi All
I just wanted to tell you about my dear girl, going on 11 this april. She is a Portuguese water dog and was diagnosed at 2 years old, when she went into crisis. It took a while to work out her diagnosis but once onto a routine with meds she has done GREAT since. She is taking a 1/4 of 5mg prednisone tablet each day and point 8ml Zycortol every 30 days, which I am able to give her myself. She is bouncy and loving life and often acts like a young dog. She has bloodwork every 6 months and 2x yearly check ups now she’s a senior girl. Yes, when added up, her medical costs are high, but we wouldn’t be without her; she is sunshine in our days!
Hi Zi,
I am glad your senior girl is doing well with her treatment and is living her best life. Thank you for sharing your experience with us. It brings so much hope to others to hear a success story. You are doing a great job ensuring your sweet girl remains happy and healthy. Wishing you both the best and keep up the good work!
Hello! Your page has so much helpful information! My dog Olive, who’s 16 months old, got diagnosed right after the new year. She had severe constipation and parvo. After parvo she was still showing symptoms and so the vet tested her for Addisons and diagnosed her with it. He’s started her on hormones and a steroid. With this she seems happier. However she is still drinking excessively, urinating a lot, and not eating very much. Should this be a concern? Every time I take her to the vet she does okay. The first day I take her home she’s fine. Second day is okay until night time and something seems off. On the third day she seems worse with shaking and not eating as much as the previous days.
Hi Amanda,
I understand your concern for your pup and think it is good you are searching for advice. Unfortunately, without examining your dog myself, it is hard to make specific conclusions and recommendations. I do think you should mention this worrisome behavior to your vet. They may need to make some adjustments to her medications or treatment protocol. Hoping you can find the answers you need to ensure your girl remains happy and healthy. Wishing you all the best and feel free to leave an update if you have a chance.
My 6 1/2 month old labrador retriever was just diagnosed with addisons. Our vet had never seen a dog this young. He also had Pavo prior to us getting him. I am wondering if that had anything to do with it. I keep saying mixed things about the causes of it. He is doing a lot better so far, but still continuing to drink and urinate a lot.
Hi Katie,
I am sorry your young pup is dealing with this worrisome disease. What a blessing he was able to make a full recovery from his parvo infection. I hope he will respond favorably to treatment and wish you all the best for many happy years ahead. Bless you!
Dear Dr. Buzby:
I wanted to say Thank You for putting up and maintaining this web site. My 5-yr-old Anatolian/Akbash, Timber, is currently awaiting blood and urine test results to try to pinpoint whether his 4th episode of vomiting/diarhea/lethargy/trembling/weakness/weight loss may be Addison’s or something else which may be related to kidney function. Your informative article, as well as your responses to doggie parents, has clarified for me what additional questions I need to ask and what I may be able to expect. So, thank you!
Hi Laura,
Thank you for the kind words and positive feedback! I am glad the article was informative and offered some guidance as you navigate this difficult path. How is Timber doing? Feel free to leave an update if you have a chance. I am very curious to know how his test results turned out. Wishing you both the best!
Thank you, Dr. Buzby. Unfortunately, I received Timber’s test results Friday afternoon, and it was not Addison’s disease. Timber has end-stage renal failure brought on by poison put out by the neighbours. Prognosis is typical for kidney failure, even for a previously healthy young dog, and I’m at the point of trying to keep his last weeks comfortable.
Dear Laura,
My heart aches for you as you try to wrap your head around this difficult situation. I am so sorry this has happened to Timber. Please know you are in my thoughts, and I am praying for your strength and comfort. Bless you and your sweet boy. ♥
I came to this article after my vet called to tell me my chihuahua, Holly, had labs that showed an unusual sodium/potassium ratio that may indicate Addison’s. She’s not having any GI symptoms, although she’s always been lethargic– I’ve never known her any other way besides chill and sleepy. He doesn’t want to proceed with the ACTH test for now. When we found her (in bad conditions) she was extremely lethargic, to the extent that when I introduced her to my other dog, she fell asleep in his face. It’s hard to describe the level of exhaustion– she pretty much slept 24/7 in my lap for two weeks. But she was dehydrated, injured, and probably had nowhere safe to sleep when she was out on her own. She does seem to crave salt and will beg for a bite of pickle. I’m going to look back at her previous labs and see if they were normal.
Hi Jessica,
I agree it is odd that Holly is extremely lethargic so often. It might be worth moving forward with the testing just to have some peace of mind. I hope you can find the answers needed to help maintain her health and well-being. Thanks for sharing your experience with us!
My 9 month old golden doodle was suspected of Addisons Disease. Base Cortisol was 1.2 on initial test. Then did ACTH test. Base was .6 and after stimulation, the cortisol rose to 7.8, but not into normal range. The question remains does he have Addisons? If not, what else would cause a low cortisol level? Is there enough of a relative rise in cortisol to rule out Addisions? This all came about because of diarrhea & vomiting unexplained by anything else. This is definitely a tricky disease to nail down. We were hoping for a definitive answer so we could begin to help him, but still nothing. Very frustrating
Dear Veronica,
I understand your concern for your young pup and why you are perplexed about these results. This disease is so incredibly tough to diagnose. Without being personally involved in your dog’s medical care it is hard to make specific conclusions and recommendations. It is very possible your boy still has Addison’s, and your vet may end up initiating therapy just to see if it makes a difference. Don’t forget you can always request a consultation with an internal medicine specialist if needed. I am hopeful you will get the answers you need to ensure your sweet boy is happy and healthy. Praying for a positive outcome and a long life ahead.
Hello. My 5yo border collie was diagnosed with Addison’s disease Sept.2022. She started out on prednosone 5mg.daily. Then switched to zycortal monthly injections. She has started to have urinary incontinence. Do you think it is the zycortal use instead of prednosone? Are monthly injections enough or should she be taking prednisone also? Thank you.
Hi Cat,
I understand your concern for your pup and her ongoing battle with Addison’s disease. It is my understanding that if your dog is taking zycortal injections then prednisone is also needed for complete supplementation. There are different layers in the adrenal gland and each layer produces a different kind of steroid. The outer layer should produce mineralocorticoids (replaced with zycortal) and the middle layer is supposed to produce glucocorticoids (replaced with prednisone). It would be a good idea to discuss your concerns with your vet and ask about prednisone. Since I have not been personally involved with your dog’s medical care it is hard to make conclusions as to why certain decisions have been made. The urinary incontinence could be a side effect of the steroids, but you may want to have your vet do some investigation to make sure nothing else is contributing to the problem. I am hopeful you will find the answers you need to maintain your sweet girl’s health. She is lucky to have someone like you advocating for her well-being!
Lovely lovely stories! God bless all the puppies !, my labradoodles seems to have Addison’s disease as well. She’s on prednisone right now. We are just treating her for IBS and she seems doing well
Hi Denisse,
I am glad your pup seems to be responding to the prednisone. I hope she can remain stable and continue to live a full and happy life. Best wishes to you both!
Kona was diagnosed at 15 weeks with Addison’s thanks to my brilliant vet. We took her to ER the day before due to lethargy and no appetite. Treated for puppy gastrointestinal upset, Addison’s was not on their radar due to her age. During the early hours of the next day she started to tremble and watching her attempting to walk my husband thought it was something neurological. He is a retired firefighter. Went to our vet who ran the appropriate tests and coordinated with a local ER to get her in immediately. It was touch and go. Her potassium levels were extremely high and her sodium was frightening low. But she miraculously pulled through. She is a mini schnauzer and of course I am going back and forth with the breeder who is in denial even though the medical tests confirm it. I even had the vet run a second set.. She is almost 7 months old now and thriving. Kona plays with our other family dogs and gets into trouble like any active puppy. She receives a daily dose of pred and monthly zycortal injections. For those of you with puppies, it’s hard to catch Addison’s, especially that young, since it presents as many puppy symptoms. We weigh her every week and collaborate with our vet to adjust her pred since she is a moving target weight wise. We also collaborate before we administer her zycortal injection. As I stated previously, my husband is a retired firefighter and under the supervision of our vet showed him that we were are competent to administer the zycortal injection. It makes management so much easier. I am hopeful that she can have a long and happy life since she brings us so much joy. My vet does consult with two internists since he has never treated an Addisonian puppy so young. He does have a number of Addisonian adult dogs that he treats successfully so thumbs up!!!
Hi Carolyn,
This is such a wonderful post! Thank you for sharing your story with our readers. This is the exact thing someone else may need to see to offer them a ray of hope. I am glad Kona is doing well and living her best life. What a blessing to have such a great veterinary team working with you to ensure her health and wellbeing is maintained. I am pulling for you and sweet little Kona. Best wishes! ♥
My Rottweiler was diagnosed at 10 months. we were packing a few boxes to move on a Sunday night, some friends came by and he was normal. the next morning he would not get out of bed. my son carried him to the car and I rushed him to the vet. he walked but he was lethargic. the vet said he had a virus. I called her an hour later and said something else was wrong and she said it was a virus. I cooked him some chicken and very soon after he had diarrhea. then he started losing balance. back to the vet we went. I was very emotional and demanded they run whatever tests were necessary. a few hours later they said it was likely addisons. they started treated him for it before the test came back. it was addisons. he is almost 4 years old now. he takes percorten and 5mg of prednisone every other day. just today he urinated in his bed so we will see the vet tomorrow. treatment costs me around $240 per month.
Hi Mandy,
I am glad you were able to get a diagnosis for your young pup as this disease can be very tricky to figure out. I hope the vet visit went well and your sweet boy is feeling better today. Thank you for sharing your experience with our readers. Wishing you the best of luck!
I have an 8 y/o APBT that was initially treat for thyroid issues. He had lost 10 pounds, is lethargic, drinking and peeing a bunch, won’t eat and is trembling. A vet tech outside our office suggested Addison LS but he’s got 2 more weeks off the prednisone and the thyroid meds before he can be tested. This dog is my rock but I’m already $650 in the hole to be told they have no idea what’s really wrong. I know the Addison test is expensive as are the treatment. Short of selling my car, I’m not sure how to cover all of this. Praying for a miracle here
Dear Gloria,
My heart goes out to you with this difficult situation with your senior pup. I understand what a financial strain this can be especially when it takes lots of testing to narrow down the cause for a complicated case. Make sure your vet is aware of your concerns, so they can help tailor the diagnostic process to best fit your needs and give your sweet boy the best outcome. Praying for answers to come quickly and a complete recovery for your dog.
Welcome to my jungle we spend over $7,000 after the diagnosis two weeks in the hospital and after 6 years of treatment now his sick again pee a lot can’t sleep at night is very hard for everyone but we think put him to sleep, because his suffering now and we are also
Dear Norisa,
I am so sorry you are having to say goodbye to your pup. I hope his passing will be peaceful and it will bring you both freedom from daily struggles. Praying for your strength and comfort. Bless you.
My white shepherd was diagnosed with addison. Could this be the cause of my happy go lucky shepherd suddenly at 9 months or so, suddenly start excessively barking at everything?
Hi Chantel,
I am sorry your Shepherd is living with Addison’s disease. While it can cause many different symptoms, excessive barking isn’t one of them. This sounds like typical behavior for some hyper young Shepherds. It might be a good idea to consult a veterinary behaviorist and see if there is training you can do to decrease the frequency of this unwanted behavior.
My 6 year old beagle, Tasha, was diagnosed in April 2021. She’d lost her fur sister Jessie in October 2020 from a brain tumor, so she’d been pretty lonely without her. I was out of state when she went down hill. My husband said she was almost limp when he picked her up to rush her to the vet. She had a low body temperature, low heart rate and blood pressure, shivers, didn’t want to eat or drink anything, and lethargic. They started the tests right away and diagnosed her with Addison’s a few days later. They said she’d probably had this for awhile (maybe all her life) and since Jessie (who was like a second fur mother to her) passed and I was gone it was finally triggered. She’d suffered from seizures starting in November 2018, but they only happened every other year. Now though it seems like she has them every other month. We’ve increased her steroid and pushed back her injections from 25 days to 28 days to try and stop the seizures, but they still can’t pinpoint why she still has seizures and why they’re increasing in frequency. It’s been a struggle this past year and a half, and I love her to pieces, but the expense takes a toll on my young family, especially after we tried everything to save her sister just a few months earlier which we hadn’t quite recovered financially from when Tasha was hospitalized. We’ve got a great veterinarian team that helps us as best they can though. They’ve taught me how to give Tasha her shots so we can cut down the expense since we can now afford the $215 bottle of her injection meds. They’ve really been great to us and I couldn’t ask for a better group of veterinarians to take care of our pets.
Hi Alex,
Thank you for sharing your story with our readers. Your experience may be just what someone else needs to hear to help them in a similar situation. I am sorry Tasha is struggling with seizures on top of Addison’s disease. It does sound like she is in good hands with your veterinary team and that you have a great partnership. Please make sure your vets and staff know how pleased you are with them, and they care they have given your dogs. It literally means the world to us to know we are making a difference in the lives of our clients and patients. I applaud you as well. You seem like one of the unicorn clients we all hope to have. Praying Tasha’s seizures can be controlled, and she stays well-regulated with her Addison’s. Best wishes to you both!
Unfortunately we lost Tasha on March 27th, 2023. We went in for her yearly on the 17th of March and the veterinarian technician noticed her white gums. Tests indicated low red blood cells, no infections, no tumors that were visual with x-rays. We were told it was either bone cancer or her immune system was attacking her bone marrow. Our vet prescribed her heavy doses of steroids, antibiotics, and immunosuppressive meds. We did a drop off, to keep the price low, every couple of days or so to check her red blood cell count, but they just kept dropping. On the 27th, we were told her levels had still not even stopped dropping, so they needed to do a blood transfusion. We couldn’t afford the $900+ (which didn’t include the transfusion). I’d even called a local pet er hospital but was told it would be between $3000-$4000. There would be no guarantee she would pull through whatever was going on with her or if she would relapse. We made the difficult decision to put her down that day. She was loved on by all the staff, who fed her some of a peanut butter and jelly sandwich and I’m sure lots of other treats while we made our way there. Having to say goodbye was the hardest, I still have guilt that we couldn’t do more for her, and I miss her everyday, even her loud baying when I’d come home from work. She was only 8.
Dear Alex,
I am so sorry for your loss of Tasha. While this new issue was completely unexpected, what a blessing the veterinary team caught it during her annual visit. I know saying goodbye was difficult, but I would have made the same choice for one of my own. Your loving decision gave Tasha peace and freedom from her struggles. May her memory live on and be a source of joy in your lives. Bless you. ♥
What if my blind and diabetic dog has addisons? Test results yesterday indicate elevated potassium levels and low eltrolights. we will test friday for addisons. i just lost my other senior dog 3 weeks ago, tux a havanese, and now my presley has this to confront. as do i.
i told vet his rear legs have been weak and she attributed it to age. plus he just lost his hearing.
again age she said. if it’s not addisons, she said we would have to start testing for something else. what else?
Hi Deborah,
I am sorry you are dealing with such a difficult situation with your senior pup. My heart aches for you and your recent loss of Tux. Honestly, there are so many possibilities of diseases to test for I am not sure what your vet will want to start with. Since I haven’t personally examined Presley, it is hard to make specific recommendations. With complicated cases like this, it might be a good idea to schedule a consult with a veterinary internal medicine specialist. They have lots of experience with cases like Presley and may have access to testing and treatments that are not readily available in general practice. I hope you are able to find some answers and help give your sweet boy the best quality of life possible. Best wishes to you both and feel free to leave an update as your journey continues.
Happened to our Maltese at 11 years old. For 11 years old she is full of energy , I’ll sprint down the street with her, take her to dog parks and she’s all over the place . Over a period of about a week started to notice a shift in her energy as she would walk a bit slower on our normal routine. She wouldn’t jump up onto the couch as well, she would look for someone to pick her up (was initially thinking she was acting spoiled lol). Started to notice her dish was still looking full after a day as well . Tried offering her the wet food which she normally chows down and she didn’t want anything to do with it . Knew then something was wrong for sure, but she otherwise had no symptoms of discomfort . Took her into the vet and her blood glucose was low and she had lost 2 lbs which for a 9 lb dog is very significant. They kept her for the day administering dextrose and fluids to stabilize her, ran the tests and she showed signs of low cortisol levels as well. Doctor diagnosed atypical Addisons . Just started prednisone therapy . She’s not back to her full energetic self yet , but doing a lot better . Appetite isn’t completely normal but she’ll eat chicken, prime rib ect (the good stuff) . Hope to see her back to her normal energetic jumping around self , with the prednisone treatment though I know she’s getting older so as long as she’s happy .
Hi Simone,
I am glad you were able to see the subtle changes with your senior girl and get her to the vet quickly. It sounds like she is on the right path and will hopefully be feeling better soon. Thank you for sharing your experience with our readers as it may help someone in a similar situation. I hope your sweet girl can stabilize on the prednisone and get back to living her best life. Best wishes to you both for many happy days ahead!
Recent diagnosis in 7yo male mix. In crisis and hospitalized until stable. Currently on Fludrocortisone 0.1 bid and prednisolone .33 bid (last dose tomorrow). He is better but still pretty tired, is very particular about food choice and has watery diarrhea. He see’s regular vet tomorrow. I was hopeful to see a bit more improvement as we are 8 days into treatment. Curious to see if Fludro is all they they recommend or if they’ll have him take Prednisilone too? My impression was just the one pill but may also depend on where his lab values are. Rough road and hate to see them feeling so badly.
Hi Lisa,
My heart goes out to you during this difficult time. Praying your boy can continue to fight and that he will stabilize and come home soon. You are correct that some dogs do just fine with only the fludrocortisone. There is about a 50% chance that they will need to supplement with the prednisone as well and these changes are made based on changing lab values over time. Wishing you and your sweet guy the best as you navigate this tough road ahead.
Molly is our 14 years and one month old female Labradoodle. Much of this article was so familiar to my wife and I as Molly was diagnosed with Addisons when she was just over a year old. She has lived a long, happy, active life and while a bit less flexible and a few steps slower than she once was, Molly is still going strong at 14. When Molly was diagnosed her doctors were quick to point out how important weight control was
to dogs with these conditions as the medications are based upon weight. Fortunately for Molly, my wife and I walk several miles daily. Between the walks and multiple other daily bouts of activity including her favorite, swimming, Molly’s weight rarely fluctuates more than 1/2 pound per month. Her doctors feel exercise and weight maintenance have led to her long life. To any facing an Addison’s diagnosis for their best friend or even themselves as humans can be Addisonian as well, Molly’s advice would be to stay active, and count calories.
Hi Butch,
Thanks so much for sharing Molly’s story and those wise words of advice! I am so glad that she has done well and has stayed active. Great job to you guys for taking such good care of her as well!
Our dog Roxie had a full-blown Addisonian crisis when she was around 6 years old. She vomited a little, but was uncharacteristically lethargic and weak. And she had episodes of trembling and quaking. And weirdest of all, during the night, we found her resting on the cold tile of the bathroom floor, rather than on our bed. What dog does that when it is not even hot out? Since she seemed to be interested in her walks, we thought whatever she had was maybe getting better. After some discussion, we did take her to our vet who ran some blood work, and we took her home. When the vet called us with the results, rather than have us call in to the recorded message, we knew something serious was happening. She told us to take Roxie to the ER right away, and that she had called ahead to tell them we were coming. It was a lot for us to process, since Roxie didn’t seem to us to be in an emergency situation. We knew the price tag would be astronomical, and we asked if we could wait and see for a day. The vet said that if we waited, Roxie might die of cardiac arrest. Well, yes, we went to the ER. Addison’s was confirmed, they kept her for 3 days to stabilize and hydrate. They gave her sub-Q hydration, so it looked like she has a sack of water under her skin that drooped and flopped around when she walked, which was super strange. We give her the monthly shot at home and the daily pred pill. Fast forward, she is now 12, has had a happy dog life, and facing the typical issues of being a healthy senior dog.
Hi Sharon,
Thanks so much for sharing Roxie’s story with us. I’m so glad that you got her to the vet and then to the ER hospital when you did. It is wonderful to hear that she is doing so well now!
Glad to see she is doing well. How much does your dog weigh? What was the monthly cost of injections? Prednisone?
thank you for this good information. my first standard poodle had this; diaganosed full blown addison mid life. but she lived 13 beautiful years.
my second standard poodle has a-typical. just on prednisone but healthy at almost 12 years old. my other 2 standard poodles do not have the disease. It is a disease that is scary but these babies can live a long, normal life with it if diaganosed early. this is important info for veterinarians as well as pet parents.
thank you
Hi Judy,
It is fantastic that your two Addisonian poodles have done well and had wonderful long lives after the diagnosis! Thanks for sharing their stories with us.