A diagnosis of IMHA in dogs can be scary and overwhelming, but integrative veterinarian Dr. Julie Buzby is here to help. She explains the condition, symptoms, diagnosis, treatment, and prognosis so you know what to expect every step of the way.

I knew something major was going on when I had three back-to-back-to-back missed calls from my friend Carolyn on a Sunday evening. She was one of my best friends in college. We live on opposite sides of the country now but we can still pick things up quickly even if we haven’t talked for a few months. Carolyn also happens to be a very dedicated dog parent with a penchant for Cocker Spaniels. When I saw the missed calls, my mind jumped to worst case scenarios. I immediately thought of her sweet Izzie, an 11-year-old Cocker who takes the cake for having the softest ears in the world.
Something is wrong with Izzie
I called Carolyn back and immediately knew from the tremor in her voice that something was, in fact, very wrong. It was clear she was holding back tears. She apologized for bothering me but said she was hoping I could help her understand what was going on with her Izzie girl. She explained that Izzie was currently hospitalized at the local specialty clinic. The vets there had diagnosed her with immune-mediated hemolytic anemia (IMHA) and were giving her a blood transfusion.
Carolyn said Izzie had been more tired than normal for the last week. But Carolyn thought it was just because they had been going on extra walks and enjoying the fall weather. The morning of her call, Izzie ate only half of her breakfast. Then that afternoon she collapsed when Carolyn took her out for her normal walk. Carolyn rushed her to the local emergency and specialty clinic, which is where she first heard the words “IMHA in dogs.”
Carolyn is one smart cookie, but she doesn’t have a medical background. So I understood how a diagnosis of IMHA could be very overwhelming. With this in mind, I set out to help her understand what to expect for sweet Izzie.
- Something is wrong with Izzie
- What is IMHA in dogs?
- How common is IMHA in dogs?
- What are the symptoms of IMHA in dogs?
- Back to Izzie
- How is IMHA diagnosed?
- What causes IMHA in dogs?
- What is the treatment for IMHA in dogs?
- What is the prognosis for dogs with IMHA?
- Izzie's happy ending
- You are not alone
- Have you ever had a dog with IMHA?
What is IMHA in dogs?
When I am explaining immune-mediated hemolytic anemia in dogs, or IMHA for short, I like to start by tackling this diagnosis one word at a time. Let’s start with “anemia.” This means a low red blood cell count. “Hemolytic” refers to a specific type of anemia where something is actively destroying the red blood cells. In this case, that something is the immune system, which is where the “Immune-mediated” portion of the name comes from.

Normally, the immune system is supposed to attack invaders like viruses and bacteria. In the case of IMHA, something causes the immune system to malfunction. As a result, it attacks the body’s own red blood cells instead. This attack can either happen in the blood vessels (i.e. intravascular hemolysis) or in the liver and spleen (i.e. extravascular hemolysis).
How common is IMHA in dogs?
IMHA is one of the most common autoimmune diseases in dogs. Good data on the true incidence of this disease is lacking, but one older paper estimated that up to 1 in 500 dogs might develop this condition. Any breed of dog can get IMHA. But it tends to be more common in the following breeds:
- Cocker Spaniels
- Poodles
- Springer Spaniels
- Old English Sheepdogs
- Irish Setters
- Collies
What are the symptoms of IMHA in dogs?
Understanding a bit about IMHA and red blood cell function can help predict the clinical signs. Red blood cells carry oxygen throughout the body and deliver that oxygen to the organs. When there are not enough red blood cells, the organs do not get enough oxygen. This lack of oxygen causes many of the symptoms of IMHA such as weakness and seeming very tired (i.e. a lethargic dog). It can even lead to fainting or collapsing, as it did for Izzie.
The over-active immune system and generalized inflammation that go along with IMHA cause some of the other symptoms such as a fever, decreased, appetite, or vomiting. Finally, affected dogs may have a yellow tinge to the skin, mucous membranes, or whites of the eyes (i.e. icterus or jaundice) or dark brown urine. Dog parents may be more likely to associate jaundice with liver disease in dogs. However, it also happens when bilirubin builds up in the body due to red blood cell destruction.
A more comprehensive list of some of the signs of IMHA includes:
- Weakness
- Lethargy
- Collapse
- Rapid or labored breathing (anemia is one of the many reasons for a dog breathing fast)
- Decreased appetite
- Vomiting
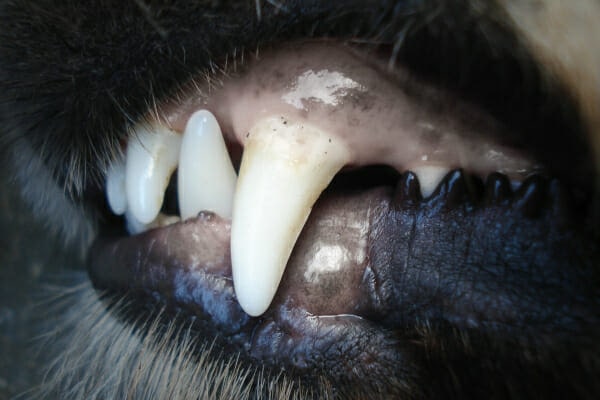
- Pale or white gums or tongue
- Yellow skin, eyes, and/or gums
- Dark brown, red, or orange urine
- Eating or licking abnormal material like dirt, bricks, or rocks i.e. pica
- Fever
Back to Izzie
When Carolyn and Izzie arrived for the emergency vet visit, Izzie was rushed right in for evaluation. The ER veterinarian called Carolyn and explained that based on her examination alone she was suspicious of IMHA. However, they needed to do more testing to be sure.
The vet shared a few of her exam findings that made her lean toward this diagnosis. She noticed that Izzie’s heart rate and respiratory rate were both faster than they should be. Her pulses felt “snappy” and her gums were pale with a slight yellow tinge instead of a normal pink color. These signs can all be an indicator of significant anemia.
They were already running a rapid blood test to measure Izzie’s red blood cell count, known as a PCV or packed cell volume. This test reports the percentage of the blood that is made up of just red blood cells.
The ER veterinarian reported these results to Carolyn while she was on the phone. For a dog, the normal range for this test is between 35% and 55%. Izzie’s PCV was dangerously low at 16%.
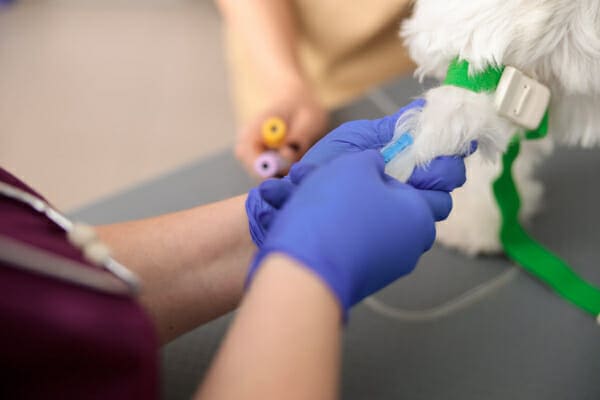
The veterinarian explained that Izzie urgently needed a blood transfusion to stabilize her. While the transfusion was running, they would also work to pinpoint the cause of her anemia and develop a more specific treatment plan. This would involve a few more diagnostic tests. Carolyn listened carefully and tearfully agreed to the plan.
How is IMHA diagnosed?
In addition to a PCV, a dog with suspected IMHA may also need a complete blood count (CBC) and a chemistry panel. A CBC measures the three main cell lines made by the bone marrow—red blood cells which carry oxygen, white blood cells that help with immune function, and platelets that help clot the blood. With IMHA, the typical result would be a low red blood cell count, an elevated white blood cell count, and a normal platelet count.
A chemistry panel looks at protein levels and can help assess some basic organ functions. The most frequent chemistry panel abnormality in a dog with IMHA is an elevated bilirubin level. This is because bilirubin builds up in the bloodstream when the red blood cells are destroyed. A urinalysis may also show increased bilirubin in many dogs with IMHA.
My personal favorite way to help diagnose IMHA is a test to look for autoagglutination. This test has a long name, but is easy to perform without any special equipment. It involves placing a drop of blood on a glass slide and mixing it gently with several drops of saline. In a normal dog everything will mix smoothly and uniformly. However, in many dogs with IMHA, the blood will clump together obviously, and the mixture will be speckled or blotchy.
This happens because antibodies (i.e. immune system molecules) on the surface of the red blood cells stick the cells together in a process called autoagglutination. The resulting clumps of red cells are big enough to see with the naked eye. A normal dog does not have these antibodies, which is why the red cells won’t clump together.
Further testing
This first round of blood tests often lead to a presumptive diagnosis of IMHA. The next round of testing is focused on confirming this diagnosis and ruling out some of those conditions that can trigger IMHA (more on that soon). Your veterinarian will likely want to confirm that the anemia is regenerative (i.e. that the body is trying to replenish the red blood cells).
This involves checking for the number of baby red blood cells, called reticulocytes, in circulation. The bone marrow should respond to anemia by ramping up production of new red blood cells and pushing more reticulocytes out into circulation. As a result, dogs with IMHA should have an increased number of reticulocytes if the bone marrow is doing its job.
Your veterinarian may also want to perform a blood smear. For this test, the veterinarian or veterinary pathologist spreads a thin layer of blood out on a slide and examines it under the microscope. With IMHA, the veterinarian or pathologist would expect to see increased numbers of cells called spherocytes. They are smaller and darker red blood cells that are left behind after the immune system attacks red blood cells and takes a “bite” out of them.
Occasionally, the vet will also recommend a Coomb’s test to check for antibodies on the surface of red blood cells. Since these antibodies are not normally present on red blood cells, a positive result fits with a diagnosis of IMHA.
What causes IMHA in dogs?
Part of the diagnostic process also involves trying to figure out what caused the IMHA in the first place. Typically, IMHA is either primary or secondary. Primary IMHA has no discernible underlying cause. Secondary IMHA occurs when another problem triggers the immune system to inappropriately attack the red blood cells.
Secondary IMHA
The three most common causes of secondary IMHA are:
1. Certain medications and vaccines
Some antibiotics, while well tolerated the vast majority of the time, are known to be potential triggers for IMHA. The most classic examples are sulfa drugs, cephalosporins, and penicillins. Vaccines are also a potential trigger. But this is a much more challenging definitive link to make. I think it is very important to note that for most patients, the benefit of routine vaccination greatly outweighs the risk of developing a condition like IMHA.
To learn more about the science behind vaccination selection, check out my blog Which Dog Vaccines Are Absolutely Necessary?

2. Infectious diseases
Almost any infectious disease process can activate the immune system and cause it to malfunction, resulting in an autoimmune disease like IMHA. Some infectious agents spread by fleas and ticks tend to trigger IMHA most commonly. They include:
- Ehrlichia
- Babesia
- Anaplasma
- Bartonella
- Mycoplasma
3. Cancer
The two most common cancers that are thought to trigger IMHA are lymphoma in dogs and hemangiosarcoma in dogs.
Additional tests to screen for causes of secondary IMHA
As you can see, there are a variety of conditions that the vet needs to look for in order to get to the bottom of why your dog has IMHA. One important step is testing for tick-borne diseases in dogs. Usually, IMHA triggered by a tick-borne infection is the best-case scenario. In these dogs, the IMHA usually responds very well to treatment and is unlikely to recur once the underlying infection is taken care of.
Your veterinarian may also discuss chest X-rays and an abdominal ultrasound to look for any evidence of the types of cancer that can sometimes trigger secondary IMHA. He or she will also carefully review your dog’s medical history for any recent medications or vaccinations that could be linked to IMHA.
Primary IMHA
Primary IMHA is what we in veterinary medicine call a “diagnosis of exclusion.” This means the vet must first rule out all the potential triggers listed above. Once he or she does that, what remains is a diagnosis of primary IMHA. Essentially, this means that for no good reason at all, the immune system has started attacking and destroying the red cells.
What is the treatment for IMHA in dogs?
Like Izzie, some dogs with suspected IMHA will require treatment to get them stabilized while the vet is running the diagnostic tests. Then once the vet confirms an IMHA diagnosis, he or she will discuss the treatment plan moving forward. Typically, stabilization and treatment involve:
Immunosuppressive medications
Vets commonly use steroid medications like dexamethasone (injectable) and prednisone for dogs (oral) to suppress the immune system in immune-mediated hemolytic anemia cases. Steroids are inexpensive, easy to obtain and administer, and work very well. It is no wonder that they are a part of the veterinarian’s toolkit for almost all dogs with IMHA. Unfortunately, steroids can also have a lot of side effects. Since IMHA is a life-threatening disease, these side effects tend to be worth the expected benefit.

Some of the steroid side effects dog parents should know about include:
- Increased thirst and urination
- Increased panting
- Agitation
- Lethargy or listlessness
- Weight gain for small to medium-sized dogs
- Weight loss and significant loss of muscle mass for medium to larger breed dogs
- Increased appetite
- Increased risk of other infections (skin infections, UTIs in dogs, etc.)
- Thinning of the skin
- A thin or dull haircoat
- Insulin resistance, which may increase the chances of diabetes mellitus or cause issues in an already diabetic dog
- Iatrogenic Cushing’s disease in dogs
Higher doses and longer courses of steroids cause more significant side effects. If your dog’s case of IMHA seems very severe, or if your veterinarian is worried about more significant side effects from steroids alone, they may decide to add a second medication to suppress the immune system.
The three most common secondary immunosuppressive medications are Atopica® (cyclosporine), mycophenolate, and azathioprine. Each of these medications has a specific set of pros and cons that will be unique to your furry family member. Your veterinarian can determine which one is best for your dog’s situation.
Blood transfusions
Most patients with IMHA will need at least one blood transfusion to help keep them stable while the medications to suppress the immune system kick in. It can take five to seven days, and sometimes longer, for immunosuppressive medications to halt the immune system’s inappropriate destruction of the red cells. In the meantime, the body will continue to rapidly break down the red blood cells.
Blood transfusions during this period of time are a temporary solution to bring the red blood cell count back up to a safe level. Many dogs need more than one blood transfusion. How fast the immune system destroys the red cells that each transfusion provides will dictate how many transfusions a dog needs.

Plasmapheresis
If a dog does not respond to these more typical first-line treatments, there are still other options to consider. Plasmapheresis is a treatment that has recently shown promise for dogs with IMHA. It removes the fluid portion of the blood, called plasma, which is what contains the immune components that are inappropriately attacking the red cells. Then it replaces the “bad” plasma with a transfusion of “good” plasma from a healthy donor dog. This treatment is related to dialysis treatment and only a limited number of specialty and university hospitals can perform it.
If you are interested in learning more, a 2021 study in the Journal of Veterinary Internal Medicine evaluated membrane-based therapeutic plasma exchange as a treatment option for immune-mediated hematologic disorders in dogs.
IVIG infusions
As another option, the vet can administer a human immune product, IVIG, to your dog over several hours. IVIG works by temporarily clogging up the receptors on the immune cells so they cannot bind to and destroy the red blood cells. Both plasmapheresis and IVIG are expensive treatments. As such, they may be cost-prohibitive for many dog parents.
Anticoagulant or antiplatelet medication
The overactive immune system in dogs with IMHA causes an increased risk of developing dangerous blood clots. Sadly, blood clots to locations like the lungs or the brain are one of the most common reasons a dog with IMHA may not survive. Most dogs with IMHA will take either an anticoagulant or antiplatelet medication.
The goal is to try to decrease the chances of developing a life-threatening blood clot. The vet may use injectable medications like heparin in the ICU setting. But at discharge, he or she will typically prescribe an oral medications like Plavix® (clopidogrel), aspirin, or Xarelto® (rivaroxaban).
Doxycycline
The antibiotic doxycycline is effective against most tick-borne infections that can trigger IMHA. Your vet may choose to start your dog on doxycycline for several reasons including:
- Confirmed tick-borne disease.
- To treat for possible tick-borne disease if you and your veterinarian decided not to pursue tick testing.
- As a way to cover the bases while the results of tick-borne disease tests are pending.

Additional medications and therapies
Some dogs with IMHA can be managed at home from the start. Others are very sick and require hospitalization. If your dog with IMHA is hospitalized, the vet will probably put him or her on IV fluids. Lots of dogs with uncontrolled IMHA also have a decreased appetite or signs of nausea. If this is the case for your dog, your veterinarian may prescribe anti-nausea medications like Cerenia® (maropitant) or ondansetron.
What is the prognosis for dogs with IMHA?
Let’s go back to Izzy’s story for a look at prognosis. Carolyn had not been able to remember everything that the emergency veterinarian had told her about IMHA. But one phrase had lodged itself painfully in her memory—potentially fatal. I had to break the news to Carolyn that the emergency veterinarian was correct.
The prognosis for IMHA is guarded, especially in the first 10 to 14 days after diagnosis. Older papers list the mortality rate for IMHA at about 50%. However, with improved treatment options, the survival rate these days is likely better.
Some dogs succumb to dangerous blood clots. For others, the reason for a poor outcome is more complicated. Around-the-clock ICU care and multiple blood transfusions are expensive. In some cases, dog parents reach a very difficult point where they cannot continue treatment due to financial constraints.
The good news is that once a sick dog with IMHA is stable enough to be discharged from the hospital the overall prognosis is much better.
What to expect long-term
Once a dog has a stable red blood cell count and can take oral medications, he or she can come home from the hospital. At this point, most dogs are on a high dose of prednisone, doxycycline, an antiplatelet medication like clopidogrel, and possibly a secondary immunosuppressive medication.
The vet will keep your dog on the higher dose of steroids until the red blood cell count is normal for about three weeks. At that point, he or she will start to taper the steroid dose very slowly. This process often lasts between four to six months and requires careful monitoring of the red blood cell count as the dose of steroid decreases.
It is possible to eventually wean many dogs with IMHA off their medications entirely. However, relapses can occur so it is important to keep a close eye on your dog. Studies indicate a relapse rate of between 12% and 20%. If a dog relapses, the vet may treat him or her with another tapering course of immunosuppressive medications.
In some cases, dogs may need to remain on immunosuppressive medications for the rest of their lives to keep their IMHA in remission. In these dogs, the goal is to have them on the lowest possible dose of medication to limit the side effects they experience while still controlling their disease.
All dogs with IMHA will need careful follow-up, close monitoring, and repeat bloodwork following their diagnosis. It is important to stay in close contact with the vet and report any changes in your dog to him or her promptly. You see your dog every day and know him or her well. That makes you the perfect person to notice when things are a bit “off” with your pup.

Izzie’s happy ending
Now that you know all about IMHA, you are probably wondering what happened with Carolyn and sweet Izzie. I am happy to report that Izzie was discharged from the hospital after getting two blood transfusions. She is peeing up a storm from her steroids. But otherwise she is starting to return to her normal Izzie self. She still has a long road ahead of her, but she has a wonderful dog mom, a top-notch primary care veterinarian, and a very knowledgeable internal medicine specialist who are all dedicated to helping her beat this disease. And she also has me, cheering her and Carolyn on from afar.
You are not alone
If like Carolyn, your dear dog was recently diagnosed with IMHA, don’t be afraid to lean on your support system. After Carolyn hung up with the ER vet, she realized that her worry and fear had kept her from processing a lot of what the veterinarian had said. This is when she picked up the phone to call me, her longtime friend who also happened to be a longtime veterinarian. You may not happen to have an old friend who is a vet, but you do have lots of other people in your corner. Use them.
Write down a list of questions and call the vet back once you have gotten a chance to process some of what he or she said. Or reach out to a friend who had a similar experience with his or her dog. Find some blogs or support groups online. I know that an IMHA diagnosis can be scary and the outlook may be uncertain at first, but you don’t need to tackle it alone. There are plenty of people ready to help and support you and your beloved dog.
Have you ever had a dog with IMHA?
Please share his or her story.


Our dog Mia has IMHA. She has had four blood transfusions and is on prednisone and is now on her third immunosuppressant. She still has not regenerating new blood cells. Our internist called our last immunosuppressant attempt a Hail Mary. We’ve been doing research and we are finding out that that is not true. We just don’t know where to go from here
Hi Kathy,
I am sorry Mia is still not responding to treatment despite all the different medications that have been tried. I understand your concern and think she is very lucky to have you advocating for her health and well-being. Unfortunately, I am not sure what to recommend as I usually defer to the specialists when dealing with these types of complicated cases. Hoping there is still a chance Mia can stabilize and begin the long road to recovery. Praying for a miracle for your sweet girl. ♥
Hi, I think my German Shorthaired Pointer’s ears are probably softer than Izzie’s, no offense. Softer than mink!!
Hi Dr Buzby
Our gorgeous 8 year old female border collie, Jessie became very lethargic and wouldnt eat her breakfast yesterday. She also seemed to find it more difficult to come up our back steps. In recent weeks her bark has changed a bit and become a bit hoarse. She has never had any health problems, has a very healthy diet, right weight and is fit. About one week ago she had a Lepto vaccine and the other vaccine they need annually ( cant recall what it is). After taking her to the vet yesterday, she has had an array of blood tests and an ultrasound. The vet was looking for a cause of the IMHA before proceeding with treatment. She had a PCV of 23 this morning but it went down to 16 as the day wore on. Her ultrasound revealed some swelling in the lymph nodes but the vet didnt think it looked like Lymphoma and . They have taken some fluid from the lymph nodes and sent them off for testing. Her bloods are consistent with IMHA and today she was showing some jaundice. Our vet is going to give her a transfusion over night and she will commence cortisone to address IMHA where the cause is unknown as well as antibiotics in case there is a urinary tract infection while they still wait for some test results to come back. We so worried about her and whether we are putting her through too much. We just hope she might stabilise over night.
Dear Wendy,
I understand your concern for Jessie and am so sorry she is facing this scary condition. I am glad your vet is taking such an aggressive approach to her treatment and think the blood transfusion is very good idea. Praying that her body will respond favorably and for things to stabilize quickly. Wishing her all the best at making a full recovery. Feel free to keep us updated on how things go.
Hi Dr Buzby
Our gorgeous Border Collie has now had 2 transfusions, been on the medication for 5 days but is starting to show some positive signs. Her PCV was 18 yesterday and is 19 today ( still not increasing much but stable), her bilirubin level has gone down significantly and although not normal there has been a dramatic improvement, she is still eating well and has been getting brighter for 3 days now. All other vitals good. She is not showing much yellowness anywhere now, gums good, tummy almost back to normal whiteness colour. The vets are pleased with the way she is going. Today is her 8th day in hospital. We visit her everyday and we have definitely seen a great improvement in her condition. The vets have diagnosed Addisons disease too but it is Ok with the medication. What do you think?
Hi Wendy,
It sounds like your sweet pup is in great hands, and I am so glad to hear that she is stabilizing! Everything you have said sounds like progress in the right direction, and while I’m sure it is hard to not have her at home, she is where she needs to be so that the veterinary team can keep a close eye on her. I hope that she continues to improve and that she is back home with you soon!
I am an American living in Rome, Italy, and have found this site. We adopted Corrado a Blenheim Cavalier King Charles Spaniel on 7 April 2024 from Catania, Sicily, where he was abandoned on 19 March for unknown reasons. He was 5 years old at the time and we knew he had vision problems as the volunteer sent us videos where it was mentioned he his eyesight wasn’t the best (we saw he bumped into things). We fell in love with his energy and sweetness and said we would take care of him as our other Cavaliers had vision problems also. Upon his arrival in Rome, we conducted a battery of exams to establish a baseline for his medical history. He was diagnosed with borderline leishmania, bilateral hereditary cataracts but was heart ok which was great given we have had two Cavaliers before with MVD among other diseases like Syringomyelia and Chiari. His HCT in April was 43%. After six months, additional tests were run and his heart values improved because we took the advice of the cardiologist to give him Omega 3 twice a day, his HCT was 40%, and the cataracts deteriorated a lot with the left eye also experiencing some paralysis. We conducted ophthalmological and neurological exams. The neurologist found nothing worrying and said the paralysis will clear up in a few months (his eye still does not blink regularly meanwhile he no longer has a droopy left jowl – this issue came to light on/about 2 Nov when we noticed him going around in circles and immediately took him to the vet) while the ophthalmologist advised the cataracts were hyper mature. We decided to have him undergo cataracts surgery which took place on 9 Jan 2025. It was a success with the exception of a curveball found during the surgery of a luxating left lens that the ophthalmologist fixed with a microscopic hook and now Corrado could see dogs and pigeons, barking and reacting to all whereas previously there may have been a delayed reaction like chasing a pigeon about 15 seconds after it passed in front of him. He was active and playful and greeting neighborhood shop owners always seeking treats. He also maintained his voracious appetite. His poop was normal for the first three days – he eats Lily’s Kitchen Salmon Supper topped with Virtus salmon/carrots/greens beans and dried carrot and sweet potato treats throughout day – but then started to appear darker, still 2.5 scale in terms of consistency which the vets said was what was important and that is what counted, noting that medications like prednicortone and atoplus (cyclosporine) plus the anesthesia would cause it to be darker. But four days after the surgery upon drinking water Corrado howled like we had never heard before in the 9 months since his arrival and almost fainted. We took him to the vet and and the HCT was 22%. They were not concerned and sent us home. The next day upon drinking water again he howled. His gums were paler than the day before and so we rushed him again to the vet. His HCT was critically low at 14% and he underwent a blood transfusion under the presumed IMHA diagnosis on 15 Jan. He stayed overnight for two nights while the clinic sent blood work to Clinica San Marco in Padua, the best veterinary sciences clinic in Italy we were told. His first HCT level went back up to 32, then 30 two days later on 17 Jan when he was released. Meanwhile, the results came back with IMHA positive and also a diagnosis of Borellia (a form of Lyme disease) which the internist believes was underlying for some time perhaps contracted in Sicily and was not caught on any of the two blood exams we did in Rome as normally that tick borne disease is not part of the line-up. From 15 Jan, Corrado started on mycophenolate, plavix and Vibravet (doxycycline), yet the HCT results varied every three days we took him to 28 on 23 Jan and 26 on 27 Jan and 22 today, 1 Feb. He has energy spurts throughout the days and does long slow walks of 30-35 min, excited to go out at first, trying to jump, but has lost a lot of muscle mass and slows down by end of walk. His gums are a light pink, but get lighter throughout the days – peaks and dips. The internist is surprised the mycophenalate is not working and has now prescribed the pharmacy to tailor the dosage to his weight (13 kg – yes, he is a husky sized Cavvie – so 156mg twice a day from 125mg twice a day). We are waiting for the new pills to be ready tomorrow. Is there anything more we should be doing? Diet wise? Also, a quick note to say the eyes are healing so well that the ophthalmologist could not stop smiling over how much progress there has been given the issue with the paralysis for which he added to stitches to outer left eye to keep more closed and ensure lubrication due to reduced blinking and the luxating lens. I have given a lot of detail and history which I hope helps.
Dear Harriet,
My heart goes out to you as you continue to battle this complex disease in your senior pup. Corrado is very lucky to have you taking such good care of him and advocating for his health and well-being. I am not aware of any diet changes that would be helpful but there may be a medication you could try. It is called Romiplostim. The use of it in veterinary medicine is still experimental but we have had a few readers report great success using it to treat a form of IMHA called intravenous thrombocytopenia (ITP). I will attach a link to our ITP article. Please look through the comments section and see if you can find the information left by a reader named Chomissa. I think you are doing a great job and what a blessing your boy has regained his sight! Feel free to keep us updated as you walk this unknown path. Wishing you both continued success and praying for a full recovery for Corrado.
ITP in Dogs: Through the Eyes of a Veterinarian and Dog Mom
I have a 13.5y old Golden who has had osteoarthritis since he was 3 years old. He has been on catrophen injection for years and using them mostly whenever he needs it and in later years doing a 4 wkly shots to help him along. Today he was diagnosed with immune mediated hemolytic anemia and we have an xray in a few days to investigate what appears to be a mass in his tummy which I realize could mean Hemangiosarcoma :/ but let’s see. For a few days, he was taking 600mg of gabapentin (28kg) and that totally caused hind leg weakness to the point that we had to lift him up to get him to move, carry him downstairs to go for a pee/poo outing (backyard) and then carry him back up stairs. He was struggling with some stiffness as where we live is super cold (central Canada) but it seems to have declined quite quickly into hardly being able to use his legs. Today after speaking to the vet, we dropped his dose by half to 300mg a day.
I wonder how quickly I might see some improvement in his hind legs ? Could this also allow him to be less drowsy? I know he is old and I don’t expect him to be as active as a puppy but I would love to have him more alert and interested in life again as he was before we started these meds.
Other meds we are now on include: gabapentin 300mg / day; galliprant 60mg /24h; prednisolone 60mg/day given twice (10 days before a blood test) and an antibiotic Clavaseptin 375mg/day (14 days only- as the blood test indicated sign of infection)
For a dog who hardly took one NSAID in his life all of this seems a lot. I have also read mixed things about galliprant not to be used with prednisolone. I just feel concerned about all the interactions and trying to digest it all. I would love if our sweet pup could go into remission and be more himself again.
Any insights/ lessons or prompts to further investigate with my vet would be so appreciated.
🙏🏽
Dear Joan,
I am sorry your boy is dealing with so many issues at once. I understand your concern and think it is good you are searching for advice. Weakness, wobbling and sedation are all possible side effects of gabapentin. The good news is these side effects are usually temporary and resolve within a few days as the body has a chance to adjust. You should start to see a difference soon, especially within a week or two. While galliprant is not supposed to have the same effects on the liver and kidneys as with other NSAIDs, I would still be cautious about combining it with steroids. When you use steroids and non-steroidals together there is a big risk of causing GI ulcerations and other severe complications. I hope your senior guy can overcome these health challenges he is facing and restore his quality of life. Praying for healing and a positive outcome. Bless you both.
My Frenchie, Beau, was just released from the hospital after spending 5 nights there, ad he was diagnosed with IMHA. He had 3 blood transfusions and is finally eating on his own. This article has been so helpful to understand the disease more. We’re now waiting to get into the speciality vet, and look for a new primary vet, as ours has no expierence with IMHA.
I’m told that dogs with IMHA will no longer get vaccinated. Is that accurate?
Hi Lisa,
I am so glad to hear that Beau is improving and has finally started to respond to treatment. It is true that vaccines can cause a relapse of IMHA and should either be avoided or given with extreme caution. Some states will not allow for a medical exemption from the rabies vaccine and other vaccines may be needed based on risk. I would discuss your dog’s situation with the specialist and see what they recommend. Hoping for continued success for your sweet boy and keep up the good work!
My hound mix developed IMHA at 9 years old. Her RBC was typically 40. It had fallen into the teens. 3 nights in the ICU with fluids and steroids turned her around. Then home care with more meds and regular blood tests. She is now 15 years old and still with me. It’s a very scary disease but some dogs do survive it. My heart goes out to those dealing with IMHA now and those with dogs less lucky than mine.
Hi Susan,
I am glad your girl has done well since her IMHA diagnosis. What a blessing you have gained so much extra time together. Thank you for sharing your story with us as it will offer hope to others as they face this difficult disease. Wishing you and your sweet girl continued success and many happy days ahead. Bless you both! ♥
Thanks for posting this article. I lost my dog, Sophie, to IMHA last week. I have been directing friends and family to this article to try to explain what happened. Nearly everything you discuss crossed my path in the few days we struggled to save my dog…..tests, treatments, symptoms…all of it.
Sophie was 10.5…but acted much younger. Other than two Grade I MCTs in the last few years, she was healthy. The very first sign that anything was wrong was on a Sunday morning…it took her twice as long to eat her breakfast. She’s normally a chow hound. That night she wouldn’t eat her dinner. She threw up overnight. I thought maybe she had a bad tooth (due for a cleaning) so I opened her mouth to check and saw the pale gums. It was about midday on Monday when I took her to the ER where she was diagnosed with IMHA.
We were transferred to a specialty hospital. She walked in under her own power….but that was the last time I saw her stand or walk. Overnight they started her on steroids and immunosuppressants and gave her a blood transfusion. They did not find a smoking gun. Nothing significant on her chest x-ray or ultrasound. The rapid tick-borne illness test run by the ER was negative. The results of the more detailed tick-borne illness panel are still pending.
By Tuesday morning her skin and eyes were mustard yellow. She was a white dog, so…it really shows. She started showing some neurological signs (including some seizures) and, based on how rapidly she was declining, we decided to do the plasma exchange*. We hoped we could sustain her long enough to give the steroids and immunosuppressants time to kick in.
By Wednesday she wasn’t really any worse, but she wasn’t any better either. We elected to try one more round of the plasma exchange. Her plasma looked so much better and she was a bit less yellow. Her body had stopped breaking down the red blood cells. We had halted the immune response. Now we just needed the rest of her to come around.
Sadly, there was too much damage for her body to recover…blood clots being the most likely culprit. The vet called me around 4:15 on Thursday morning to say she was declining and having more seizures. I drove over and we put her down.
From normal and healthy…to dead…in 96 hours. It happened so fast. This disease is terrible. I am still in shock.
*I should note that all my dogs have pet insurance. There’s no way I could have afforded to try the plasma exchange treatment without it. She probably would have died within 48 hours without the plasma exchange.
Jennifer,
What a stressful and heartbreaking 96 hours. You did everything you could to try to save Sophie’s life, and I have no doubt that she knew how much you loved her. Thinking of you as you process and grieve this loss. ❤️
I just had this happen to my 2 year old boy. This is almost exactly what we went through, but didn’t get to the plasma because he started seizures and they were concerned he had a clot that had traveled. He declined so fast and I couldn’t bear to see him keep struggling. I had just over 24 hours from when I first noticed any signs, to losing him. He was fine the night before, woke up stumbling and peeing brown red. My local vet didn’t correctly diagnose him and the ER did, but it just didn’t help him. I don’t know if steroids earlier would have helped, and not wasting 4 precious hours at the first vet, I have never heard of it and am trying so hard to understand how and why this happened. It was the worst thing for such a sweet, young dog and I struggle with what I could have done differently for him.
Dear Rachelle,
My heart aches for you with the loss of your beloved pup. It is normal to ponder all the “what ifs” while grieving, but please don’t let guilt weigh you down. You did everything you could to give your boy the best chance at survival. There were probably no earlier signs or symptoms to miss and I’m not sure there was a way to change this outcome. I am certain your boy knew how much he was loved and that your presence during his final moments was a comfort. I hope with time your heart can begin to heal, and you can find peace. May the memories of all the good times you shared stay with you always. Bless you.
I have a dog that was getting lethargic and eating dirt but otherwise acting fine. When I took him to the vet after many tests, it turned out he was severely anemic and we started treating him for a stomach ulcer, pancreatits, and possible IMHA. One issue with the IMHA diagnosis is his anemia is non-regenerative. Over a 3 week period of time, he’s lost over a pound (his normal healthy weight is about 12 lbs.) despite my continuing to increase his food. He’s up to 3 times what he used to eat. His appetite is fine. He did a course of Doxycycline, we’re still treating his stomach but I think we’re about done with that. He’s only vomited once that I’m aware of, and infact only had diarrhea once. He had a blood transfusion last week after which he felt GREAT for about a day, then his gums were pale and tacky again and he was back to lethargy. He’s also taking steroids, mycophenolate, and gabapentin. We talked about doing a bone marrow test, but basically my vet said anything we find we’re already treating for or it isn’t treatable. I’m really afraid he has cancer.
I thought I had a question but I guess not. I’m just trying to find hope somewhere. He’s having breakthrough pain, his gums are still pale and tacky (he had pink gums for ONE DAY after the transfusion). I’m just so scared for one of the best dogs I’ve ever had=(
Hi Julie,
My heart goes out to you. It is so scary to watch a beloved dogs face a health crisis and not see the much-hoped-for improvement. It sounds like your vet has put together a wonderful treatment plan for suspected IMHA. Based on the short response time to the blood transfusion I agree that blood is either getting destroyed rapidly or being lost somewhere in the body rapidly. I’m wondering if it would be worth going forward with a consultation with a veterinary specialist as a way to leave no stone unturned. Yes, perhaps you will find something bad that isn’t treatable. But at least that way, you may have a better idea of what is triggering the anemia and what that means for your dog. This definitely sounds like a challenging case. I’m so sorry that you are having to face this with your dog. Thinking about you and hoping that things will turn around for him soon! ❤️
Our 4 year old Springerdoodle started picking at his food about a week ago. 3 days later he went severely downhill, not eating and barely moving. We took him to the emergency vet where he was diagnosed with severe primary IMHA, PCV at 12. He received a blood transfusion and all the meds mentioned in other posts with an immediate boost to a PCV of 34 sustained overnight, and ate well at the hospital. While on my way to pick him up and transfer care to our local vet he suffered some sort of neurological event (eyes twitching, crooked walking, uneven gait). We went ahead and brought him home. We are continuing care with our vet and so far his PCV is holding but he refuses to eat, even though an appetite enhancer drug has been added to the mix. We are feeding him a high protein drink through a dropper right now and our vet is going to give him an IV with electrolytes in the morning. We have offered every food imaginable, all the recommended things like chicken, rice, low fat hamburger, even ice cream just to encourage him – no luck. Hoping the IV will give him the boost he needs to start eating again.
Dear Kim,
I am so sorry your boy is experiencing such severe symptoms after his IMHA event. It sounds like the veterinary team is doing all they can to give him the best shot at recovery. How are things today? Did the IV fluids help to improve his appetite? Praying all is well and for his health to be restored. Feel free to leave an update and let us know how things are going.
hi,my dogs ame is Morpheus. He is a gsd and he is about 1 yrs and 6 mos old and about 95lbs. He had gotten sick a week before christmas dec 2023. He was in the hospital for about a week and was diagnosed with IMHA. Fast forward to april 2024 he is fully recovered and off his Cyclosporine, Prednisone, and blood thinners. He originally had his first attack due to an allergy shot he was receiving every 6 weeks (cytopoint) Our vet firmly believes hes okay but had us sign a rabies exemption paper in VA. Fast forward again to present day june 7th 2024. My husband is in the marines and we are stationed in NC and we have an issue where the base is possibly rejecting Morpheus from being registered on to base because of the rabies exmption. they will test him to see if he still has it in his system from his first rabies vaccine. I need advise, do i A. give up my dog or B. get him rabies vacinated with a risk of another IMHA attack? Please i need input,help,advice,prayers, etc….
Hi Evelyn,
I am sorry you are facing this extremely difficult situation with your pup. It would be best to discuss this issue with an internal medicine specialist. They can give you all the details of risk vs. benefit from vaccination. Although it is a bit controversial, you can administer steroids prior to the vaccination to try and prevent the immune system from reacting negatively. The problem is you are suppressing the immune system and therefore may also suppress the effectiveness of the vaccine (the immune system has to respond to the vaccine for the dog to be fully protected). Best case scenario is the Rabies titers come back high enough and you don’t have to worry about repeating the vaccine. Hoping you were able to get things figured out and make the best choice for Morpheus. Feel free to leave an update if you have a chance. Best of luck to you both!
Hi, my dog Kobe is currently in the hosipital due to IMHA. He did it eat for one day and the next started to urinate blood. We rushed him over to the ER and we’re told his heartbeat was weak and his pcv levels are at 13. He’s currently been through one blood transfusion and his numbers are now at 18 after twelve hours from the transfusion. We are on day two and he still won’t eat and is still urinating blood. The vet said he might need to stay because he want had appetite but I’m hoping he can fight through this. Kobe is a 1yr and 10 months golden doodle. ❤️
Hi Josh,
I am so sorry Kobe is fighting this terrible disease. I am glad you were able to get him to the ER quickly and they are doing their best to give Kobe every chance to pull through. Hoping he can stabilize and start the recovery process. Praying for a positive outcome for your sweet boy.
In Nov of ’23 our then 11-year-old dog started vomiting on a Friday. I thought she got a hold of some candy at Halloween. Sat, we woke up to piles and piles of vomit, I tried giving her some Pepto still thinking it was something she ate and shouldn’t have. She normally takes medication pretty easily, but this became a struggle. I make some chicken and rice and she wouldn’t even go near the food, so I became very worried at that point and rushed her to the emergency vet. She wasn’t herself during the car ride or sitting in the vet office which is when I noticed her tongue and gums were completely white. Vet came in and did some bloodwork and confirmed it was Primary IMHA. She was at a 24 but they wanted to keep her overnight to stop the vomiting and give her fluids. We went to see her that night and they let her go home saying she was doing better and finally eating. Sunday was not any better, so I rushed her back to the ER Vet, and they tested her blood levels again. She was at a 12 this time. She received a blood transfusion and was able to come home a few days later. She’s been on a pretty high dose of prednisone and still on mycophenolate. Her CBC levels still are mid 20’s with a one time high of 34 since all this started. She has since turned 12 and having her monthly checkups with the vet for bloodwork. Couple weeks ago, her numbers went down to 27 so we are now back to every 2 weeks for CBC. Took her this week because she started vomiting and her number is down to 24. Not sure if she is going into a relapse. Scared that if she does relapse, she will not have the outcome she did the first time around or that I can afford another round being just a few months in-between. She was always my energetic wild child of a furbay but since Nov she has lost a lot of body mass and has not fully gone back to the furbaby she was. This disease is horrible, and I hate to see so many of you going through it as well. Lots of love and hugs to all of you.
Dear Kristi,
I am so sorry you are facing this difficult disease in your senior girl. I can only imagine how worried you must be with this slow decline in her red blood cell count. I am hopeful that she will continue to respond favorably to the medications and be able to stabilize. Feel free to leave an update and let us know how she is doing. Praying for healing and a positive outcome.
I moved out of the house a few months back. The family dog and I were inseparable and it was super hard to do so. I visit him a few days a week. In the past few weeks he seemed a little more off than usual. He was being super picky with his food, sniffing it then walking away, laying around, just overall seemed down. We chalked it up to being depression from the split but we decided to get him checked up at the vet. Our first visit held nothing concrete. His rbc count was a little bit lower than normal (i think around 36%?). Xrays negative for any foreign bodies. We were sent home with instructions to just give him to Pet-tinic to try and help him get some iron in his body. Vet calls us a couple of days later and ask to bring him back in for another look. This time a second vet examined his labs. His rbc percentage 3 days after the first appointment was around 34%. The vet looked at his blood slides and concluded that Cooper has IMHA. He said that we caught it very early so thay his outcome looks positive. He started us on prednisone with weekly cbc checks. He mentioned that if all goes well we can slowly wean off the medicine and hopefully Cooper enters remission.
Hi RB,
I am sorry you have been through so much over the past few months. What a blessing you were able to notice these subtle changes to your pup and get a diagnosis before things had the chance to progress. Hoping the prednisone will be enough to get the IMHA under control and praying for a quick resolution for your sweet boy. Thank you for sharing your experience with us. Wishing you all the best for happier days ahead.
Hi RB,
My pup was just diagnosed with IMHA. His current treatment is prednisone. Thankfully he is eating well and drinking. He’s slower, but can get around. How is the prednisone working for your pup? Mine has only taken 4 doses. Thanks for your response.
Hi,
About 3 weeks ago my dog Emmett seemed off—lethargic, eating sporadically—for a couple of days. Although he “bounced back” we took him to the vet. His CBC showed mild regenerative anemia, his blood was clotting, and other indicators of IMHA.. He also had an ultrasound that showed no sign of cancer or anything else causing the anemia. At the moment he is stable and on Plavixx, an antibiotic, Sucralfate, and something to replace his carprofen, which the vet discontinued. He now is waiting 2 weeks until his next CBC to see if these drugs address possible secondary IMHA. My question is about the timeframe. Is this normal? He’s ok now but I’m really concerned this could progress to an emergency while waiting for an official determinative diagnosis. If it’s IMHA, and it definitely seems like it is (to me anyway) should he get in sooner and start treatment to avoid an emergency?
Thank you for your time.
Hi Perry,
I understand your concern for Emmett with these abnormal results on his lab work. I know you are anxious to get your boy on the road to recovery, but if he is currently stable, I would hate to rush to put him on very strong immunosuppressive medications. As long as his symptoms are mild and your vet is comfortable with his blood counts, then I see nothing wrong with scheduling a recheck in two weeks. Of course, if you start to notice a change in behavior or new symptoms arise, I would contact your vet right away. Hoping Emmett will continue to improve and praying he can make a full recovery. Wishing you both the best of luck!
Hi, we lost our beautiful cockerpoo at only 6 months old to IMHA. She had 2 blood transfusions and was on all the medication. We were lucky to have her home for 5 days after the blood transfusion, but sadly she lost the fight. Her little body wasn’t strong enough. We are heartbroken and didn’t know about Imha! We miss her dearly and pray for better quicker treatment for our beloved babies!
Hi Angharad,
My heart goes out to you with the loss of your puppy. I am glad you were given the opportunity to spend those 5 days at home together before she passed. Wishing you comfort and peace during this difficult time. Bless you. ♥
Our 1yr 10 month old 69 lb male pitbull got diagnosed with IMHA a couple weeks ago spent 6 days in the hospital and received all the bells and whistles- 3 blood transfusions, all the medications, and an finally an IViG infusion that I believe helped stabilize his red blood cell count It was as low as 14 and 11 at one point. He was discharged 6 days ago 10 lbs lighter, with jaundice and a RBC count of 19. He has since gotten his appetite back, has increased energy and his gums are finally looking pink! My concern is he looks more skinny and bony than when he was discharged. He of course has a follow up next week but wondering if the medications can cause that much significant muscle loss in a dog his size? Or maybe he was swollen from the IV fluids and now he isn’t? He came home with steriods, antibiotics, anticogulant, etc. Thank you!
Hi Oly,
Goodness your poor boy has been through so much over the last few weeks! I am glad he seems to be improving and responding well to the medications. Steroids can cause a loss of lean muscle mass, but I am not sure I would have expected it to happen this quickly. I do think it would be best to discuss this with your vet at the recheck and get their expert opinion. Hoping things will continue to head in the right direction and praying your senior guy can make a full recovery.
Our 21 month old standard poodle was diagnosed with IMHA 3 days ago. She first started being lethargic on a Sunday with labored breathing. We took her to a vet hospital where they were focused on a respiratory issue, They did a chest x-ray, CBC, Chem 10, and platelet count. She had a fever of 105 and an RBC of 25. The vet on staff prescribed Rimidal and told us to follow up in 48 hours. The next day however (Monday) we noticed her eyes and gums yellowing and took her back to the hospital where they did more blood testing and diagnosed the IMHA.. Her RBC was still 25. She started prednisone Monday night and it is now Thursday and her eyes are almost completely white again. I can see some pinkiness returning to her gums. She is drinking and eating.. Her respiration appears slower and less labored. However she is still quite lethargic and tires very easily. We have a follow up on Monday. Are we on the right path? I am still concerned about the lack of energy and wondering how long before I should see her acting more like herself.
Hi David,
I can only imagine how scary these last few days have been for you and your family. I am glad the vet was able to make a diagnosis and get treatment started quickly. It sounds like your girl is doing better and all her symptoms are improving. Gaining her energy back will take some time. Try not to get too impatient with the recovery process. Hoping things will keep going in the right direction and praying for no setbacks. Feel free to leave an update if you have a chance. Wishing you all the best and keep up the good work!
4 days ago, my dog was at the vet for his annual blood work/heart worm and a nail trim. The next morning, he didn’t eat and was very tired. At one point, he seemed dizzy and collapsed. The next day, I found a vet that did a CBC and his HCT was 3.9%. She said it was bad, but ultimately said to start with meds and not a transfusion. The next 12-24 hours past without much improvement, I reached out to another vet with his blood work and they requested I bring him in for a transfusion now or he might not make it. Does anyone have thoughts or opinions on why their thought process was so different? Ultimately, he had a 10 hour blood transfusion last night and is still on his meds. His HCT seems to be holding, but it working through some fluids on his abdomen. She is keeping him for a few days to monitor. I am hopeful that we can monitor this and avoid a relapse. I don’t have pet insurance, do you think I could still get it in case of a relapse? Anyone else have any thoughts or recommendations for him? Unfortunately, I was traveling during this so have to establish a new primary care provider next week when I go home.
Hi Phillip,
I am so sorry you experienced this worrisome situation with your pup especially while out of town. While some things in veterinary medicine are straight forward, others are more subjective and depend on the individual vet’s experience and personal preferences. This is one of those subjective situations where you could probably get a recommendation from 5 different vets and all 5 could be different but at the same time all be acceptable ways to proceed. While you may be able to obtain pet insurance, they may not cover anything related to IMHA as this would now be considered a preexisting condition. I encourage you to contact different insurance companies and gather as much information as possible. Hoping your boy is feeling better and was able to make a full recovery. Best wishes to you both and feel free to keep us updated with any new developments!
My 9 y.o. Lab/Pit kix was diagnosed last Thursday. it happened literally all of a sudden. Wednesday he was fine and then Thursday he was completely down. we had an emergency visit and he was diagnosed. he wad at 25% so we didn’t need the transfusion. he was given sub-q fluids, a b12 shot and a steroid shot. we were sent home with immunosuppressive meds, antibiotics and more steroids. Friday morning around 2am he ate a beef stick and some meat baby food and drank water. he was also able to walk to greet his dad when he came home from work around 330 am. he hasn’t been able to walk at all Thursday. I have high hopes that his numbers are improving. he doesn’t have much interest in kibble but will eat homemade food and drinks plenty of water. I’m so thankful I’ve found this page. we’ve all just been a mess at home. we have a follow up apt Wednesday
Hi Tara,
I am sorry Kix had to endure this scary situation. It sounds like you acted quickly and were able to get treatment started right away. How are things today? Hoping your boy was able to make a full recovery. Feel free to leave an update if you have a chance.
My 9 year old Pitbull mix Dixie has developed this IMHA disease, we caught it on the first day when she was walking slowly, she was on the prednisone (day 2) and azathioprine (day 3) and unfortunately we can-not afford the transfusions. She has gotten worse it seems and she is now lying in bed not moving, stiff legged, her only thing is breathing, she wont eat and i have been using a plastic syringe to give her water, she can sense I’m there, she tries to get up lightly sometimes and cant so she lays back down and breathes heavy, she was at 19% HBC i believe it was called. she has another appointment Monday. I’m praying tomorrow she can start to recover as i am fearful she will not make it.. It has been 2 days since she has eaten.
Dear Hugh,
My heart aches for you as you watch your girl struggle with this terrible disease. From what you describe, I am very concerned that Dixie’s blood count is continuing to drop and am afraid she may not make it. If there is any way you can reach out to your vet now, I highly recommend you not wait till the next recheck. Praying for a miracle for you and Dixie.
Hi there! My 7 year old corgi was diagnosed with IMHA back in April/May of this year. She got down to 16% at one point. We opted to not do any transfusions as we could not shell out any more money (nonetheless thousands of dollars) on a treatment that may or may not work. So we put her on prednisone, atopica (cyclosporine), azathioprine, and eventually an anti-Parkinson’s drug as she had complete muscle atrophy for a while- couldn’t jump or get up the stairs at all. She has since recovered and the tapering of prednisone had begun. However, I have noticed over the last week or so that she isn’t super interested in her food like she had been (and normally was before the illness) and she has had recurring diarrhea every day. I have a vet appointment scheduled but worried she is relapsing now.
Hi Rebecca,
I can only imagine how worried you must be for your sweet girl with her recent decrease in appetite. I am glad you have a vet appointment scheduled and hope you can get some answers quickly. Hoping this is just a temporary side effect of stopping the prednisone and not a relapse. Feel free to leave an update when you get more information. Praying for a positive outcome. Bless you both.
Thank you for sharing Izzy’s story. I never heard of this until this Wednesday. Our Daisy did have all the symptoms of IMHA: not eating, very lethargic, yellow skin/gums/eyes. I knew something was wrong because she NEVER skips a meal; so I took her to the ER Wednesday, where she was diagnosed with it. It all happened so fast; and after I took her to the ER she got worse and worse. It’s been a two day rollercoaster but she is still fighting hard. The scariest thing is that her bilirubin is very high and making her feel terrible. After a blood transfusion yesterday she felt a tad better but that made her bilirubin increase further (to 24). They’ve been giving her anti nausea meds but she still is not eating. I am told bilirubin that high makes them feel miserable. RBC came down again this morning. She will likely need to do another transfusion today just to keep her alive. Now we wait and hope the steroids kick in and her body starts making more blood. My question is: if there’s anything that can be done to shut down the immune system faster. I also read that removing the spleen could help. Also, she hasn’t eaten since Tuesday and I’m hoping that isn’t making it worse. Thank you!
Dear Amanda,
I am sorry you were faced with this tragic situation with Izzy. It sounds like you did everything possible to give her the best chance at survival. Was she able to keep fighting and stabilize? Hoping Izzy is still with you and made a full recovery. Feel free to leave an update if you have a chance.
Hi Dr. Buzby,
Have you ever seen a dog with IMHA/ITP following vaccination with pancytopenia? My baby’s symptoms fit so well with everything I’ve read (including anecdotes) on IMHA, but I’m wondering if low WBC count would virtually eliminate that possibility… He was 10 yo, and we’d never had a CBC on him to know if maybe he just naturally had a lower than normal WBC count. I hate not definitively knowing what took him from me…
Hi Sarah,
My heart goes out to you with the loss of your sweet boy. I have not personally seen pancytopenia following vaccination, but that doesn’t mean it isn’t a possibility. I am used to seeing this condition with a bone marrow issue (such as cancer) or due to tick borne diseases. Ultimately, anything that stimulates the immune system, like vaccines, can in rare cases cause the body to overreact and lead to very strange issues. I wish I could give you a definitive answer but hope this will help to bring some closure.
Our 8 year old pup has been at the hospital with primary IMHA since Wednesday. It’s beena huge mix of emotions. I have an extremely hard time being away from him and he’s already on his 3rd transfusion all of which are adding to an exorbitant bill. I just don’t know what to do. Some of the vets at this place are very hopeful and some the complete opposite. I also don’t know if him being at the hospital so long is the best quality of life. We truly don’t know what to do or what the right answer is here.
Dear Eli,
I am so sorry you had to go through such a difficult ordeal with your senior pup. It is so hard to know what is best and how to proceed in these situations. Hoping your boy was able to keep fighting and praying all is well. Feel free to leave an update if you have a chance.
Lola, my 10 year old Bulldog mix is currently fighting for her life having been diagnosed with IMHA on Saturday. She has had 2 rounds of transfusions and began a steroid treatment.
It all happened so fast….
Wednesday night she wasn’t interested in dinner. Thursday she seemed tired and slept a lot between walks. Friday afternoon she found a quiet spot to rest and didn’t get back up until I carried her downstairs to head to the ER early Saturday morning.
She is my best friend and my heart is broken.
Dear Matthew,
My heart goes out to you as you navigate this difficult path. How is Lola doing today? Praying she can keep fighting and work her way to a full recovery. Stay strong and know you are not alone. We are all pulling for you and your sweet girl. ♥
My border whippet was just diagnosed with IMHA two days ago. She was fine one day and really really off the next day. I rushed her to the vet and dropped a bunch of money on tests. IMHA was quickly diagnosed and we started prednilosone, a stomach protectant because she was on meloxacam and an antibiotic. Her platelet count was 22% the first day, down to 17% at the start of the next day when I took her back in and at 15% when I brought her home that night. I am lucky to have put pet insurance on her… otherwise I would be over $2K in debt with bills so far. I had them do an ultrasound of her belly to make sure there was no cancer… a previous dog had similar symptoms when she had splenextic cancer. Today when she went in, her level was 13.5%… I still asked for a blood transfusion to help by her time.
What are the chances, if she beats this, that she can return to her normal fun of agility, disc and flyball or is she now a house pet? I will love her nonetheless but I am a realist and also need to prepare my young daughter for no more playing with her in the yard the way we used to. I know this could be a long road and we are only at the start.
Hi Carla,
I understand your concern for your pup and this unknown future. I hope she is still fighting and am praying for a full recovery. As for her chances of living a normal life post IMHA diagnosis, they are very good! While she will be at risk for a possible relapse in the future, exercise shouldn’t be a major trigger. Things I worry about are substances (vaccines, etc.), diseases, and issues that will elicit an immune response or cause the immune system to overreact. Of course, I would want to default to whatever your vet or the specialist recommends. But I would not completely count out the possibility of agility, flyball, or playing in the future. Best wishes to you and your family. Feel free to update us as things progress.
Our 7 year old shih tzu, Rio was diagnosed with IMHA yesterday. About a week ago I noticed a decrease in his energy levels but thought nothing of it because he was eating, urinating and having normalish bowel movements. Then 2 days after that he had no energy and dark poops. Then it was sleep all day and had to force walks. I just figured he was tired due to all our summer walks. 5 days later his skin, tongue and eyes got white and he wasn’t his normal over energized self who would bark at the mail man and get over excited to play with our kids. His RBCs were at 15% and the doctor and now he’s on prednisone and doxy. He’s eating some basic food but won’t touch his regular dry food. drinking a lot and peeing. Hasn’t had a bowel movement in 2 days. Growing up I couldn’t have a dog where I lived but always wanted one. For my 40th birthday Rio joined our family and overnight 7 years later this horrible disease has consumed him. it’s scary because we don’t know if he will return to his normal self and get better at all. we have a f/u on Saturday but the last 12 hours he looks really pale and basically gets tired walking to his wee wee pad and back.
Dear Chad,
I am so sorry Rio endured the effects of this terrible disease. I understand your concern and know you would do anything to help him feel better. How are things today? Hoping you received good news at his follow up and praying things have turned out for the best. Feel free to leave an update if you have a chance. Bless you and your sweet boy.
I have now lost 2 beautiful Cocker Spaniels to IMHA. One at 9 years old and the other at 10. It is such a horrible, devastating disease. I am so happy to see many success stories in the comments! I wish everyone who has to fight this battle with their pet all the best. You’re not alone! I’m terrified to get another dog and lose him to IMHA too, but I miss the companionship and unconditional love they can fill your life with. I hope more research is underway for this disease so that more dogs have a fighting chance with better treatment options that don’t affect their quality of life. Thank you for this easy to follow and concise article!
Hi Sky,
My heart goes out to you on the loss of your two Cockers. IMHA really is a terrible disease, and I’m so sorry to hear that it claimed the lives of two of your dogs. I agree with you that is always scary to open yourself up to the potential of losing a beloved dog, but they also bring so much joy and light to your life. I hope that in time it becomes clear to you if you should get another dog, and that you can find comfort in the wonderful memories you have of the dogs you lost. Thinking of you!
Hi my sweet boy was diagnosed June 18 with IMHA. He spent a week in ICU and came home june 25. He had a recheck this past Thursday and got a great report. Next week he goes again and then 2 weeks after we see if we can start weaning him off. He’s eating and drinking normal minus being extra thirsty bc of meds.’ He’s also eating like crazy thanks to meds. However he appears to be smaller still and maybe even losing weight.. I’m slightly worried bc he seems smaller now than when I brought him home . We were told it’s type one and that all organs were fine with no disease no internally bleeding and no masses which im thankful for just so worried about him being smaller.. is this normal ?
Hi Jana,
I am glad your boy is responding well to the treatment and his blood work continues to improve. Without examining your dog, myself, it is hard to know exactly what you mean by him being smaller. This could be weight loss and/or muscle loss which can be a side effect of steroid administration. Have you mentioned this concern to your vet? They should be able to evaluate your pup and let you know what changes have occurred. How are things with your sweet boy today? Hoping he has made a full recovery and was able to wean off the medications. Feel free to leave an update if you have a chance.
My dog began to also seem smaller, lost some weight. She could no longer jump on the couch or go up stairs (which is very unfortunate as our house is at least 8 steps to get inside). It turned out she had muscle atrophy from the steroids and they had to put her on an anti-Parkinson’s drug to help her nerves fire off. She has since built her muscle back up and can jump on the couch and go up stairs again! Maybe this is something to bring up to your vet!
my 15 year old pom was diagnosed 5 weeks ago. we caught it at her yearly check up before any symptoms began. she was at 17%. they started low dose prednisone as she also had a grade 5 heart murmur so fighting fire with fire at this point. she’s also on the cyclosporine. she’s had ultrasound and x-rays that show no underlying secondary cause for the imha. her numbers have been holding steady around 28%. she breaths deeply but still no other symptoms (except pale gums) we’re trucking along. praying for the best and making sure her quality of life stays high. she still bosses us around for treats and dances around until she gets them. our 15 year old girl has gone thru so much in her years. siezure after hitting her head. broken leg after jumping off a high chair. heart disease and now this. she’s so brave and strong. thank you for your article.
Hi Angie,
I’m so glad that you caught your pom’s IMHA so early and that she is holding steady. It sounds like she has had her share of challenges over the years, but continues to have a great attitude. I hope things are still going well for her now. Please feel free to give us an update!
Unfortunately IMHA stole my precious 2 yrs old Wren-egade from us. We noticed she was off on Wednesday and then Thursday she wouldn’t eat. During grooming I noticed her ears were yellowish inside. called my vet and they said to bring her in Friday. She laid beside me for the evening and then noticed what appeared to be blood in her urine. I loaded her up and too her to the emergency vet. They diagnosed IMHA and we started a transfusion because she was critically anemic (down to 12%) annd her bilirubin was an 15. Even with the transfusion we never got higher than 21%. The next vet on duty was great and a godsend with her specialty being autoimmune diseases and 25 years experience. Unfortunately by 8am Wren’s chances of survival dropped to 50-60%. I went to pick up an immunosuppressive they didn’t have on hand and in that 2 hrs Wren’s chance dropped to 10% as her bilirubin was off the scale, She was suffering strokes from thromboembolisms and all I could do was hold her as she passed. I am devastated! We don’t know what caused it, why it happened to such a young dog, and never expected to lose her in the space of 17 hrs. It just seemed like I stepped into a vortex of her needing a transfusion but knowing this would further overload her system with bilirubin because her immune system would be destroying those red blood cells too and trying to find a way to stop or at least slow her immune system. She was my constant companion, ever curious about the people and pets walking by (hence her nickname of Mrs. Cravetz) and ever loving and ever ready for a walk. My heart goes out to ever pet parent who has to deal with this horrid disease…..🐾
Dear Roxanna,
I am so sorry for your recent loss of Wren. Although 2 years was definitely not enough, I am certain she lived a happy and fulfilling life. Thank you for sharing your experience with us as this may be very helpful for others in a similar situation. May the memory of your sweet girl stay with you always and be a blessing in your life. Wishing you the best for brighter days ahead. ♥
My little shih tzu was diagnosed yesterday with IMHA. They sent her home with prednisone, cerenia and azathioprine. Said to come back in a week. It appears this illness can go south in a day or so, concerned waiting so long for a recheck. I’m so scared for this little girl.
Hi Denise,
I understand your concerns and worry for your Shih tzu. I hope the medications will be able to get things under control and help her to stabilize. Praying she will make a full recovery and her recheck will bring good news. Feel free to leave an update if you have a chance.
I wasn’t sure how to leave a comment on the article without replying. My apologies. My dog is currently being treated for IMHA and so far so good. We are about three weeks in and she’s doing much better. I know it’s going to be a long haul as we continue to wean her off the steroids. Im ok with the excessive drinking and urinating like a race horse. This article is excellent in explaining everything that we need to know from beginning to end. I appreciate you for that. I do have a question moving forward. I know constant monitoring and possibly life long medication to help manage or prevent and episode in the future is good, as my vet is suggesting cyclosporine. I’m reading a lot about diet. What are your thoughts on that? I’m seeing a lot about a diet that is high in iron and low in grains. I currently cook for my dog now so I just want to make sure she’s eating the right food.
Hi dvon,
I am glad to hear your dog seems to be doing well with the IMHA treatment so far. I agree that diet is very important and can make a big difference in a dog’s health. Unfortunately, I don’t have much to recommend specifically for this condition. Iron is critical especially when dealing with blood loss, but you also don’t want to over supplement. I am not sure why it would be good to avoid grains? I have many clients that prefer to feed home cooked meals over a store-bought food. This is a great way to ensure your pup is getting high quality nutritious foods as long as you also make sure it is well balanced and not lacking in essential nutrients. The best way to do this is to consult with a veterinary nutritionist before making changes to a dog’s home cooked diet. How are things today? Hoping all is well and your girl was able to finish weaning off the steroids. Wishing you both the best for many happy years ahead.
Hi Julie,
Thanks for this very informative and well written piece!
My dog Isla (patterdale terrier) is currently in remission from IMHA and has been on low dose prednisolone for a while now. My vet tells me there is no scientific evidence that maintaining this low dose will keep her in remission as dogs are just as likely to relapse whether they are on the maintenance dose or not.
I would love to see her free of the steroids but I really don’t want to see her go through another episode, it was absolutely heartbreaking last time. What do you think about the low dose maintenance?
Best regards,
Andrew
Hi Andrew,
I am glad Isla responded so well to treatment and is now doing great! Most specialists recommend trying to get off the steroids, if possible, to avoid all the potential side effects. There are other immunosuppressive medications that can be used instead of prednisone if it is determined your girl needs to stay on something long term. It might be a good idea to schedule a consultation with an internal medicine specialist and get their expert opinion. How is Isla today? Feel free to leave an update if you have a chance.
My 10 year old Goldendoodle Rosie was seen at urgent care vet center due to lethargy and weight loss. Her CBC revealed decreased low RBC count, high WBC and zero platelets. Her chest X-ray and abdominal US were clear. So my her vet started her on prednisone and an immune suppressant, mycophenolate and some GI meds. The thought was it is either immune mediated or underlying cancer. She immediately responded with improved energy and seems back to her old self but her blood work each week keeps declining despite being on the meds. It has been 6 weeks. I took her to medical hospital 3 weeks ago bc of black stool and bruising. They wanted to admit her for blood transfusion and more testing. I opted to bring her home for quality of life. My vet feels there is an underlying cause destroying her red blood cells and platelets. Most likely cancer. I did not want to leave her at hospital. Am I doing the right thing but not putting her through a blood transfusion and hospital stays?. She seems comfortable and very happy at home. Her reticulocyte count now is at 199 and RBC at 2! Just not sure how long she can’t last with these blood levels . We are not ready for her to go. 🙁
Thank you
Hi Lorri,
My heart goes out to you as you face this difficult situation with Rosie. I am not sure there is really a right or wrong way to proceed. I think choosing palliative care is a good and loving option as long as Rosie is comfortable and not suffering. Make sure you stay in close contact with your vet so they can monitor your girl’s quality of life and give you guidance about if/when it may be time to say goodbye. Praying for your strength and comfort as you navigate this hard path. Bless you both.
My at the time, almost 11 year old black lab was diagnosed with IMHA 13 months ago after numerous tests. Her hematocrit was at 16 percent and I was so afraid I was losing her. For this past year, she has been on a high dose of Predisone, Clopidogrel and Cyclosporin. She was taken off the Cyclosporin and that was replaced with Mychophenolate due to her lack of significant improvement. She would get slightly better, that her hematocrit would drop again, I started to do a lot of research on the computer. which led me to a company called The Pet and Nutrition Center. They seemed to have a wealth of information about IMHA so I decided to try some of their products. It was worth a shot, I felt I had nothing to lose. They recommended numerous supplements and I did purchase several. The ones that I felt made the most difference in my precious girl is the ChlorOxygen (which is also found on Amazon), Liver Glandular powder and the Daily Multi Plus. Although she is still on the Mychophenolate, she is off of the Predisone and her hematocrit is now relatively stable at 32 percent. I plan to increase the ChlorOxygen and hope I will continue to see improvement! I do not work for the company and don’t know anyone that does, but I wanted anyone that has had an unfortunate such as this one to have hope, In my opinion, my precious girl would not be alive today, if it weren’t for these supplements.
I wish you the very best! Dogs are such a blessing!
Hi Christine,
Thank you for sharing your experience with our readers. I am so glad these supplements made a positive impact on your girl’s health. I am definitely intrigued! What a blessing your pup is stable and enjoying life. Wishing you both the best for a happy future. ♥
Hi. My name is Hannah, and we have a 3 year old doberman pinscher who was diagnosed with secondary IMHA almost 2 weeks ago. He is at the MSU Veterinarian Hospital being treated. His first night going in, his red blood cells were at 7%. After an emergency transfusion, they went back up to 17%. He has been started on immunosuppressants and steroids. He has also had 2 more blood transfusions since being admitted. He usually does good the first night after his transfusion, but on the second night, his levels will drop again. He is going back and forth between 13% and 20% red blood cell level. Does this mean he needs more time for his medicine to fully work? It seems as if he’s responding to it, just not as quickly as we would like. Unfortunately, transfusions are expensive, and we cannot keep giving them to him. We just do not want him to run out of time because of costs. It has been almost 2 weeks since starting steroids and immunosuppressants. Is it common for the dogs to take this long responding to the therapy? Thank you!
Hi Hannah,
I am so sorry you are facing such a difficult situation with your young Doberman. I understand your concern for your pup and the worries that come with nearing the end of your financial limits. There really is no definitive answer for how long it can take for this to stabilize. Some dogs take several transfusions, for others they just need time, and then for some they may never stabilize, and difficult choices have to be made. How are things today? I am hoping your sweet boy is still with you and fighting to make a full recovery. Praying for a miracle!
My 6 year old Morkie started having red rashes all of his belly and wouldn’t eat. The vet diagnosed him with IMHA as result of a tick. He was given antibiotics and Steroids along with another medication that was used as chemotherapy. The Vet told us that he was a very sick dog and didn’t know if he could save him. After about 3 months of the medications his blood counts started to return to normal. My dog seemed like he was getting back to his old self. He was eventually taken off of the medications, but blood test revealed some liver damage in which he was given medication for. He did well for about a year. All of a sudden he stopped eating so we rushed him to the vet in which blood test revealed a relapse. He was given another round of the same medication but this time he didn’t respond. Each day he kept getting worse until he couldn’t walk any more. He went very quickly and I had him put to sleep a week later. I’m just second guessing what if we would have caught it sooner. He had just had his blood tested 6 weeks earlier. He seemed perfectly normal one day and the next he wasn’t eating.
Dear Todd,
My heart aches for you with the loss of your beloved pup. I understand how your mind ponders all the “what ifs” while grieving but please don’t let the unnecessary burden of guilt weigh you down. You did everything you could to give your boy a chance at recovery. It is likely your boy’s body was unable to respond to treatment and you would have been facing the same outcome even if you had known this was coming days earlier. I hope with time your heart can begin to heal. May his memory be with you always. ♥
Hi!
My dog was diagnosed with IMHA almost 3 months ago and nothing seems to be working. She has received now 2 blood transfusions and she is on prednisone, mycophenolate and azathriopine. We started with the prednisone and cyclosporine and her blood levels just kept dropping. Now with the new medication the levels are still dropping and I am at loss… She received one shot of erytropoietin last week, but it doesn’t seem to help either, at least based on today’s blood work. Is there anything we can still try? My dog is only five years old and she used to be the happiest little pup out there and I would do anything to help her
Hi JM91,
I understand your concern for your dog and this difficult diagnosis she has received. I can only imagine how worried you must be since all the treatments that have been tried thus far have not shown the results that were expected or hoped for. Without personally examining your pup, it is hard to know what to recommend. Unfortunately, some dogs just don’t respond to treatment, and I hope your girl is not one of them. If you have not already, I highly recommend you schedule a consult with an internal medicine specialist. They have lots of experience dealing with complicated cases like your girl seems to be. Wishing you both the best and praying for a miracle. Feel free to leave an update if you have a chance.
Our 9 year old cocker spaniel was diagnosed with IMHA on October 7, 2022 after being lethargic all day and having dark red urine and orange feces later in the day. We rushed him to the vet school at Mississippi State University. He received dexamethasone, cyclosporine, several blood transfusions, and finally IVIG as a last resort. He coded late at night on 10/10/22. The vets were able to revive him so we could say goodbye. We knew he wouldn’t make it through the night, and if he did he would have no quality of life, because he was gone for 12 minutes before they brought him back. He passed away at 5:15 am on 10/11/22. We were so hopeful he would make it, but we knew there was a high probability that he would not. This was the first time that we heard of this condition. I wish we had noticed taken him to the vet when his only symptom was lethargy, but we had no idea something like this could be the cause.
Dear Brennan,
I am so sorry for the loss of your senior pup. Please don’t carry around the burden of the “what ifs” and try to allow yourself some grace. It is very possible that even if you had taken your boy to the vet earlier, the outcome would have been the same. You did everything you could, and it sounds like the veterinary staff gave it their all. Ultimately, I am glad you were able to be with your sweet boy for his last moments. I have no doubt he knew how much he was loved and that it was a comfort to have you by his side. I hope with time your heart will heal. Thank you for being willing to share you experience with our readers. Bless you.
My 9 month old shepherd/hound mix (Teddy) was diagnosed with IMHA 4 weeks ago. He was at 15% he was given a blood transfusion which he had a reaction to but they slowed the transfusion down and gave him medicine for his face swelling. He came home 3 days later and was on 100mg prednisone. He was nothing like our puppy, he would give you dirty looks if you pet him or he’d take a side step away from you. Or he would sit and stare into space. Very lethargic, very hungry. He got better each week and by the 3rd week he was up to 32%. Then week 4 he went back down to 25% and his white blood cells went up. They put him on mycophenolate and placix and a 3rd round of antibiotics and they reduced the prednisone by 20 mg because that can raise his white blood cells also. He is starting to have small bouts of being his old self. He seems more focused and he licks us now, he licks our older dog, he sometimes lets us pet him and he’s wagging his tail more. He seems more like a fifteen year old dog and I worry about long term effects of the prednisone but at this point just want him to survive. I am going to ask my vet about adding iron rich foods to his diet, if that would help rebuild red blood cells I will do anything. I lost a 3 year old dog just this past January of possibly an auto immune disease which makes me think I have something unknown in my house or yard. But he had died because of something effecting his liver and he was having seizures. I was told they are not similar. The paranoia from not knowing what caused this is ridiculous. Reading the above stories has helped me a great deal.
Hi Stacey,
I am so sorry your young pup is struggling with IMHA. I know it is a rollercoaster of emotions as you watch Teddy take two steps forward and one step backwards with his progress. It sounds like your veterinary team is staying on top of things and Teddy is fighting hard to make a full recovery. I am hopeful you will see more of the fun energetic puppy return as the days pass. Praying for your strength and comfort for your heart. Feel free to leave another update if you have a chance.
Hello,
My 15 year old mini dachshund Rose was diagnosed of IMHA late July 2022. She has her first blood transfusion on Aug. 10th. Her RBC was at 14 when she received blood and went up to 35. She stayed in the hospital overnight. Rose was a very energetic dog. Didn’t think something was wrong with her until about 2 weeks ago she started being picky with food. We thought it was just her age. Luckily it was close to her annual exam and vaccine and this is when we found out about IMHA. Been seeing an internist. She originally prescribed Rose 5mg of prednisone twice a day and cyclosporine 0.2 mg twice a day. Been seeing her every two weeks for blood work. Her blood just keeps on going down but her appetite is there. A good side effect of prednisone. Here’s a little history of her blood test:
7/25 – 21 (family vet)
8/8 – 12.5
8/9 – 14 (internist)
8/10 – 35 (blood transfusion)
8/24 – 19 (24 outside lab) (mild elevation on WBC and liver enzymes due to steroids)
9/7 – 17 (outside lab 19)
9/20 – 16
9/21 – 30 (blood transfusion)
10/6 – 21( 22 outside lab)
Vet added another medicine on 9/21 and decreased the predinisone to just 1 pill once a day. The new medicine is leflunomide 1/2 a pill once a day. We did another blood test on 10/6 and her blood unfortunately went down again.
We are scheduled to do a cyclosporine blood test on 10/12 to check if she’s absorbing adequate amount of the medicine.
We are being patient as we were told it does take time for IMHA to respond to the medicine. How long is a while? Could it be that she’s old and won’t respond to medicine? She’s been a healthy dog no other issues. She did had another immune disorder when she was 2. Resorption lesions. Her teeth were all removed back then and she was fine after. Should we keep doing what we are doing? She may need another blood transfusion in November. How long do we keep doing this? I am doing my best to keep her comfortable and prolong her life but didn’t want her to be in pain and don’t want her yo leave me yet. Please let me know your thoughts.
Hi Jen,
I am sorry Rose is not responding to her treatment the way you and her vet had hoped. It can take months to find the right balance of medications to get an IMHA patient stabilized and that isn’t taking into account any relapses. Ultimately, some dogs just don’t respond to treatment and then you have to make tough decisions about quality of life. There is no way for me to tell you how long to keep trying. That is a conversation you need to have with your vet. Talk to them about your concerns and they can let you know if hospice or palliative care may be more reasonable. I hope Rose can keep fighting and make it to a point where she stabilizes. Praying for your strength and clarity to know what is best for everyone involved. Bless you.
Our seven year old golden doodle Daisy was diagnosed with IMHA in June of this year. She was in ICU total of 16 days. Multiple transfusions and even PTE “plasma exchange”. Was released on a multitude of medication‘s including 40 mg prednisone, Plavix, Mycophenolate, and blood pressure lowering, she’ was better in July, August, and most of September. She had gained about 20 pounds over this time because of the prednisone. Two weeks ago she had what I would consider her best day since her diagnosis, running, jumping, chasing a ball. 48 hours later she was lethargic, not wanting to eat, had a temperature. We took her back to the University hospital and she was admitted again With blood count at 14%. This was her first significant relapse. Blood numbers originally were around 14%. The criticalist vet did another plasma exchange but unfortunately her blood was no longer a match for blood transfusion. We made the hard decision to bring her home, enough was enough. She declined over the next 48 hours to the point of us needing to say goodbye. In the end she would not eat, she could barely lift her self up but could not go further than 3 feet before dropping to the floor again. Our team of doctors couldn’t be conclusive but they believe the origin was leptospirosis activating secondary IMHA. A note for others to think about if your situation requires making a difficult decision – when we said goodbye we had a hospice vet make a house call, we’ve done this twice and saying goodbye in a familiar setting we have found is difficult but we believe it is most comfortable for the patient.
Dear Doug,
I am so sorry for your recent loss of Daisy. You did everything you could to maintain her quality of life and when the time came, you allowed her to find rest and peace surrounded by the ones who loved her most. She was a lucky girl to have spent her life with you and your family. Thank you for being willing to share your experience. May Daisy’s memory continue to be a blessing.
Thank you
My 9 year old Pitt mix was jot eating 2 weeks ago. on Sunday so just layered around and did not want to go out ti pee. Sunday night she did not est again and felt like she might have a fever. Monday my daughter took her to a vet. they did a blood test and x-rays. they told her ro take her to the er. she took her and they said she needed a blood transfusion. after many test and 2 more blood transfusions and medications, they could not figure out what the cause was. on friday I asked If she was stable enough to go to Texas a & m for. a second opinion.. her blood count was at 16. I was told on Thursday she had a uti and pancreatitis. the vet told me she was stable enough to take her. she passed away 15 minutes Fter we left the er. How would I know by all of the test that was done if she would have been? does that sound like a dog that was stable? I heard after she passed that there is stem cell therapy that can help with imha. it has a 75% success rate. do you know anything about that?
Dear Alice,
I am so sorry for the recent loss of your senior girl. It sounds like the veterinary team worked very hard to try and save your pup. There was no way to know your girl would take a turn for the worst as soon as you left to drive her to the vet school. Unfortunately, critical changes can happen quickly and with little to no warning. I have very minimal knowledge of stem cell therapy for IMHA. This is still a very new emerging therapy option. Due to the nature of this therapy, it is only available at select specialty hospitals and can be very expensive. I am not sure if there is a practice in your area that offer’s stem cell therapy or if it is available at A&M. You went above and beyond for your sweet girl, and I have no doubt she knew how much you loved her. I hope with time your heart will heal and her memory will be a blessing.
Really appreciate this site. My Pom, Tinker, was diagnosed with IMHA in 2016, at 3 months old, following a dystemper booster. As I lived 1 hour from University of Illinois, my vet got us an appointment there, as at first she didn’t suspect IMHa due to Tinker’s young age, nor did U of I. Tinker got a transfusion, was put on prednisone, long story short, finally off it after close to 18 months (1 relapse). Now, however, we’re having flea problems. And she’s allergic to them. This is our fourth, and worst, season. Treat her and house with Cedarcide, which was wonderful last year, not so much this. Have tried diatomaceous earth, no help. Various other things.
Spoke to an old friend who was my vet for years, he said children’s Benadryl didn’t act on the immune system, but I’m not happy with other things in it. Was happy to read your take on collostrum, as I was considering trying that. Nutritional yeast was considered, but all the chews have garlic, which my holistic vet says NO GARLIC. She has since left the area, so I’m lost now, none like her here now. And she was a pet chiropractor, also. Currently use colloidal silver for healing the skin, diluted vinegar when it’s just itchy. Can you offer any suggestions/help for us? Have heard of Carnivora, but no details if it’s safe. Also have tried hemp oil and CBD oil with no results.
Thank you for being here.
Hi Laurie,
I am sorry to hear that your holistic vet has moved from your area. It is so tough to have such a wonderful relationship with a medical professional and then have to try to find a new one! Just to make sure I am pointing you in the right direction, are you looking for recommendations on natural flea preventatives or treatments for itchy allergic skin?
My 5 year old pup was diagnosed with IMHA in May 2021 and had a blood transfusion and steroids but after 5 days in hospital we were able to bring her home . After finishing all of the meds, her blood tests have been clear and positive ever since . Now we are wondering how to proceed with vaccinations as we are looking to move back to Australia. Also concerned about having her around other dogs during the trip back and quarantine which is compulsory in Australia. Any guidance and thoughts would be very welcome . We are so grateful she is still with us and so healthy but at some stage soon we need to start making our return travel plane .
Hi Alexis,
I understand your concerns with having to vaccinate your pup. This is a very tricky situation. My best advice is to talk to an internal medicine specialist. You can see if they have any ideas of treatments or therapies that could lessen the risk of triggering an IMHA spiral post vaccination. Your other option is to talk to the authorities in Australia and see if there are any alternatives due to your dog’s specific situation. Maybe they would allow your vet to send blood to a specialty lab and have vaccine titers checked? I am not sure you will have options to choose from. When dealing with government entities and the import of species that can carry diseases of concern to other animals and the human population, your hands may be tied. I hope you can find a safe resolution to this issue and your sweet girl can continue living her best life.
My dog Ginger was recently diagnosed with IMHA. July 1st she was a normal, playful 9 year old Havanese and the next day she was lethargic, lost her appetite and over the next few weeks began to lose weight. On July 2nd we took her to the vet for a small ear infection and the doctor noticed she had been scratching in one spot which caused an infection. She was given Simplicef 100mg and a dose of Cytopoint to control the itching. I didn’t know enough at the time and wish I could have gone back to that day and not given her those shots. I would take an itching, vibrant, playful pup than what has transpired over the last few weeks. I believe it was the influx of meds that caused her immune system to go into overdrive. I was hoping to know if this is something you have seen as a vet and if, once the meds leave her system the immune system will revert back to normal? All too often we try to medicate the problem away and cause more issues…
Hi Seaford Dad,
I understand your concern and grief over what has happened with Ginger these last few weeks. Unfortunately, there is no way to know if a dog’s immune system will overreact to medications or injections. Your vet had a good treatment protocol which is the standard of care in veterinary medicine. No veterinarian would diagnose a secondary bacterial infection due to itching and leave it untreated and allow it to progress and cause a myriad of potential complications. Hindsight is definitely 20/20 and it would make things easier if we could predict these rare complications before they happen. The antibiotic you mentioned (Simplicef) is in the cephalosproin class mentioned in the article that is a potential trigger for IMHA. This alone may have been the cause, but IMHA can also be triggered by vaccines, infections, or just by the immune system itself. The medication should have long cleared her system by now. There is no way to know how long the immune system will stay reactive and continue to cause issues. Simplicef is commonly used by veterinarians worldwide with great success for cases just like Ginger. I am sorry she happened to be one of the few whose body didn’t respond in the expected way. I hope Ginger will stabilize and be able to make a full recovery. Praying for a positive outcome. Bless you both.
Wow, this is the first time I’ve seen cytopoint mentioned as a potential culprit for IMHA. My dog was on it for two years – getting it every 4-6 week as advised by my vet. He almost died with a RBC level of 14. Two transfusions later he was able to come home. We’re about 5 weeks out from his ICU stay and his blood work showed that his RBC levels dropped 5%. I have been looking all over the internet to find links between anemia and cytopoint and have found nothing! Sending you and your pup lots of love.
Hi Kara,
I am afraid you may have misread part of my reply. The Cytopoint was not the suspected culprit of the IMHA but was instead the antibiotic Simplicef. Simplicef is in the cephalosporin class which was mentioned in the article as a potential trigger. I am sorry your pup is still struggling to get his RBC levels stabilized. I hope he can make a full recovery and continue living his best life. Best wishes to you both!
Our Maltese was diagnosed with primary IMHA in January 2018. Swiffer was 1st misdiagnosed after taking him to the vet twice. I knew he was dying. we rushed him to an emergency vet, recommended by his groomer. He was kept there for a couple days. He had to have a blood transfusion. After we brought him home it was touch and go for awhile. vet visits (we switched vets!) every couple days with bloodwork checked, and monitoring, since he was on prednisone and another drug. The good news was we were able to slowly taper him off these drugs pretty within a few months. Our vet agreed our dog would no longer be vaccinated.
The GREAT news is Swiffer has been in remission for 5 years!!
Hi Sherrie,
This is such an amazing story! Thank you for sharing your experience with our readers. What a blessing Swiffer is still with you and thriving 5 years later. Wishing you both continued happiness. Give your sweet boy a hug for me!
My dog has been diagnosed with IMHA for years. He’s doing fine and no meds, but he’s not able to get his vaccines because that would trigger his IMHA. Is there any way for me to fly with my dog even though he cannot get his rabies vaccine?
Hi Emilie,
That is a tricky situation. While I completely understand the risks of vaccination in a dog with IMHA, the state governments do not make allowances in rabies laws. Your best bet is to contact the airline you plan to use and see if they would take a written statement from your vet. You may also have to contact the state vet for the location you plan to travel and see what their recommendation would be. My guess is there will not be an allowance made since rabies it a public health issue and a disease for which there is no cure.
Our Bentley was diagnosed with IMHA yesterday. Initially last week on Thursday it wasn’t presenting itself to the vet just a high bilirubin. He wasn’t getting any better over the weekend and I noticed his tongue being a pale pink. We took him in yesterday. I am glad that the vet was able to give answers, Hoping that he starts to feel better. He is currently on 20 mg of prednisone. After one dose he at least was eating and drinking more. Long road, and having a mom and husband with an auto immune disease as well at least I know a little of what to expect with him.
Hi Alisha,
Thank you for sharing your experience with our readers. I am sorry your pup is dealing with an IMHA diagnosis, but glad you have some experience with auto-immune diseases. It is great that you were able to get him to the vet so quickly and start treatment right away. I hope the medication will help improve Bentley’s condition and allow him to make a full recovery. How are things today? Feel free to leave an update if you have a chance. Praying for healing for sweet Bentley.
Hi, My little doxie Peanut so far isn’t improving as much as my vet has hoped.. when I first brought her in Monday night her red blood count was at 7 after her first blood transfusion it went up to 17. Then the next day dropped down to ten and then did another transfusion the next day and it was still around that number then yesterday her red blood count dropped back down to 6 and their now doing her 4th blood transfusion now which takes four hours and have her in an oxygenated warming tank to hopefully take the strain off her heart by giving her more oxygen. Monday then started her on the Dexamethasone and protonixs because she was throwing up Monday and Tuesday she finally started eating and had to dishes of chicken that they give there and she held that down and didn’t throw up. But, yesterday Thursday night she did not want to eat for them nor me.. all she seems to want is water water water. When she see the the bowl of water she gets up and tries to get it and we give her a little at time to not upset her stomach. But last night she threw everything up.. but she’s also on iv fluids to help hydrate her. And they started her Atopica Wednesday night.. around how long would it take for these medications to kick in her system to see if it will help? And then for her nausea do they give dogs Zofran ( Ondansetron)? Or do you think that would be too much on her system? I’m just trying to think of anything to help her at this point. Before she got sick she is a very active dog and runs around it’s not like she’s old and never has energy.. this literally came out of no where Monday and she such a sweet sweet little girl.. I just want to make sure I’m giving her the best chances to make a turn around and improve.. I’ve been researching this as much as I can online reading a bunch of articles about IMHA1/ Idiopathic immune-mediated hemolytic anemia. Cause I think she’s not eating now cause her stomach is upset and I’m trying to see if Zofran might help and settle her stomach a little more so she can maybe it? Any helpful information I would be so helpful! My vet said he only treated this once before and that dog passed away after it’s 4th blood transfusion. I’m so sorry again for all these questions.. she’s like my little baby..🥺
Hi Dee,
I understand your concern for Peanut. I have read both of your comments and gone over all of your questions several times. Honestly, my best recommendation is to get a referral to a veterinary internal medicine specialist. It sounds like your vet has been staying on top of things and using the standard medications for this condition, but I think talking to a specialist would help ease your mind. They can let you know if there are other treatments that should be considered and answer any lingering questions you may have. Since I haven’t examined your little pup myself, it is difficult to make specific conclusions and recommendations about medications and symptoms. I hope you can find the answers you need to make the best choice for sweet Peanut. I pray she can make a full recovery and has many happy days ahead. Feel free to leave an update any time you like. Wishing you the best.
My little doxie was just diagnosed Monday. My vet is trying to do as much as he can to help her. Her red blood count when I first found her sick and it came out of nowhere the day before she was fine.. I found her curled up in her dog bed with throw up by her mouth and picked her up and saw urine underneath her and it was that dark orange color and rushed her in. They did blood work and an ultrasound and her red blood count was at 7% and we were told the only way she would make it through the next was blood transfusion she had her first one Monday night and one again Tuesday and two yesterday.. because after the transfusion it went up to 17% but the next day dropped back down to 7-10% so he did two yesterday and started her on Dexamethasone Monday and Tuesday and switched her prednisone yesterday and then started Atopica yesterday night. The first day she was super lethargic and had no energy and couldn’t even lift her head, now she’s able to get up and stand and walk around a little in the crate, and is wagging her tail and giving kisses. And they also have her on Pepcid for her stomach. And first day her body temperature was low also it was 98 so they have had her on a heating pad also. And yesterday night when I was with her after her transfusion she went back up to 102 her temperature. I know I was told recovery wouldn’t be a next day thing and can take over a week to see improvements. I’m wondering if there are any other types of medications that may also help her? And I read that with the blood transfusion with this condition they might also form blood clots that can travel so now I’m a little worried about that.. any advice that can help my dog a little or ideas that might help more then Atopica and prednisone, that I could give ideas to my my vet of other medications that might help her better and let my vet know. I’m sorry for so many questions this is all new to me and scary I can’t imagine if I lose her 😢.. thank you so much if you have any ideas that may help!
Our Doxie had 4 transfusions. 11 days in hospital. He went as low as 13% and now up to 42% with the help of steroids. The blood transfusions are like buying time until the meds work! Benny is still on Prednisone and Cyclosporine and will most likely be on those meds for another 4 months before we are decreasing the levels.
Hi there… Our dog Kahlua is a Frengle (half Frenchie Half Beagle) and she is 11yrs old. A year ago she was having issues of not eating and tired and took her to her Vet and they did an ultrasound as well as extensive blood work. Started her on steroids and she turned around. Of course hungry all the time..lol.. but come this past January she was on a 1/4 of a tab of steriods every couple of days. Now 3 weeks ago on a Tues she was perfectly fine in the morning and when I came home from work she was a different dog. Wouldn’t eat, could barely walk. Wed morning 2am couldn’t even get up a small step. Carried her slumped over my arms to her Vet. Her red blood cells and platelettes dropped dramatically. They gave her a massive injection of steriods and it turned her around. She was put on 20mg of steriods a day and was tested 2 days later and her platelettes jumped back up. She is now also on IMURAN. she is eating and drinking, peeing, and walking like a champ but she is beyond restless, barely sleeping, and wanting to eat all night long. This has been going on almost 4 weeks and We are trying sleep aids but they are not working. we have done trazadone and melatonin and now we tried Valium and now gonna add melatonin back in the mix cause I need my baby to just rest to get even better!
Hi Niza,
I can only imagine how scary it must have been to see Kahlua decline so rapidly a few weeks ago. I am glad you were able to get her evaluated by your vet so quickly. What a blessing that they were able to find the cause and start treatment. I know these side effects of the steroids (restlessness and hunger) can be stressful, but it sounds like the benefits definitely outweigh them. I hope with some time the steroids can be tapered to a lower dose but still remain effective at keeping your girl stable. With a lower dose you should notice a decrease in the side effects as well. Make sure to stay in close contact with your vet and keep them updated on her behavior at home. Praying for a positive outcome and many happy days ahead. Best wishes!
My sweet boy was diagnosed with primary IMHA in February 2022. One day he was fine, the next day everything has changed. Unfortunately, he did not respond to treatment. Miss him everyday.
Dear Nina,
I am sorry for the tragic and unexpected loss of your sweet pup. I can only imagine the heartbreak you experienced, but am sure your boy knew how much he was loved. I hope with time your heart will heal and his memory will be a blessing. ♥
Dr. Buzby,
My 8 yr old choc. lab mix, Lucas, has recently been diagnosed with IMHA. After 3 wks of prednisolone and doing better, he crashed again after stopping the pred. So the vet started the process over again. Currently on 30 ml. once a day till RBC is normal. Current blood work is, RDC 4.28, HCT 32.4, HGB 10.9, RETIC 212.0, and PLT 137.
I want to treat as naturally as possible, is it safe to be giving immunity boosters like immune supporting mushrooms or bovine colostrum. Seems like a catch 22, suppressing the immune system, but also wanting to strengthen it to stop it from destroying itself. I cant give up, and need to try anything I can, but want to make matter worse. Thank you
Hi Gordon,
I understand your concern for Lucas and think it is great you are researching for ways to help. Unfortunately, I do not personally know enough about different mushroom species to be able to speak to their usefulness or their potential to cause harm. As for the colostrum, I would be worried about it stimulating the immune system and causing the IMHA to worsen. There is some research that shows it may be able to “quiet down” an overactive immune system, but others have noticed the opposite effect. Also, there is some concern with quality control in colostrum supplements and the potential for toxins to be present. There are several different manufacturers, and each product varies greatly. It might be a good idea to consult a veterinary internal medicine specialist or a vet that practices integrative medicine or more eastern medicine. I hope you can find the best ways to keep Lucas stable and feeling good. Praying for a positive outcome!
Can another dog donate for blood transfusions like for people? My daughters dog just got diagnosed with this and I have a huge Pitt Bull that is willing to help her little sister if she can. We don’t have a lot of money so I’m worried.
Hi Anna,
Yes, other dogs can donate blood for transfusions! With that being said, dogs have blood types just like humans do. So, it is important to know what “type” the donor and recipient are to prevent reactions. Generally speaking, a transfusion can be done once without getting the type matched, but if a second transfusion is needed it would have to be a correct match.
that’s what saved my 2 yr old Jack Russell. the vet here has a blood bank that hasbeen gathered from some of his healthiest patients. we are very blessed. Abby is still alive and active
Hi Sandra,
I am glad the transfusion was exactly what Abby needed. What a blessing to still have your sweet pup by your side!
We are now 14 weeks into IMHA diagnosis. Meg is a 10 year old Springer. As so many other people have said she was fine one day and off her food the next. The diagnosis initially was her liver as she was very jaundice. The blood tests showed IMHA. My vet immediately put her on 30 mg prednisolone. Her blood count increased for a couple of weeks so her dosage was reduced. This unfortunately caused her bloods to crash again and she collapsed. She has now been on 30mg prednisolone for about 8/10 weeks and about 30mg Imuran to try and stabilize her RBC. She has had a couple of urine infections and unfortunately more than a few relapses. Her bloods can be at 32 one week… Back to 22 the following with no reduction in meds. We have now had another full blood test which has showed that her RBC is still being attacked. My vet has increased her prednisolone to 40mg and her Imuran to 37.5. He is also testing her faeces to make sure there isn’t a stomach bleed that is reducing her count. Being as we are 14 weeks in with no clinical improvement we are starting to lose faith. Is this normal? We are starting to think she’ll be one of the unlucky few that don’t recover. The worst of it is, she actually looks quite well. But… She isn’t allowed any excercise and as others have said, she’s very hungry and thirsty and tired. Any advice would be most appreciated as we feel completely at a loss with it.
Hi Emma,
I understand your concern for Meg and these relapses of IMHA. As I am sure you know, some cases are more complicated than others and take longer to be well regulated. I would not lose hope yet! It is never a bad idea to talk to a veterinary internal medicine specialist with difficult cases like Meg. They may have ideas about additional treatments/therapies to try. If nothing else, they can let you know if you are on the right track with your current medications and help answer any questions you may have. I am praying Meg will stabilize soon and get back to living her best life. Hang in there and feel free to leave an update any time you need some encouragement or a listening ear. Bless you both. ♥
On April 25, 2022, my golden retriever Jack was diagnosed with IMHA. Him and his sibling sister Jill had turned 3 years old 4 days prior on 4/21. Jack was born with bilateral patella laxiation and predisposed to hip dysplasia so once in awhile he will show signed of discomfort and lameness. For this he gets carprophen. I have never had to give him any more than one to take care of his symptoms. These episodes typically are a few months apart where he requires one carprofen. On their Birthday and they decided to run away from me. They always come right back, but this time jack had ran a little too hard. Carprophen can be given every 12 hours and in the next four days following his runaway activities he received three carprofen in four days. Well under the limit! Then Monday the 25th he was lethargic and would not eat or drink. Went to the vet for x-rays bloodwork, a shot of antibiotics and a shot of steroids and sent home to return the next day if he didn’t seem better. Of course the next day we returned to which he received IV fluids and by noon I was getting a phone call that he needed to be taken to the emergency vet hospital where he was diagnosed with IMHA. We are now at almost a month out. Five days in the hospital and $10,000 later my baby golden, Jack is at home trying his best to recover from this disease process. This recovery process is for sure a roller coaster. There’s no certainty to what caused him to develop IMHA. Of the huge list of possibilities the only thing that fits our scenario is my golden is also mixed with Australian Shepherd. Sheep dogs are one of the breeds that is predisposed to the possibility of developing IMHA and carprofen can cause IMHA even though the probability isn’t high. So with lots of meds two different times in the morning and two different times at night. Lots of healthy foods being given and more prayers than you can imagine we are on the road to recovery. So please keep Jack in your prayers. His sister Jill will be devastated if we lose him. She was severely depressed while he was in the hospital. I wish I could share pictures on here I have loads of them from the hospital when I thought he was going to die and I took his sister to see him. Then pictures at home with him and his sister , both with huge smiles on their faces.
Hi Sue,
I am so glad that Jack is on the road to recovery and finally seems stable. Thank you for sharing your experience with us as it may help someone else in a similar situation. I hope Jack will continue to thrive and have many happy days ahead with Jill by his side. Best wishes!
🙁 my 18 month old English Cocker Spaniel was diagnosed with IMHA on Monday. She was perfectly active on Sunday but I noticed orange pee in the morning followed by Port Wine coloured pee at night. Called the ER that night and my description of “bloody pee” probably led them to think it was non emergency UTI condition as she was still very active and wanting to eat and play. She peed blood again in the morning, refused to eat, refused to play and I took her to the vet to realise it was IMHA. She’s not “matching” with any blood donors because her blood is clotting even the donor’s blood but they went ahead with the negative blood donor’s blood transfusion (she’s +) because it was safer for some reason. She’s starting on Flebogamma tomorrow. What I would like to ask, is age a significant factor for surviving this? I’ve read way to many articles on IMHA online and this has been the most positive and hopeful one.
P.S. Her RBC was at 21 when she was admitted, dropped to 17 in the evening and was at 10 when she received the blood transfusion.
Hi Allison,
I am glad you were able to get your pup evaluated and treatment started so quickly. I know how scary and uncertain things must be right now. I did not see any information in the literature that would suggest a difference in outcome based on the age of the dog at onset of IMHA. I hope your sweet girl is stable and adjusting to her medications. Feel free to update us if you get a chance. Praying for a complete recovery!
My dog Frankie (9 1/2, 50 pounds, mixed rescue) was diagnosed with IMHA on Tuesday April 26th 2022. It came on suddenly Tuesday morning-she was lethargic, wouldn’t eat and not herself (just the day before she was full of energy and chasing squirrels in backyard). My mobile Vet has Covid so I took her to VCA emergency. Her red blood count 31%, her white blood cell was high, chest x-ray clear, ultrasound clear except her spleen looked a bit textured? which they thought could be from working hard to create red blood cells. High billirubin, dark urine. By 8pm her red count was down to 22% and was static till Wednesday morning but her vitals were good. It went down again Wednesday afternoon and was static until Thursday morning (this morning) when it dropped to 14% and they told my husband and I to come visit before the Blood Transfusion.
She was weak but I was relieved to see she was very much still herself, she wagged her tail and licked my face and was very happy to be with me. Her spirit was strong. She is getting her first blood transfusion as I type this and we are very anxious.
The clinic just sent over information about the Human Immune Globulin (Privigen) 50mLVl transfusion. Saying it might be the next step. It is very expensive, crazy expensive. But man, seeing her this morning- still vital and hopeful and wanting to come home. Is this treatment the thing that could bring her home? How long after a blood transfusion till she feels better and the medicine can do it’s job?
Hi Bonnie,
I am glad you were able to get Frankie to the emergency clinic and treatment started so quickly. In my experience, dogs usually feel much better within hours of getting a blood transfusion as long as their blood count stabilizes. It sounds like Frankie is fighting and giving this disease everything she has to pull through. I hope she is doing well and back home with you resting peacefully. Feel free to leave us an update if you have the time. Wishing you both the best.
My dog got the IMHA diagnosis on Friday with around 22% hct. They told us it wasn’t severe enough for a transfusion so they sent us home with cortisone and antibiotics since they also found out he had some unknown infection. His condition kept getting worse and we took him back today, 2 days later, and they told us his hct was down to around 8% and that he needed a blood transfusion immediately. After the transfusion he seemed much better and the vet told us he was at 14.5% hct and that we was good to go rest at home. The vet injected him with cortisone and told us to give him half a pill tonight.
We’ve now been home for about three hours and his condition has drastically worsened since we got home. His gums are pale again and he’s struggling with standing. My issue is that the vet told us that if this transfusion didn’t work and he didn’t stabilise after it, it would be pointless trying again. Is this opinion correct? I’m afraid to bring him back to the vet in case she’s going to tell us to put him down if we have other options.
Dear Bea,
I am sorry your boy is struggling and seems to be declining so rapidly. It sounds like he is critical and needs emergency attention again. I understand wanting to find a solution to help restore your pup’s quality of life and give him more time. Unfortunately, there is a risk that your dog may not respond to the blood transfusion even if it is repeated. Also, with each subsequent transfusion, you risk having a life-threatening reaction to the transfusion itself. With that being said, ultimately you have the right to ask for another transfusion if you want to pursue further treatment. As I type this response, I am wondering how things turned out yesterday and praying you still have your sweet boy with you. I hope you were able to get him stabilized and keep fighting this battle. If you have time, feel free to leave an update. Bless you both. ♥
I’m surprised to read that you say if he didn’t respond to one transfusion he likely won’t respond to a second. In your article you state that most dogs need at least one transfusion which leads me to believe it’s common for them to have more than one. I’m asking because my dog is currently receiving his second transfusion as I type this.
Dear Andrea,
Thank you for calling this to my attention! I reviewed the previous comment and response and realized my error. While it is common to need several blood transfusions for IMHA it is not the same for other conditions that can require blood transfusions. I have edited my response as to prevent any further confusion. I apologize and hope your dog is stable and in the recovery process. Praying all is well today. ♥
My 8 year-old mini schnauzer was just diagnosed with IMHA today. However, her presentation was described by the vet as unusual. Rewind 2 weeks ago, our girl was not acting like herself, not eating and laying around alot. We took her to the vet and her labs showed HCT 24.9, HgB 7.5, MCHC 30.1, RBC 3.3, MCV 73.7, RDW 22.2, MPV 19.9, Retic Hgb 25.7, and ALKP of 1079. The vet (covering for her normal vet) felt she may have a gastric ulceration, but her stool also showed small amount of a bacteria…. not sure which. They gave her an iron and vit b12 injection and sent her home on Metronidazole, Sucralfate, omeprazole, and Cerenia. She did not really improve over the following week, so we took her back and they did more blood work, x-ray, and ultrasound. Her pancreas and spleen were inflamed and enlarged on ultrasound, and she was constipated. The vet (her regular vet) felt she had pancreatitis at that point and hospitalized her for IV fluids and meds to treat the above, as well as enema and meds to correct constipation. She stayed 2 days in animal hospital and was discharged home on Sucralfate, Famotidine, and Reglan. She was better for a few days and then regressed, they then had us bring her in for steroid shot and prescription for oral steroids, thinking this was needed to reduce inflammation in pancreas. Things did not really improve, so we took her back today and blood work revealed worsening anemia (HCT 20, HGB 6.5), ALKP (1700), elevated WBC, and I believe the vet said her bilirubin was elevated and possibly low platelets. She said her labs did show functioning bone marrow. She was suspicious of a splenic tumor, but ultrasound of spleen, pancreas, liver, and heart did not reveal any tumors or cardiac concerns. She checked for heartworms, Anaplasma, Ehrlicia, and Lyme. She also mentioned doing a blood smear. To be honest, I was so overwhelmed with everything, I know I am not remembering all the things she tested or mentioned. However, she feels at this point all signs point to IMHA, but does not think she needs a transfusion based on her clinical presentation. She gave her another shot of iron dextran, and sent us home on oral Prednisone 10 mg. twice daily, Mycophenolate 125 mg. twice daily, and wants us to continue the Sucralfate, Famotidine, and Reglan. In addition, we are to maintain a low carb diet, as her glucose is already elevated by the steroids she was on, now the dose is doubled. From all the research I have done this afternoon, I am somewhat concerned about her not being on something to prevent clots, as this seems to be universal. Would it be possible her platelets were too low for this? I am going to reach out to the vet Monday to ask, but did not know if anyone here had insight or felt like this is something I should not wait until Monday to address. To be honest, I am so scared, as she already gets very short of air with little activity and seems to breathe heavy with anything she does, even laying down. Sorry for the long post, I am just very worried and looking for any input from others who have been through this.
Hi Heather,
I am sorry your Schnauzer girl is dealing with such a difficult disease process. I understand your concern and worry for her wellbeing. It sounds like you have a good partnership with your veterinarian, and they are being quite thorough with their diagnostics and treatment plan. It is very possible they are waiting for the platelet count to increase before starting an anticoagulant medication. I hope you were able to talk to your vet today and discuss your concerns. Don’t forget you can always schedule a consult with a veterinary internal medicine specialist. They have a great deal of experience with complicated cases and may have access to testing or treatments that can be cost prohibitive in general practice. Praying your sweet girl is able to remain stable and live a long and happy life. Wishing you both the best!
Our dog is 12 years old and was recently diagnosed with IMHA. She had to have a blood transfusion because her Hct went down to 14%. The Hct went down to 20 even after the transfusion, but then went up to 25%. We were hoping that was a good sign and that it would continue to go up, but it had only been holding steady for about a week and a half. The vet now wants to start her on Cylclosporine to help suppress her immune system. I’m a little concerned because he wants to start her on 50 mg/ twice a day. She is only about 13 lbs. Everything I can find says her dosage should be 25 mg/day. I know that the drug is usually prescribed for skin problems and might need a higher dose for IMHA, but that seems very high to me. Do you know if 100 mg/day for that size dog is ok? Thank you.
Hi Kory,
I am glad to hear that your dog seems to be stabilizing since the blood transfusion. I understand how scary it can be to think about giving your pup a medication that will suppress her immune system. Since I haven’t examined her myself, I can’t make specific suggestions about medications dosages. It sounds like you have a good working relationship with your current veterinarian. I recommend you talk to your vet and discuss your concerns. They can let you know if the cyclosporine dosage is increased and why they feel this dosage is needed at this time. I hope your girl continues to improve. Wishing you both many happy days ahead.
My girl took about a solid month to really start seeming herself again. There will be ups and downs. But with close monitoring, there is hope
My 3 year old Australian shepherd, Beau, was diagnosed with IMHA June, 2021. It was the scariest experience of my life. I noticed he was lethargic, not eating as much, and had pale gums. I’m so grateful an emergency vet in my area was able to see him immediately. His hematocrit was low, and at first they suspected IMHA, but his blood slide looked normal. The next day I took him back, they did more bloodwork and his blood cells were ‘sticky’ this time. They made the definitive diagnosis of IMHA that day. He was sent home with me and started prednisone, mycophenolate and clopidogrel. A few days later, he collapsed going down the stairs and had trouble using his back end. He had a blood clot in his back leg. My boyfriend and I literally rearranged our lives and our house at this point, to help him still do the things he loved in what we thought would be his last days. We were so fearful of the IMHA diagnosis and concerned the blood clot would not break up, or more would form.
Today, Beau is doing great! His blood clot broke up, his hematocrit is back to normal levels and he is back to his crazy, spunky self. He has been able to get off the prednisone and clopidogrel. We are now slowly weaning him off the mycophenolate. I am so grateful that it was caught so quickly and he never needed to spend a night in the hospital or have a blood transfusion. I am also grateful for his amazing vets who helped Beau and our family through these trying times. I have finally come to terms with his diagnosis and have been sharing his story trying to raise awareness. It is definitely a roller coaster ride filled with uncertainties. I always have the fear of a relapse in the back of my mind.
Thank you for sharing this article. You explained this disease in easy to understand terms, which is so important for parents whose pets have this disease, and to spread awareness. I wish no pets or pet parents would have to go through this and am hoping for more positive outcomes and research to be done on IMHA in the future.
Best,
Amanda & Beau
Hi Amanda,
Thank you for the kind words about the article. I am so glad Beau is doing great and weaning off his medications! I really appreciate you sharing Beau’s story and your experience with our readers. I pray you never have to experience a relapse and that you and your sweet boy have many happy years ahead to make wonderful memories. ♥
Hi. My dog was just diagnosed on Thursday. I was able to bring him home after his diagnosis with meds. He spent a few hours at the vet. But he’s still lethargic and weak. I’m very worried. How long did your dog take to start showing signs of major improvement
My dog was just diagnosed with IMHA. Currently he is in the hospital at a really good veterinary hospital in DC. So far his hematocrit has dropped no lower than 16.9. He is on prednisone and an immuno suppressant and doxycycline he has been admitted to the hospital for the third day as of today with the hopes that maybe coming home tomorrow. So far he has had two blood transfusions. Looking tomorrow to see what the results of his bloodwork are after this transfusion and maybe come home. I miss him so much he hasn’t been home in three days and I haven’t slept in three days. I just need to read about dogs that have survived this to give me hope. I need him to come home. I need to you and cuddle with him and help him through this. I’m really devastated but I got a stay strong.
Hi Shelly,
I am glad to hear your sweet boy is hanging in there and seems to be stable. I understand how worried you must be for him and how badly you want him home with you. Know that you are doing everything you can and that he is in good hands. My heart goes out to you as you navigate this difficult and uncertain future. I hope everything continues to go smoothly and that your boy will be back to his normal happy self very soon. I wish you both the best and keep us updated. ♥