Did you know that some form of dental disease in dogs affects 80% of our beloved canine companions by the age of two years? Integrative veterinarian, Dr. Julie Buzby, teams up with veterinary dental specialist, Dr. Heidi Lobprise, to explain the causes, treatment, and prevention of dental disease (i.e. periodontal disease in dogs).

To understand dental disease in dogs, let’s take a look at the story of Minnie, one of Dr. Lobprise’s patients in her veterinary dental specialty practice. This adorable, middle-aged small breed pup was beloved by her parents, the Johnsons. They ensured she was up-to-date on her vaccinations, received regular heartworm and intestinal parasite prevention, and was taken to the groomers at least monthly for her spa day.
In fact, the groomer brushed Minnie’s teeth at each visit. Plus, the Johnsons had Minnie’s teeth scaled twice a year at a place that offered anesthesia-free dental cleanings. They thought they were doing the right things for her dental health. After all, her teeth looked a lot better after these cleanings, and they didn’t have to worry about her going under anesthesia.
However, even after these efforts and giving Minnie dental treats, the Johnsons noticed that Minnie still had bad breath. So they took Minnie to their veterinarian for a check-up. There they learned something that took them by surprise—while the surfaces of the teeth looked fairly clean, Minnie had significant dental disease (i.e. periodontal disease), much of which was hidden below the gum line.
Why take dental disease seriously?
Before we go any further, I want to explain the three reasons dental disease and dental care should matter to all dog parents.
- By the age of two, 80% of dogs have some degree of periodontal disease. Sadly, it is “the norm.”
- Dental disease in dogs and cats can be painful and debilitating. If you’ve ever experienced a tooth abscess or chronic mouth pain, you know that this may be a fate worse than death.
- Dental disease is generally preventable and treatable.
What is dental disease in dogs?
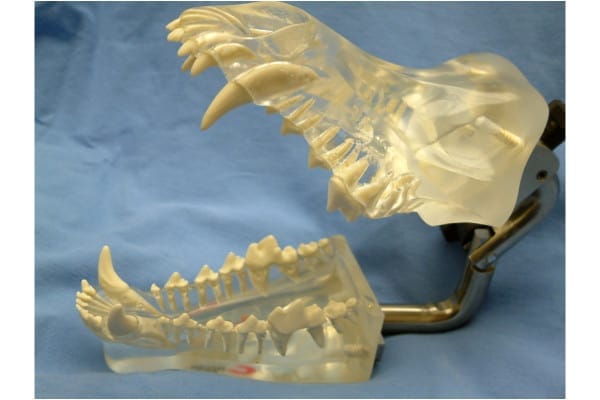
First of all, let’s get a better picture of a dog’s teeth. The general anatomy of dog teeth is similar to human teeth. The teeth are anchored in place by a group of supporting structures—gum tissue, ligaments, and bone—called the “periodontium.” When these tissues become inflamed, the term periodontal disease (i.e. dental disease) may be used. Because the periodontium’s function is to hold the teeth in position, periodontal disease can lead to tooth root exposure, tooth loss, and bone loss. This is in addition to gum recession and gingivitis.
You’ve probably heard the term gingivitis on a television commercial about human oral health. We think of it as gum disease. The “gingiva” is the gum tissue, and “gingivitis” means inflammation of that gum tissue. (The suffix “itis” in a word, generally indicates inflammation.) Gingivitis represents the early stage of periodontitis (i.e. inflammation of the periodontium). Here is the good news: Gingivitis is reversible. However, if you do nothing to address gingivitis, periodontal disease will continue to progress.
How does periodontal disease occur?
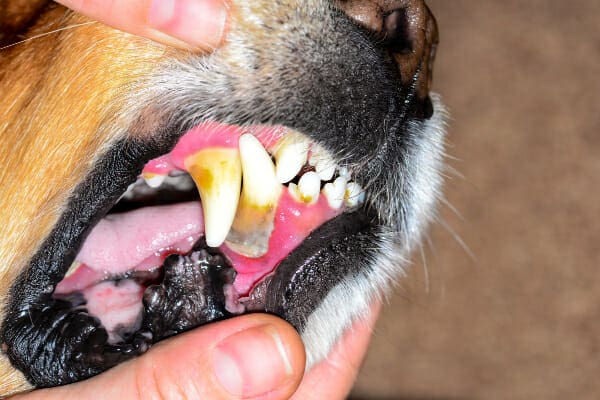
First plaque—that soft, slimy stuff you feel on your teeth when you wake up—starts forming on the teeth. Bacteria make up part of the plaque, along with salivary proteins and food material. If you brush the plaque off, that can prevent any infection or inflammation. However, if the plaque stays on the teeth, minerals from the saliva harden it into tartar, which is firmly attached and can’t be brushed off.
Periodontal disease progresses from there when the bacteria, and even the immune system of the dog causes infection, inflammation, and eventual destruction of gum tissue and bone. This destruction often results in periodontal pockets (i.e. gaps between the tooth and the gums or bone) below the gum line. Since much of this damage is below the gum line, it makes sense that an anesthesia-free dental cleaning does nothing to address the “root” of the problem.
What are the stages of periodontal (dental) disease?
The degree of dental disease that dogs can present varies widely. In fact, there are stages of periodontal disease, each with a different prognosis (expected outcome). Gingivitis represents stage 1. Stage 2 through 4 are categorized based on the degree of bone loss or periodontium detachment. Since only the surface of a tooth can be seen on an awake dog, periodontal disease staging is best performed under general anesthesia with the use of dental probing and dental X-rays.
- Stage 1: gingivitis
- Stage 2: early periodontal disease (less than 25% loss of attachment)
- Stage 3: established periodontal disease (25-50% attachment loss)
- Stage 4: advanced periodontal disease (more than 50% loss of attachment)
What are the symptoms of dental disease?
As periodontal disease progresses, you may notice the following signs:
- Bad breath (a result of the bacteria in the mouth)
- Pawing at the face (often one of the signs your dog is in pain)
- Reluctance to open the mouth/resistance to being touched around the face (more indicators of pain)
- Changes in the way the dog eats/chews food (i.e. chewing predominantly on one side; dropping food from the mouth, etc.)
- Decreased appetite/weight loss
- Swelling underneath the eye (a sign of a dog tooth abscess)
- Sneezing or asymmetrical nasal discharge
- Swelling around the mouth/face/eyes
- Drainage from the mouth (saliva, blood, pus)
- Swollen lymph nodes in the neck or behind the jaw
- Dog losing teeth
How is dental disease in dogs treated?
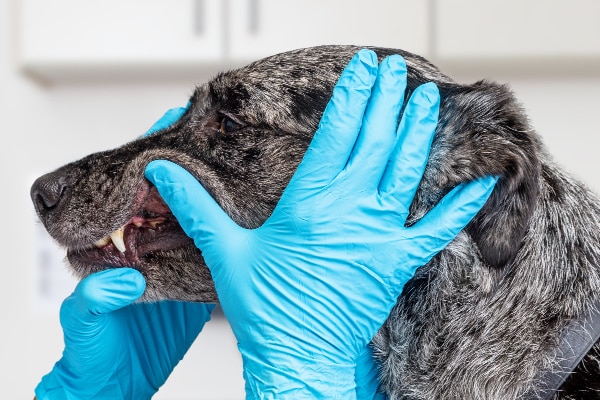
First, your vet will start with an awake oral exam. Then if he or she feels that your dog’s dental disease is significant enough to require professional care (rather than at-home dental care), a dental procedure under anesthesia is generally the next step. General practice vets commonly perform dental procedures, but there are cases (as you will see with Minnie) when they may recommend referral to a veterinary dentist.
Your vet (or veterinary dentist) will likely provide you an estimate of the cost. Please be aware, though, that the vet often cannot assess the full extent of the damage under the gum line until your dog is under anesthesia. This is why the actual procedure cost could vary from the estimate.
Professional dental care for pets can be very expensive but is priceless in terms of the benefit it provides your dog. Both Dr. Lobprise and Dr. Buzby have seen countless dogs’ lives transformed when the pain and inflammation is resolved through a complete dental procedure.
To give you an idea of what to expect during a dental procedure, let’s go back to Minnie’s story. While each dog’s situation may be a bit different, learning how Dr. Lobprise addressed Minnie’s dental disease can help put your mind at ease if your dog is facing a dental procedure. As always, talking to your vet (or veterinary dentist) about your concerns is a good idea, especially if you are wondering, “Is my dog too old for anesthesia?” or “Is my dog too old for surgery?“
Minnie’s referral to a veterinary dentist
Minnie’s regular veterinarian recommended a complete dental procedure to fully evaluate the teeth, take dental X-rays, do deep cleaning, and extract or treat diseased teeth. The vet explained that this must be completed under general anesthesia because an awake dog wouldn’t tolerate these procedures, and it wouldn’t be fair to expect him or her to do so.
While the Johnsons were concerned about needing to use general anesthesia, their veterinarian did a thorough physical exam (including listening to the heart) and pre-operative blood work to look for any underlying health issues. With a clean bill of health, Minnie’s parents now felt more confident about scheduling a dental procedure.
Due to Minnie’s age and the likelihood that she would need several extractions, her veterinarian had given her parents the option of going to a board-certified veterinary dentist (Dr. Lobprise in this case) for her care. Small dogs like Minnie have limited amounts of jaw bone and often crowded teeth. This means periodontal disease can be a big issue for them. Sometimes the bone loss from periodontal disease can result in a fractured jaw, especially in the region of the large lower first molar. All these factors make dental procedures in small breed dogs more challenging.
A board-certified veterinary dentist has extensive experience in periodontal disease treatment and extractions. This allows him or her to not only provide optimal care, but also do it more quickly than most general practitioners. In a small breed dog with significant periodontal disease like Minnie, this can be quite advantageous.

Step 1: An awake oral exam
When you take your dog for an appointment with your veterinarian or a veterinary dentist, you can expect that he or she will first examine your dog’s mouth while your dog is awake.
The goal during this part of the exam is to inspect the patient’s teeth, lips, and gums first. Then the vet will gently open the mouth to look at the tongue, roof of the mouth, and the back of the throat. (Some dogs are more compliant than others.) All of this can be done in a matter of seconds, which is good because patients do not just cooperatively open wide and say, “Ah!”
PRO TIP: Training your dog to cooperate for having his or her mouth opened is a valuable asset during veterinary exams, and also when administering medications and performing home dental care.
When Dr. Lobprise examined Minnie’s teeth, she noticed that the crowns (i.e. visible surface of teeth) did look fairly clean. However, she could see indications of periodontal disease like reddened, inflamed gum tissue due to bacterial infection, and even one or two teeth that looked discolored. Sometimes a discolored tooth can indicate that the inner contents (i.e. the pulp and nerve) might be dead. The blood supply (part of the pulp) and nerve need to stay alive to keep the tooth healthy. Otherwise the tooth is at risk for infection and abscess formation.

Step 2: Complete dental procedure under general anesthesia
In general, a dental procedure at a veterinarian’s office should include the following:
- General anesthesia
- Dental X-ray
- Scaling (cleaning) and polishing of the teeth
- Potential extractions (if necessary)
Preparation for anesthesia
Prior to anesthesia, Dr. Lobprise thoroughly examined Minnie, looked at her bloodwork, and determined that she would be a good candidate for anesthesia. To help put Minnie’s parents’ minds at ease about the anesthesia, Dr. Lobprise discussed the care that Minnie would receive:
- Pre-anesthetic sedation and pain injections.
- IV catheter for intravenous fluids to keep her hydrated.
- An endotracheal tube placed in her windpipe to administer oxygen and anesthetic gases as well as to prevent any fluid or bits of tarter from getting into her lungs.
- Careful monitoring while under anesthesia and during the recovery period. The veterinary nurse assigned to monitor anesthesia uses specialized equipment to track blood pressure, heart rate, ECG, respiratory rate, blood oxygen levels, and body temperature.
- A warming blanket or other warming device to help maintain body temperature.
Evaluation of the teeth, gums, and bone
Once Minnie was under anesthesia and stable, Dr. Lobprise thoroughly examined the entire oral cavity. She used a periodontal probe (marked in millimeters) to look for periodontal pockets (i.e. gaps in between the teeth and gums or bone where there has been periodontal destruction). The veterinary dental team also took Minnie’s dental X-rays. Unfortunately, these tests revealed Minnie needed at least 14 extractions!
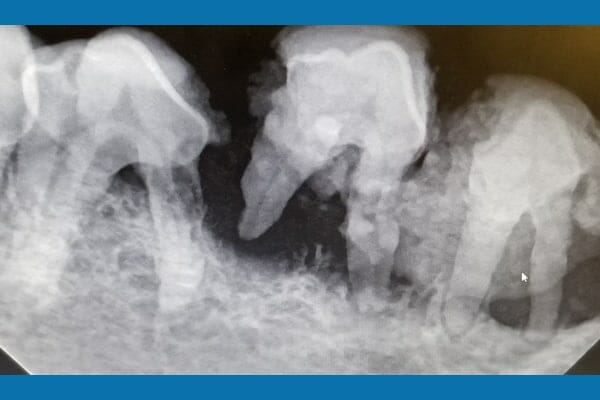
The gum loss found during the exam and probing and the bone loss found on dental X-rays showed a lot of hidden tissue destruction that couldn’t be seen when Minnie was awake. If this tissue loss is minor, the veterinary dentist can do some deep cleaning called root planing. However, once supportive tissue loss exceeds 50% around a tooth, the tooth is no longer stable and needs to be extracted. Otherwise, the infection and bone loss can continue and the jaw may become unstable.
Communication with dog parents
Dr. Lobprise typically calls the dog parents at this point to give them the updated treatment plan. In Minnie’s case, she let them know ahead of time that this update will often involve more extensive work than what can be guessed from the awake oral exam. Understandably, Minnie’s parents were concerned about the extensiveness of the periodontal disease, how Minnie would handle the oral surgery, and of course the additional costs. They were also worried about how she would eat after all those teeth were gone.
Dr. Lobprise assured them that removing this chronic infection was not only the best thing to do for Minnie’s mouth, but for the rest of the body as well. It has been shown that the presence of untreated periodontal disease is associated with heart, lung, liver, and kidney problems. Plus, the long-lasting inflammation has long-term effects on general health and the immune system.
Extraction of diseased teeth
The dental team had already placed local blocks (numbing injections), so Minnie would feel no pain, even under anesthesia. (This is similar to what your dentist might do if you need dental work.) The local blocks allow the veterinary team to keep the general anesthesia as low as possible. Additionally, they provide pain relief for the patient for several to many hours after the treatment.
Dr. Lobprise proceeded with the tooth extractions, taking great care with the lower jaw where the bone loss was critical. Then the veterinary team took post-operative X-rays to ensure Dr. Lobprise had gotten all of the roots out safely. Finally, Dr. Lobprise closed the gum tissue with sutures that dissolve on their own.
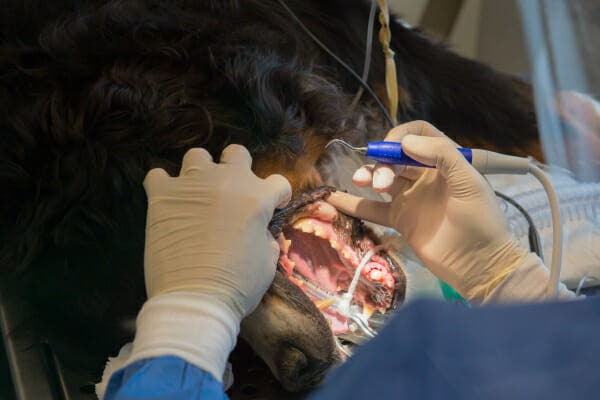
Recovery from anesthesia
After a final check to ensure all tartar was cleaned off and the teeth were polished, the veterinary team started the recovery process. A veterinary nurse stayed close to Minnie and continued to monitor her vital signs. Once Minnie was awake enough to cough and swallow, the vet nurse removed her endotracheal (i.e. breathing) tube. Some patients need additional fluids in recovery, but Minnie wasn’t one of them. Since she was doing so well, the vet nurse transferred Minnie to her recovery suite but continued to monitor her.
Continued recovery at home
The veterinary team called her parents to let them know the procedure had gone smoothly and Minnie was waking up well in recovery. The team let Minnie’s parents know that Dr. Lobprise usually likes to keep her patients at least two hours post-recovery. This allows the veterinary team to ensure there are no complications and that the patient is awake enough to be discharged.
Though a little groggy, Minnie was happy to see her parents when they picked her up. The veterinary team sent Minnie’s parents home with a list of comprehensive recovery instructions for that evening and the following days. It covered all the common dog parent concerns, including pain medication administration and softening the food due to the sutures.
When the dental team called Minnie’s parents the next day, they learned that Minnie had been really sleepy the night before and only ate and drank a little bit. However, Minnie’s parents were happy to report that she had already perked up that morning. She had eaten her softened breakfast, gone the bathroom as usual, and was even jumping around a bit.

Two weeks later when Minnie came in for her recheck, her parents were ecstatic to inform Dr. Lobprise that she was feeling so much better. They said she was like a new dog!
As an aside, this is not the first time Dr. Lobprise has heard this kind of news. In fact, both Dr. Buzby and Dr. Lobprise report that it’s one of their favorite parts of dental patient care.
Dental care really does change lives!
Why can’t my dog have an “anesthesia-free dental cleaning” instead?
It’s important to point out that a dental procedure under anesthesia should not be equated with a “gentle dental” or “anesthesia-free dental cleaning.” These controversial anesthesia-free dentals remove some of the plaque and tartar located on the visible part of the tooth (about 40% of the whole tooth). The teeth may look clean, but this just gives dog parents a false sense of security. As discussed earlier, the tartar and plaque cleaned off the tooth surfaces are literally just the tip of the iceberg when it comes to periodontal disease.
There is no good way to safely check periodontal pocket depth, do an extensive oral exam, take dental X-rays, or extract teeth on an awake dog. It doesn’t matter how well behaved or calm the dog is. He or she isn’t going to sit in a dentist chair and compliantly hold his or her mouth open like a person does.
As a result, an anesthesia-free dental really just addresses the visible problem. It cannot allow for thorough inspection and treatment of the area below the gum line where the bacteria that cause dental disease thrive. In other words, it does not adequately attack the root of the problem.
For the American Veterinary Dental College’s official position on anesthesia-free dentistry in pets, read Anesthesia-Free Dentistry: Know the Facts.
How can I prevent dental disease?
Unfortunately, the big player that determines your dog’s dental future is one that you have no control over—genetics.
Toy and small breed dogs are highly susceptible to dental disease, and large breed dogs are affected to a lesser degree. Your dog’s DNA not only dictates eye color and fur type, but it also dictates the health of your dog’s teeth starting from puppyhood.

Dental care strategies for dogs
However, we all know there is wisdom in focusing on what we can change and not what we can’t. Therefore, let’s focus on five critical things you can do to keep your dog’s mouth healthy:
- Schedule well care vet visits that include professional oral exams.
- Plan and budget for dental cleanings.
- Create a daily at-home dental care routine for your dog that includes teeth brushing. To learn how to brush your dog’s teeth at home, please read my article, Should I Brush My Dog’s Teeth: 7 Tips & How-To Video. (For your dog’s safety, keep in mind that the answer to the question “Can you use human toothpaste on dogs?” is a resounding “No!”)
- Talk to your vet about other dental products you can incorporate into your dog’s daily routine. Brushing your dog’s teeth is still the gold standard, but products from the Veterinary Oral Health Council (VOHC) Accepted Product List can add some fun and variety to your dog’s dental care. All products on this list have undergone extensive testing to ensure they are effective at reducing plaque and tartar. (Bear in mind, though, that VOHC makes no safety claims. It is still your responsibility to choose appropriate products for your dog’s size and chewing strength.)
- Select safe chew toys for your dog that are unlikely to cause tooth fractures. For Dr. Buzby’s veterinarian-recommended tips, read Safe Chew Toys for Dogs and Are Antlers Safe for Dogs? 3 Reasons to “Chews” No.
The importance of your role in the care of your dog’s teeth can’t be emphasize enough. As your dog’s biggest advocate, you can help your dog by taking the steps outlined above to prevent dental disease.
Finding the pearly white lining
If your canine companion is part of the 80% of dogs who have some form of periodontal disease by the age of two, take heart. There are solutions!
Please talk with your veterinarian about the causes, prevention, and treatment options for your beloved dog. And do not delay. Your dog is counting on you to get to the root of better dental health.


Has your dog had a professional dental procedure with your veterinarian?
If so, what was your experience?


All you need to do is realize what your own mouth would feel and smell like if you hadn’t had your teeth brushed in years to understand the gravity of not caring for your dog or cat’s teeth! Teaching pet health and safety, I hear from many what a different it made in their pet’s life, to get a thorough cleaning. Dogs that were just written off as “old” have become puppy-like again. They are finally able to get nutrition and not be in pain. A toothache can make a human grouchy, so you know it can for your best furry pal as well. There are many types of paste and oral care, so find what works best for your pet and you. Remember, just like not letting our pets get overweight, ensuring a healthy mouth is truly OUR responsibility! Thanks Dr. Julie for all this GRRReat info!
Amen and amen! Thanks for sharing this wisdom, Denise!