If your senior dog was recently diagnosed with vacuolar hepatopathy in dogs, you may have a variety of questions and concerns. Integrative veterinarian Dr. Julie Buzby is here to help. She explains what vacuolar hepatopathy is, common causes, symptoms, diagnosis, treatment, and outlook to help put your mind at ease.

Your dog’s liver is one of the most important organs in his or her body. While perhaps less exciting sounding than other internal organs—like the heart that pumps every minute of every day—the liver has many roles when it comes to maintaining overall pet health. The liver does all of the following:
- Produces bile in order to digest food and convert fats into usable energy.
- Helps break down and remove harmful toxic substances from the body.
- Creates and stores a special version of glucose called glycogen for later use when needed.
- Generates proteins that are necessary for blood clotting and keeping fluid in the blood vessels.
- Houses “first responder” cells that work for the immune system.
- Stores necessary vitamins and minerals.
Certain diseases or conditions can inhibit the liver’s ability to work properly. Parts of the liver can become infected or inflamed in a variety of situations, which may result in problems at a cellular level. One particular liver disease that affects the inside of liver cells is called vacuolar hepatopathy.
What is vacuolar hepatopathy in dogs?
Vacuolar hepatopathy (VH) is a condition that affects hepatocytes, which are cells that make up the liver. Small spaces or holes known as vacuoles develop inside the cytoplasm (i.e. jelly-like liquid inside cells). Vacuoles can form from cellular damage or other insults. They may contain air, water, fat (lipids), or a stored form of glucose called glycogen.
What are the complications of vacuolar hepatopathy?
Physical injury or the presence of toxins can damage the hepatocytes. As a result, the cells may become swollen or vacuolated. It may take days or weeks for these types of injuries to heal if they do heal at all. Some hepatocellular damage can lead to permanent changes in the liver. This result in chronic inflammation and other changes such as:
- Hepatic nodules—These benign, cyst-like growths occur inside liver tissue. They may result from chronic insults to the liver. The term “nodular hyperplasia” describes hepatic nodules that result from an overgrowth of vacuolated hepatocytes.
- Portosystemic shunts – Sometimes due to VH, the body forms abnormal blood vessels that create a connection between the liver’s blood supply (i.e. the portal vascular system) and the blood supply to the rest of the body (i.e. systemic circulation). Normally, these two blood supplies are separate.
- Portal hypertension—VH may lead to elevated blood pressure inside the portal vascular system of the liver. It may be a result of chronic scarring (cirrhosis) of the liver and may lead to gastrointestinal bleeding or free fluid in the abdomen called ascites.
- Hepatocellular carcinoma—Scottish Terriers seem to be prone to developing VH. In this breed especially, VH may increase the risk of hepatocellular carcinoma, a type of liver cancer.
What causes vacuolar hepatopathy?
In general, veterinarians break the causes of VH into three categories:

Steroid-induced VH
A dog’s adrenal glands normally produce very small amounts of a certain type of steroids called glucocorticoids (i.e. cortisol). These adrenal steroids help regulate glucose levels in the body. This is a very good and necessary thing when glucocorticoid levels are normal. However, increased levels of steroids can increase glycogen production and therefore glycogen deposition in vacuoles in liver cells.
Chronic use of steroid medications like prednisone for dogs is one of the most common causes of vacuolar hepatopathy. In a study published in the Journal of the American Veterinary Medical Association looking at 336 dogs with vacuolar hepatopathy, 55% of the dogs had been taking steroids. Additionally, steroid-induced VH may also occur in Cushing’s disease in dogs. This is because overproduction of glucocorticoids by the adrenal glands is the hallmark of Cushing’s disease. In the same study of 336 dogs with VH, 11.8% of them had Cushing’s disease.
Secondary VH
VH also can develop as a result of other disease processes. Dogs with diabetes mellitus or hypothyroidism in dogs are more likely to have excess lipids in their blood. This increases the risk of hepatocytes developing vacuoles filled with lipid.
VH has also been associated with chronic disease conditions such as:
- Cancer (including lymphoma in dogs and liver cancer in dogs)
- Immune mediated diseases (such as immune mediated hemolytic anemia or IBD in dogs)
- Neurologic conditions (including IVDD in dogs or degenerative myelopathy in dogs)
- Heart disease in dogs
- Kidney disease in dogs
- Hepatitis (i.e. liver inflammation) or other causes of liver disease in dogs
In some cases, researchers think that VH may be a result of dogs with chronic illnesses being under stress. The body naturally increases the release of cortisol from the adrenal glands during times of stress as part of the “fight or flight” response. Since cortisol is a steroid hormone, too much cortisol from chronic stress can cause vacuolar hepatopathy in the same way that excess steroid medication usage and Cushing’s disease can.
Idiopathic VH
There are some occasions where the cause of VH is unknown (i.e. idiopathic). Scientists have proposed that steroid hormones like progesterone may play a role in development but have not definitively proven that hypothesis yet. It seems that Scottish Terriers may have an increased risk of developing idiopathic VH.

Which dogs tend to have vacuolar hepatopathy?
Typically, VH is more common in middle aged to older dogs with the median age being nine years. One study indicated it may occur more often in female dogs. As previously mentioned, Scottish Terriers are at increased risk.
What are the symptoms of vacuolar hepatopathy?
There are many dogs with VH who don’t display any clinical signs. And any symptoms that are present tend to be more commonly related to the underlying cause of the VH. In certain cases, particularly if diabetes or Cushing’s disease are present, dogs may have an increase in thirst, an increase in urination, and an increase in appetite. Similar signs may occur in dogs who are taking steroids.
Long-term use of steroids or increased levels of cortisol in the blood can eventually weaken muscles so that the abdominal body wall takes on a rounded or “pot-bellied” appearance. Dogs with vacuolar hepatopathy may also pant more and have a thin hair coat.
How is vacuolar hepatopathy diagnosed?
Your veterinarian may suspect that there is a liver issue if your dog has any of the clinical signs or risk factors associated with vacuolar hepatopathy. Sometimes, the vet notices he or she can palpate the borders of the liver during a physical exam. This suggests that there may be liver enlargement as the liver edges are not normally palpable in most dogs.
The vet may also decide to run routine blood work to look for elevations in liver enzymes. Dogs with VH may have marked increases in alkaline phosphatase (ALP). Other liver enzymes like alanine aminotransaminase (ALT) and gamma-glutamyl transferase (GGT) may be normal or show mild increases. Since other factors can explain an increase in ALP (i.e. dental disease, certain medications, bone disorders, and other liver conditions), your vet may discuss additional testing with you.
This may include X-rays and an abdominal ultrasound to look for further evidence of hepatic disease. This imaging can show evidence of liver enlargement and any changes to the overall architecture of the liver lobes. For example, ultrasound may reveal a “Swiss cheese pattern” to the liver that may indicate vacuolar hepatopathy.
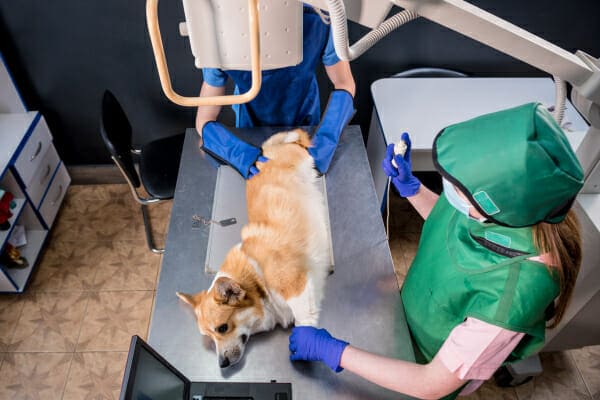
Using a liver biopsy to confirm VH
Definitive diagnosis of VH requires a liver biopsy under deep sedation or general anesthesia. In some cases, the vet may use an ultrasound to guide the biopsy collection. One option is to perform a fine needle aspirate (i.e. use a small needle and syringe to gather a collection of cells). This is an inferior method to using a specialized needle called a Tru-Cut biopsy needle. The FNA only gets a small sample while the Tru-Cut can collect a larger sample. Having more cells from a Tru-Cut biopsy may yield more accurate test results.
In other cases, a vet may decide to either collect the samples laparoscopically or during an abdominal surgery. While these methods are more invasive than an ultrasound-guided biopsy, they also provide excellent samples and better control over what portions of the liver the vet samples.
What is the treatment for vacuolar hepatopathy?
There is no specific treatment or cure for dogs with vacuolar hepatopathy. However, controlling any concurrent diseases is a great place to start. Addressing diabetes, Cushing’s disease, or other conditions often helps decrease the symptoms of VH. Dogs with diabetes usually need to receive insulin injections and must have a tightly-controlled diet regimen. For dogs with Cushing’s disease, they may respond to medications like trilostane or mitotane that suppress excess release of cortisol.
If the dog has been taking steroids, gradually weaning him or her off of them is ideal. Often, but not always, your vet will be able to find a different medication that can take the place of the steroids.
In general, nutritional support is usually the main focus of therapy. Diets that are rich in antioxidants can help support the liver. Additionally, supplements such as Denamarin® containing S-adenosyl-L-methionine (SAMe) will amplify the liver’s ability to repair itself.
Some dogs can benefit from ursodiol, a medication that helps with the flow of bile. To aid in digestion, the liver releases substances called bile acids into circulation. A healthy liver will take these bile acids back up, but a diseased liver will not. Ursodiol can prevent the build-up of toxic bile acids. It also is theorized that ursodiol may prevent damage to hepatocytes.

What is the outlook for dogs with vacuolar hepatopathy?
The good news about VH is that it is unlikely to directly impact the life expectancy or quality of life for most affected dogs. However, the specifics of the outlook depend on what the underlying cause might be.
For example, if your senior pup has VH secondary to diabetes, he or she may have a very good outcome as long as his or her diabetes is well controlled. Even better, if steroid usage was the cause, discontinuing the steroid may reverse VH altogether!
On the other hand, some dogs with VH, especially Scottish Terriers with idiopathic VH, will eventually progress to the point of having decreased liver function or occasionally develop liver cancer. Thankfully, that isn’t what happens in the majority of VH cases.
I understand it can be difficult and stressful anytime your dog is diagnosed with a medical condition. But if there was ever a “good” liver problem to have, it would be vacuolar hepatopathy. It isn’t life-threatening and typically won’t keep your dog from fully enjoying life. With quick intervention and good supportive care, you can minimize your canine companion’s clinical signs and continue to have a wonderful life together.
Has your dog been diagnosed with vacuolar hepatopathy?
Please comment below to share his or her story.


My dog was diagnosed with VH earlier this year.
Is it normal to see the liver enzymes, particularly ALT and ALP, continue to slowly rise with VH?
My dog’s ALT has been anywhere between 175-300 over the past year and ALP between 189-400 in that timeframe too. Over the past couple of months though, both ALT and ALP have been in the high 400s to low 500s. We have done a recent repeat ultrasound and it is about the same as it was at the beginning of the year and no concern for cancer.
Is a steady rise in enzymes normal progression of VH?
Also, is there any concern for dogs with VH to undergo general anesthesia?
Thank you,
Hi TJ,
These are great questions and I hope I can offer some insight. It is possible for the liver enzymes to steadily rise with VH. The areas of liver that are damaged by the cells containing the vacuoles can cause a progressive decline in liver function. Risks with general anesthesia will be greater in dogs with VH because the liver is the main organ that helps to metabolize (or clear out of the system) the drugs used to induce and maintain anesthesia. With all that being said, it would be a good idea to make sure other diseases, such as Cushing’s, have been thoroughly ruled out. Is your dog taking any supplements to help the liver heal? If not, I would recommend you talk to your vet about Denamarin as a possibility. I hope you can find the answers you need to help your sweet boy continue to live life to the fullest. Best wishes and good luck!
My 12 year old AST just got back ultrasound guided needle biopsy report. The cells were determined to by marked hepotocytic swelling and vaculization. Cushings and Atypical bushings ruled out and no evidence of diabetes. She has increased thirst, peeing, hair loss on her tail and less energy as day progresses. Good appetite as always. No hepatitis, inflammation, neoplasia seen. The mass is on the right lobe of her liver. this internist is now advising to do a CT scan and liver lobectomy. This whole process of trying to get a diagnosis has been very frustrating. Looking to see if there is something besides Denamarin which did not help her to support her liver. Her ALP was last 3005. No mass showed on her ultrasound 1.5 years ago when enzymes elevated to 1300. All other blood work is coming out in normal range. Any direction you can provide would be appreciated as I feel I am being led down a rabbit hole and all I want is to help her feel better. Thank you
Hi Debbie,
I understand your concern and frustration with this difficult process of obtaining a diagnosis. It sounds like your pup is a complicated case and your vet is working hard to unravel the details. While a needle aspirate/biopsy can give us a good idea of what is happening in the liver, the only way to get a definitive diagnosis is to get a larger sample for the pathologist to evaluate. Your vet may be worried the mass could be cancerous even though the cytology did not show any suspicious cells. If this is the case, then removing a portion of the liver may be the best next step. Ultimately, it is your decision how far to pursue this issue. If at any point you would rather focus on palliative care, please let your vet know and be honest with your feelings and expectations. Also, you may want to look into the services of a holistic veterinarian or one that practices Traditional Chinese Medicine. There may be options of herbs or other therapies to try that could help relieve some of your dog’s symptoms. I am hopeful you will find the best way to bring your girl comfort and minimize the worry and stress. Wishing you both the best of luck and keep us updated if you have a chance!
My dog has just been diagnosed today. We have been trying to figure out the problem. He has been in a lot of pain off and on and the pain is happening more frequently. I’m waiting for the vet to call me back to see where we go from here. I just wish I knew what to do to lessen his pain
Hi Nicloe,
I understand your concern with your dog’s uncontrolled pain. What is it that your pup was diagnosed with? The reason I ask is vacuolar hepatopathy does not cause pain, at least not that I am aware of. I do think you should talk to your vet and find out if additional testing needs to be performed. I hope you can find a treatment that works best for your dog and will resolve his issues. Best wishes.
Yes. She was. She is 14 yrs old and has been on and off steriods for yrs do to allergies. She has not had any steriods in a few month hoping this is the reason. She has no cushion and she is not a diabetic from what previous test show. She is on low fat gastro royal canin food and dermarin as of now. Returns to vet for blood work tomorrow. Keep her in your prayers
Hi Jamie,
I hope your appointment with your vet for the blood work went well today. Praying you can figure out the best way to help your sweet girl. Keep us updated!