Finding out your senior dog’s blood work showed a high ALP can be confusing and concerning. Thankfully, integrative veterinarian Dr. Julie Buzby is here to help you make sense of high ALP in dogs. She explains what it is, why it can sometimes be elevated, and what the next steps might be.

Sampson, a 12-year-old Jack Russell Terrier mix with a zest for chewing sticks and chasing squirrels, was in to visit me recently. During a particularly vigorous stick chewing session he had cracked a tooth. As a result, he needed a dental procedure under anesthesia to remove the damaged tooth and clean the rest of his teeth.
I always recommend some basic bloodwork prior to any of my older doggy patients going under general anesthesia. Pre-anesthetic lab work helps ensure a dog isn’t at an increased risk for complications with anesthesia or the specific procedure. It also has the added benefit of occasionally picking up on medical issues before they become a bigger problem. That was how we found that Sampson’s ALP, while normal on his last yearly bloodwork, was now moderately high.
Sampson’s dog mom, Sarah, was the proactive type and had many questions about ALP. I answered her questions in detail before we formulated a plan.
What is ALP in dogs?
The abbreviation “ALP” stands for alkaline phosphatase, which is an enzyme many routine blood panels may measure. Primarily, the liver produces ALP, though there are other sources too. We will come back to this later in the article because it is important.
Within the liver, ALP is found along the outer layer of the liver cells. Even more specifically, it is associated with the liver cells that line the bile ducts. Alkaline Phosphatase’s normal job in the body is complicated, and actually isn’t critical to understand here. But what is important to understand about ALP is that it is a sensitive indicator of liver or gallbladder dysfunction.
A brief physiology lesson
The liver is an amazing organ that has, by many estimates, over 500 critical jobs in the body. To name a few, the liver is responsible for:
- Removing toxins from the bloodstream
- Regulating blood sugar (along with the pancreas)
- Taking old red blood cells out of circulation
- Releasing clotting factors
The liver is also responsible for making bile, which flows through ducts in the liver to the gallbladder. Bile is then released from the gallbladder into the GI tract where it helps with digestion.

With all these important functions, it would only make sense that keeping tabs on your dog’s liver is an important part of keeping him or her healthy. This is where ALP liver enzymes (among other liver enzymes) comes in.
How would the vet detect high ALP levels in dogs?
When your veterinarian performs general wellness blood work on your dog, either as part of a yearly exam or as part of a pre-anesthetic check-up, chances are the blood work will include a chemistry panel. This test measures protein and electrolyte levels. It also includes values that can offer clues about the function of the liver, kidneys, and pancreas.
For a chemistry panel, the vet or vet nurse will draw a small amount of blood from your dog and place in a test tube. Then, your veterinarian may sometimes perform the blood tests with an in-house laboratory machine. Alternatively, he or she can send your dog’s blood to an outside veterinary diagnostic lab. If your veterinarian runs these tests in-house, your results may be ready the same day. But if your vet sends the blood out, it can take several days for the final results to be available.
Liver values
The markers related to the liver on a chemistry panel include ALP, ALT, GGT, and total bilirubin. The liver also makes glucose, cholesterol, albumin, and BUN. These levels can give clues to how well the liver is functioning.
ALT, or alanine transferase, is what is known as a “hepatocellular” liver enzyme. When the cells of the liver are damaged, this enzyme leaks out into the blood. Elevated ALT is often more worrisome than high ALP to veterinarians since it indicates ongoing damage to the liver cells.
ALP and GGT are what are known as “cholestatic” enzymes. This means that elevations predominantly occur if there are issues with the flow of bile, either within the liver, or as it leaves the gallbladder.
Forms of ALP
Earlier we touched on the fact that the liver makes alkaline phosphatase (ALP), but other places in the body make it too. The three most important forms are ALP from the liver (L-ALP), ALP made in the bone (B-ALP), and ALP that is released in response to excess levels of corticosteroids (C-ALP). A chemistry panel measures all three of these forms together as ALP. Therefore, based on the chemistry panel alone, it is not possible to determine which form is contributing most to an elevated ALP.
Liver ALP
As the name implies, L-ALP elevations are often related to issues with the liver. This is the focus of much of the rest of the article.
Bone ALP
Increased ALP activity is common in young dogs who are growing rapidly because normal bone growth releases B-ALP. Generally, these dogs are less than a year old. In a young dog, a mild elevation in ALP is not a worrisome finding if the remainder of the liver values are normal and the dog is otherwise feeling well. However, conditions that cause ongoing damage to the bones, such as bone cancer (i.e. osteosarcoma) or infections within the bone (i.e. osteomyelitis), can also cause elevations in B-ALP levels.

Corticosteroid ALP
The liver produces corticosteroid-induced ALP in response to elevated blood steroid levels. These high C-ALP levels can either be due to the body producing increased amounts of steroids, as with Cushing’s Disease in dogs, or they can be from oral or topical steroid-containing medications.
What causes high ALP in dogs?
Many times, a vet will find high ALP in senior dogs. In fact, it is one of the most common lab work abnormalities in older dogs. An elevated ALP is very sensitive in its ability to assess for hepatobiliary disease (i.e. diseases affecting the liver, gallbladder, or bile ducts) in dogs and cats.
This means that most dogs with significant liver disease will have an elevated ALP. That sounds like great news, right? If that’s the case, an ALP blood test should be the perfect way to help decide if your dog has liver disease.
Unfortunately, it is not quite that simple. While a high alkaline phosphatase level is very sensitive, it is not also a non-specific finding. This means that lots of other conditions aside from liver disease can cause an elevation in ALP. The list of conditions that can cause an elevated ALP includes:
Liver or gallbladder conditions
Any disease that causes a back-up of the flow of bile (i.e. cholestasis) will cause increased serum ALP levels in dogs. Cholestasis can be due to primary liver disease in dogs. Structural problems that block the flow of bile out of the liver, into the gallbladder, or from the gallbladder into the intestinal tract, can also cause a high ALP in dogs. Finally, secondary liver diseases (i.e. other conditions that cause ongoing damage to the liver) also will cause an elevated ALP level.
Primary liver diseases include:
- Infectious hepatitis due to ascending bacterial infections, Leptospirosis, etc.
- Chronic active hepatitis
- Copper storage disease
- Benign nodular hyperplasia
- Vacuolar hepatopathy in dogs
- Hepatocellular carcinoma (i.e. a type of liver cancer)
Gallbladder diseases include:
- Cholelithiasis (i.e. gallstones)
- Cholecystitis (i.e. gallbladder infection)
- Gallbladder mucocele in dogs
- Bile duct carcinoma (i.e. cancer of bile ducts)
Other medical conditions
Many medical conditions that are unrelated to the liver itself can also cause a high ALP. They range from non-worrisome to very concerning. Some of these include:
Endocrine diseases:
- Diabetes mellitus
- Hypothyroidism in dogs
- Cushing’s disease
- Hyperparathyroidism
Non-liver cancers:
- Lymphoma in dogs
- Pancreatic carcinoma
- Osteosarcoma (i.e. bone cancer)
Other diseases:
- Pancreatitis in dogs
- Gastroenteritis (I.e. inflammation of the stomach and intestines from various causes)
- Osteomyelitis (i.e. bone infection)
Toxins
Any toxins that cause substantial liver damage can also cause a high ALP in dogs. However, these elevations will not normally be as significant as the increases in ALT levels. Some toxins that cause liver damage are:
- Xylitol toxicity in dogs
- Cycad palms (i.e. sago palms)
- Zinc
- Aflatoxin
- Amanita mushrooms
- Blue Green algae toxicity in dogs

Breed-related elevations
Certain dog breeds can have increased ALP levels without it being a problem. The most common breed-related cause of increased ALP is Benign Familial Hyperphosphatasemia in Siberian Huskies. Scottish Terriers can also have a similar condition.
Medications
Some medications also are connected with elevated ALP in dogs. Two of the most common are:
Phenobarbital
This is a common medication vets use to treat dog seizures that can benignly increase L-ALP levels. However, phenobarbital can also occasionally cause damage to the liver. This means that if a dog taking phenobarbital has a high ALP, it can be hard to determine if the ALP elevation is no big deal, or if it might indicate a bad reaction to this medication.
If you find your dear dog in this situation, your veterinarian will likely start by evaluating how your dog is feeling. He or she will also look at the levels of the other liver values on the chemistry panel. In cases where the ALP elevation is severe, your dog is feeling poorly, or your dog has other liver enzyme elevations, then your veterinarian may recommend additional liver function testing.
In some cases, dogs will need to stop phenobarbital due to concerns about liver damage. The good news is that in most dogs, the liver values quickly go back to normal when the vet weans them off phenobarbital and onto one of the other medications available to help control seizures.
Steroids
Oral steroids, like prednisone for dogs, commonly cause moderate to severe elevations in ALP. Higher doses of steroids, such as those used for immunosuppression in cases of IMHA in dogs or other immune-mediated conditions, tend to cause higher ALP elevations.

Luckily, the increase in ALP from steroids does not generally correlate with long-term liver damage or liver dysfunction. However, it is important to know that once the dog stops taking steroids, it can take much longer—up to several months—for the ALP levels to normalize.
If your dog has an elevated ALP level, ensure you tell your veterinarian about all the medications your dog is taking or has recently taken. Some eye and ear medications and skin sprays or ointments contain steroids. Even these topical steroids can lead to ALP elevations during or after treatment.
Is a higher ALP automatically worse for dogs?
You may be wondering if you can use the degree of ALP elevation to tell you how bad the underlying problem might be. It would be easy to think that if a dog has a very severely elevated ALP, her or she might have a worse prognosis. Happily, this is not always the case.
Some benign and completely reversible issues, like taking high doses of steroids, can cause very severe elevations in ALP. However, if there is not an obvious reason for the high ALP (like taking a course of steroids), then your veterinarian may use the degree of elevation to help decide how aggressive to be with additional diagnostic testing.
What are the next steps for a dog with a high ALP?
If your dog has a high ALP, your veterinarian will start with a detailed medical history and thorough physical examination. In many cases, clues from the exam and history can help point your veterinarian to the next best diagnostic test to perform.
Every case is different, but the most common and least invasive next step is often to perform full lab work. This typically includes a CBC (i.e. complete blood count), full chemistry panel (if the ALP elevation was found on a “short” panel), T4 level, and urinalysis. If the remainder of your dog’s lab work is normal, he or she is otherwise feeling well, and the physical exam reveals no major concerning changes, then your veterinarian may elect for the “watchful waiting” approach.

With this approach, your veterinarian would hold off on performing any additional diagnostic testing right now. He or she will repeat lab work periodically to monitor trends in the ALP and other liver values. If the ALP improves or remains mildly elevated, then together you may elect for continued “watchful waiting.” If the ALP elevation gets worse, repeat bloodwork shows other abnormalities, or your dog develops any new medical symptoms, then your veterinarian will likely recommend additional diagnostic testing.
Liver function testing
One additional non-invasive lab test that your veterinarian might recommend is a liver function test which measures bile acid levels. Bile acids are made in the liver, stored in the gallbladder, and released into the intestines to help digest fat after you, or your dog, eats a meal. If the liver is working well, these bile acids are pulled back out of the bloodstream to be recycled and used again. However, if the liver is not functioning well, it is unable to remove the bile acids from the bloodstream and the bile acid levels will be high.
Your veterinarian can measure bile acid levels by taking two blood samples and sending them to an outside veterinary diagnostic lab. Your dog must have fasted for 12 hours prior to the first blood draw. Then your veterinarian will feed your dog a small snack, which should cause the gallbladder to release bile acids. Next, the vet will take another blood sample two hours later to see if the liver was able to remove the released bile acids from the bloodstream.
Elevated bile acid levels tell your veterinarian that your dog has a significant problem with his or her liver. But it does not provide any information about the underlying cause of the liver problem. If your dog has elevated bile acid levels, your veterinarian will likely recommend additional testing or referral to an internal medicine specialist.
Imaging
Your veterinarian may also recommend some liver imaging. In general, X-rays and ultrasound are the two most common types of imaging offered in veterinary medicine. While X-rays are a useful tool for many issues, they have limited ability to evaluate the liver.
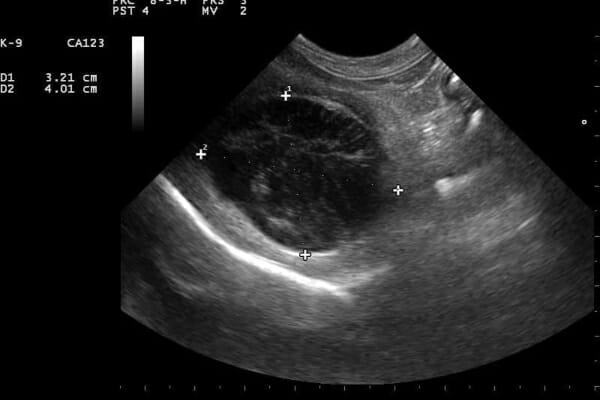
An abdominal ultrasound is much more useful in this regard. An ultrasound can evaluate for masses or nodules in the liver and can also assess the gallbladder for signs of infection, gallstones, or a mucocele. Plus, ultrasound can help determine if there might be other medical conditions like pancreatitis or Cushing’s disease that are causing a high ALP.

Liver sampling
One limitation to ultrasound is that while it can determine if the liver looks abnormal, it cannot definitively pinpoint the underlying cause of masses, nodules, or other abnormalities. Some nodules are benign changes, while others represent cancer. There may be clues on ultrasound that a mass or nodule is benign or malignant. But to know for sure the vet must take a sample of the liver. The two ways to sample the liver are fine needle aspiration or biopsy.
Fine needle aspirate
If your veterinarian finds nodules, masses, or other liver abnormalities, he or she may recommend a fine needle aspirate as the next diagnostic step. To perform an aspirate, your veterinarian will use an ultrasound probe to guide a small needle into the area of concern in the liver. Once the vet gathers the cells in the hub of the needle, he or she will squirt them onto a glass microscope slide. Then your vet will submit the slide to a veterinary pathologist for review.
In veterinary medicine we often start with fine needle aspirates over biopsies. This is because this testing is less expensive, less invasive, and the vet can do it while your dog is awake or with just mild sedation. The drawback of aspirates is that they do not always yield a diagnosis. If results are inconclusive, the vet may still recommend a liver biopsy.
Liver biopsy
A liver biopsy is the most definitive way to determine the underlying cause of liver enzyme elevations. However, it is more invasive than many of the other tests. To perform a liver biopsy, the vet will remove a small piece of the liver and submit it to a veterinary pathologist. Your vet may obtain the sample through an open abdominal surgery or laparoscopic surgery. Alternatively, your vet may use a large needle tool (i.e. the Tru-cut biopsy technique) which is significantly bigger than the needle for a fine needle aspirate.
Unlike a fine needle aspirate, which your vet can do on an awake dog, the vet will always perform the biopsy under general anesthesia. Although it may raise the question in some dog parents’ minds of “Is my dog too old for anesthesia,” a biopsy can be a very useful tool. It allows the vet to submit an actual chunk of liver tissue for evaluation. This can give a clearer idea of what is going on in the liver than a fine needle aspirate can.
Since biopsies are a more aggressive test, they may not be warranted in cases of mild or even moderate ALP elevations where the dog isn’t symptomatic and/or doesn’t have elevations in other liver enzymes. However, every dog and every case is unique. Your veterinarian will take your furry family member’s medical history, exam findings, and full lab work results into account when making his or her recommendations.

Back to my patient, Sampson
I am sure at this point you are wondering what happened to Sampson. We did perform full lab work, which aside from the ALP elevation, was beautifully normal. Apart from his sore tooth, Sampson was his normal squirrel-chasing self. He was energetic and had a great appetite.
We knew that his tooth was uncomfortable. Together his mom, Sarah, and I decided it was best to go ahead with his dental procedure. I am happy to report that the procedure went great. Sampson recovered uneventfully and is back to enjoying his crunchy dog biscuits and even the occasional stick (although sticks are not on my list of safe chew toys for dogs).
We rechecked lab work a month after his procedure and the ALP elevation was still there. Since Sarah is the proactive type, we decided to schedule an ultrasound for Sampson. The radiologist reported changes in the appearance of his liver that looked consistent with benign nodular hyperplasia, which was good news
I let Sarah know that benign nodular hyperplasia is very common condition in many senior dogs. It causes benign nodules to form in the liver and a mild to moderate ALP elevation without an elevation in the ALT. Changes on ultrasound can make the radiologist suspect this condition. But ultimately it would take a liver biopsy to rule out more nefarious causes of nodules.
After weighing the pros and cons, Sarah decided to continue monitoring for now. Sampson will come back in a month to monitor his ALP value. And then in a few more months he will have another ultrasound. I have a hunch that this is just going to be a blip on the radar for good old Sampson, and that the local squirrels won’t be able to rest anytime soon.
Talk to your vet
If like Sampson, your dog’s blood work showed a high ALP level, the best thing you can do is have an in-depth conversation with your veterinarian. Sometime being presented with all the different diagnostic options can feel a bit overwhelming. But at the end of the day, you and your trusted vet should be able to work together to create a plan for your dog—be it a “watchful waiting” approach or further diagnostics—that you feel confident about.
Hopefully, the elevated ALP will turn out to be nothing significant for your senior dog. But even if it does indicate a more serious problem, remember that your dog has a great ally in you and your veterinarian. Together, you can tackle whatever the future brings and keep making memories in the process.
Has the vet ever found a high ALP level in your senior dog’s blood work?
Please comment below to share your dog’s story.


Hi, I have a question. Can mexiletine cause a rise in ALP in senior dogs that already have an elevated ALP?
Hi Ann,
Yes, mexiletine is known to potentially cause issues with liver function. So, any dog taking this medication would need to have their liver enzymes routinely monitored for changes. Hoping you can discuss risks vs. benefits with your veterinarian and work together to find the best path forward. Wishing you and yours all the best.
My 13 year old Chihuahua Terrier mix is seemingly healthy other than his liver enzymes. His energy levels are surprisingly good as he still runs.
A year ago 1/15/25 I took him to TruVet specialty because he looked like he was in a lot of pain was getting growly when his stomach was touched or if I tried to pick him up. A full blood panel and urinalysis was done, but I could not afford to do medical imaging as well. He had urinary crystals and hes overweight so they prescribed me a urinary SO metabolic kibble. They sent me home and said it’s probably a slipped disc and/or osteoarthritis and he’s been on Galliprant & Dasuquin since then. Only other medication he is on is Simparica trio. And the dog food.
At that time, his ALP was 386 U/L
Since that vet visit a year ago, Leo nows displays all of the symptoms of Cushing’s.
I just had another blood panel done and now his ALP’s are in the 1500s.
The vet wanted to do a low-dose dex so he did that we just got the results back and they were negative. Now she wants to do an abdominal ultrasound, possibly a liver biopsy.
I feel like we are back at square one. 
What would you recommend doing next?
In your professional opinion does this case still give you hints of Cushings and would an abdominal ultrasound rule out liver disease?
I was thinking I would ask about the Denamarin supplement.
Hi Jessica,
I am sorry your pup has been through so much over the past year. I am not sure what other symptoms of Cushing’s your boy is exhibiting at home, but the elevated ALP alone would not necessarily point me in that direction. I think an abdominal ultrasound is a great next step. Not only can you get an idea of what the liver looks like, but it can also rule out other issues such as a gall bladder mucocele, kidney or bladder stones, and certain kinds of cancer. Denamarin is wonderful and you can definitely discuss it with your vet. Hoping for clear answers and an easy solution. Feel free to keep us updated on how things go.
My 5-year-old Shih Tzu, who is slightly overweight, had TPLO surgery in May 2025. Pre-op blood work showed ALP levels in the 400s. Since then, we’ve retested her regularly, and her ALP fluctuates between the 300s and 700s. Most other blood values are normal, except for a slight increase in her ALT above the normal range in one test. The internist prescribed Denamarin and Ursodiol, after which her ALT returned to normal and her ALP dropped by 200. She has also had several ultrasounds, which showed all her organs look fine, with just a bit of sludge. Moving forward, we will continue monitoring and retesting in a couple of months. Additionally, she has a grade 2 luxating patella in her non-TPLO knee. She used to eat a high-fiber, raised right pancreatic support diet with psyllium husk, but now she eats Royal Canin Shih Tzu and a homemade chicken and rice recipe. She behaves normally and has lots of energy. I am unsure why her ALP levels keep fluctuating.
Hi Goli,
I understand your concern for your young pup and think it is wise you have taken such a proactive approach to this liver issue. Without playing a personal role in your dog’s medical care, it is hard for me to make specific conclusions. I can say that I am very suspicious that the sludge seen in the gall bladder may be the underlying culprit. I assume the ursodiol helped to reverse some of the gall bladder problems and that is why the ALT was able to return to normal. As long as there are mild ongoing issues with the gall bladder, the ALP will probably continue to fluctuate. Routine monitoring is a great way to ensure things remain stabilized. Wishing your sweet girl continued success and many happy years ahead.
My rat terrier Ollie had an elevated ALP for the first time at his annual physical. He has a very round belly, but none of the other accepting symptoms of Cushing’s. However my vet ordered a first catch analysis which was negative for Cushing’s. Then he received an all day Dexamethasone Suppression Test which was also negative. He will occasionally wake up in the morning not hungry, will eat some grass sometimes we vomit but usually not and we’ll get his appetite sometime later in the day. He is a very active little guy, about nine years old.. my vet also did an ultrasound it did not find any abnormalities in the liver. The vet advised to wait and then recheck the urine and blood. She also wanted him to lose weight and we have been pretty successful, I have started feeding him fresh Pat chicken which is low in fat and cut way down on the treats. He has lost from 26 pounds to under 25 pounds in about a month.
He seems so happy now, and other than this abnormal test result and the occasional tummy upset which she has really always had often on. I am just really reluctant to put him through more testing.
In trying to do research on my own about what could cause this that was not liver disease or Cushing’s I saw the effect that long-term steroid treatment can have. My little dog has suffered with allergies on his skin and repeated ear infections. For the ears he has been given Mometamax many many times. Could this cause the elevation in his ALP?, I do not have the exact value but it was described as mild. I want him to be happy and to feel good, but I am afraid that if I don’t pursue this he may suffer and I don’t want him to deteriorate physically either.. I wonder about repeating bloodwork for this liver enzyme after he has been off this ear medication that I now know contains steroids, and to make sure that he is fasting when he has his blood work. I know that’s very conservative but I’ve had many many dogs over my lifetime and have learned that sometimes the way your dog acts is the best indication as to whether medical treatment needs to be more aggressive. Since he does not have Cushing’s, could my theory that his ear medicine is causing this mild elevation in ALT be correct?
As a result of the Dex Suppression test he is terrified to even go into the waiting room of the vet. When I took him in to get his nails trimmed he practically climbed on top of my head and did everything he could to get out of the office and back to the car. This is very unusual he is not usually this way at the vet. I am worried that this emotional state will also affect the bloodwork result. Is that a valid concern?
I am hoping that limiting steroid based medicines and continuing to lose weight will be adequate conservative treatment of this elevated enzyme but I don’t want to have my dog suffer long-term health affects for me not pursuing this in more depth.
Ollie looks a lot like the little dog in the picture at the beginning of your story. Even the little gray face. He is quite the corker, and except for the days when he seems to be off his kibble for a few hours in the morning leads a very active life. We walk every day about 2 miles and he plays with his toys in the house. Although at age 9 he also likes just chilling with me.
Thank you for listening to my story and being a sounding board. This has been the most helpful article I have ever read on the elevated ALP.
Hi Sharon,
I understand your concern for Ollie and think he is very lucky to have you advocating for his health and well-being. While topical steroids can cause changes to the body, I can’t say for sure if this is what is happening with your pup. It is wonderful that your vet is taking such a proactive approach and has done all the preliminary testing. I hope that nothing major will come from this and the liver enzymes will start to stabilize. Wishing your sweet boy many happy years ahead. Feel free to keep us updated on how things go.
My 11 year old Boston Terrier was scheduled for cataract surgery, 12/3. He had all the testing done due to anesthesia. On his bloodwork, his liver values were high. ALT-835,
AST- 99 and his ALP was 1900. The opthamologist wants to postpone surgery until he is seen by his internal medicine vet.
He had been seeing her for a couple years for GI issues. They found he had severe reflux, and delayed gastric emptying.
He was doing well on meds and recently lost interest in his food unless I cooked boiled chicken and boiled hamburger. We noticed his reflux got worse than usual as well. We finally did get him eating well by buying the fresh dog food and he loves that and gobbles it down, so then I thought he was just being picky.
They mentioned possible Cushings due to the elevated liver values, but doesn’t have the typical appearance and pot belly, etc.
I will be making an appointment with his internist on Monday. Of course we are disappointed to put off the surgery since he’s blind and it’s sad watching him bump into things, but we’d rather have him safe.
Do these values look indicative of Cushings and since his reflux is worse, possible gallbladder?
I’m glad I found this article on elevated ALP values. You get searching around Google and see the worst scenarios that it could be.
Hi Kathy,
I am sorry your boy is facing these unknown issues with his liver. I understand your disappointment about having to postpone his cataract surgery but agree it is for the best. These numbers don’t seem typical of Cushing’s disease to me, but that doesn’t mean it isn’t a possibility. They do make me suspicious about a gallbladder problem, and this definitely warrants further investigation. I am glad you are already planning to have the internist evaluate your pup. Hoping for definitive answers and a clear path forward. Wishing you and your sweet boy all the best.
Hi Sharon!
I’m going through almost the exact same thing with my dog. Suspected Cushing’s, but the low dex test was negative and now they want to do an ultrasound.
I would love to connect with you!
Heres my email if you’d like to connect!
[email protected]
About 2 weeks ago we took my pup Fred (10.5 yrs old) to the vet for labored breathing/panting. Upon exam we found out he had a heart murmur and was getting fluid build up around his lungs. They did labs and imaging and suggested we do an echo to see what is going on. We were sent home on an antibiotic and a diuretic to see if it would help and were told nothing else on findings at that time. We found he had B1 Degenerative Mitral Valve Disease after the echo report came back and was told that can happen in senior dogs. No longer than a week had passed since the report came back and we had a serious turn of events. In the morning, Fred went outside, had breakfast and seemed very normal. By 10 am he had collapsed by the back door in a pile of urine and stool and was drooling and panting. We called the vet who suggested visiting an ER as the would’ve best equipped to evaluate and treat him. He had pale gums and was in an unstable condition. During their exam they noted fluid around the abdomen and upon aspirate, found it was all blood. The vet said she noticed on Fred’s most recent labs (that were taken on the first visit above) his alk phos was very elevated (>2000) which led her to believe this was Hemangiosarcoma and a tumor/mass had ruptured suddenly causing these issues. We unfortunately had to make a quick, unexpected decision to put him down due to poor prognosis. Could his increased alk phos have caused some of the fluid build up they initially saw? Looking back on things he had been loosing weight and had quite a round belly for some time. Should we have looked into the alk phos at the same time as the murmur and other respiratory issues or being he was 10 would that value not have alerted you right away to question other possibilities? I feel like there are so many things left unanswered.
Dear Karissa,
I am sorry for the unexpected loss of your beloved pup. An increased Alk Phos will not cause fluid buildup, it is rather just a “warning” sign that something is wrong and needs to be investigated. But with the original heart and lung symptoms your boy had, I too would have focused on the heart issue first as it was more life threatening and critical at the time. Hemangiosarcoma is tricky and can often develop with no symptoms present until it is already at a very advanced stage. Here is an article with more information and I encourage you to read through the comments section as well: Hemangiosarcoma in Dogs: Symptoms, Treatment, and Life Expectancy
Hoping you can see that you made a loving choice to give your boy peace and freedom from his struggles. May his memory stay with you always and continue to be a blessing in your life. ♥
My 8½ year old Smooth Fox Terrier had a blood test 4 days ago. We took him to the vet because he is gaining weight and he barely eats. he always leaves his breakfast so in reality is just eating at dinner time. He has been lame since June but has no injuries, no pain, no arthritis so the vet thinks its because he is carrying around all this extra weight., he is 25kg and probably should be around 15kg. Its very puzzling since he doesn’t eat much as i said.
His ALP levels were 1467 and his glucose is 166. The vet gave us Obesity food and measurement for a 20kg dog instead of the 25kg that he weighs, so it’s quite strict. He’s still not eating breakfast. I have started walking him for longer. I was worried that with him being lame in his back left leg it would cause him pain but he seems to be loving it. We have walked for an hour every morning plus play time in the sea. We are going back in one month for more blood work and a weigh in.
I am just confused how he has gained so much weight and if the ALP and glucose are high because of the weight gain or if there is an underlying problem.
Hi Adele,
I am sorry your pup is experiencing these worrisome symptoms. I agree it is concerning and think it may be time for more in-depth investigation. Did your vet check a urine sample to rule out diabetes? Also, it might be good to rule out Cushing’s disease. Don’t forget, you are your dog’s best advocate and it’s ok to push for more answers if things don’t seem right. Hoping you can partner with your vet to get a definitive diagnosis. Praying for a clear path forward and a positive outcome for your sweet boy.
Hello and thank you for this very very helpful information. Yesterday I learned that my 9 yo Australian shepherd’s ALP levels were shockingly high at 2400 (though after reading through the comments I have seen higher numbers here and your responses were very comforting!). The rest of his bloodwork was normal. We have an abdominal ultrasound scheduled for next week.
My question is, to what extent might stress cause a spike to ALP numbers? We unfortunately had our annual wellness visit during a thunderstorm, so he was already anxious when we arrived, and he hates the vet clinic and hates needles. They had to put a muzzle on him because last time he nipped at the vet while she was aspirating a lipoma. They took him away from me for part of the exam. So I *know* he was wildly anxious. Could this account for the alarmingly high ALP? Did his body just get flooded with cortisol? He seems his normal self otherwise. Appetite is good, energy seems normal, and his bowels are working fine.
Next week I will dose him with gabapentin and trazodone before we go!
Thank you again.
Hi Allison,
I understand your concern for your boy with this new abnormality that appeared on his lab work. I wish we could blame this on stress and anxiety, but unfortunately, that doesn’t really affect this liver enzyme. I am glad you have an ultrasound scheduled and hope it will offer some additional information. Praying for clear answers and an easy solution. Feel free to leave an update if you have a chance.
I too am dealing with this with my 11 year old beagle, Scout. he just got his yearly bloodwork done and his ALT is 309 and his ALP is 7730! the vet is very concerned. unfortunately, she doesnt have the ability to do imaging so I have to have someone else do it so I am figuring that out. she said that is the best option to see what is going on but said with those levels, she almost guarantees there is a mass. he is eating and drinking fine and is still very active and loves to play so I guess that is good. it makes me feel better until I can get him into a place to get the imaging done. this article definitely helped me understand better though so thank you!
Hi Edward,
I am sorry Scout is facing this unknown issue with his liver. Hoping you can get the ultrasound scheduled quickly and that it will provide the needed answers. I will attach links to other articles with more information that may prove helpful moving forward. Wishing you both all the best and feel free to leave an update if you have a chance.
1. High Liver Enzymes in Dogs: A Vet Explains What It Means
2. Liver Disease in Dogs: Signs, Symptoms, Causes, Treatment
3. Hepatitis In Dogs: Causes, Symptoms, and Treatment
4. Liver Cancer in Dogs: Types, Treatment, and Prognosis
We have a lab/boxer mix that is 12 years old. In 2021, she had an ALP of 800 that our vet wasn’t concerned about since all other tests were normal. We have recently moved and the new vet is concerned but yet the first blood test with them was the same result. Other than being covered in fatty tumors for a few years, she is completely healthy. We have had several of those lipomas investigated and they are always benign. New vet put her on denamarin and did a recheck although the recheck didn’t get performed until a few months later but the ALP increased to 1200. We are doing another round but of all our dogs she was the healthiest and is the last one standing. She will be 13 soon, living well past the average lifespan. She doesn’t drink a lot, has a great appetite, chases the laser pointer and still follows us room to room like she’s a puppy. My question is can this be because of the lipomas? There are quite a few of them so maybe she has some on her liver? Would/could benign nodular hyperplasia be a concurrent finding with lipomas?
Hi Jennifer,
I understand your concern for your senior girl and think she is lucky to have you advocating for her health and well-being. Benign lipomas will not affect the liver. Even malignant liposarcomas rarely metastasize and the liver is very low on the list of potential sites for them to infiltrate. On the other hand, benign nodular hyperplasia is a very common finding and tends to develop with age. Without playing a personal role in your dog’s medical care, it is hard to offer specific conclusions and recommendations. I can say that if you are wanting to investigate further it may be good to consider a consultation with a specialist. Hoping for answers and a clear path forward. Wishing you both all the best. ♥
My 7 year old Cocker Spaniel has had an elevated ALP for one year. It started in the 300s, but has been over 2,000 for 6 months. Other liver values are normal. Cushings ruled out. Ultrasound revealed very small liver nodule that appears to be benign. She took Denamarin for 8 months and ALP continued to increase. She’s been on liquid milk thistle and dandelion and ALP is 2461. She’s had extremely elevated lipase and amylase for 2 years, but on a gently cooked low fat veterinary diet and always been asymptomatic. Recent bloodwork shows lipase is normal, but lipase is still high. What should we do next? One internist suggesting trying Ursidiol to see if it helps bring dorm her ALP. However, gallbladder appeared normal on ultrasound. Thank you for any insight!
Hi Angela,
I am sorry your pup has been having these ongoing issues with her liver. I agree with the internist that Ursodiol may be the next thing to try. This is very puzzling, and I can only imagine how frustrating it must be to have done so much testing and treatment and still be left with more questions than answers. Hoping new information will come to light very soon. Praying for a clear path forward and a positive outcome for your sweet girl.
Dear Dr. Buzby,
I hope you see my comment. My Yorkie who is around 10 y. o. has extremely elevated ALP.
Jan 30th: 520
Apr 14th: 2800
May 21st: 1925
Today, June 23rd: Over 2400
He’s on organic home cooked diet (chicken, fish, veggies and some berries) and has been on Milk Thistle, Dandelion Root, Turmeric and Mushroom Tincture since April. The ultrasound 2 weeks ago showed normal liver, kidney, and adrenal glands. Gall bladder had an anechoic teat shaped lumen with mild sedimentation. Our vet thinks it could be Cushion’s but my Yorkie does not drink water at all, other than when it’s extremely hot weather. He doesn’t pant, nor has a pot belly, his appetite is normal. The ONLY change that I’ve noticed is sometimes he pees more (longer in one try) than usual but it’s not every time that he goes on a walk AND sometimes there are some urine drops left on the couch/bed when he gets up after laying down.
Considering he has no definite symptoms of Cushion’s and the ultrasound didn’t reveal anything abnormal, what would your suggestion be at this point? Are there any other blood or any other types of tests that I could ask my vet to perform to figure out the underlying cause of such high ALP levels?
Thank you advance!
Olena
Hi Olena,
I understand your concern for your senior guy and agree this is a puzzling situation. Unfortunately, without playing a personal role in your dog’s medical care it is hard to offer specific conclusions or recommendations. It is quite abnormal for the ALP become this elevated without having other values be outside the normal range. Is the ALP the only thing elevated on the lab work? The problem with ALP is it is not very specific and can be affected by many things. If ultrasound shows the liver is normal, then it may be time to look elsewhere. I am suspicious about the gall bladder changes you mentioned. It may be wise to investigate that further. Don’t forget you can always ask for a referral to an internal medicine specialist. Hoping you can get the answers you need to ensure your sweet boy remains happy and healthy for as long as possible.
Hi and thank you for allowing me to comment … and everyone else. Your site is so informative. Well we have a wonderful 10 year old Chihuahua / Italian Greyhound mix. Last year she had a small mast cell tumor removed from her lower belly. She also has developed lipomas;; we have been testing when necessary and all benign. Kynda had bloodwork last year and all was normal. We just had a yearly checkup and her bloodwork showed a normal alt but alp at 199 which was 79. last year. The only difference in her diet is 25mg of Benadryl and a liquid mushroom support supplement daily. I am thinking the mushroom support might be having a negative effect? We just started her on Denamarin. She is happy, acts normal, loves chasing lizards.
I am wondering if we should have an x-ray done or maybe wait the 3 months and have another blood test. Might you have any further comments, please. So appreciate it.
Hi Susan,
I understand your concern for your senior pup with this new abnormality that was revealed on her lab work. I would be very surprised if the mushroom supplement was causing this issue. More than likely the two are completely unrelated. Denamarin is a great idea, and I hope you will see the positive effects reflected on the recheck lab work in a few months. I am not sure an x-ray will offer the type of answers you are looking for. If you wanted to pursue more in-depth testing, abdominal ultrasound is probably the way to go. But honestly, with only a mild increase in this one liver value, I would not normally recommend further testing at this point. Try not to stress over the “what ifs” and take things one day at a time. Praying for favorable results and a positive outcome for your sweet girl.
In Sept 2022, my dog was 10, closer to 11 with ALP of 268. Retested just that 2 months later and it was 257. In May 2024, he had bloodwork for a dental and it was over 350 I believe and the vet recommended an ultrasound which I passed on at the time. We had him tested for Cushing’s last year I believe and that was ruled out. Now he was sick with diarrhea for over a week, went and did all the things, xrays, bloodwork. Still waiting on those results. His PSL levels have been high previously too, with no pancreatitis symptoms, although I can tell when he has nausea, which has been an issue for years. Can pancreatitis cause elevated ALP? What level do you think is considered extremely high and definitely in need of further evaluation? I’m seeing people comment on here with levels over 1000, making me think the 300’s isn’t that bad.
Thank you!
Hi Gloria,
I understand you are hesitant to pursue further testing for your pup. While an ALP in the 300’s is not an extreme elevation, it is cause for concern. Also, your vet is not just looking at this one result but rather evaluating the trends. If there is any chance there is a liver problem that just hasn’t become severe enough to cause symptoms yet but could be caught early while treatment is still possible, your vet would rather be proactive than reactive. Yes, pancreatitis can cause other internal organs to become irritated, but again, your vet is looking at the trends over a period of time. Ultimately, you have to do what you are comfortable with and decide how far you want to go. Hoping for answers and a clear path forward. Praying for a positive outcome for your sweet boy.
This is the most informational article I have found. My vet didn’t even give me this type of info. So our little Bella is 12 and is in great shape from what I can tell. She had blood work a little over a year ago and her ALP was 1,460 and she mentioned I just needed to watch for increased drinking and urination. We just had her tested again last week and it’s up slightly to 1,487. She said it’s not increasing much and to take the wait and see approach (but then suggested almost $1,000 worth of tests). As you can imagine I am worried but should I be? I mean is that super high? Her panel came back great other than Globulin at 4.7 and Reticulocyte Hemoglobin at 21.7. Neither looked that far out of range. She does have some minor stomach issues (West Highland Terrier) but I have gotten them under control. I would live some advice and should I get a 2nd opinion without spending tons more money. I’d love to try something naturally first. Thank you!
Hi Shelley,
I understand your concern for your girl and think it is great you are searching for advice. While her ALP is quite elevated, I am happy to see that it hasn’t changed much over the past year. You could start her on a liver supplement such as Denamarin and then recheck her levels in a few weeks/months. But it may be time to think about more in-depth testing to ensure nothing serious is being missed. Abdominal ultrasound can be helpful to get a look at the shape and size of the liver and see if any nodules or masses are present. There are also other blood tests that offer additional information on how the liver and other organs around it are functioning. Ultimately, you have to do what you feel most comfortable with. You can take things as slow as you like or decide to be more aggressive with testing at any point along this path. With Bella’s current situation, I don’t think there is truly a right or wrong choice. Hoping you can get the answers you need to find a clear path forward. Wishing you both all the best and praying for many happy days ahead for your sweet girl.
about three years ago suddenly my beloved service dog was ill and cleared in pain. went right to the vet … blood work showed ALT 508 ALKP 279. …..he was put on a pill.with SAMe and sillimartin….and told he must never be given commercial dog food,no beef ….and only a diet of homemade white rice, chicken breast,i added blueberries and one egg a day and olive oil….he took the medicine as long as possible,but he is allergic to milk thistle….he recovered. Thank God for the healing….today he had a liver panel done…ohhhhh ALP 328 ohhhh….ALT 111….. tomorrow he will be tested for inflammation in his adrenals …he will be at the vets all day …..he is my beloved service dog…my stroke left me without feeling in my throat….when i was severely ill with covid he woke me up at three am ..a piece of chicken was swollen in my throat.. blocked my airway. sonce then he listens to me breath. and awakens me if my breathing changes….. he is a nine year old boarder collies lab mix…. please share your thoughts. very kind regards Suzanne Smith RN
Hi Suzanne,
I am so sorry your beloved pup is facing this unknown liver issue. I am glad your vet is planning to do some testing and hope they can get definitive answers. Don’t forget you can always ask for a consultation with an internal medicine specialist if needed. Praying for a clear path forward and a positive outcome for your sweet boy. ♥
Hi. My dog Chico just tested high for ALP. All of this other bloodwork results were in the ideal range, and he is a very healthy and active 9-year-old. He has epilepsy and has been on phenobarbital and Levectracetam for years. Last year his ALP was 700 and now it’s 1200.
My vet recommended several possible options. We could put him on a milk thistle supplement called Denamarin, which sounds kind of woo to me. We could test him for Cushing’s disease, or we could have an ultrasound test. Because of his general lab results and excellent health, I’m inclined to think it’s phenobarbital-related and not something to freak out about. On the other hand, he is my little muffin boy. Would you recommend changing his seizure meds? Is Denamarin legit?
Hi Karina,
I am sorry Chico is starting to show some elevations in his liver enzymes. I too would be suspicious about the phenobarbital as the culprit. It may be best to rule out other causes before switching seizure medications as phenobarbital has the highest success rate. But I definitely recommend trying Denamarin. It is the BEST liver supplement available (in my opinion) and the only one I use on my own dogs. It can’t cure liver failure but helps protect the liver from ongoing damage and promotes liver healing and detoxification. Hoping you can get the answers you need to find a clear path forward for Chico. Best wishes to you and your sweet boy.
Hi I was needing some help. My dog over the weekend stopped eating her food but will eat treats or human food. She randomly has that wheezy cough like she’s trying to cough something up so we took her to vet. Ultrasound showed enlarged liver and spleen and gallbladder was normal size but had sludge in it they said. Bloodwork only showed ALP elevated to 170, GGT elevated to 34, and total bilirubin elevated at 1.7. We have no idea what is wrong with her and I’m so scared for my dog. Starting her on antibiotic and ursodiol to see if she feels better and eats again. Do you have any insight into what could be wrong? Also she had a low platelet count that they don’t know why.
Dear Alex,
I am sorry your girl is having some issues and understand your concern for her health and well-being. I wish I could offer insight or guidance, but there just isn’t enough information at this point to make specific conclusions. There are SO many possible causes it is hard to narrow them down to a short list. We do have some great articles about several of the conditions you mentioned. I will attach links, and you can read through them when you have time. Hoping you can continue to partner with your vet as you both navigate this unknown path. Praying for clear answers and an easy solution for your sweet girl.
1. High Liver Enzymes in Dogs: A Vet Explains What It Means
2. Enlarged Spleen in Dogs: 7 Causes
3. Gallbladder Mucocele in Dogs: What You Need to Know
4. Low Platelets in Dogs: Thrombocytopenia
Thank you! They just called me this morning that there is a mass on her spleen so she needs a splenectomy. Unfortunately the low platelet count is our issue now to try to get it up so she can make it through surgery!
Hi Alex,
I am glad you were able to get some answers, but I understand this is just the beginning of a long road ahead. Here is an article you should take a look at: Splenic Masses in Dogs: Types, Diagnosis, Treatment, and Prognosis
Praying for your dog’s platelet count to stabilize so she can proceed with surgery. Wishing you both all the best and feel free to keep us updated on how things go!
Our 11 year old pitbull, Mr. Peaches, had his routine bloodwork late last summer show elevated ALP- around 270. In 2023 it was in normal range. Our vet tested for Cushings and the came back negative. We have had hepatic panels done every couple months since and they increased to 293 the first recheck, and remained exactly the same for the most recent panel. All of his other enzymes are within healthy range. I am curious as far as how elevated his numbers seem after reading some of these comments from other readers- would you call an ALP at 293 mild/moderate/high/severe? We are considering having an ultrasound done, also planning to start denamarin (sp?) soon.
The only other health issues we have noticed with Peaches is over the last year he has had a couple bouts of diarrhea, and one episode of vomiting recently. All tests from those instances did not show anything (X-rays, fecal samples) so vets thought he probably got into something on a walk we didn’t manage to get away from him, but I wonder if it could be related to the elevated ALP? He does whine sometimes but my husband thinks he just wants attention, and usually stops when we both sit next to him (rather than one person sitting next to him).
Hi Maggie,
I understand your concern for Mr. Peaches and think he is lucky to have you advocating for his health and well-being. Different vets will have different opinions about this ALP level, but I would consider it to be a mild elevation. I LOVE Denamarin and think the ultrasound is a great idea. This way you can ensure there are no other issues contributing to the high liver enzymes or catch it early if something definitive is found. Hoping for favorable results and a clear path forward. Wishing you and your sweet boy all the best. ♥
Hi,
My Siberian Husky male is 4 yrs 9 months old. We usually do annual blood work for him. In 2023 he started having seizures so we started giving him phenobarbital, after 6 months we did blood work found he has high ALP 582 doctor suggested to change from phenobarbital to kepra. After using kepra for 6 months we again did blood work his ALP was 205 U/L. After 1 year i.e., Feb 2025 we did annual blood work his ALP was 266 waited for a months and did one more blood work in Mar 2025 his ALP reduced to 10 points now it is 258 U/L. Vet suggest for ultrasound. Can you suggest us if we need to do ultrasound or watch and do blood work next month april to see if it is normal? what do you suggest?
Hi Sunitha,
I understand your concern for your Husky with how his ALP levels keep changing. I think the ultrasound is a good idea. The problem is you may not get any definitive answers. The reason your vet is recommending this more in-depth testing (if I had to assume) is they are trying to be proactive. I would hate for there to be something serious going on that is remaining hidden for now, that you might be able to catch early and effectively treat but end up missing it and allowing it to progress just because you decided to forgo the ultrasound. Waiting for the next blood work recheck is fine. But if these liver values continue to rise, I would not ignore them for long. Hoping for favorable results and a clear path forward.
My Lab mix, Jack, is almost 11 years old. In January he was straining to defecate and developed an anal prolapse. That was fixed and our vet suggested that he be on MyraLax and soft food for a week following as the prolapse healed. Then we were to gradually re-introduce his kibble along with the soft food. He started straining again and we took him back for a recheck 10 days later. It hadn’t prolapsed again. He was given metronidazole on Jan 23 because of a concern about colitis. He finished that medication and his stools started to firm up in February but not normal by any means. We noticed he started drinking a lot of water and would urinate what seemed to be a excessive amount but we thought it might be due to the medication. Then on Feb. 21, he started having watery diarrhea again. We took him back to our vet on Feb 24. He did an exam and found what he felt was a small anal sack tumor. We had brought in a urine sample with us and our vet also ordered a full chem panel. We got the results the next day. Albumin was low at 2.4 g/dl, Globulin was high at 3.8 g/dl, AST was high at 70 IU/L, ALT was high at 142 IU/L, ALK Phos was very high at 621 IU/L, GGT was high at 34 IU/L, and Total Billirubin was slightly high at 0.5 Mg/dL. Calcium was slightly low at 82 mg/dL. Our vet expected the Calcium to be high because of the anal sack tumor. The UA came back with cocci observed so a suspected UTI. Our vet suggested that we have an ultrasound to check for an spread of disease and to check his liver.. We are taking Jack in this morning for the ultrasound and we are both worried about what finding they may report.
Dear Kay,
My heart goes out to you as you face this worrisome situation with Jack. I am glad your vet has been proactive and is ordering these extra tests. Hoping for definitive answers and favorable results. Feel free to keep us updated on how things go. Wishing your sweet boy all the best.
Our 12 year old pitbull Sadie was diagnosed with Cushings disease in Nov 2024 after she started to have increased thirst and urination. She was put on 60mg of Vetoryl as she was 64 lbs. ALT was 204, ALP 461 and GGT was 33 (Lipase was 333). January 15th, she was incredibly unstable and had a seizure so we immediately stopped Vetoryl and her vet gave her a steroid injection and gave her 2.5mg of prednisone for 3 days to counteract the Addisons crisis. Those few days, we had our Sadie girl back. She was energetic, happy, silly.
Jan 30th, our vet started her on 30mg of Vetoryl and within 4 days we were told to stop it again as she was shaking quite bad, wasn’t eating, was lethargic, etc.
February 12, we did an ACTH which now came back as normal, not cushings, so vet suggested we do a complete panel again. ALT was 129, ALP was 403 and GGT was 14 (Lipase was 409). We were told her liver values were improving which was a good thing.
Fast forward 2 weeks, her shoulders/front legs are spasming whenever she is trying to relax and she is groaning and moaning anytime she is trying to lie down like she can’t get comfy.
Feb 23rd we rushed her to an ER after several hours of discomfort. ER ran complete panel again and now her ALT is 268, ALP is 853 and GGT is 29 (Lipase is now 1,945). They did an ultrasound and they did find a mass on her liver and they did a needle aspirate of but they don’t believe that is causing her the discomfort and are urging us to have her tested for cushings again as her adrendal glands were also thickened. All other organs were fine. We have an appointment with internal medicine tomorrow but am wondering what could have caused her numbers to double + in two short weeks. She went downhill so quickly and everyone just tells us “she’s a special case”.
Dear Meg,
I am sorry Sadie is having these ongoing issues with her liver. I agree, her situation has me puzzled and not sure what sort of advice to offer. I think partnering with a specialist is the best course of action. How did the appointment go? Were they able to offer suggestions about testing to treatment? Hoping there is a clear plan moving forward and praying for a positive outcome for your sweet girl.
My dear sweet Sasha has an alkaline phosphate level ALP of 3334. They want me to do an LMy dear sweet Sasha has an alkaline phosphate level ALP of 3334. They want me to do an LDDST test. Alt is 203. She is very fearful and they always sedate her. I would rather see an ultrasound than leave her at vet entire day, not many bushings. Symptoms. She has gained weight and does pant at rest but happy active pooch that loves walks. What is your advise? That level is off the charts!
Hi Sandee,
I am sorry Sasha is dealing with these elevated liver enzymes. While an ultrasound could be helpful, I also think the Cushing’s testing is a good idea. Your vet could probably get both done in one day and spare your girl from having to make multiple visits. There are options for anti-anxiety medications that could help make her visit less stressful for everyone involved. Hoping you can get the answers needed to ensure Sasha remains happy and healthy.
Wow! Thank you for this informative read! My almost 10 year old golden/husky mix had her annual labs (including urine) and her ALP was the only abnormality. It jumped from 500 in late 2023 to 800 as of yesterday so our vet is concerned for atypical Cushing’s disease. She has no other symptoms and the only medications she gets is Claritin daily for allergies and Meloxicam as needed, usually no more than once a week, often less. The diagnostic options he provided were sending out a test for Cushing’s or an abdominal ultrasound to rule out tumors or anything else that may be wrong with her liver. I am leaning towards the ultrasound, but wondering if that provides any value to diagnosing Cushing’s if that is indeed what she has? She has a history of arthritis and focal seizures (very infrequent, only maybe 1x per every 2 years). Is there anything else we should ask our vet about? Thank you, Amanda
Hi Amanda,
I understand your concern for your pup and think she is lucky to have you advocating for her health and well-being. It sounds like your vet is being very proactive and thorough with testing and diagnostics. I think the ultrasound is a great idea. If your girl does have Cushing’s they may be able to spot an enlarged adrenal gland. You can always ask for a consultation with an internal medicine specialist if needed, but I think you are on the right track. Hoping for clear answers and an easy solution. Wishing your girl all the best for many happy days ahead.
Hi there!
My ~9 year old Shih Tzu/Cairn Terrior/Pekignese mix (we did a DNA test), Pumpkin got bloodwork done prior to her dental cleaning in November of 2023. During this test, they realized that her ALT was slightly elevated (around 200) so she went on Denamarin and we monitored bloodwork. The levels only went down slightly (by ~10), so we did an ultrasound and the doctor didn’t find anything. They then told us further intervention wasn’t needed and that we should continue the Denamarin and do bloodwork every 6 months. Now it is January of 2025, a little over a year later, and our vet finally recommended seeing an internal doctor (I had asked multiple times in the past, but they said it wasn’t needed until now). The internal doctor did bloodwork and another ultrasound, as quite some time has gone by since the last one. The ALT remained the same—only slightly elevated (and around 10 less than the original bloodwork a year prior); however, the ALP is now ~400. The most recent ultrasound still didn’t find anything wrong. They want to test for Cushing’s, so we will be doing that next week. She has some of the symptoms, but most of which, have been present since we adopted her at three years old. She’s always had a little potbelly, has always panted/overheated easily, has always been lethargic when she isn’t going on a walk (she loves her daily mile walk and peps right up for this), and has always consumed an excessive amount of water (but no excessive urination ever). So, I was wondering if you had insight on what else could be going on with her? I love her so, so much and I feel so badly she has to go through this and go to so many appointments. Any help would be greatly appreciated.
One other thing I should note is that a few months before discovering any of these elevated levels in 2023, she was bit by a tick (in CT). The bite site looked swollen after and she had a swollen lymph node. It was winter and I hadn’t given her the Simpirico that month, so I was very concerned that she had Lyme Disease. I brought her to the vet and they treated her with antibiotics. After this, they did a Lyme Quant C6 Antibody test and the result was <10, so they weren’t concerned. I figured I’d mention this though because I saw you mention tick borne illnesses in other comments. If this was the case, what are the possible illnesses she could have? Again, any and all help is greatly appreciated. Our little dogs have always lived long lives (15 years plus) and I have been sick over the thought that something could be seriously wrong with Pumpkin at age 9. Thank you so much for your time and help in this matter!
Dear Brittney,
I understand your concern for Pumpkin and think it is good you are searching for answers. She is very lucky to have you taking such good care of her and advocating for her health and well-being. I think it is wise to move forward with the Cushing’s testing and would also encourage you to discuss the possibility of retesting for Lyme (as long as the last testing was not recent). Other tick-borne diseases commonly diagnosed are anaplasmosis and ehrlichia. I am glad you are working with a specialist and hope you can start to unravel this puzzling situation. Hoping for clear answers and a straightforward plan for treatment. Feel free to keep us updated on how things go. Praying for a positive outcome for your sweet girl.
My 5 yo dog Nash began to vomit periodically in June, 2024. He also seemed to have less energy and began sleeping more. An ultrasound showed an enlarged liver but no tumors. His ALP has increased from 1,030 in September to 1,729 in December. He was placed on Ursodiol in November when his ALP was 1,669. Although the medication seemed to slow the increasing levels, he is being tested for Cushing’s in 2 days. Based on the forgoing, is there anything else you would recommend? Nash is an 18 lb Maltese/Havanese mix.
Hi Laura,
I am sorry Nash has been through so much over the past few months. From what you have mentioned it sounds like your vet is being proactive and has already done all the testing I would normally recommend. It may be worth repeating the ultrasound at some point to see if anything has changed. How did the Cushing’s testing turn out? Hoping you can get the answers needed to ensure your pup is on the right course of treatment. Wishing you both the best of luck and feel free to leave an update if you have a chance.
Our Lucy is 12.5 and a 32lb. Corgi lab mix we think. 6 weeks ago she quit eating her normal dry dog food and is picky about the chicken/turkey and white rice we now feed her. She still gets excited for walks and loves chasing cats and treats and her energy level has not changed. She just has eating issues. Her blood test came back with an ALT level of 173 and her ALP level was 313. Her ultrasound revealed two small masses on her liver of 3.9 cm and 4.1 cm . We don’t know if an aspiration is necessary because if they’re benign we probably won’t do anything because we are afraid of anesthesia at her age and if they’re cancerous we probably won’t do anything. Is a liver sample necessary to see what’s going on?
Hi Heather,
I am sorry you are facing this difficult situation with Lucy. While a liver aspirate may offer additional information, you still might not get a definitive diagnosis. If you were planning to pursue surgery or chemo (or whatever the treatment recommendation may be) then getting a diagnosis would be very beneficial. But if you are leaning toward palliative care and treating symptoms, then I am not sure the additional information is needed. How are things today? Praying Lucy’s condition has stabilized, and her appetite has returned. Feel free to leave an update if you have a chance. Bless you both.
My 12 year old Golden Retriever had an elevated APL test today. She will be 13 in April. Her blood work in May was perfect and everything else on her blood work was good, She has an under active thyroid and is currently on thyroid medication. She has also been given Rimadyl to take as needed for her mild arthritic stiffness and soreness. Our vet ordered a urinalysis today to rule out Cushings. She does pant off and on but has for a couple years now – it mostly seems tk be related to temperature as she tends to get too warm. Our vet says the elevated APL is not necessarily indicative of disease and may just be because she is a Thyroid dog and her liver is just working harder. She doesn’t appear to have excessive thirst or hunger. I don’t notice a “pot belly” or any hair or skin changes…although she does tend to be more unsure or unsteady on our tile floor… so I am hopeful. I am pretty nervous and scared. I have had a Cushings dog and it’s not fun. Thank you for you informative read.
Hi Stacey,
I understand your concern for your senior girl with these recent changes to her liver. I am glad your vet is running some tests to rule out Cushing’s and other possible causes. Also, be aware that NSAIDs such as Rimadyl can cause liver issues in some dogs. It may be worth discussing this with your vet. Hoping for quick answers and a clear path forward. Bless you and your sweet girl. ♥
My five-year-old Yorkshire terrier needed dental work so the vet did a full blood panel found an elevated ALP 1999, after dental procedure and several teeth removed we waited six weeks and tested again. ALP dropped slightly. Waited another six months and now ALP is over 2000.. not sure what to do next
Hi Jennifer,
I understand your concern for your young pup. From what you describe it does sound like more in-depth testing will be needed to try and get some answers. Your vet may decide to send off additional lab work or recommend an abdominal ultrasound. Have you started your dog on a liver supplement? Sometimes they can make a big difference in liver health and function. Hoping you can continue to partner with your vet to resolve this problem. Praying for a positive outcome for your pup and many happy years ahead.
C 9 yr old cavapoo has addisons ( monthly zycortal 0.33 and daily 0.5mg pred) and IBD which is controlled with a fully hydrolyzed diet ( zd). 3 weeks ago she jumped off the bed and hurt her shoulder, later that night I gave her pardale and she was sick with stomach cramps. Took to oncall vet ALP usually 250 for her normal was now 600. ALT lower end normal value as previous. WCC normal and electrolyte ratio normal. all other bloods from FBC normal. After another dose of pardale as advised she was sick again. After this I ceased pardale and increased her daily steriods instead to help inflammation to 1mg per day. She was back to normal within 12 hrs no more stomach pain and shoulder limp cleared within 3 days. During this time they also noted ear yeast infection they issued surolan steriod ear drops 2 x daily both ears, they repeated bloods 10 days later and all still normal apart from ALP now 1000. The following week after this she is still asymptomatic and good appetite and lots of energy and no more sick than the 2 episodes after pardale they carried out ultrasound and all normal in spleen, gallbladder and liver. The vet is still concerned regarding the solely raised ALP incase diffuse liver condition that was not evident on ultrasound despite no further symptoms and doesn’t feel the increased prednisolone dosage and steriod ear drops could create such an increase in ALP and feels if further increase in few weeks wishes to do liver biopsy. I’m anxious regarding this as been told in past very risky for Addison dog and with her general health she has not dealt well with even minor sedation previously and allergic to painkillers and vaccines. Can doubling her steriods and using otic steriod drops along side potentially have the ability to cause this spike and would 3 weeks be enough time to see it stabilise or reduce. many thanks x
Hi Anna,
Goodness, your poor pup has been through so much over the past few months. I am sorry you are facing this worrisome situation with her liver. I would not think the increased prednisone or eye medications would make this drastic of a change on blood work in such a short period of time, but I guess anything is possible. I am glad your vet is being so proactive and recommended the ultrasound. If you are not already working with an internal medicine specialist, it may be time to consider asking for a referral or consultation. How did things look at the recheck? Hoping for answers and a clear path forward. Praying for a positive outcome for your sweet girl.
Dr Buzby,
Thank you for having this site – it has helped me a lot while I research and cope with my dogs liver issues. To start, in 2022 her ALP was 416, March of 2024 – 2059, July 2024 – 2225 and now in October 2024 – 2400. My Stacey shows no signs of any other issues and other liver numbers are all good. We gave Denamarin for 2 months and sadly ALP rose. We are now trying Hepato TruBenefits and will retest blood work in 6 months along with my vet suggested ultrasound. Is there anything you can add to what I have or suggest?
Hi MaryAnn,
I am sorry your pup is having these ongoing issues with an elevated ALP. I understand your concern and think it is great you are searching for advice. An abdominal ultrasound would be a great next step and may offer the answers needed to find a clear path forward. Also, if testing has not been done for tick borne diseases that may be helpful as well. Wishing you and your girl all the best of luck and keep up the good work!
ALP is up again.now at 3315 after the Hipato. ALT and AST remain normal. I am leaning towards the ultrasound now. Stacy shows no signs of slowing down at all. any opinion that you can share?
Hi MaryAnn,
I am glad Stacy seems to be feeling well and has maintained her quality of life. I still think the ultrasound is a good idea and may offer the answers you seek. Don’t forget you can always ask for a consultation with an internal medicine specialist if needed. I will continue to keep you and Stacy in my thoughts as you navigate this difficult path.
Hi Dr,
our 11 years old golden retriever has started to loose his back legs since February 2024.
ran blood test and found alp quite high.
ALB/GLOB : 0,8
S.G.P.T. S.G.P.T. (cinétique uv) : 70 U/L (23-212)
ALKP : 1091 U/L
GGT : 11 U/L (0-11)
The vet did a stim test and said the results were not obviously to say if it was Cushing or not ( T1 : 151 T2 : 752 )
We then did an ultrasound, nothing is showing, he is actually in pretty good shape.
he has lost a lot of muscle in his back legs and loosing strength, struggling to get up, will stop and just collapse if we walk too far.
we are waiting for his results as we did a myeloscan yesterday and his blood test had reached 1600 ALKP
Spinal fluid taken for test too, we just don’t know what’s wrong with him.
Appreciate the great article, thanks for sharing this knowledge.
regards
Hi David,
I am sorry your senior guy is facing this unknown condition, and I understand your concern. It sounds like your vet is being very thorough with testing. I hope you will get some answers soon. Praying for a clear path forward and many happy days ahead for your sweet boy. Bless you both.
Our 13 year old Havanese has an elevated ALP that jump by over 400 points to 682 in the last three months. She is panting, but was on prozac for anxiety. She seems normal other than urinating often, but we got her from a breeder and our girl had four litters with 28 puppies. That’s a lot of pressure on a very small bladder and like human women, we think her bladder is just weaker from her pregnancies. We also looked up side effects of prozac and one of them is panting. Our vet wants to do a complicated 8 hour test where we have to leave the dog there, and/or an abdominal ultrasound. I think at her age, she would stress at staying at the vet all day and we should just retest in a few months. We also don’t think the prozac is worth it and believe it may be worsening her panting. I would love your thoughts on the prozac side effects and when to take a wait-and-see approach given age and ALP levels. Thank you in advance for your time 🙂
Hi Lori,
I am sorry your senior girl is dealing with these worrisome symptoms. From what you mentioned, it sounds like your vet is suspicious of Cushing’s disease and is wanting to test for it. I think this is a good idea. All of the symptoms you listed can be associated with Cushing’s. I understand your concern with the stress that can come from being in the clinic all day. If you decide to forgo testing and would rather pursue palliative care, that is ok. Here is a link to another article with more information: Cushing’s Disease in Dogs: Symptoms, Diagnosis, Medications
I would not be worried about Prozac causing panting and would use it if your girl is truly dealing with uncontrolled anxiety. I do wonder if some of her anxiety behaviors could be caused by Cushing’s or another underlying medical issue that has not been diagnosed yet. Praying for answers and a clear path forward. Wishing your sweet girl all the best.
Hi, our 10 year old Wire Haired Fox Terrier has been lethargic so the vet ran bloods and found his ALP to be over 700. A CT scan revealed a growth on the spleen which looks benign but we can’t be sure and also gallstones. He has been taking Desitolit and Hepatosyl and the ALP has reduced by 24 % to in the 600s. We are having bloods again in 60 days. Is this ALP level very high I have seen some results of in the thousands on this thread? Also could the gallstones be causing raised ALP? Can you suggest food to suppprt liver health?
Hi Jane,
I am sorry your senior guy is facing these worrisome issues with his liver, gallbladder, and spleen. I understand your concern and think it is good you are searching for advice. While his ALP is not the highest I’ve ever seen, it does need to be taken seriously. With the abnormalities that were found on ultrasound, I would highly recommend you consider asking for a consultation with an internal medicine specialist. Gallstones can definitely affect the liver but there could be so much more contributing to this situation. Hoping you can get the answers you need to find a clear path forward with treatment. Praying for healing and a positive outcome for your sweet boy.
My 13 year old Australian Cattle Dog mix Maggie hasn’t been feeling well for the past two weeks, we have been back and forth to the vet. They say she has pancreatitis and her ALP levels are at 1881 which are a little higher than they were in January when we did a test for Cushing (which was negative). She isn’t keeping down any food, she is staying hydrated. We have tried Panoquell injections, entyce to eat, and Cerenia for nausea. Nothing seems to work. An x-ray showed an enlarged liver and we were on Denamarin but they vet took her off of it to focus on the pancreatitis. All of her other lab work is normal. We just aren’t sure of the best road forward. She won’t eat anything!
Dear Katelyn,
I am sorry Maggie isn’t feeling well and you are struggling to maintain her nutrition. It sounds like you are doing everything you can, and I am not sure of other advice to offer. Some dogs benefit from a probiotic like Purina’s FortiFlora. Restoring gut health can do amazing things. Hoping your girl can continue to fight and praying she can make a full recovery. Feel free to leave an update and let us know how things are going, if you have a chance.
My 7.5 yo border collie fell sick the end of May. After two blood transfusions and a whole host of medication at the ER she made it out with a diagnosis of IMHA. She was on the usual med cocktail of Cyclosporine (Atopica), Prednisone, Plavax, etc. After two weeks her red blood count was still hovering in the mid-20s, so not great and the Vet thought she should be doing better but we held off on adding Azathioprine to the mix. Fast forward two weeks to the beginning of July, she fell ill with what we assume was a liver infection – elevated liver enzymes, weak, lethargic, vomiting and terrible diarrhea, but red count number in the low 30s so her anemia wasn’t the problem. IV antibiotics and a three day outpatient hospital stay and she was getting better again. Two weeks later, she is still not wanting to eat and elevated liver numbers, we experiment and take her off cyclosporine (still on prednisone and plavax)… and she’s great! Energy levels are up, her behavior returned to normal, eating like a horse, we think she’s on the right path but when we get her red blood numbers back yesterday, she’s at 24.5 – devastating. Because of her elevated liver numbers we’ve just started her on Mycophenolate to see if we can get her red blood count back up and her anemia under control. If you have any insights on this progression I would love to hear as we’re grasping at straws now.
Dear Holly,
I am sorry your girl has been through so much over the last few months. I understand your concern and applaud you for taking such an active role in advocating for her health and well-being. Your vet is already doing everything I can think of to try and balance these two different issues. If they are not consulting with an internal medicine specialist on this case then that is something you could discuss. I hope your pup can keep fighting and pray she will stabilize. Wishing you and your sweet girl all the best.
My 6.28 lb 12 year old long haired chihuahua’s ALP was 194 and her Cholestrol was 347. She hasn’t been interested in food. No vomiting but had small soft slimy stool before I took her in. Her whole life she’s been healthy and there were never any concerns until around when she was 7 we spayed her cause she was producing milk. But other than that she has been well. Her energy levels are like any senior dogs but my doctor didn’t really do much when finding out her high values. She told me the possibilities but she’s having me wait 2 days and if it doesn’t get better then we would want to do X-rays. But my concerns right now is getting her to eat and drink water which today would be the 3rd day, we’ve tried many different things like white rice, kibble, wet food, treats. What can you recommend for now I’m very concerned that she isn’t eating. And also why does her appetite decrease?
Noemi,
I understand your concern for your senior girl, and I am sorry she is unwell. Unfortunately, without examining her myself, it is hard to make specific conclusions or recommendations. You can ask your vet about an appetite stimulant, and they may have some critical care food that may be more appealing to her during this time. If you want to proceed with testing, be honest with your vet and make your wishes known. Hoping for quick answers and a clear path forward. Bless you and your sweet girl.
my mixed terrior has an ALP of 457 Baxter (my fur baby) his glucose 123, ALT 48, BUN/ Creat Ratio 23.3
protien 7.6, BUN 11.6. our vet isn’t sure what is wrong yet. Baxter came home with a different personality after his teeth cleaning and loosing..just moping around but still wants to eat soft food. but no interest in his doggy sister or brother and just laying by himself. I have to give him medicine which makes him not like me at this time either. 😂
Hi Pamela,
I am sorry Baxter’s lab work is showing some abnormalities, and I understand your concern with his recent change in personality. I hope your vet will be able to continue the investigation and get the answers you need. Praying for a clear path forward and quick results. Best wishes to you and your sweet boy.
Hi,
My 8.5 year old hound mix rescue recently had 11 teeth extracted a few due to periodontal disease and an abscess. Her pre-anesthesia blood work came back with a High ALP 2136 and a slightly high ALT 127. She has been on Denamarin for about 2.5 weeks and just had a recheck. The ALT went down but the ALP went up a few digits. She is acting fine. Eating, running, sleeping well. It’s very hot in NJ. I do notice she is urinating more but not sure if it’s because shes drinking more from the heat? Sometimes asks to go out but doesn’t go. My vet is thinking Cushings but wants her to come in for an abdominal ultrasound. Does this sound like the next step? I am so worried! Is all of this information super concerning? Thank you so much!!
Hi Lori,
I understand your concern for your senior girl and think it is great your vet is taking things so seriously. An abdominal ultrasound sounds like a great next step and will help to get a visual on the physical structure of the liver. I wouldn’t be too worried at this point. There could be an easy way to get things back on track. Hoping for answers and a clear path forward with treatment. Wishing you both all the best and praying for healing for your sweet girl.
Thank you for this great article! My vet just told me my almost 10yo dog Daisy has ALP of 227 and 6 months ago it was 228. She’s prescribing Denamarin and we’ll retest in 30 days. Your article has reassured me that the results are no reason to panic. Thanks again
Hi Kristen,
I am glad you were able to find some comfort and reassurance from the article. I think the Denamarin is a great idea. Hoping Daisy will respond favorably and praying for improved results on her lab work next month. ♥
Hey, I have a female Siberian husky, 10 years old, 71lbs (overweight). She had surgery for pyometra May 11th, 2023. I did pre check up blood work and her ALT was 95 and her ALP was 298. They did a biopsy of the liver while in the surgery due to a spot on the liver. The biopsy results stated the spot was due to the sepsis of the pyometra.
May 26th, 2023 My dog got her staples removed and I redone her liver test. ALT was 186 and her ALP 269. The vet said it wasn’t nothing to worry about due to how sick she was with the pyometra.
June 28th, 2024 a year later I got a wellness check and went ahead and redone the liver test. ALT was 205 and her ALP was 1,160. Which is significantly higher than what it was a year prior.
I haven’t noticed any signs that are unusual with my dog besides her not having as much energy as she use to and sleeps a lot. She is a scared dog as well which lead me to Cushing disease but she did not show any symptoms of this besides having anxiety. I also did notice how much glucosamine she was receiving when adjusting her diet and once I stopped the supplement 4 days ago I’ve notice a drastic difference. She no longer hides, she gets on the bed and looks out the window, no longer runs on loud noises, she seems to want to go outside more and be around the family, more barking and howling. Just overall more energy and looks happy. Before she looked tired all the time and possibly in pain or sad.
May 26th, 2023 I put her on Dasuquin Advanced just for the extra joint support. My dog food (Merrick salmon and sweet potatoes) has 400mg of glucosamine and chondroitin sulfate 400mg and the supplement I give daily has 900mg of glucosamine and 350mg or chondroitin sulfate. I feed her about a cup and a half a day plus one supplement in the evening.
With this being said I wonder if the to much glucosamine and chondroitin sulfate could have caused these elevation in her liver?
Hi Zoiee,
I understand your concern for your girl, and I agree what you describe is worrisome. I have never known these supplements to cause an issue except in an extreme case where a dog ate an entire bottle in one sitting. Most of the research I looked through said dogs were given close to 2000mg per pound each day for 12 months without any issue. So, a 10-pound dog would have received 20,000mg each day in the study with so adverse effects. Of course, some dogs don’t follow the rules and I can’t say for sure that the glucosamine didn’t cause this issue for your pup. Ultimately you have to trust your intuition as you know your girl better than anyone. It may be time to do some more in-depth investigation such as abdominal ultrasound or advanced lab work. Hoping you can get the answers you need to ensure your pup remains happy and health for as long as possible. Wishing you all the best. Bless you and your sweet girl.
Hi there!
My little Chaplin is a 12 year old mixed rescued dog. He weights 17 lbs.
He has been living with a heart murmur which he’s been taking Pimobenden for.
I’ve also been giving him some supplements. Co Q10, salmon oil, probiotics and CBD oil.
He’s full of life, very active, drinking and eating normally. Nothing out of the ordinary until a couple of nights ago.
As he napped beside me, all of a sudden he woke up crying in pain. For the next few minutes he sat with his back curved, his tail between his legs and he would slightly fall to one side. After those few minutes he was back to his normal self and has been acting normally ever since.
His blood work came back with ALT 124, ALP 328 and Lymphocytes 1.0 and everything else was normal.
Do you think there is a reason for worry?
Hi Elizabett,
I am sorry Chaplin experienced this worrisome episode a few days ago. Without examining him myself it is hard to make specific conclusions. From what you describe I am a bit suspicious it could have been seizure activity. Dogs with seizures will often have normal lab work. This may have been a one-time event and hopefully you won’t ever see it again. If you do, the most helpful thing would be to see if you can catch the episode on video. Getting to witness this firsthand would help your vet in making a definitive diagnosis. Praying your sweet boy is feeling well and living his best life. Bless you both!
Hello! Our 10 year old terrier/spitz mix had a trend in Alk Phos from normal, to 250, 950 over 2 years in her pre-dental bloodwork., otherwise completely normal labs and acting healthy and happy. We did an US which was normal with mild gallbladder sludge detected. The Vet started her uraodiol, and we repeated in 2 months. Unfortunately it went even high to 1183 and rhwy would not give anesthesia for dental, and told next steps are a CT or FNA. We got a second opinion, and we’re told evated Alk Phos isn’t worrisome with a normal US and likely coming from a dental infection. New vet is going ahead with dental due to 2 likely infected teeth, and is fairly confident it will reverse issue.
Hi Julie,
I understand your concern for your senior girl with this increasing liver value. It is true that dental disease can cause the liver enzymes to be elevated and a dental cleaning can sometimes resolve the issue without further treatment. I would offer one word of caution. The presence of gallbladder sludge can lead to other more worrisome issues and needs to be closely monitored. I am not sure I would label these ultrasound findings as “normal”. I am glad you have found a vet with whom you can place your trust and work together to restore your pup’s health and well-being. Wising you all the best and praying for a smooth and successful dental procedure.
Hello everyone,
I’m reaching out for advice and to share our experience with our 6-year-old German Shepherd, Tyson, who is currently battling severe liver disease. We recently received his latest blood test results, which are quite concerning.
**Key Laboratory Results:**
– **ALT (Alanine Aminotransferase)**: 4800 IU/L (normal range: 10-125 IU/L)
– **ALP (Alkaline Phosphatase)**: Above 6000 IU/L (normal range: 23-212 IU/L)
– **Total Bilirubin**: 2.1 mg/dL (normal range: 0.1-0.6 mg/dL)
– **Creatinine**: 4.2 mg/dL (normal range: 0.6-1.6 mg/dL), indicating Grade III acute kidney disease
Additionally, we’ve noticed Tyson’s eyesight deteriorating rapidly, almost to the point of blindness.
We are deeply worried about Tyson’s health and his eyesight, and we would greatly appreciate any advice, shared experiences, or recommendations on managing such severe liver conditions.
Thank you all in advance for your support and guidance.
Dear Abhay,
I am sorry Tyson is experiencing these severe elevations in his liver and kidney values. With both organ systems being affected and this happening so acutely, I would strongly recommend testing for leptospirosis or tick-borne diseases. Is there any chance he could have been exposed to a toxin or poison? An abdominal ultrasound may be warranted, and I would also ask about a referral to an internal medicine specialist if needed. Hoping you can quickly get some answers and find a clear path forward with treatment. Wishing you all the best and praying for a positive outcome.
My dog is an 18 yr old doxie he has had a tooth problem for approx 1 yr plus due to his age I do not feel comfortable putting him under anesthesia so the doctor has been giving me periodically. Clementa myosin to treat his tooth infection after each round his tooth seem to get better, and then just reappear again a few months later, as you could see the swelling under his eye when he gets worse, I had blood work done recently to check for any type of infections or to see if safe to get the tooth extracted ! His results were all normal except the following high on ALT 207. Alk 385 WBC 30.9 platelet count 450 differential Absolute Neutrophils 2557.4 Bands 618. And a low T4 <0.5 so the vet put Sam on a liquid antibiotic called Amoxicillin w/clav 200mg / 5ml thyroxin 0.1 mg 2x daily and pro hepatic cat/small dog And When the amoxicillin ran out he was givenh zydaclin for his tooth again as it looks like it popped due to blood all over my bed from his mouth and swelling has gone down under his eye My question is does he need to be on the pro hepatic and thyroxin for long term if so those too meds are gonna cost too much every mo so are they necessary? I asked the vet and they said yes I guess in your opinion does this sound right ? And would you recommend him getting that tooth pulled at 18 yrs old ? And how bad is his blood work ? Liver and thyroid?
Hi Leann,
I understand your concern for your senior Dachshund with this ongoing tooth issue and lab work abnormalities. Unfortunately, without playing a personal role in his medical care, it is hard to make specific conclusions and recommendations. The pro hepatic sounds like a supplement to try and help the liver function better. While this is not a mandatory treatment, it could be the only thing available to help prevent liver function from worsening and keep liver failure from occurring. The thyroid medication is definitely for life, as untreated hypothyroidism can eventually degrade your dog’s quality of life. I am not sure if having the tooth extracted is the best course of action for your pup. But I do know that removing the tooth is the only way to completely resolve this issue and age alone should not be a deterrent to anesthesia. I will attach links to other articles with more information and great comments from other readers. Hoping you can find the advice you need to make the best choice for you and your sweet boy.
1. Is My Dog Too Old for Surgery?
2. Is My Dog Too Old For Anesthesia?
3. Senior Dog Tooth Extraction: What to Expect
4. How to Recognize a Dog Tooth Abscess and What to Do About It
My 8-9 yr old little terrier mix had her annual exam and bloodwork on 5/21/24. All results came back in the normal range except positive for heartworm. Her ALT was 24, ALP 8. She was put on doxycycline, which made her extremely ill. Her Heartgard case required a confirmation test for heartworm in order to pay for the treatment. One week later on 5/29/24 her heartworm test came back negative and her ALT skyrocketed to 4335 and ALP 1255. I don’t know what to do for her. I feel the doxycycline is making her very sick.
Hi BT,
I am so sorry your little pup is having these severe issues with her liver. It is hard for me to get the full picture of what is happening without being personally involved in your dog’s case. If the confirmatory heartworm test was negative, then I guess I am a bit puzzled as to why the doxycycline is still being used since it was part of the heartworm treatment. I am not sure if the medication is to blame for your girl’s elevated liver enzymes, but think more investigation is needed. Does your vet have the ability to do abdominal ultrasound? Hoping you can get the answers you need to restore your dog’s health. Feel free to keep us updated on how things are going. Best wishes.
thank you for this opportunity: 2 weeks ago, my 6 yo ?(previously healthy) Morkie ” George” had a massive seizure. At first I thought he hadn’t survived it, then thought he’d had a stroke as recovery was very slow. It was frightening. He saw an out of hours vet and commenced medication to control seizures. Pexion 100mg bd. His blood work came back with ^ALP >1200. Everything else ok apart from ^ cholesterol. His urine on dipstick is full of protein. A few days later the abdominal scan was found to be normal. His (sorry forgot the name) straved -blood- feed- blood test ” was a slightly elevated but the lab had reported not abnormal enough to warrant further investigation”.
During this time the Pexion has been increase to 150 MG bd to get better seizure control. I’ve just sat with him at 315am uk time having a massive seizure. it’s heartbreaking
and I’m at a loss as to what’s going on. How life has changed in 2 weeks.
I’d value your opinion
thank you Donna
Hi Donn8,
My heart goes out to you as you face this worrisome situation with George. While I am not familiar with Pexion (it is not available in the U.S.) it is common for some dogs to need more than one seizure medication to get things under control. If there is any way you can schedule a consultation with a veterinary neurologist, that could be very helpful. How are things today? Is your boy feeling better or is he still struggling? Hoping you can find the answers you need to help get him stabilized. Praying for healing and a positive outcome.
Bandit my 10 year old female Shih Tzu was acting very lethargic. did not eat for 48 hours, nor would urinate. off to the vet we go. Blood work and urinalysis is done. Everything is normal except for ALP 5718! way high. Next step ultrasound, all is good there also. Sent home to keep an eye on her.
Still very lethargic and not urinating as she should be. I am very worried and don’t understand why her ALP is so high and Dr doesn’t know why, nor give her any medication to bring it down. HELP!
Hi Gloria,
I am sorry Bandit is facing this difficult situation and you are left with more questions than answers. Without playing a personal role in her medical care it is hard to make specific conclusions and recommendations. I encourage you to talk to your vet about staring a liver supplement/protectant. Even if it doesn’t help, it shouldn’t hurt. Also, it may be time to ask for a consultation with a specialist. Hoping you can get some answers and narrow down the cause. Feel free to leave an update and let us know how Bandit is doing. Bless you both.
My vet told me to get Denemarin from Costco. It’s a supplement for elevated liver enzymes. Costco carries at the pharmacy.
Hi Doctor,
My very loving over extremely healthy active 15/16 year old mixed pup Lucky, we walk at least 1.5 miles a day but lately he’s been slowing down a bit and panting a lil more. I took him to the vet about 6 months ago, blood work at that time was fine. They suggested an oral trio heartworm/tick/flea med. He had a few crystals in his urine so they suggested I try wet food (i was cooking food for him because he had his teeth extracted 3 years ago. chicken breast and sweet potato.). He had a reaction to something. Excessive itching, skin bumps, yeast action, some bleeding. Which turned into swelling/licking/scooting anal area. Discontinued wet food and treated with Apoquel and medicated shampoos biweekly to weekly. Apoquel helped but discontinued after two bottles due to cost. Skin seemed to be getting better dog was sleeping better and less itching but he started having bloody stool. Took him back recently he had a skin infection and anal gland infection. I think because of the trio med but after comprehensive senior dog bloodwork ALT 134, ALP 434, GGT 24, TBilirubin 0.4. I have been really spoiling my dog with treats and steak dinners. Could this be related to the allergic reaction or is the allergic reaction indicative of something else. Vet thinks Cushings, Liver disease, Cancer, or hypothyroidism and wants to test for all but at 16 and really active and happy I don’t know even if he had any of the above if I would treat for it. I know you’re not my Vet and not treating Lucky but would a wait and see be appropriate in this case? I am hesitant to get the US Abd or other comprehensive testing for Cushings. Your thoughts are greatly appreciated. Thank you for taking your time to read this.
Hi Meera,
I am sorry you are facing this difficult situation with Lucky. Anything newly introduced into your dog’s diet could cause an allergy flare up if he is sensitive to the ingredients. It is hard to narrow down a specific cause with so many changes occurring at the same time. It is always ok to forgo testing and treatment as long as you pursue palliative care. The goal of any course of treatment should always be your dog’s comfort and well-being (quality of life over quantity). If Lucky is still experiencing these worrisome symptoms, I am not sure it is in his best interest to just wait things out. Something needs to be done to restore his health or offer relief. If you wanted to pursue testing, an abdominal ultrasound could be a great way to get some answers. I hope you can get the advice you need to make the best choice for everyone involved. Wishing you all the best and praying for a clear path forward.
Dr. Buzby, Thank you so very much for all of your in depth articles. I have a 14 1/2 year old mix rescue. I have had Lucy since 2011. She averages 70 lbs and is pure white. We believe her to be pit bull and lab? In 2019, after the loss of our best friend, Joseph the bullmastiff, Lucy had several “episodes” in succession. It was 4/3/2019, she came in from morning bathroom and like a windup toy running out of steam crumpled down and curled tightly to the right. All that moved were her eyes, darting all around. After about 30 sec she ‘released’ and wanted to play. She had 3 more within a half hour. Fast forward to current day. Lucy has exhibited what I know now are precursors, off balance and shaky eyes, but I will catch it and it seems that probiotics always make things better and making sure no one gives her food. A few months ago the doctor wanted a blood panel due to showing signs of thyroid issue. Her ALP was over 800, and she had hyperthyroidism but her kidneys et. al were fine. I took her back and her thyroid has leveled out but the ALP has only dropped to 760. Lucy does have large lumps, the largest inside of her rib cage closest to her belly.
I am not writing for advice, unless you feel inclined. I am writing to let the public know that staying in abusive relationships not only harm them, but can slowly kill you best friend. I hold myself accountable for Lucys condition. I finally was able to have my vet fully comprehend the level of captivity I have endured for almost a decade, and unfortunately Lucy has too. She deserves a medal and I promised her a mommy that doesn’t cry and a place where we can be safe and not afraid to laugh. And that’s what I am on my way to do for her right now. She is my only friend and my only family and I hope that of someone reading this is being subjected to abuse, please get away. I wont say it will be easy or better, but if you have a life depending on you, it will be better for them. No more excuses.
Dear Debra,
I commend you for having the strength to make some very tough decisions to improve the quality of life for yourself and Lucy. You are such an inspiration to me for having the courage to take a stand and speak out about your experience. Thank you for sharing your story with us. I hope you and your sweet girl have found some peace and are headed for brighter days. Wishing you nothing but the best and give Lucy a hug for me! ♥
Hello. I am hoping you could help me with my 10 year old maltipoo whose ALP was 1250 5 months ago. A year and a half prior, he was at 350. We put him on Denamarin 5 months ago and his level is at 900 today. The vet said all of his other bloodwork was fine. Should I be concerned? What could it be? His ALT was normal along with all other typical lab work. Thank you in advance!
Hi Alina,
I understand your concern for your pup with these changing ALP levels. What a blessing the Denamarin seemed to help and now the results have decreased. As the article states, there are many things that can cause the ALP to be elevated. Unfortunately, without playing a personal role in your boy’s medical care I can’t make specific conclusions. Hoping things will continue to head in the right direction and praying for complete resolution to this issue.
I am the owner of a 13 year old Hungarian Vizsla and I am a little bit distressed about the high alkaline phosphatase levels. We have been experiencing abnormal lab values since he was 7 years old. At that time we went to the vet for polyuria and polydipsia and the blood work showed a significant variation in alkaline phosphatase. The alkaline phosphatase value is usually between 2000 and 3000. In addition to alkaline phosphatase, his pancreatic enzymes have been elevated at times , as well as cholesterol and triglycerides. She has had all possible tests but nothing concrete has been confirmed. Alkaline phosphatase is steroid induced but Cushing’s and all other hormonal problems have been ruled out. She also had a severe pancreatitis at 9 ( probably secondary to the above problem), which she thankfully recovered from without any problems. She is on a steady diet and eats a special veterinary food, but every time blood is taken her serum is cloudy and full of fat. Over the years, there have also been ultrasound abnormalities in the liver. Currently, the liver structure shows inhomogeneity and there is a large nodule. She also had a liver biopsy from this nodule with a Tru-cut biopsy technique , which showed that glycogen is stored in the liver. Finally, the doctors concluded that she probably has some kind of hereditary fat metabolism disorder and is currently taking fat reducers, but her serum is as opalescent as before. I am desperate because she has been under constant monitoring and we noticed the problem at the very beginning, but we have not had any meaningful answers as to what is behind the ugly lab values and the ultrasound has slowly started to show a deteriorating picture which makes me feel helpless. The overall condition of the doggy is otherwise very good and even now she is very active and lively. However, I am afraid that the disease is causing changes to his liver that may shorten her life.
Hi Viktoria,
I understand your concern for your girl and am so sorry you are in this difficult situation. The only thing I can think of to offer as advice is maybe it would be good to pursue genetic testing. There are several options available and I’m sure the internal medicine specialist would be able to recommend one. I hope you can find a way to maintain your pup’s health and quality of life for as long as possible. Praying for healing and a clear path forward.
Our 16yr old Chi-Chi mix just celebrated her 3rd year post SRT for right sinus cancer. Her bloodwork levels have always been a bit odd, primarily her neutrophils and occasionally platelet count.
At the time of her SRT her liver enzymes were elevated so she was started on Denamarin. In the past 2 years her bloodwork has continued to deteriorate and in the last year she has shown signs of slowing down. A few days ago she started to have difficulty using her back legs. It was as if they had frozen. This has occurred intermittently.
The vet has done bloodwork and X-rays without coming to a conclusion. Her ALP level is now 2198, up from 1544 a year ago, 530 two years ago and 298 three years ago. Her GGTP is 62 up from 35, 21, and 13. Her cholesterol is up to 943. Platelet count is 370, neutrophils are 1922 and monocytes are 217. Her T4 is now 1.6, down from 1.4, 2.5, and 5.4.
The signs appear to point to Cushings, but from what I have read, only a large pituitary tumor would cause the hind leg issues.
She is a survivor, but we don’t want to put her through a lot at her age. Do you have any suggestions as to the diagnosis or additional diagnostics? Thank you.
Hi Joe,
I am sorry your senior girl has been through so much over the last few years. Unfortunately, I don’t have any good ideas as to what could be causing the elevations in her liver enzymes. If you are wanting to pursue further testing, an abdominal ultrasound could be very helpful. Also, you can always ask for a referral to an internal medicine specialist. They may have recommendations on testing or therapies you could try that wouldn’t be too stressful for your girl. Hoping you can find a way to improve her health and wishing you all the best for many happy days ahead.
My 12 year old Bichpoo has had a high ALP for the last 4 years. They did an ultrasound 3 years ago but that did not show anything explicit. She was put on Denamarin. Two years ago they added Ursodiol to be taken daily. I just received an email from the vet that her ALP went from 2252 to 2722 over the last six months and her ALT is now 170. She also said her pancreatic enzyme is much better. She suggested I either repeat the blood test in a few weeks or schedule another ultrasound. My girl does not act sick. The only change I noticed is an increased appetite. My vet wants to see senior dogs every six months and do bloodwork. Every time I take her the results are that her ALT is too high.
Dear M.,
I am so sorry you are facing this difficult situation with your senior pup. It sounds like your vet is trying to stay on top of things and being proactive with the medical decisions that are being made. I understand how stressful it must be to still have more questions than answers. It may be worth considering a consultation with an internal medicine specialist. I am glad your girl is feeling good and is still able to enjoy life. Wishing you both all the best and praying for many happy years ahead.
Renuka de Silva
Sri Lanka
Dear Doctor,
My Cockerspaniel mix female dog Mishty is 7 years of age.Few months ago she got Tick fever and her Liver ALT has increased to 400.The vet has given her Liv.52 with other Medications.Doctor now today I have checked her Blood Liver Test.ALT normal but ALP 800.Doctor can you please give me some information about what to do.Our Country Sri Lanka is a Poor Country.We have few experience Veterinary Doctors.Please doctor please give me some advice.Thank you.
Hi Renuka,
I am so sorry Mishty is having issues with an elevated ALP on her lab work. It is good news that her ALT is now normal as this enzyme is much more liver specific and would indicate the liver was having problems functioning properly. Since the ALP can be elevated for any number of reasons, it is harder to narrow down the cause without in-depth testing. I was not familiar with the Liv 52 supplement you mentioned but took the time to look over the ingredients. I did not see Milk Thistle mentioned, which is a very good natural supplement that helps to promote liver healing and protection. If you can find a Milk Thistle supplement that might be a good addition to what you are already doing. Here in the U.S. I use a product called Denamarin with great success. Hoping you can find the best way to ensure Mishty remains happy and healthy for as long as possible. Wishing you all the best and keep up the good work!
My sweet pup is 14 this month, a little 10 pound Havanese. They suspect Cushings (ultrasound a year ago didn’t show any issues but liver numbers elevated). He doesn’t have a pot belly, has always had a good appetite, hair does seem somewhat thinner throughout but not terribly, and thankfully no incontinence or strange thirst. I feed him a fresh food turkey or chicken diet (brand is Raised Right) that is lower carb. I add fish oil daily and some organic pumpkin powder for fiber. The vet did give me Denamarin which I’ve just started him on. Will bring him back to vet every six months for blood work – should I have it done more frequently? Also, are there foods I should avoid giving him – I was adding a fresh canned sardine (no oil or salt added) once a week, but read somewhere those are bad for dogs with Cushings. Should I stop all flee/tick, and heart worm monthly treatments? He’s an inside dog and does not go to dog parks or kennels. Thank you – much appreciated!
Hi Candace,
I understand your concern for your little pup, and think he is very lucky to have you advocating for his health and well-being. I am not aware of any issues with dogs with Cushing’s and feeding sardines. I highly recommend you continue giving monthly parasite prevention. While your boy’s risk might be low, I would much rather err on the side of caution and prevent a tick-borne disease (Lyme, ehrlichia, anaplasma, etc.) and possible deadly heartworm infection, than try to treat them after the fact. Also, most heartworm preventatives deworm for intestinal parasites as well. This is very important because several species of these GI parasites are contagious to humans. I feel like the current recommendations from your vet to monitor lab work every 6 months seems pretty standard. I usually only push to run labs more frequently if things are changing fast or I am seeing drastic changes. If you would like to have lab work repeated sooner, I am sure your vet would be happy to oblige, and you would only need to ask. Hoping your sweet boy is doing well and wishing you all the best. Keep up the good work!
hello, my 8 year old Bichon Frise has gone through bladder stone removal, she had 7 big stones (1.6 cm ), ofc my vet did a full blood test before the surgery and everything was normal, we changed her food to Hills CD, since the stones were sent to a lab and from results she needs to be on that food for the rest of her life, one and half months past since then and one day she was throwing up and making choking noises and shaking, i toke her to the vet he did a scan and seen nothing but 1 stone in her kidney (1.6 cm), we did a full blood test and found her ALP 2000 and her ALT was 176, we did an ultrasound and found everything was ok, he did say there are some leftovers of the infection in her bladder, also he said she had a lot of poop, I wanted to ask if it can be that the kennel cough, the kidney stone and the leftovers of the inaction in her bladder can make her ALP jump so high in 1 month, right now we are testing her for Cushing syndrom via a urine test, we also tested her for parathyroid gland and was negative
Hi Song,
I understand your concern for your girl with the recent abnormalities on her lab work. Without playing a personal role in your dog’s medical care, it is hard for me to make specific conclusions. Generally, I would not expect to see problems with the liver due to bladder stones or kennel cough but that doesn’t mean it isn’t possible. I am hopeful that your vet will continue investigating until the cause can be determined. Praying for answers and a clear path forward for your sweet girl.
Just took my female 15 yr old bird dog mix to vet today because she has a large amount of gas every night and has had 2 focal seizures within the last month. So much gas that she paces and can’t settle down to sleep. Had been thinking it was sundowners but she is alert and not confused at all. My gut says it is the amount of gas making her act the way she does in the evenings. Had full blood panel and thyroid tested. Everything was normal except ALP was 1200.. Had ultrasound and everything looked great there too. Vet suggested using a hydrolyzed protein food and do an elimination diet. Starting that today but was wondering if you had any thoughts?
Hi Jeanne,
I understand your concern for your senior girl and think it is great you are searching for ways to help her. Any time I have a patient with GI issues I recommend trying a probiotic supplement. You would be amazed at what a simple supplement can do to help restore normal function in the stomach and intestines. Gut health is a big deal! Hoping the new diet will be beneficial and make sure you keep your vet updated on any new developments. Best wishes to you and your sweet girl.
Hi Doctor. Mickey is 14 years old rat terrier (possibly older, he’s a rescue) . Not active, sleeps a lot but still has good spring in his steps and waggy tail. Last year is ALP was around 1300 and ALT around 170. This year with no changes, the ALP went down to 800 and ALT stayed about the same as before. He’s a picky eater. His abdomen is distended, Vet said start of Cushing disease. Mickey’s only med is Omeprazole daily. Lately we noticed he gets restless at night, wanting treats but not his food, or another night he went around the house restless. Vet prescribed gabapentin, we think a bit of dementia. His hearing is poor as well. Now the the real problem he’s had brown/gold, yellow watery diarrhea for 5 days. He’s not interested in his food at all but does take his favourite treats. He’s always up in the night to drink and go out to urinate or poop several times a night leaving us with little sleep. Does this sound like late stage liver disease? We are contemplating letting him go.
Hi Brigitte,
I understand your concern for Mickey. I wish I could give you specific advice, but without examining your pup myself it is hard to make definitive conclusions and recommendations. Since his lab work has improved, it is hard for me to believe that his liver dysfunction could have progressed to a more advanced stage. It sounds like there may be something else causing (or contributing to) these symptoms. Please reach out to your vet and let them know about the diarrhea. They can do a quality-of-life evaluation and let you know if it is time to say goodbye or recommend further testing and treatment. Hoping you can find the answers you need to make the best decision for your sweet boy. Wishing you both comfort and peace.
My 14 1/2 year old CairnTerrier has an elevated ALP of 1700 and from a xray we just from out that she has an enlarged liver. The vet said she has had a history of of high ALP but because there have been no additional symptoms they never recommended additional testing until now. She was at the vet to treat her bloody diarrhea which she has had a history of for several years. This and a little arthritis and sensitive stomach have been her only issue. We are now faced with what to do as a next step.. She seems fine and walks 3 times a day and is active. With her advanced age we are hesitant to get an aggressive treatment and are really considering to just keep an eye on it since she is not showing any other symptoms (she has had some trouble on occasion with vomiting up her water) and just let her have a peaceful senior life. The vet did not give any simple ideas for treatment.
Hi Maureen,
I am sorry your senior girl is having issues with her liver. I understand not wanting to pursue a lot of testing or aggressive treatment. Palliative care is always a great option. At the very least, you could talk to your vet about starting a liver supplement. I have had great results with Denamarin in my own patients. It supports normal liver function, protects the liver from damage and helps with detoxification. Hoping you can find the best way to ensure your pup remains happy and healthy for as long as possible. Best wishes and good luck!
Our almost 13 year old Chihuahua Terrier mix is scheduled for surgery in 2 days for gallbladder removal. She’s had Cushings for almost 5 years with virtually no symptoms and no medication. We took her in for what we thought may be a UTI last week because she was leaking urine. Upon taking her in they did blood work and found her ALP levels to be extremely elevated at 3200 Her GGT is also elevated as well as her WBC, platlettes, and potassium. They also said protein was spilling into her urine. They suspected a gallbladder muscoele and upon doing an ultrasound, suggested gallbladder removal and biopsies of her liver/stomach. She’s been on Ursodiol for almost a year for previous gallbladder concerns, so this is the next step and hopefully it will solve some of her issues. Should we expect her Cushings to be worse now? Could not treating her Cushings have caused any of this? Any tips or advice? She doesnt act 13 at all so we really hope she has at least another 5 years. We don’t want this to be the start of her deterioration.
Dear Samantha,
I am sorry your senior girl is dealing with so many issues at once. I would not think surgery would cause her Cushing’s to worsen but I’m not sure we will really know what to expect until that time arrives. I do not think the gallbladder issues would have been caused by not treating the Cushing’s disease. My best advice is to take things one day at a time. Focus on getting through surgery and on the post-op recovery. Then with time you will know if the Cushing’s has remained stable or if treatment will be needed. Wishing your sweet girl all the best and please keep us updated on how she is doing!
First thank you for sharing all this info, it really helped me make sense of the blood test results. I couldn’t find a way to comment except for the reply.
My 8 yr old Azlan a GS, AUS, and Collie mixed , has had elevated liver enzymes but only the ALP, most recent was 485. Reading others comments they are sharing numbers in the 1000’s and so I’m wondering if I could change his diet along with liver supplements to see if that makes a difference. He was on the Denamarin for 30 days but no change in his diet. His weight has never fluctuated more than 3 lbs so no issue there but read how high protein food can affect liver enzymes. Another important note is he was tested for MMM due to indented head. Test came back as borderline. He’s never had any eating issues and has a talent of carrying 2-3 toys/bone at once and like I said no change in weight and he’s a pretty active dog. The vet wants to do a low dex test which will be costly and if that doesn’t show anything then an ultrasound which is even more costly. Just not sure what to do.
Hi Rachel,
I understand your concern for Azlan and think he is lucky to have you advocating for his health and well-being. Trying to find a cause for an elevated ALP can take a bit if trial and error and a lot of patience. I would bring up the topic of a diet change to your vet and see what they think. It is possible this could offer some great benefits. As for the other testing your vet has recommended, it sounds like a good plan of action, and I would be planning to do something similar for one of my own patients. Don’t forget you can always request a consultation with an internal medicine specialist if needed. I am hopeful that you will get some answers and be able to find a clear path forward. Wishing you and Azlan all the best. Feel free to leave an update and let us know how things are going if you have a chance.
Hello and thank you for being here.
My 13+ chi-mix rescue was put on Carprofen for arthritis almost 2 months ago. She did not have labs prior. I took her for labs yesterday and I’m puzzled by the results. First I’ll tell you, she does not want to go for long walks, and is somewhat lethargic, but she wags her tail, has a very good appetite, normal stool, no diarrhea or vomiting, no changes in behavior. She has been extremely thirsty and urinates OFTEN, Glucose is perfect.
Her labs:
AST 207
ALT 685
ALP 3628!!!
Cholesterol 373
Platelet count 940!!!
Cystatin B – High 164, but SDMA – Normal – 10.
Specific Gravity – Low – 1.016
Blood – High 3+
pH – low 5
Protein – High 2+
BUN – High 35
everything else is normal.
Bilirubin, GGT and Albumin – normal.
This seems odd. at first I thought liver & kidney injury from Carprofen, then it doesn’t look consistent with liver injury or disease. Someone mentioned Cushings Disease.
Can you make an educated guess as to what this may indicate. I understand it’s just a guess.
Thank you. – Concerning, scared, dog mom.
Hi Lisa,
I am sorry your girl is having these strange abnormalities on her lab work. It definitely seems like there needs to be more in-depth investigation with the liver. It may be worth stopping the NSAID and trying a different pain medication just to be safe. This would be a great discussion to have with your vet. There are liver supplements that help improve function and are protective that can be used try and decrease these values. Also, with the presence of protein and blood in the urine it could be a good idea to treat for a possible UTI. Of course, the most important part of evaluating a patient is the physical exam and without being able to personally examine your pup, I can’t make specific conclusions or recommendations. Hoping you can find the answers you need to navigate this unknown path. Wishing you both nothing but the best!
Hello. My 7 1/2 year old Schnoodle has had “mildly elevated” liver enzyme lab results since first measured at 2 years of age. Last week they were ALT 158, ALK Phosphatase 255, which is higher than before, especially the ALK. All other chemistry/CBC work-up was normal. My vet is uncertain what the next step will be, other than measuring water intake for 72 hours. Your thoughts please– greatly appreciated!
Hi Donald,
I understand your concern for your pup and think it is good you are searching for answers. Here is a link to another article that discusses the recommending testing and possible treatment options: High Liver Enzymes in Dogs: A Vet Explains What It Means
Hoping the information will help guide you along this difficult path. Wishing you and your sweet boy the best and praying for a positive outcome.
I have a English / French bulldog mix named Angel that has an ALP of 353. I’ve done some reading on the joint supplement glucosamine and that it can be bad for a dog with underlying liver issues. Is this true? and could this have caused the elevated ALP? I just got these boys results last week. I haven’t given the joint supplement to Angel in about a month now. I’ve ordered a special liver health prescription dog food for her. I don’t know what to do.
I’m particularly frightened as I just lost my dog Daisy, an olde English bulldog, to liver failure a month ago.
Hi Amy,
I understand your concern for Angel and am so sorry for your recent loss of Daisy. From the articles I searched, it seems as though glucosamine could cause a mild progression of liver dysfunction. This is because glucosamine is metabolized by the liver so it will cause the liver to have to work a bit harder. But the liver dysfunction must already be present. I could not find definitive evidence of glucosamine being the primary cause of liver issues. So, I do not think the glucosamine caused your dog’s elevated ALP, but now that you know about these abnormal blood work results it might be a good idea to discontinue the supplement out of an abundance of caution. Hoping you can find the cause of Angel’s liver problems and start the appropriate treatment. Praying for a positive outcome!
hi I have a 5 year old short hair terrier/cocker spaniel she just had her annual blood work done a little early for next year since we were getting annual heart worm/tick testing done. my vet called me with the results and said that Oreo’s ALP levels are high and now we go on Wednesday for an ultrasound of her liver… I’m worried for her , my sister just had her beagle Jinger put to sleep because of her declining cushings disease she was only 5 years old we both got our dogs within weeks of ech other. I hoping that Oreo doesn’t have cushings… she has no other symptoms of this but she does get ear infections/yeast over growth in both ears other then that she eats normal she plays like crazy runs ,just I’m just hoping this turns out to be something else that can be treated with medication for a longer life with me and her sister Mooey . What are your thoughts? thx April N.
Hi April,
I understand your concern for Oreo with these new changes to her bloodwork. I think ultrasound is a good idea and I am glad your vet is being so proactive with testing. Hoping you get some definitive answers and there is a clear path forward. Wishing you both the best and praying for a positive outcome. Feel free to leave an update as you continue your journey.
Hello!
I have 14-year-old Pomeranian shih-tzu mix. She has been on two rounds of antibiotics for a UTI that she just can’t shake. Her last labs showed an elevated ALP of 628. Could antibiotics be responsible in causing a spike in ALP levels?
Hi Alex,
I am sorry your senior girl is having so many health issues. While there are some antibiotics that can have negative effects on the liver, I would not normally expect this after treating a UTI. It sounds like this may require some more investigation. Hoping you can partner with your vet to get some answers and ensure your sweet girl is headed in the right direction.
I have a 13 year old Chiweenie that was just diagnosed with Cushings disease. Her ALP result came at 3049 Reference value should be 5-160 U/L. This being so way off the chat, Is there still hope? We just started a regime with Demamarin for 2 months.
Thank you for any input.
Sheila
Hi Sheila,
I am sorry your pup is dealing with liver dysfunction. I am assuming it is probably a side effect of the Cushing’s disease. Did your vet start your girl on a treatment for the Cushing’s? In my experience, the liver function usually improves as the Cushing’s disease becomes more regulated and the symptoms decrease. Hoping this is the case for your dog as well. Wishing you the best of luck.
Hi thank you for all the information my 12 year old terrier mix we went to the vet to have some warts removed from her head they had to do bloodwork and her results came back high ALP 967 and high PLT 605 and low LYM 0.79 so after that was tested for Cushing not that and also passes her bile acid test what could be the causes and she doesn’t seem bothered at all by any of it
Hi Heidi,
I am sorry your senior pup has these abnormalities on her lab work. I am glad her Cushing’s test was negative and so far, everything else seems to be ok. Without playing a personal role in your dog’s medical care I am afraid I can’t make specific conclusions. It sounds like you will have to do more in-depth testing if you want to find the cause. Maybe you can talk to your vet about what the best next step would be. They may recommend abdominal ultrasound or even scheduling a consultation with a specialist. Hoping you can get some answers soon. Best wishes to you and your sweet girl.
I have 2 6month old Aussaliers brother and sister Flash, and Molly from the same litter. They just had their little boy and little little girl surgeries this week and we have their first bloodwork done so that we had a baseline in their chart and everything came back normal except their ALKP or both high Molly was 239 and Flash was 262 They have been fasting 12 hours prior to bloodwork being done with this of caused the ALKP to be high? Should I be concerned? The vet says that the mild elevation in their bloodwork is normal because they are growing. I just wanted to get a second opinion. We do not feed them anything except their dog food which is science diet and they are exercised well. Any feedback would be great and appreciated. Thank you.
Hi Melissa,
I know it it can be concerning anytime your dog has bloodwork abnormalities. Hopefully it will ease your mind to know that yes, like your vet mentioned, ALKP elevations do sometimes occur in young growing dogs. In this case, the elevation typically comes from the “bone version” of ALKP rather than the “liver version” so it isn’t usually a cause for concern. Especially since it was the case for both of them, rather than just one of them, bone growth seems to be the most likely explanation. However, there is certainly nothing wrong with asking your vet for some follow-up bloodwork after your puppies are fully grown (or sooner if you are noticing anything is off with them). Hope that helps!
Was happy to come across your article on high ALP levels. My daughter’s 11-year old YorkiePoo had a recent level of 1207, it was 1003 in May, 290 in 2/2020. The vet prescribed Denamarin and the levels did not go down after 30 days. Now is recommending more testing and pushing a $600 ultrasound, or an in-house test for $100 that could tell them if he has a liver disease or damage, or another one for $170 where they can figure out which ‘protien its coming from’. My daughter, of course, loves her dog and wants what is best, but doesn’t want to go in debt because of tests and then what may come after. Remy has the energy of a puppy, eats and drinks well, normal fecal movements and shows no sign of anything wrong. Can I ask you advice? Your article was so easy to understand, I’m hoping you can provide a second opinion and guidance. Thank you!
Hi Vicki,
I understand your concern for your daughter and her pup and think it is great you are reaching out for advice. I know testing can get expensive and everyone has a financial limit. Unfortunately, finances can also limit our options and make owners face some difficult decisions. It is very possible that even though her dog is feeling well now, Remy may start to show symptoms if things continue down this path. Your vet is trying to get ahead of things and get answers before Remy becomes sick or painful. In a situation like this, I too would be recommending abdominal ultrasound and some additional lab work. With that being said, it doesn’t mean it all has to be done right away. I think it would be best for your daughter to talk to her vet and make sure they are aware of her concerns and wishes. Her vet should be able to prioritize the testing and work with her to meet in the middle. I am hopeful that working together as a team you can find the best way to proceed. Wishing you all the best and praying for a positive outcome.
We have a pure bread Beagle named Daisy who is 4 years old.. last November we had ALP bloods checked and they were 353, Had them checked today (one year later) and they are at 903… All else is normal with her, all other bloods were normal range (ALT etc). Had her tested for cushings a year ago and it was negative, also had ultrasound of abdomen a year ago and was negative. Urine test was negative for proteins a year ago.. What are your thoughts?
Hi Emma,
I am sorry Daisy is showing a steady increase in her liver values over the last year. It may be that when the tests were originally performed, the disease process was not far enough along to show any other abnormalities. If you repeated the testing now, you may in fact find something to help point you in the right direction. Also, it might be a good idea to schedule a consultation with an internal medicine specialist. Cases like this are hard when you do everything right but still are left with more questions than answers. I would also recommend talking to your vet about trying a liver supplement such as Denamarin if Daisy is not already taking one. Feel free to leave an update as things progress. Wishing you both nothing but the best.
Our dog is old and his old bones aren’t what they were. However, up to now he had still enjoyed going for a walk and had a big appetite. In the last couple of weeks he’s eaten less and less, and now is not even interested in his treats. He’s a big dog and was 38 kg a few weeks ago but is now down to 34.4 kg. He still likes a walk each day (though it’s usually less than 30 mins, instead of what used to be an hour or more) and drinks normally. Blood tests today revealed a very high ALP level; the vet said it was “in the thousands” (I spoke to him over the phone and it wasn’t a great line) with elevated ALT (I think) levels too. The vet wants to have him in to do an ultrasound and a liver biopsy but he’s over 14 years old and I wouldn’t like to put him through that, especially as he probably doesn’t have much longer anyway. It’s possible he may have had a seizure or TSA recently. He spends most of his time sleeping these days. Is it time to say goodbye?
Hi Mike,
So sorry to hear about your dog’s recent decline. The amount of weight he has lost plus the elevations in ALP (and maybe ALT) are definitely concerning, especially coupled with him not wanting to eat much of anything. I agree with your vet that an ultrasound and biopsy would be the next steps if you wanted to look for answers, but it is also perfectly fine for you to decide that those aren’t things you want to pursue at his age. You know your dog well, and you know what is best for him.
In terms of thinking through when it may be time to say goodbye to him, there is usually a window of time in which euthanasia may be the best choice. Based on what you have said, he may be approaching or already in that window, but I can’t tell you that for sure. Sometimes filling out a quality of life scale or having a conversation with your vet (or an end-of-life-care vet) can help bring some clarity. I’m including links to a few articles that you may find helpful too.
Thinking about you as you wrestle with this difficult decision. ❤️
Here are those links:
1) When to Euthanize A Dog With Liver Failure: A Vet’s Advice
2) Using a Quality of Life Scale for Dogs
3) Preparing for Your Dog’s Euthanasia: 10 Thoughts for Peace
4) How Will You Know When It’s Time to Euthanize Your Dog? 5 Caring, Heartfelt Messages
Hello,
My Siberian Husky Chloe just turned 9y on November 2. I took her to the vet in October since she was having weekly diarrhea with only one case of vomiting each episode. I had a full panel blood test done in October which resulted in ALP just over 1500. she was prescribed a low fat diet which would not settle well with her tummy so I opted for another brand of food that she did do well with to ease the diarrhea symptoms. i followed up with the vet 3 weeks later to do a single panel test and the ALP levels dropped to just over 1000. However her globulin levels were 5.2 over 4.8. She also started to become severely flatulent. However after adding a probiotic supplement to each meal, her flatulence has subsided to just some rare occurrence. she has no symptoms as of today other than mild flatulence and random gulping noises. I assume the gulping is from acid reflux. Also her stools are no longer diarrhea but in the middle of firm and diarrhea. it looks normal but when picked up, the texture feels like loose playdough or cake mix. The vet wants to do a bite test and an ultrasound but I feel as though a wait and see is more appropriate considering her symptoms are very mild. what are your thoughts?
Thank you and regards,
Jeff
Hi Jeff,
Sorry to hear about Chloe’s recent tummy troubles and elevated ALP. It is great that her ALP is going down and her stools are improving, but it sounds like she isn’t quite back to normal yet. Whether you decide to give it more time or pursue further diagnostics at this point is ultimately up to you. I agree with your vet that a bile acids test and ultrasound would be the next logical steps should you want to dig deeper into her significantly elevated ALP. But I also understand where you are coming from with wanting to give it more time since the ALP is trending downward and her symptoms are improving. What you decide to do depends in part on how aggressive you want to be and how the results of the bile acid testing and liver ultrasound could change her treatment and monitoring plan and/or her prognosis. Since I haven’t been involved in her case, I can’t give you more specifics about the pros and cons of waiting vs. doing the testing, but I think it is worth discussing with your vet as he or she would likely have some insights.
I hope you feel peace about whatever decision you make and that Chloe keeps improving!
My 14 and 1/2 year old jack russell has been on Rimadyl for the last 2 -3 years for his arthritis. As part of his heath check he had his bloods tested and his ALP has come back at 566. His other liver and kidney tests are all normal.
Is 566 on the high side and something to be concerned about and could this be caused by the Rimadyl? What should our next steps be?
Hello Newts,
I’m sorry to hear that your pup had an elevated ALP at the last health check, but thankful that the other liver and kidney values are still normal. ALP elevations are a fairly common finding in older dogs and can have a variety of causes, which can make it challenging to decide how worried to be. Rimadyl has been known to contribute to an elevated ALP in dogs, so it could potentially be the cause. But so could benign nodular hyperplasia (a common condition in older dogs) and many other things. Without being able to examine your dog, I can’t give you any concrete recommendations about the next best steps. However, I do think it is worth talking to your vet about what he or she thinks would be best. Sometimes monitoring the values for now is all that is needed. Other times that might be changing to a different pain medication, adding in a liver support supplement like Denamarin, pursuing further diagnostics, etc.
I hope that you are able to have a good conversation with the vet and leave feeling confident in whatever the plan ends up being.
Hello Dr. Buzby:
Hope you are well. My Male dog is 12 years old and has a high alp of 270 and 160. These elevations started last year. Last years numbers were: Mild elevation in albumin 4.3 (2.5-4). ALT 169(0-120), ALP 159 (0-140)
The doctor says that he would have to take ursodiol his whole life, is this warranted, are there any other alternatives to naturally lower these numbers? Do natural liberal supplements work like Zesty paws brand for liver? I haven’t received much explanation as to why this is happening just that it’s a progressive disease and age related. No other alternatives or explanations offered. Please let me know what I should do and what questions I should ask because the responses I receive are very brief but without much explanation. I’ve read gastrointestinal issues can cause these elevations as well. What would you recommend be our next step?
Thank you so much for your attention,
Hi Marlene,
I understand your concern with your pup’s elevated liver enzymes and applaud you for doing your research and looking for answers. Thankfully the elevations are still mild at this point, but it is good to keep them on your radar. The list of causes of elevated liver enzymes is unfortunately quite long, which can make it challenging to pinpoint an exact cause in some situations. I’m actually in the middle of writing another blog about elevated liver enzymes, so you can be on the lookout for that one too. But in short, if you want to dig a bit deeper into why these numbers are elevated, you may want to consider making an appointment with a veterinary internal medicine specialist. They should be able to do some additional diagnostics (ex. liver ultrasound, bile acids test, etc.) to get a better idea of what is going on, and then create a treatment and monitoring plan. Since the internal medicine specialists focus just on diseases of the internal organs, they are often able to give more in-depth answers than a general vet, who focuses on disease of the whole animal.
In terms of supplements, I don’t have any experience with the Zesty Paws liver supplement, but it look like it contain milk thistle, which is a popular liver support ingredient. However, my personal favorite liver supplement, and the one I frequently recommend for my patients, is Denamarin. It combines milk thistle and SAMe to help support the liver. Sometimes Denamarin does help lower, or at least stabilize the liver values, so it (or a similar product) could be worth a try!
I hope you are able to find some clear answers and a plan that you can feel confident in. All my best.
Thank you so much for sharing your knowledge. My 12.5 year old golden retriever had a scary episode in July with the appearance of total fatigue and no interest in food. The vet ran blood work and his WBC was 79.1K with Neutrophils of 71K, ALP 174. He started acting normal again and we repeated blood work which showed WBC 14.9K but ALP increased to 207. Vet did a crude abdominal ultrasound as they are not experts but said his organs looked good. He was acting normal except for more particular about food so we decided to watch & wait. Three months later he had two morning seizures so blood work repeated and WBC up again to 40.2K with Neutrophils 35K, monocytes 1.6K and ALP up to 497. His glucose was low at 60. ALT has been in normal range. My vet is thinking insulinoma but I’m wondering why she isn’t worried about ALP.
My pup had an emergency splenectomy two years ago for a massive bleed which turned out to be a benign football sized spleen tumor. Could the absence of a spleen cause elevated ALP? Or WBC? Platelets are high too (500-665).
My vet suggests rechecking glucose with no mention of ALP. I’m not ready to say good-bye so this is a hard road to navigate.
Hi Pam,
I understand your concern for your pup and think it is great you are advocating for his health and well-being. Without examining him myself and playing a personal role in his medical care, it is hard to make specific recommendations. The ALP is not very liver specific and can become elevated for any number of reasons. This may be why your vet is more focused on the obvious issues. They are probably hoping that if they find the cause of the abnormal blood cell counts and glucose, then it will also explain the increased ALP. Hoping you can get some answers quickly and find the best treatment options for your Golden boy. Don’t forget you can always ask about a referral to a specialist if needed. Best wishes for a positive outcome!
Hi Pam! Did your pup ever get a diagnosis? My girl has high wbc (neutrophils) and high alp. The vet is trying to figure it out. We are doing an ultrasound.
Hi
Our 11 year old cairn/ yorkie cross had ALP of 2613 in July
We changed to heptatic dog food and cut out treats etc
Yesterday we were told the levels were 4400
The vet hasn’t suggested what the cause is or what this means
She is otherwise healthy for her age and loves to get out for walks
Is there anything you can suggest
Hi Dee,
I am sorry your senior pup has these elevations in his liver enzymes. It sounds like you really have two options. One would be to continue to monitor and offer palliative care. The other is to proceed with more in-depth testing to try and get a diagnosis. This could involve more lab work, ultrasound, or even contacting a specialist. I think it would be best for you to have a more detailed conversation with your vet. Make sure to voice your questions and concerns and be honest with your feelings about how things are progressing. Hoping you can get some answers soon and find the best way forward. Wishing you all the best.
My Ivy girl has been very active and healthy.. She will be 12 in 3 months. She had her first ear infection and while at the vet we decided on her senior panel. Since 2021 her ALT jumped from 36 to 350. ALP from 21 to 500. She eats well, poops great and drinks plenty, pee is good… No signs of anything other than my assumption that older aged has slowed her down.. I don’t know if these numbers are hugely significant since the vet said her enzymes are ‘slightly’ elevated. She lost her umphhh ! I am hopoing for the best . I love that girl and cannot stand the idea of losing her right now… Does Denamarin help or is she past that?
Hi Buck,
I understand your concern for your senior girl and this slow rise of her liver enzymes. There is no way to know for sure if Denamarin will help, but it certainly shouldn’t hurt! If your vet is willing to prescribe it, I would say give it a try. I have seen supplements do wonderous things for situations just like yours.
Thank you for your article. I would appreciate your thoughts on our boston terrier Alice. Her ALP levels were normal in 2019 but from 2020-2023 they have jumped each year from 162 to 506 to 781 to 977. We had imaging done a couple of years ago and they identified a mass in her gall bladder. Rather than pursuing invasive treatments we have been seeing how she does because she acts normally. The .vet suggested we could try Denamarin to see if that helps with her levels. What are your thoughts? Thank you very much!
Hi Jennifer,
I understand your concern for Alice and these increasing liver enzymes. Without examining her myself and knowing all the details it is hard to make specific recommendations. I do love Denamarin and frequently prescribe it for my own patients. I am curious to know exactly what the “mass” was that was seen on ultrasound. It may be possible to have the gallbladder removed and improve your pup’s prognosis depneding on what the actual diagnosis is. Here is a link to another article with more information: Gallbladder Mucocele in Dogs: What You Need to Know
It may be time to think about a consultation with a specialist. Hoping you can find the best way to keep your sweet girl happy and healthy for many years to come. Best wishes to you both!
Hello Doctor, my girl Sage is 8 1/2-9 years old. She’s part dachshund part don’t know. I rescued her from getting euthanized. She started panting hard about 9 months ago and I was worried about her heart because she had gained weight when I had a knee replacement. Took her to 2 vets and finally to a third vet. As soon as he saw her, he said that she looks like she has Cushings. So we tested her.. she tested positive, well it also turns out she has diabetes and her Alp number is super high at 2400, her Alt is 398 . So she’s on insulin. He prescribed the liver supplement but I wanted to know if that’s all we are going to do for her liver. He said yes, because he didn’t have alot of hope for her liver numbers. Well I have an autoimmune liver disease that I take Ursodiol. My daughters dog had liver issues and her vet prescribed Ursodiol. I asked about Sage getting on that and he said he’s never prescribed that for liver issues. Well it’s helped me and it helped my daughters dog. So I told him that I wanted to try it for her. We will be getting our blood work again in a few days. But in the past 3 weeks cushings has started to mess with her so today I’m starting her on Trilostane. Im going to have an ultrasound done on her next week. Im hoping for miracle. I don’t know what else to do for her. Trying to find a good dog food for her but there’s seems to be alot of bad food out there. Boy are we tired! Thanks for reading Georgia
Hi Georgia,
I am glad you were able to get some answers and now know exactly what your girl is dealing with. I hope the ursodiol will help decrease the elevated liver enzymes and offer your pup a better quality of life. Sage is lucky to have you advocating so strongly for her health and well-being. Thank you for sharing your experience with us. Wishing you both the best and keep up the good work!
Georgia, my 10 year old has had similar symptoms. Panting for a couple of weeks and then the first seizure. She is is now on Keppra, but still has heavy panting. Her AlP is at 370 and the vet wanted to test for Cushing but I’m not sure. Did you find out any more on your dig?
My dog is 12 years old and has had IBD for 6 years. She was on low dose budesnoide for the last 6 years which she never had any GI flare ups and recently took a turn for the worse. She suddenly went blind (SARDS) and has bloody diarrhea that ended her in urgent care. She has had two abdominal Ultra Sounds which which were normal but her ALP is at 1900 and shows no signs of coming down. On her last blood work her ALT was 143 ( slightly elevated) but she is on low 4 mg of Medrol and thyroid medication. The vets really don’t say much. Could all this be form the steroids? If she has autoimmune then how is it treated?
Thank you!
Hi Jan,
I am so sorry your senior girl has been through so much. These elevated liver enzymes could definitely be just due to the steroids. Unfortunately, the risk of side effects may be worth it for the benefits they provide. If there was an autoimmune disorder present, the treatment would be to suppress the immune system. This is commonly done using steroids. So, the odds of this being the cause is probably pretty low. I hope your girl can keep fighting and is able to make a full recovery. Sending you all my best. ♥
Hello,
First off I want to say this page has been super insightful and given me so much information about high ALP in dogs, so thank you!
My 11 year old lab mix recently got a routine blood panel test and a couple things came back. His ALP is higher than the normal range at 318, his Total Bilirubin was 0.4, and his CPK was elevated at 954. Lastly, his urinalysis test came back as dilute at 1.007 and trace occult blood. Everything else was in normal levels. My vet said it’s possible that it could be Cushing’s so she wants to do a test for that, but he’s not really exhibiting any symptoms of it (he’s always had a big appetite, always been a big water drinker, no skin issues etc). I think it’s worth doing the test but wondering what other possibilities it could be based on those combinations of elevated results above?
Thank you so much.
Hi Amanda,
I understand your concern for your senior guy and these elevated liver enzymes. I do think the Cushing’s testing would be a good idea. There are just too many other possibilities to list them all, but the most common would be primary liver dysfunction or a mass in the liver. If I had to guess I would say your vet will probably recommend x-rays or an abdominal ultrasound at some point to see what the liver looks like. I hope you get the answers you need to move forward with the best course of treatment. Wishing you both the best of luck for a positive outcome.
Hi Dr. Buzby, thank you for sharing this story. I’m an ER physician myself and you’d think I’d be calm and collected with health news – but not when it comes to Marlowe. She’s an 11 year old Shih-Poo and I’ve had her since my first year of medical school.
She’s in great health physically but over the past year I’ve noticed what I thought (and my vet agreed) were lipomas. Some blood work revealed an elevated ALP – first 403 in March and now 560 in July. Today her lipase came back at 780 and her cholesterol at 8.9.
Her remaining liver function tests, albumin, bilirubin, glucose levels, creatinine, and CBC were all normal, but I’m very worried about her blood work. She has had increased thirst and a rounder tummy lately.
She had a liver ultrasound and it was enlarged but showed no masses. Her adrenals looked ok too. Does this mean it’s a pituitary issue?
Her last Urine SG was concentrated, so the thought of cushings was put aside, but I wonder if that’s what she has. She’s a very happy and healthy girl and I’m so hoping there’s a benign answer for all of this.
Any insight about what could be contributing? Any chance there’s a dietary or exercise fix?
My primary vet offered referral to the vet general surgeon which I was thinking about.
If you had any thoughts about what your next steps would be if she was yours, I’d be super grateful. I’d do anything for my dog.
Hi Gemma,
I understand your concern about this elevated ALP in Marlowe. You are right that these symptoms could be early signs of a pituitary dependent Cushing’s disease, but not necessarily. Have you discussed Cushing’s testing with your vet? Also, it might be worthwhile scheduling a consultation with an internal medicine specialist. I feel like you are on the right track with the diagnostics that have already been performed. Your girl might also benefit from a trial course of a liver supplement/protectant such as SAMe, Milk Thistle, or Denamarin. Your vet probably has a favorite they keep in the clinic and recommend to their clients. Hoping you can get to the bottom of this puzzling situation. Wishing you and Marlowe the best for a bright future. Feel free to keep us updated on how things progress!
Huckleberry, 9, m/n, raw-fed pittbull who is 107lbs of perfect love bug.
Hx of EVERYTHING THAT CAN GO WRONG DOES GO WRONG as he is an ER and specialty RVT’s dog 😛 typical.
Parvo (type c) as a fully vaccinated at 1 yr old (almost lost him!) anaphylaxis for no reason we could find, ruptured ear drums, foxtails, pneumonia, torn and repaired ACLs, allergies….the works.
He is my $40,000 dog.
polyuria/polydipsia for 1 month.
bloated.
grunting. restless and trouble sleeping.
hesitant to give him carprofen as my most recent BW was 2.5 yrs old.
Cushing’s? peritonitis? ascites? My mind when to cancer.
Brief u/s showed enlarged but healthy spleen (visible on the right side) , no free fluids or abnormalities.
Only BW that wasn’t WNL were:
RBC 8.86 5.39 – 8.70 M/μL H
Hematocrit 60.8 38.3 – 56.5 % H
Hemoglobin 21.2 13.4 – 20.7 g/dL
ALP 264 5 – 160 U/L H
Chloride 107 108 – 119 mmol/L
Cleared for tram/carprofen and it’s been a little better. He can relax. The tramadol helps him a LOT (not super common ya) and has even reduced the drinking–which our doc said can be from stress and a sort of self-soothing thing.
Can the bloating and thirst be the very start of Cushing’s?
He does have some thinning skin on his abdomen.
They told me to not worry about it yet as it’s a difficult and expensive Dx but I can’t help but think that’s what it is.
Maybe it’s the case of “you know more than the average joe so you assume the worst” but it’s hard not to with Huckleberry as he had an affinity for near-death experiences his entire first 5.5 years of life.
He one time HIT A CAR.. HE… hit the car!! I almost fainted.
If I wanted to pursue these weird symptoms, would the next step be a Cushing’s day at the vet?
Full ultrasound with IM?
Do you have any suggestions?
This was helpful to read and I appreciate you.
Thank you for doing what you do.
Hi Cole,
I agree it is SO HARD to be subjective with your own dog! We know too much and sometimes it’s just enough to be dangerous. LOL. Of course, I have to give you the disclaimer that since I haven’t personally examined your pup I can’t make specific conclusion and recommendations. With that being said, this could be the early stages of Cushing’s. The problem with that disease is we usually only treat if symptoms are present even if you get a positive diagnosis. You are treating to get the symptoms to resolve. So, I’m not sure that even if you get a positive Cushing’s result you would want to risk the possible side effects of the medication to treat bloating and increased thirst. There really isn’t a right or wrong answer at this point. If having “answers” will give you peace of mind, then I say go for it. Just know you may spend the money and time and end up exactly where you are right now. I wish I had some super helpful advice but at least you’ll know you aren’t alone and I’m keeping you in my thoughts. Wishing you and Huckleberry the best. Feel free to keep us updated!
Hello. Our 10 year old Maltipoo has ALP of 1400. All other values were in the normal range. He is on 3 different eye drops. Latanaprost, NeoPolyDex, and Dorzolimide. Can these eye drops affect ALP?
Thanks,
Hi Steve,
I understand why you are concerned about this elevated ALP in your senior pup. Eye medications can definitely have systemic side effects, but they are usually mild. Specifically, the “Dex” in the NeoPolyDex is a steroid and steroids can cause elevated liver enzymes. But the dose that is in the eye medication is VERY small and even if it had an effect on the liver, I would not expect it alone to cause an increase of 1400. To find the cause of this abnormal ALP results I think you will need to look elsewhere. You may want to talk to your vet about what the next best step would be (abdominal ultrasound?) to get a diagnosis. Wishing you the best of luck!
My 8 year old Dalmatian has ALP of over 2000+ but doesn’t have cushings has he was tested 3 weeks ago. What else could cause this issue? It’s been this high for over 2 months. He had a quick ultrasound on his liver when he was having a CT for a spinal issue. But vet couldn’t see anything.
Hi Katie,
I understand why you are concerned about this extremely elevated ALP. I am glad the ultrasound was normal but feel like this may still need some additional investigation. Unfortunately, there are just too many possibilities to list them all. Some of the first things your vet may try to rule out are tick borne diseases, an autoimmune disorder, atypical Cushing’s disease, or damage from a toxin. Don’t forget that you can always ask for a consultation with an internal medicine specialist if needed. How is your sweet boy doing today? Hoping things have started to turn in the right direction. Praying for a positive outcome.
I just learned our almost 12 year old, small, mixed breed (chiweenie terrier) dog has very elevated ALP, plus elevated ALT and GGT. We had the blood work done because his water consumption has grown enormously. This has led to incontinence due to his very full bladder and him having less control at his age. He has an ALP of 2191, an ALT of 370 and a GGT of 43. All other blood chemistry markers were normal. He’s pretty healthy otherwise, still has a great appetite and still loves his play. He is slowing down a bit all the same. Long walks are harder for him.
My vet told me the ALP was off the charts, but I didn’t realize how abnormal until I read the “elevated” ALP values people have posted here for their dogs. Now I am even more worried.
Our vet said an ultrasound would be the next step, possibly followed by a biopsy, but I really don’t know that I would want to put him through that and the outcomes are likely limited anyway. I’m in a quandary as to what we should do next, other than watch and wait, perhaps retesting in 6 months.
Hi Bruce,
I can understand your concern with your senior pups elevated liver enzymes and increased thirst. It can be difficult to know how deep you want to dig to find the reason for those changes. I would agree with your vet that an ultrasound is often the next logical step in the search for answers, but I also don’t think there is anything wrong with you deciding to recheck the values in a few months. A lot of it really does come down to how badly you want to know the “why” behind the enzyme elevations and how that information would change the plan for your dog’s medical care. If you decide to take a wait and see approach, you could always ask your veterinarian about liver-support supplements like Denamarin, SAMe, or milk thistle. They probably have a favorite product that they think works well. I hope you are able to find clarity about how to proceed. Please feel free to keep us updated!
Last year the vet found my dog’s ALP to be elevated. It was over 1000. I was told to wait a year and see if had changed. On 5/18/23 they rechecked, and her ALP is 1581. They prescribed SAMeLQ 225 tabs. I’m to take her back in 3 months. No one said anything or asked questions about what she eats. Surely her diet would be a good starting point in helping reduce her ALP? She is a seven-year-old Cairn Terrier. She doesn’t overeat, but her belly is large.
Thank You.
Hi Laura,
I understand your concern for your dog and this abnormal ALP result. While diet can be important, it probably will not have much effect on lowering the liver enzymes unless there is something in the food causing the liver to become aggravated in the first place. I am sure if the SAMe supplement has not helped to reduce the ALP at the next recheck then your vet will move forward with additional testing. Since you mentioned your girl has a large belly, they may want to test her for Cushing’s disease. It is possible they might also recommend additional blood work or even an abdominal ultrasound. I hope you can get some answers and find a clear path forward with treatment. Wishing you both the best and feel free to leave an update if you have a chance.
Today I took my Coco in for her yearly shots. Since she had finished the SAMeLQ 225 tablets, I asked to have the ALP rechecked. It’s now higher. She has been on Hills liver dry and a little wet dog food. I am to take her back in a few months for another recheck. I’m concerned that it’s Cushings. Is there anything else I can do?
Regards,
Laura
Hi Laura,
I am sorry Coco’s ALP is still elevated despite the SAMe supplement you have been giving. If you have lingering concerns and want to go ahead and pursue further testing, I highly recommend you discuss this with your vet. As long as you understand it can take some time to get a diagnosis and are willing to commit to the financial aspect of investigating, I see no reason why your vet would not be willing to schedule some diagnostic tests. Many times, veterinarians will err on the side of caution and give things some time because we get fussed at about how much testing costs. I am not saying this is the reason your vet has recommended another recheck in a few months, but it could be. Without playing a personal role in your dog’s medical care it is hard to make specific conclusions. It is never wrong to voice your opinion and ask questions until you are comfortable with how things are proceeding. Hoping you can get some answers soon and help Coco start getting back to living her best life.
I am taking my 14 year old peak-a- tease in for an abdominal ultrasound. He had geriatric blood work done and it was Overall good but his ALP, was at 537 in August 2022 and now has increased to 1699. He is healthy otherwise. I just feel nervous as to what we might find in the ultra sound, if anything I suppose. Reading these other posts have been helpful.
Hi Christina,
I understand your concern for your senior guy and this abnormal liver value on his blood work. I am glad you decided to move forward with an ultrasound in hopes of obtaining some answers and possibly a diagnosis. What did you find out? Praying for good news. Feel free to leave an update if you have a chance.
My dog’s ALP level was 64 in October and as of last week was 223. She’s also had high ALT levels for a while. Last week they were 392 and that’s after six months of specialty food and taking denamarin.
My dog’s ALP went from 64 in October to 223 last week. She also has high ALT level at 392. Her MCH and MCHC levels are low.
I’m not sure what any of this means. She’s almost six, is a mixed breed, and has lots of energy.
Hi Christine,
I understand you have concerns about these elevated liver enzymes on your dog’s blood work. It can be difficult to find a cause without investigating further and doing some additional testing. Please make sure you are discussing this with your vet. They may recommend abdominal ultrasound, more lab work, or even a consult with a specialist to try and make a diagnosis. I am hopeful you will find the answers you need to ensure your girl is happy and healthy. Best wishes and good luck!
I have a 10 yr old Great Dane that has severe v. tach. The vet wants to put her on Propafenone as the solatol is not helping on its own. However she has a alp of 685 and I understand that the new drug should not be given with pre-exitsting liver damage. I was looking for a second opinion if this drug should be used given the circumstances? Any information would be helpful as I have worn out the internet trying to find any type of answer.
Thanks for any insight
Hi Yolanda,
I am sorry your Great Dane is struggling with chronic V. Tach. I have to admit I do not have much personal experience with treating this condition and can’t give you advice on if the Propafenone is a good idea. It is hard to weigh the pros and cons when thinking about the heart arrhythmia, possible liver dysfunction, and the fact your pup is already of advanced age for her breed. This is where I would suggest scheduling a consultation with a specialist. A veterinary cardiologist or internal medicine specialist would be a wonderful resource for this situation. Hoping you can get the answers you need to make the best choices for you and your sweet girl. Bless you both.
Our 11 yr old Husky showed an ALp of 176
5 months ago. In the past 3 days she has had a sudden onset of blindness, from seeing to not seeing . Trouble getting into a vet. Could this be an infection that if treated soon could stop or reverse her sudden loss of eyesight?
Hi Barbara,
Yes, this sudden onset blindness could be due to an infection. There are also many other possible causes such as high blood pressure, diabetes, cancer, idiopathic retinal detachment, etc. When dealing with eye issues, time is always of the essence. I highly recommend you have your dog evaluated by a vet as soon as possible, even if that means taking her to an emergency hospital. Praying for a positive outcome for your sweet girl.
Wow, this was such a great article! The most detailed one that I have found on the internet so far related to ALP. Thank you for this and thank you for allowing us to ask questions!
I was able to cross reference all these other levels (ALT, GGT, and total bilirubin….and glucose, cholesterol, albumin, and BUN) to the blood work we have done. Luckily my 10 yr old (almost 11yr old) cocker spaniel doesn’t have the other levels high. They are normal except for most recently higher amounts for Lymphocytes (5,256) and Cholesterol (375). The vet prescribed antibiotics (Cephalexin 500mg – 24 pills) because when he checked him he said he had an ear infection. They didn’t do the detailed ALP test to show the 3 levels. But the ALP for my dog is at 1,699. What I find interesting is that is has gone up over the years….
In May 2018 the ALP was 187, Nov 2018 the ALP was 291, in July 2019 it was 785, in Jan 2020 it was 1,215 and now in March 2023 it is 1,699. Does that sound alarming? He drinks a lot of water. He has a lot of energy. I haven’t had any other tests done on him but I am wondering if it has to do with Cushing’s Disease because he has a pot bellied appearance. I will read up on that. The vet that I took him too said the high ALP could be related to muscle pain or teeth tartar. Would love to get a second opinion? Thank you Dr. Buzby!!!
Hi Tanya,
Thank you for the kind words and positive feedback about the article! Of course, since I haven’t personally examined your dog, I can’t make specific conclusions. But I too would be a bit suspicious about Cushing’s disease, especially since you mentioned the potbellied appearance. It might be a good idea to talk to your vet about pursuing an abdominal ultrasound. This way you can get a better look at the liver itself and evaluate the other internal organs for abnormalities. Since you mentioned reading up on Cushing’s, I will attach links to other articles with more information. I am hopeful you will find the answers you need to make sure your sweet boy is well taken care of. Best wishes and good luck!
1. Cushing’s Disease in Dogs: Symptoms, Diagnosis, Medications
2. Trilostane for Dogs With Cushing’s Disease
Hi Dr. Buzby,
I’d like your opinion. My 10 year old affenpoo had his senior blood work done. I took him in because I noticed he’d been peeing more frequently. I thought maybe old age but let’s get him checked out. All blood work, red and white blood cells, and liver enzymes except ALP came back normal. His ALP was 1400. They also did an ultrasound of the bladder and a urine analysis. Bladder was fine. Urine analysis not so concentrated. They want to a low dose dexamethasone suppression test as the next step. But from what I’ve read there seems to be other things that could cause an elevated ALP and would also result in a positive pituitary cushing’s disease. After reading your article I wonder if the next best step is an abdominal ultrasound?
My worry is is receiving a positive cushing’s disease when something else may be ongoing. Any thoughts would be appreciated.
Sincerely,
Melissa
Hi Melissa,
I understand your concern with these abnormal results in your senior pup. Without playing a personal role in your dog’s medical care I can’t really make specific recommendations. An abdominal ultrasound could be a good idea and definitely won’t hurt (other than costing you some money). You may also want to consider scheduling a consultation with an internal medicine specialist. From my point of view, more information is always better. I hope you can find the answers you need to get to the bottom of this puzzling situation. Wishing you both the best and praying for a clear path forward.
My old Vet accidentally overprescribed metronidazole an antibiotic to my dog Cooper for 30 days for high ALP, 3 times over normal and gallbladder wall thickening 2 mm. . I asked him any side effects, he said no. 21 days later having metronidazole Cooper couldn’t walk, I tried to make appointment with my local vet, they had no openings. So I took Cooper to Emergency Hospital. I told them Cooper was taking metronidazole.First vet at emergency hospital in Kalamazoo told me he a back sprain, prescribed painkillers and muscle relaxers. . Two days later Cooper was having seizures, drooling, eye twitching and couldn’t stand, I took him back to emergency hospital, second vet said he was a brain issue. I asked both emergency vets could it be toxic, they said no. I had him euthanized. Three days later my local vet called and said he overprescribed metronidazole for his body weight 29 lbs (dose of metronidazole was 500 mg twice a day for 30 days) and for too long, he said Coopers symptoms were caused by the drug reaction to the metronidazole , he didn’t have a back sprain or brain issue. The prescribing vet for metronidazole said he made a mistake and prescribed too high of a dose. The metronidazole could have been stopped and he probably would have been okay. I’ve been crying for 4 weeks. I don’t trust vets anymore.. I didn’t know and no one told me metronidazole could cause severe drug reactions, especially at high dose. My best friend is gone. I am broken and feel so quilty about euthanizing my best friend.
Dear Bruce,
My heart aches for you with your tragic loss of Cooper. I understand why you are grieving and wish I could take away your pain. You did what you could to make sure your boy didn’t continue to suffer, and I am certain he knew how much he was loved. I hope it has helped to be able to share his story with us and pray with time your heart can begin to heal. May the memories of all the good times you shared stay with you always. Wishing you comfort and peace. Bless you. ♥
My almost 10 year old cocker spaniel had knee surgery in January. ALP then was 340. doc was ok with that number as he’s an older dog. On Feb 10 he had a follow up and weighed 39 lbs. I noticed weight loss, loss of appetite and changes in stool. Took him in yesterday and repeat blood work shows ALP 8000. Dog is eating and drinking, good spirits, hasn’t had a bowel movement yet. Dr is keeping him on fluids and running more tests. He said he’s only seen this 1 other time. Thoughts on this number? I while heartedly trust my vet but just doing a little reading up on high numbers.
Hi Jennifer,
I am sorry your senior guy is having issues with elevated liver enzymes. While this high ALP is alarming, it may not be anything serious to worry about. There is really no way to know for sure without a definitive diagnosis. Since I haven’t examined your pup, myself, I can’t make specific conclusions. I do think running more tests sounds like the best course of action. I am confident your vet will try their best to keep your sweet boy happy and healthy. Praying for answers and a clear path forward. Feel free to leave an update if you have a chance.
My almost 12 year old Lab, Carley, two months had an episode where her gait was affected. She seemed like she couldn’t walk right. This had happened 6 months previously as well. My vet examined her after the first episode, When it happened again she suggested doing lab work, CBC and CM.
Her lab work was all good except the ALKP was 570 and ALT was 626. I started her on Denamarin. Lab work was repeated in 2 months and the ALKP is now 1166 and ALT is 739.
I am for the last week feeding her a Liver Care diet. Last night she started having a twitching most of the night and seemed more restless.
I have been in contact with my vet last night and today. She seems to be doing better today. Pretty much her normal self. The way things looked last night I felt like she might need to be euthanized. The vet suggested starting her on Prednisone 5 mg but after reading about prednisone it looks like it might cause the ALKP to increase more.
I plan to call her back now to ask about that. Any ideas or suggestions would be helpful. Thank you.
Hi Linda,
I am sorry Carley is having issues with elevated liver enzymes. You are correct that prednisone can cause these liver values to increase more depending on the situation. Did you vet mention what they are trying to achieve with the steroids? If an immune mediated disease is suspected, then prednisone would be the best way to start treatment. While you are discussing these concerns with your vet, you can also ask about some additional testing such as blood work to check bile acids, tick titers to rule out diseases like leptospirosis, and possibly abdominal ultrasound to make sure there is no mass present in the liver. Without examining your dog, myself, it is hard to make specific recommendations. I hope these suggestions will be a good starting point and will help guide the conversation a bit. I am hopeful you will find the answers needed to find the best course of treatment for your sweet girl. Praying for a positive outcome. Best wishes and good luck!
Dr, Buzby,
Our 9 year old Sheltie had an elevated ALP level in September of 322 and ALT of 295. Took Milk Thistle and rechecked this past week due to an abscess caused by secera an infected tooth and the ALP had shot up to 800 and ALT dropped some to 232. We are doing an ultrasound next week but I can’t help but worry it will uncover something bad. He does not act sick, is playful, eats well and hasn’t had any changes in behavior or eating drinking. The vet mentioned Cushings and arthritis being a possible contributor but my question is could it be all dental related? His teeth weren’t great in September but he now has severe dental disease, which could explain the spike from 322 to 800. (Vet stated his genes cause him to have excessive plaque build up even with frequent dentals at the vet.) If it were cancer, wouldn’t there he be exhibiting symptoms? Trying to stay hopeful for our sweet boy……
Hi Susan,
I understand your concern with these elevated liver enzymes in your Sheltie. I am not sure that dental issues alone would cause the numbers to be this high, but it definitely could have contributed to the recent increase since September. I think ultrasound is a great next step in this investigation. Did you get some answers? I am very curious to know what the results showed. Praying your senior girl is feeling ok and there is a clear path forward with treatment. Feel free to leave an update if you have a chance.
We adopted our dog about 2.5 years ago when she was about 3 years old from our local humane society. About five months ago we had. a baby. At the same time we had a baby, we noticed our dog was drinking more water, peeing more, and her legs would shake at random times. We thought it was a behavioral issue related to the baby, so we put off getting her to a vet. Last week, we took our dog to a vet. Her physical exam was fine, but in her blood work they found elevated ALP and GGT. Our dog also went from 24 pounds in July to 17.4 pounds in January (her ideal weight). The vet recommends a Cushing’s test. Could it be anything else?
Hi Kat,
I understand your concern with these elevated liver enzymes in your pup. Yes, these abnormal results could be something else other than Cushing’s, but this is also the testing I would perform first. You have to start somewhere, and this is the most logical testing to begin with. I am sure if the Cushing’s test is negative your vet will recommend the next step. You may be looking at more lab work and possibly an abdominal ultrasound. Try not to worry yourself too much in the meantime. I pray you can take things day by day and will have the strength to navigate the unknown road ahead. Hoping for the best for your sweet girl and congrats on the new baby!
My senior (will be 13 in May) pit mix, Jazmine, just went in for her annual checkup, which includes full blood panel at her age. Her ALT was 378 and her ALKP was 1429! Aside from having a small heart murmur, she is very healthy. But she is starting to slow down a lot. She also has an odd occasional cough. Like a choking sound. My vet put her on Denamarin Advanced, and will recheck in 8 weeks, unless something changes. My first baby passed away at 13, out of nowhere. She was fine one day, throwing up the next, rushed her to the vet thinking pancreatitis, because she’d had it before, they kept her overnight, and called the next day for me to come in. They said her blood count was dropping so fast, she wouldn’t make it through the day. I still have no idea what happened.
Hi Katie,
I understand your concern about Jazmine and these elevated liver enzymes. I am glad you had her examined by your vet and have started her on the liver supplement. If things do not improve as hoped, the next step will probably be x-rays or ultrasound. If at any point you want to proceed with more diagnostics instead of waiting for the recheck, don’t hesitate to let your vet know. I hope you find the answers you need to help restore your sweet girl’s health and quality of life. Praying for a positive outcome.
My 11 year old beagle has a ALT of 512, AST of 92 and ALP of 5901.
She’s been on Denamarin for about a month since the tests were done.
She recently started not eating her dry food – she eats it and then spits it out, so we switched to canned food (prescription). And now has a rash on her abdomen as well…
Any thoughts on next steps – or things to look for? Can older dogs with this high of levels be helped with Denamarin typically?
Hi Amy,
I understand your concern for your Beagle and these elevated liver enzymes. I have seen Denamarin help cases like this but of course many times it requires additional treatment. It sounds like it may be time for further investigation. Make sure you are staying in close contact with your vet and keeping them updated. They may decide to do additional blood testing like checking bile acids, screening for tick borne diseases, or ruling out other issues like leptospirosis. Ultrasound of the liver is also a common next step. If at any point you feel the need to reach out to a specialist (internal medicine) just ask your vet. They should be able to make the referral. I hope you can find the answers you need to help your senior girl continue living her best life. Feel free to leave an update if you have a chance.
My 9 and 1/2 year old rescue mix received high ALP scores about six months ago. She’d gained some weight with the rest of the household through covid and had gone from her usual 10 pounds to around 19 (she looks like a tiny teddy bear and my boyfriend can’t stop himself from giving her treats!) so they recommended we put her on Denamarin and work on getting her weight down. She’s been on Denamarin for about six months now and her ALP remains high, despite a deep dental clean and more than 5 pounds weight loss, so her doctor is recommending an ultrasound so she’ll have a better sense of what might be happening so she can recommend next steps. The veterinary hospital is still operating under covid protocols, which I totally respect and appreciate – but it means we don’t get a lot of time with her veterinarian to discuss.
Hi Tara,
I understand your concern with these elevated liver enzymes in your senior girl. I am glad you are planning to move forward with the abdominal ultrasound. Please make sure you let your vet know you need some more time to discuss your dog’s situation and have your questions and concerns addressed. You may be able to request an appointment slot just for a consult. This way you get plenty of one on one even if it has to be over the phone. I hope the ultrasound results will help to guide the treatment process. Praying for a positive outcome for your sweet girl.
Hi,
I have a 12 year old American Bulldog who I adoptee at age 1. Prior to his adoption he was nearly bald with red skin that the adoption center treated and told us he had a yeast allergy and to do non grain/ limited grain diet. Over the years that is what wr have done. He’s done fairly well but with fairly consistent red allergic paws the past few years that vets said likely food allergy or seasonal allergies. As we stick to yeast free, they said it could be a protein allergy or seasonal allergies now too.
Last month we noticed white flakey patches on his spine, and some balding on his tail and randon red patches . He also began panting very heavily in the evenings after his meal.
We consulted with the vet and did an antibiotic for possible infection om his skin. Bumps changed to more red. Vet saw him last week and discussed could be food allergy related or concerns for Cushions Disease. We drew blood work. Today received the results of Alkaline Phosphatase of 1842! and Platelet count of 500,000.
We are having him do a Dexamethasone test with blood draw twice at 4 hrs and 8 hrs after to see the bodies effect on regulating Cortisol to see if Cushions Disease, while the test can’t necessarily determine up front which Cushions Disease it may be. We will be proceeding with these tests, but I wonder if the high Alk. Phosphasate could be causes by systemic yeast or other inflammatory causes.
A human I know had high levels and found out their levels were due to a systemic yeast, verses a yeast culture. My dog we did a skin test for infection or yeast prior to this blood work with no yeast/ infection showing. Are there tests to check for systemic yeast? or other concerns with our case?
Also, he gets stressed during blood draws so I’m wondering what would be a normal elevated Alkaline Phosphatase level due to cortisol increase in stress.
Hi Lovemydog,
I understand your concerns with this elevated liver enzyme found on your dog’s lab work. Since I have not examined your dog myself, I can’t make specific conclusions or recommendations, but I will try my best to give you good information to research or discuss with your vet. Here is a link to another article about Cushing’s disease: Cushing’s Disease in Dogs: Symptoms, Diagnosis, Medications
From what you are describing, Cushing’s would be my first suspicion as well. It sounds like your vet is working through all the standard testing to rule out this possibility before moving on to other diagnostics if needed. While stress can raise cortisol levels in the body, I have never seen it cause the ALP to increase outside the normal reference range. With an ALP of 1842 there is no way this is caused by stress alone. Yeast infections are common on the skin of dogs with allergy problems, but I am not familiar with issues of high systemic yeast levels. Gut health is very important, but I am concerned something else is causing your dog’s elevated enzyme levels. Hoping this testing will give you some clear answers and allow your vet to decide on a course of treatment. Best wishes to you and your senior boy.
My little girl is a 10 year old miniature schnauzer weight at 12.5kg. She has a very large fat lump which she was booked in for surgery in June to get removed along with another smaller lump which is growing rather rapidly (it is affecting her balance and soon it will affect her mobility). Unfortunately on the morning of her scheduled operation her blood work came back poor. Her ALP was 1139 and her ALT was 220. Lottie had an ultrasound which didn’t show up any irregularities. She was put on Samilyn, a liver supplement, for a month and then had another blood test to check ALP and test for Cushings; test came back negative but her count had raised to 2812. In September, she had a liver biopsy (and whilst under, a full dental clean – for the first time). Again, biopsy results were normal. On the vets advice we changed her diet to a hepatic diet and Samilyn supplement. Another blood test mid October and her ALP has raised to over 7000. The vet said that they see dogs with liver disease with a 2000-3000 count so they’ve not seen anything like this in a dog who, other than her ALP, is showing no signs of liver disease. They are now recommending a CT scan. It feels like significant costs but backward steps. We are very worried about our little girl.
Hi Tracey,
I understand your concern for your senior girl with these severe increases in liver enzymes. My best recommendation would be to schedule a consult with an internal medicine specialist. They have lots of experience with complicated cases like your pup and may have ideas about other testing that needs to be performed. Has your dog been tested for leptospirosis or tick-borne diseases? It sounds like your vet is staying on top of this and working hard to get some answers. I hope you can get a diagnosis so treatment can be started quickly. Praying for a positive outcome. Feel free to leave an update if you have a chance.
My dog has very similar blood test numbers (negative for cushings and >2000 alp). She seems completely normal in behavior and appetite but the vet wants to do a liver biopsy. Have you found out anything additional for your pup?
Have you found out anything additional? My 11 year old mini schnauzer has the same situation going on and I’m at a loss as to what to do for him next!
Hi good evening . I have a shih tzu 10 years old. A month ago her vet did a full test and my dog has her ALP 900. She has dry skin that make her have dandruff in top of her body. Not in leg no in the belly . Doctor said she is going to treat her with anipryl. 5mg . But I don’t see any improvement. Also doctor prescribed her fluconazole for her skin but not improve as well. I decide to find another internal vetereniarian. Any information that you can give me because I’m worried 😟
Hi Damarys,
I am sorry your senior girl has had some abnormalities show up on her blood work. It sounds like your vet is suspicious of Cushing’s disease. If this is the case, your dog may need more testing to get a definitive diagnosis and decide if the problem is caused by the pituitary gland or the adrenal glands. Anipryl is usually prescribed for Cushing’s that is pituitary dependent. Since I haven’t personally examined your pup, I can’t make specific conclusions or recommendations. It is always ok to get a second opinion if you have lingering questions or concerns. The goal is to find a vet with whom you are comfortable partnering to address your dog’s health issues and wellbeing. I hope you can find the answers you need to make the best choices for you and your sweet girl. Wishing you the best of luck.
Hi, our 11 year old lab/ Dane mix just had his yearly physical and senior blood panel .. all results were perfect except his ALP was 1138. He is acting his normal self , not eating or drinking anymore than his normal piggy self , playing, going for daily walks , skin / fur good . .. vet wants to test for cushings . I’m not sure if we should wait and see or go ahead with testing . I’m reluctant because he has no other blood work numbers out of whack .
Hi Deb,
I am glad you were able to catch this abnormality on routine lab work. It is not a bad idea to pursue further testing. With that being said, it is usually not recommended to treat for Cushing’s unless symptoms are present. So, if your dog is not symptomatic, treatment would not be needed even if the testing is positive. When investigating an elevated liver enzyme, I usually see most vets opt to run additional lab work (bile acids, etc.). Some even like to have an abdominal ultrasound preformed to rule out a tumor. I have also started patients on a liver supplement for a few months and then rechecked blood work to see if the liver values have decreased. I hope you can find the answers you need to make the best choice for you and your pup. Ultimately, I hope you and your vet can work together to maintain your sweet boy’s health and wellbeing. Best wishes!
Our 13 year old male Chihuahua/Terrier mix has a ALP of 219, MCHC of 32.5, ALT 207 and Creatine Kinase level of 219.
We just scheduled his teeth cleaning at the vet and they will be sedating him so, is there any concern doing the teeth cleaning with the blood levels mentioned above?
Hi Jack,
There is always some risk with anesthesia even if blood work is completely normal. Your vet is aware of these liver abnormalities and should be able to tailor the anesthesia protocol to your dog’s specific needs. Many times, dental disease alone can cause an increase in liver enzymes. If blood work is rechecked a few weeks after the dental procedure, you may find these levels have improved just from treating the dental issues. If you have any lingering questions or concerns, don’t hesitate to discuss them with your vet. I hope the procedure goes smoothly and your pup is feeling great again in no time.
Hi Dr. Buzby:
I love reading your blogs and just stumbled across them while looking at your toe grips! I am all about holistic medicine for the whole family including our big floof.
This comment is
1) to ask about Encore Mobility;
2) diet recommendations for our dog with HCC and arthritis;
2) my attempt to illustrate to hoomans why it’s important to advocate for your animals even when a vet chalks new symptoms up to old age.
Our dog Caesar is a 12yo male ChowChow. He was 8 when we rescued him. He was diagnosed with hepatic cellular carcinoma in July 2022 after an ultrasound (ordered to see his adrenal glands/rule out Cushing’s) revealed a 12cm mass on his liver. Adrenal glads were fine. CT w contrast confirmed heterogenous round shape/location, along with some multifocal hypoattenuating cysts within the renal cortices and chronic right-sided coxofemoral joint luxation with pseudoarthrosis formation.
A dexamethasone suppression test confirmed he did not have Cushings, so Caesar underwent an exploratory laparotomy on 8/23/22 where they removed the liver mass with good margins and has fully recovered from the surgery. BIG 13″ incision!
Rewind to when we first got Caesar in 6/2018. At our first check up the vet felt plenty of arthritis in his shoulder and hips and started him on dasuquin advanced and he is still on that. When an occasional limp would present, our vet would just do a 1-2 week course of rimadyl (wonder drug for Caesar) and limit his walks to “bathroom and back” so to rest the affected joint.
Fast forward to summer 2021 –he was snapping and very grouchy to almost everyone except me and my husband (even for a Chow). No limping or whimpering or even licking a foot. After hours of evaluation, his trainer and I concluded he was in chronic pain from his arthritis and the vet concurred. Vet started a course of adequan injections, but I didn’t see any difference after 7 months so we d/c. Vet performed a full body set of xrays in March 2022 and his arthritis had progressed. Vet started him on rimadyl as a maintenance dose and sure enough he was a new dog. (all of this vet work was driven by me driving them crazy).
In April 2022 his annual physical was performed. I reported symptoms of 90-100 breaths/minute 24/7, including at sleep. He was drinking LOADS of water and had a voracious appetite(always been very food motivated tho). The vet felt like his spleen was prominent upon physical examination and did a cardiac xray that was fine.
Full blood panel was performed and his ALK/ALPs were elevated. Vet stopped his rimadyl immediately and started Denamarin, with a plan to begin Galliprant after 10 days of Denamarin. Those 10 days were AWFUL. Trembling hind leg, mobility was worse than BEFORE he went on the rimadyl. He was only on rimadyl for 2 weeks before the bad liver results, and it was like the denamarin was making him worse – which is ridiculous of course (milk thistle can’t hurt anyone).
Finally the “detox” was over and we started the Galliprant (100mg, 1x/day) and he has regained decent mobility, but not as good as on rimadyl.. We repeated a blood test in June 2022 and those ALPs were still elevated. Vet wanted to wait and see – and I insisted on the ultrasound. You already read the rest.
I have worked in the human healthcare environment as a hospital and physician practice administrator for 25 years, so I’ve learned enough clinical info through osmosis to know when we press forward for answers on humans, and I didn’t want our dog to be treated much differently. But if I was a banker, he would still have a grapefuit sized mass in his diaphragm, and on a 60 lb dog, that’s like a beachball to my body.
Result: normal water intake, normalized appetite. Will have an ultrasound in 2 months to see if anything is growing back.
He still struggles with his hips – the CT showed the right one is BAD.
Do you think he would benefit from encore mobility in conjunction with Galliprant? He is also on Curcumin C3 and dasuquin advanced w MSM.
Diet: I blend rosemary, basil and turmeric with water packed sardines and use as a topper on Health Extension venison kibble, along with pureed pumpkin (bc I can’t have that anal gland smell in the house EVER AGAIN).
Any suggestions on ramping up the anti inflammatories through diet?
Longest comment ever – thanks Dr Buzby!
Hi Ashley,
Caesar is one lucky boy to have found you! I applaud you for taking such an active role in advocating for his health and wellbeing. I think his current diet and supplement regimen sound great. As for Encore Mobility, it could be an added bonus to all the amazing things you are already providing. I feel like the New Zealand deer antler velvet is such a game changer and isn’t found in any of the other supplements you currently use. You may also want to look into acupuncture or laser therapy to help with arthritis pain and decrease inflammation. Have you heard of PEMF therapy? I will attach links to other articles that may offer additional information. Best wishes to you both and keep up the good work!
1. PEMF Therapy for Dogs: 7 FAQs Answered by a PEMF Expert
2. Natural Pain Relief for Dogs: 13 Methods
3. Dog Arthritis Treatment: 8 Ways to Help a Senior Dog at Home
My 9 year old Boston Terrier was shedding a whole bunch more than I’d ever noticed. He left a halo of fur where he had been sleeping. I worried about Cushings. He had no other symptoms. He had a senior blood panel and everything was good but ASP was 818. Vet recommended x-ray/ultrasound investigation. However given his overall good health, In leaving towards Denamarin and retesting his liver enzymes. Should a month suffice?
Hi Jess,
There is really no way to know for sure how long it may take the liver to respond to the supplement or if it will respond. Since I haven’t personally examined your pup, it is hard to make specific recommendations. A month is a reasonable time period to recheck lab work. If you don’t see the improvements you are hoping for, I think the ultrasound investigation sounds like a very good next step. Best wishes!
Hi Dr Buzby, my 9 year old male Pomeranian Fazzie had an ALP of 934 and ALT of 250. He has had ultrasound which showed enlarged liver and a swollen right adrenal gland. He has been drinking a lot more water and is always hungry. He has had three seizures in the last 5 weeks unfortunately also . We are waiting on more blood work for Cushings and a cortisol check w last blood work which was three separate blood draws at 4 hours apart w fasting for Fazzie
Is there anything else this might
be? And there seemed to be no tumor on adrenals so can it be a pituitary tumor causing the problem I am wondering?
Btw… he had blood work three weeks back and levels were half of the latest results I shared w you
He’s currently taking Proteliv drops and Vit B in liquid form
Thank you David
Hi David,
I understand your concern for Fazzie and these worrisome abnormalities found on lab work and ultrasound. Cushing’s disease can be pituitary dependent or adrenal dependent. The extra bloodwork should help to distinguish the source if your pup is indeed diagnosed with Cushing’s. Luckily, Cushing’s is treatable, and symptoms usually resolve quickly once therapy is initiated. If the testing doesn’t provide the answers needed, you can always schedule a consult with a veterinary internal medicine specialist. I will attach links to other articles with additional information on Cushing’s. I hope you find the answers you need to give Fazzie the best life possible. Praying your vet is able to make a diagnosis and get things stabilized quickly. Wishing you both the best!
1. Cushing’s Disease in Dogs: Symptoms, Diagnosis, Medications
2. Trilostane for Dogs With Cushing’s Disease
7 year old Maltese/Yorkie has chronically elevated ALT (800) with cell damage, vet said AST very high too. Ultrasound scheduled next week. Our pup has had a few bouts of pancreatitis this past year and sometimes will go 2 days without eating, behavior is definitely changing lately with more naps and less interest of favorite things. Vet mentioned a look at his gallbladder during ultrasound. How many days of not eating should you worry?
Hi Tracey,
I understand your concern about these liver changes and decreased appetite in your little pup. I am glad you have an ultrasound scheduled with your vet and would be interested to know what they find. Since I haven’t personally examined your dog, it is hard to make specific conclusions about when to worry with the lack of eating. There are so many factors to consider such as blood sugar levels, hydration, etc. I hope the ultrasound findings will offer you some answers and guide you in the treatment process. Praying for a positive outcome.
My 11 year old yellow lab, Goldie, had blood work that indicates a high ALT level (296) and a high ALKP level (560). She is on Samilyn and milk thistle. Her ALT level has only increased slightly over the past year (from 219 a year ago to 296 now). Bur her ALKP level has increased from 346 a year ago to 560 now. What else should we do to help our dog?
Hi Cindy,
I understand your concern for your senior Lab and these increased liver enzymes on her bloodwork. If your pup has been on supplements for a year and the values continue to rise, it may be time for some additional testing. There are other liver specific blood tests that can be sent to the lab and an abdominal ultrasound may be warranted to see what the liver looks like. You can also request a consult with an internal medicine specialist. This is the perfect time to talk to your vet and discuss your concerns. Let them know you are ready for the next steps in the diagnostic testing process.
Hi Dr. Buzby. I have a 9.5yo (approx) Corgi/German Shep mix (my service dog) who on a recent exam showed an ALP of 190. Her urinalysis showed that her urine was diluted. It has been incredibly hot and humid and she has been drinking considerable amounts of water; however that fluctuates depending on the heat and this in and of itself it not unusual for her. Her appetite has been high (also, in and of itself not unusual for her), though if you tell her ‘drop it’ or ‘leave it’ she will. That said, she has virtually zero prey drive and I would think if her appetite were insatiable – especially with a cat in the house as well – that would be an issue. Her vet suggested a steroid-challenge blood test, as he suspects Cushings. I asked if we could pull back a bit on her water overnight and retest her urine to see if her body is still diluting; he agreed so long as we don’t totally withhold. That will be done this weekend.
Given that she has always had a hearty appetite, always compensated for heat by elevated water consumption and that her urine came back dilute, is it possible that this is an anomolous finding? I will repeat her bloodwork in a month or two when the weather cools.
Thank you for your input.
I neglected to add one detail – she has ALWAYS had a penchant for eating poop from the cat’s litter box (nasty, I know). We use Breeze pellets for the cat. Do you believe this could be a factor? We started using the Breeze pellets about 3 or so years ago. Thank you again.
Hi Lee,
I would not be worried about the Breeze pellets. And although I don’t think it would contribute to the symptoms you described in your original post; it might be a good idea to make sure your pup is negative for intestinal parasites.
Hi Lee,
I understand your concern for your senior guy and these recent abnormalities found on his bloodwork. As I was reading your comment, I was already suspicious of Cushing’s even before I saw where you mentioned it. I am going to be honest with you…. I think you should go ahead with the recommended testing your vet has discussed and not worry with trying to withhold water. Cushing’s disease causes an elevated level of steroids in the body. One of the side effects of steroids is increased thirst. I think the odds of this being anomalous finding are very low. Here is a link to an article with more information about Cushing’s disease: Cushing’s Disease in Dogs: Symptoms, Diagnosis, Medications
I hope you can get some answers quickly and start the appropriate treatment plan to give your pup the best quality of life. Wishing you both the best of luck.
Hello. My doogy son teddy is somewhere between 11 and 13. He has glaucoma. He has recently had an increase in appetite, decrease in energy, and sometimes trembles. He had bloodwork done and his cardio lab work was all normal. All 4 thyroid markers came back significantly low and he is now on thyroid medication. The vet said everything else was normal, but upon looking at the results, I noticed that his ALP is 249. Could this be because of his low thyroid numbers. Is that why he trembles? Does he need to be on Denamarin? He seems to be in some pain as well. Any guidance is appreciated.
Hi Jeanette,
I understand your concern for Teddy and the health issues he is facing. Since I haven’t examined your pup myself, it is hard to make specific conclusions and recommendations. If liver enzymes are found to be slightly elevated on one set of lab work, that doesn’t always mean there are ongoing liver issues. Thyroid levels can cause changes in almost every system of the body. There can be a one-time spike in liver values that would be completely resolved and back to normal if bloodwork was repeated in a few weeks. Also, many medications can cause changes in values seen on bloodwork. My best recommendation is to discuss your concerns with your vet. They can let you know why this number did not cause worry in your dog’s specific case or if a supplement should be considered. Please be sure to tell them you are suspicious Teddy may be in some pain. Trembling can be a sign of discomfort. I hope you can get the answers you need to feel comfortable with Teddy’s treatment plan. Praying everything can be stabilized and let your sweet boy keep living his best life.
I have a 11 year old GSD mix whose senior wellness bloodwork came back with very high levels of ALP(1110), slightly elevated GGT(17) and very high cholesterol(823). She has also had the following symptoms for the past 6 months:
Thinning hair(Lost a lot of hair – used to have a full bushy tail and now spindly, can see skin. Similar hair loss in other areas)
Very thirsty and drinks about a gallon + of water every day
Has an increasing pot belly
is always hungry and eats anything she can find on the ground
She’s already on proin for her spay incontinence for past 2 years or so. We are suspecting Cushings and she’s going in for her test in a couple of weeks. Any thoughts ?
Hi Guru,
I was already thinking Cushing’s before I made it to the end of your comment. It sounds like your vet is on the right track and this is the first thing that needs to be ruled out. I hope the testing will give you a definitive answer so treatment can be started right away. If your senior guy does have Cushing’s, then you should notice positive changes relatively quickly once the medications are administered. Praying for a positive outcome. Feel free to leave an update if you have a chance.
My dog Phoenix (13.5 yo) has very elevated ALP (1723 UL) and ALT (254). My vet prescribed Denamarin for 30 days. However, after about 10 days, he would throw up, and then had severe diarrhea, so the vet said to discontinue use. What do I do now? He is currently on Hill Science Diet – IB -Low Fat Prescription kibble. as he has a history of pancreatitis. He also takes a probiotic daily, dasaquin, and Welactin Fish Oil, and takes Heartgard monthly. Is there something I’m missing? Thanks for any info.
Hi Joan,
I am sorry Phoenix is dealing with elevated liver enzymes and doesn’t seem to be able to tolerate the Denamarin. The only way to find the best treatment is to first get a diagnosis. If you want to pursue diagnostic testing, the next step would probably be additional labwork and abdominal ultrasound. It would be a good idea to talk to your vet about your concerns and see what they recommend. You can also look into scheduling a consult with a veterinary internal medicine specialist. I think you are doing the right things and Phoenix is lucky to have you advocating for his health and wellbeing. Best wishes to you both.
Hi! I’m curious, does the Denamarin help with the elevated ALP, ALT, or both? Thank you in advance.
Hi Kimberly,
The Denamarin helps with both liver enzymes (ALP & ALT) since it acts as a liver protectant and contributes to liver health and repair.
My almost 8 yr old female spayed Shih Tzu hasn’t been herself for about 6 months and in Feb of this year we had blood tests done and her bloodwork was good except for an elevated ALKP of 451 on 2/22.. Yesterday, Aug. 16, we had more bloodwork done and her ALKP had jumped to 1783 U/L and is quite significant. She is not feeling that good and she, vomited yellow bile two nights in a row last week. No vomiting since. She is a great eater and is still eating and drinking water but her tail is always down and she seems more nervous She whines a lot but that is typical of what she does.. My vet has an ultrasound scheduled for next Wed., 8/24. She weighs 8.2 lbs and is small for her breed. She is also constantly scratching her underside (by her back legs and front legs) for some time now and they cannot find out why. She has no redness or anything on her skin but it’s almost like OCD. I have been spraying those areas with DogMX medicated Hot Spot & Anti-Itch Spray and maybe it helps a little but I just read that it could affect her liver. Is that true? I am worried sick about her and would like your comments on what is going on. Thank you very much.
Hi Elaine,
I am sorry your Shih Tzu is having issues with her liver function. I am glad your vet has scheduled an ultrasound and would be very curious to find out the results. I researched the DogMX spray you mentioned and found that one of the active ingredients is a steroid. Steroids are known to affect the liver if used long term, but this is usually when they are taken orally. Topical steroids like this spray can cause internal changes, but not to the same degree as oral medications. I would be highly surprised if the spray was the culprit behind this issue or if it even contributed at all. Don’t worry yourself too much about it, but it might be a good idea to discontinue the spray for now just until you get a diagnosis. I hope the ultrasound can give you some answers. Praying for good news and that treatment can be started quickly. Feel free to leave an update if you have a chance.
Dexter, my 12 yo soft coated wheaten terrier recently had some elevated, and rising ALKP levels over the past year. After a level of 571 vet recommended milk thistle, and he had a recheck and remained elevated (slightly more so into the 600 level for ALKP). The ALT levels have remained steady at 188. I have decided to proceed with an ultrasound next week. 1) should I be worried regarding the procedure since there is sedation involved? 2) is this a moderate or extreme elevation? 3) are there any other tests I should be asking to have done? Dexter is eating and drinking normally, and his allergies as a matter of fact have been the most under control they have been in YEARS, but the rising liver levels worry me! I hope all goes well with my guy – are there any other things I should be doing or questions I should ask the doc?
Thanks!
Hi Corey,
I understand your concern with these elevated liver enzymes in your senior pup. Dexter is lucky to have you advocating for his health and wellbeing. I would not be worried about the sedation for the ultrasound. This is generally very light sedation and can usually be reversed if needed. It is hard to say if these elevations are considered moderate or severe. I have definitely seen much higher numbers than what Dexter’s labs are currently showing. There are many more tests that can be done to evaluate the liver and rule out potential causes, but I too would recommend starting with the ultrasound. Wait to see what the ultrasound results reveal, and then further testing can be better tailored to your dog’s specific needs. Also, you always have the option to schedule a consult with a veterinary internal medicine specialist. I hope you receive positive results from the ultrasound and can figure out the best way to help Dexter with his liver issues. Wishing you both the best. Feel free to leave an update if you have a chance!
My female 14yo Mini Schnauzer’s bloodwork showed ALT 824 (251 in early June), ALP 1680 (62 in early June), GGT 23 (normal in June). She’s been drinking a lot, peeing more, loves to eat, and going on sniffaris. She’s her usual self.
Vet sent referral for ultrasound.
Please, how would you explain these elevations, and how would you proceed?
Thank you!
Hi Andrea,
You are right to be concerned about your Schnauzer and these recent changes to her bloodwork. Since I haven’t examined her myself, it is difficult to make specific conclusions and recommendations. I think your vet is on the right track and an abdominal ultrasound would be the best next step in making a diagnosis. There are many diseases and issues that can cause an elevation in liver enzymes. I think the ultrasound results will help to narrow things down and then other lab work or diagnostics can be recommended based on the new information obtained. Best wishes and feel free to leave an update if you have a chance.
A couple of things…..
I have a 13yr old female poodle Shitsu mix. ALP 677 with a normal range of 5-160. My vet prescribed her Danamarin for 30 days and a retest. Good call?
Also, is there prevention either by diet or exercise or do some dogs just get it and others don’t?
Thx
Hi Mike,
Yes, Denamarin is great! Sometimes we will try a supplement to see if it can correct the issue before moving on to more advanced and costly testing. Please know that the testing can be pursued at any point. So, if you are concerned about the effectiveness of the Denamarin or just want to have more answers, your vet can move on to the next step if needed. If the supplement does not help to reduce the ALP, they will probably recommend additional blood tests and possibly an abdominal ultrasound. While there are some toxins and diseases that can affect the liver and cause an increase to the ALP, some dogs just get it, and we don’t know why. I assume genetics are to blame but we don’t know for sure. I hope the Denamarin will be the solution to your senior girl’s problem. Best wishes and good luck!
Hi I have an 8 yr old cockapoo. Just been to have a routine op to remove two small lumps. This was cancelled as routine bloods showed ALP 521 and ALT at 180. Urine showed blood. Liver scan on Thursday and antibiotics for ? UTI. Meg ate a full Easter egg about 6 weeks ago and had medically induced vomiting! She has no other symptoms at all. How worried should I be. I’m a sensible dog mum but she is my world!
Hi Jen,
I understand your concern about Meg and these new abnormalities that have developed on her lab work. I would not be overly worried about the UTI at this point. As long as the bacteria that is causing the problem is sensitive to the antibiotic that was prescribed, it should clear up within a few weeks. As for the elevated liver values, it could be cause for concern, but you won’t know for sure until the testing is completed. It could be something simple that can be resolved with a special diet and a supplement. I am praying that the ultrasound on Thursday reveals positive results and a treatment plan can be started. Feel free to leave an update if you have a chance. Wishing you and Meg the best.
Rocky, my 5yr old pure bred Beagle has a high ALP on his blood work. He has severe allergies so he is on apoquel a d 2 benadryl daily and on Ultamino science diet for almost 2 yrs now. He was throwing up one nigtht and anorexic for almost 2 days so I decided to let him to the vet, his Vet assessed him and his blood got tested. All his other liver enzymes are normal, only the ALP is above 600. Doc prescribed Denamarin 2 tablets daily. How will Denamarin help? Will that reverse his high ALP? How long should he be taking denamarin? Could the apoquel be causing his high ALP count? How about his ultamino?
My dog is also overweight, is that something that can elevate his ALP?
His Vet is great and has known my Rocky for a long time.
Thank you!
Hi MG Rob,
I understand your concern for Rocky and this recently elevated ALP. I am glad you were able to have him evaluated by your vet and get some answers. I really like Denamarin and have seen great results in my own patients. Denamarin is a liver protectant and helps with liver health and repair. At some point, I am sure your vet will recheck Rocky’s lab work. If the ALP has returned to normal, your vet may allow you to discontinue the supplement. Apoquel is supposed to be safer for the liver than other anti-inflammatories, so I would not think this was the cause of the elevated ALP. Diet and weight also should not cause an increase to liver enzymes. You may never know for sure what caused this liver insult. If the supplement does not show the improvement your vet is hoping to see, they may recommend additional lab work or even an abdominal ultrasound to look at the liver. I hope you see positive results at Rocky’s next recheck. Best wishes to you both.
My 9 year old Maltese had senior panels done and almost all levels were normal with the exception of the ALP and cholesterol. The ALP was well over 6,000. They are going to do a 12 hour fasting test in 3 weeks. He has year round allergies, is overweight at 18 pounds, and is on 5.4 apoquel and cytopoint shots every 3 weeks. He always been a huge water drinker. He tends to pant heavily quite frequently. Any thoughts on the 6,000 ALP? I can’t find any other reference of such an extremely high level. I would like to know what food or supplement could help his liver function. I feed him only grain-free foods, both dry and wet food. Thank you!
Hi Cathy,
I know how concerned you must be about this elevated liver enzyme on your senior boy’s blood work. Try not to get too worried at this point as it could turn out to be nothing at all. I have definitely seen levels this high (and higher) resolve with little to no intervention. I am glad your vet has a plan in place for follow up testing. I am curious to know what the results will be. There are several good supplements available that help with liver function such as Denamarin. Your vet probably has one they like and recommend and would be willing to prescribe. I would love an update once the testing is completed if you get a chance to write back. Praying your sweet boy continues to feel good and gets positive results.
I have a 14 year old dog with a ALP of 800 in May and in October jumped to 1000. All over blood tests came back normal. Some weakness in legs. Has been thirsty and can’t hold urinating more than two hours. His spleen was removed 5 years ago, spotty and enlarged. The Vet says I could do more testing why the ALP levels are high, such as an ultrasound and biopsies. I am not convinced that will find anything. Suggestions for over the county remedies and thoughts of diagnosis? Thank you!
Hi Finn,
I understand your concern for your senior dog with these increasing liver enzymes. Unfortunately, without further testing there is no way to know what the cause could be, and it is hard to make specific conclusions. I do like to start my patients on a liver supplement that helps protect the liver from further damage and can help restore function. Denamarin is my favorite, but you can also just use Milk Thistle. I encourage you to discuss this with your vet and they can help you figure out the appropriate dose. Here is an article with more information that may offer additional guidance and advice: High Liver Enzymes in Dogs: A Vet Explains What It Means
Hoping your sweet boy has many happy days ahead and I wish you both nothing but the best!
Hi,
My 14-month old 43 pound mini bernedoodle has had significantly elevated ALP levels for the past 6 months. His most recent test it was around 2700 and had slightly elevated white blood cells. He has been fully grown for a few months now.
He is clinically healthy and not showing any signs of not feeling good. We put him on a liver supplement for 30 days and the ALP level was higher than his previous test. We have also done an ultrasound which did not show anything.
We are going to do a blood test that they should should help isolate why the level is elevated….liver, bone or muscle.
Has anyone experienced such high levels or these types of numbers in such a young dog?
Hi Nathan,
I am sorry you are dealing with such difficult issues in your young pup. It sounds like you have a good partnership with your vet and a plan for further testing. Unfortunately, this may be a long road ahead before you get a diagnosis. Don’t forget you always have the option to consult with a veterinary internal medicine specialist. They may be able to offer additional information or pursue more advanced imaging/testing that might not be available in general practice. I hope you can find the answers you are looking for. Praying your sweet boy can turn this around and live a long happy life. ♥
My 12 year old 7kg dachshund Chihuahua mix Sophie just measured 2577 for her APL (her vet told me 131 was normal). Her ALT was 150 so a bit above normal. She needs dental work done including cleaning and this was caught on the pre anesthesia blood work. She has degenerative heart valve syndrome, a grade 3 heart murmur and has been on vetmedin 1.25mg for the last 6 months for that. She has a history of interverbial disc disease and had surgery 2015 to correct paralysis from that. The high APL came out of nowhere. 6 months ago when I found out about her heart condition I changed her food to a mix of hills prescription diet kidney care wet food and hills prescription diet digestive care dry food. She’s going to have an ultrasound in a month to see if there’s a tumour or something. Everything else with her is good, I did add in the greenies tooth brush chews to help with her teeth a month or so ago and she is not good with changes to her diet so had some diarrhoea issues but had the fortaflovia (spelling may be wrong here but the powder on her food). I’m panicking a lot since we don’t know the worst/best case scenario but this 2577 with 131 as a normal range seems really bad 🙁
Hi Courtney,
I understand your concern for your senior girl with these high liver values. Fortunately, it sounds like your vet is staying on top of things and has a plan to follow up with ultrasound. Dental disease by itself can cause increased liver values which may return to normal after a thorough dental cleaning has been performed. Yes, your girl’s ALP is quite high, but I have seen them even higher and still return to normal after making a diagnosis and starting the appropriate treatment. So, I do think you need to keep running tests and looking for answers but don’t forget to stay positive and hold onto hope for a good outcome. Wishing you and your pup the best.
My 6 year old male schipperke just got bloodwork done and they found slightly elevated ALP levels, but nothing else seems to be wrong. He is on a liver supplement now and we will retest in a month. In the meantime we are just really hoping it turns out to be nothing. Very worried about our not-so-senior boy. He’s always been so healthy. Not sure where we went wrong.
Hi Kelly,
It doesn’t sound like you have done anything wrong. In fact, I applaud you for having routine wellness lab work done! This allowed your vet to catch this early and intervene on your little guy’s behalf. It is quite possible that everything could be normal on his recheck labs and this was all just a “fluke”. I hope the liver supplement does its job and all the worry will be over soon. Best wishes to you all.
I have a Mini Schnauzer 16 lbs who will be 12 next month. She had bladder surgery at 1 and has been on Hills CD since. Last September (after eating approved treats from a new vet at our same office) she started a new stone and was quite ill. At that time xrays were done as well as extensive blood work and medications. She recovered. Although her liver ALP was elevated. In November she had another blood test and it was up to 431 and she started taking Hipaticlear. Yesterday she had blood work in prep for a dental on 2/14 and again her ALP was elevated to 617. The vet (the young one who suggested the treats is no longer there) said she is good for the dental and we will do another blood test 30 days after. She suspects her teeth may be causing the increase although she did have a cleaning last year as well. My question is the number (I did find ant info on the actual numbers) and whether she is in any danger.
Hi Kathie,
I am glad to hear your girl recovered from her most recent bladder stone episode. I am amazed that she hasn’t had any other issues with them in the past 11 years! Your vet is correct that dental disease can cause ALP to be elevated. Many times, the ALP will return to normal or decrease after the dental procedure is completed if the dental disease is the underlying cause. Since I haven’t examined your dog myself, I can’t make specific conclusions or recommendations. There are additional ways to check liver function such as more advanced blood testing and ultrasound. You won’t find specific information about ALP numbers and their correlation to what is happening in your dog’s body because a high ALP doesn’t point out a specific issue or disease process, but rather gives you a broader picture that something is off. And just because the ALP is high doesn’t tell you if the underlying cause is life threatening or rather benign. If you have any concerns about your girl’s risks with anesthesia, make sure to discuss them with your vet. I hope you can find the answers you are looking for to help make a decision you are comfortable with. I wish you and your sweet girl the best.
My senior dog (16 year old cockapoo) has an increased ALP from October (2300) to January (7000). Her ALT was slightly elevated.
My dog is having trouble with her back legs, having accidents in the house (both) and just starting to look like she is failing.
Dr. would like to do ultrasound, however, whatever is found, we would not seek treatment, so we are taking the wait approach.
Dr. gave us a number of things it could be but just wanted to know if you have any insight as to whether this increased level mean she is dying.
Thank you.
Hi Diane,
I am sorry your senior girl is starting to struggle with her back legs and having accidents in the house. I understand how frustrating it can be to see your dog decline and not know how to help. As for your question about the high ALP and the possibility of it being fatal, I think this is exactly why your veterinarian was recommending additional testing. Without getting a definitive diagnosis there is really no way to know what the prognosis is or what the future may hold. There are many reasons for ALP to become elevated, some are pretty benign issues while others could be life threatening. If you need more information or want to better understand what is happening with your girl, I highly recommend you talk with your vet and consider going forward with the ultrasound. Best wishes to you and yours.
My dog 11 year female had a slightly high ALP – 248 in Nov 24 and started Livox Liver Supplement
2nd Jan she suddenly started vomiting and CBC was normal but ALP – 237, ALT – 62. Vomiting was stabilized by 4th Jan
4th Jan – ALP – 676, was even higher. Started Livox Liver Supplément and N-Acetyle L-Cysteine Tablet and low fat diet
7th Jan – ALP – 817 gone up even higher, Continue – Livox Liver Supplément, N-Acetyle L-Cysteine Tablet. Started – Ursodeoxycholic Acid Tablets 300 mg and Augmentin 375 mg
7th Jan – 1st Ultrasound – showed mixed echogenic irregular growth on lift cranial liver lobe. Dia 2 cm and hyperechoic ring target sign. However no facilities to do any further investigation.
12th Jan ALP – 499, ALT 83 – Stopped Augmentin but continued the other three medicines
25th Jan ALP – 1967 – Started Augmentin again
27th Jan ALP – 1793, ALT – 275, CBC – normal
29th Jan ALP – 1278
01 Feb ALP – 1054
05 Feb ALP – 887 – Stopped Augmentin as no infection and continue other medicines
7th Feb – 2nd Ultrasound. Exactly same as the Ultrasound on 7th Jan. No increase or decrease
23 Feb ALP – 1215 – gone up again, ALT – 232, Urine analysis normal
The doctor is puzzled as CBC is always clear. However, it seems she only responds to Augmentin Antibiotic but there is no infection shown on the CBC
She eats normally and normal appetite
She has lost weight in the last 4 weeks, probably due to strict bland low fat diet.
Can you please advice why the ALP could be responding to antibiotics when there is no infection or any other things we should look at
Hi Kushan,
I am sorry your senior girl is having these ongoing issues with her ALP. Unfortunately, without playing a personal role in her medical care it is hard to offer specific conclusions or recommendations on how to proceed. Since you still have more questions than answers despite all the testing and treatment you have tried, it may be time to ask for a referral to an internal medicine specialist. Hoping you can find the answers you need to ensure your girl has many happy days ahead. Feel free to keep us updated as things progress. Best of luck to you both!