What causes anemia in dogs? This question might be at the forefront of your mind if you just found out your dog is anemic. To equip you with knowledge so you can better help your pup, integrative veterinarian Dr. Julie Buzby takes an in-depth look at the top 10 causes of anemia in dogs.

Waiting on the results of your beloved pup’s bloodwork can be stressful. Even if the testing was part of a routine health screen, you may still worry about a new health issue cropping up. This feeling can be compounded if your pup has not been feeling well or if your veterinarian had cause for concern based on the physical exam findings.
I get it. But for me at least, feeling informed can help tamp down those waiting-game jitters. So why not snuggle up with your canine companion, try to set your worries aside, and let’s see if we can pass the time by diving into the top 10 causes of anemia in dogs—which happens to be one of the most common bloodwork abnormalities.
- What is anemia in dogs?
- What are the signs of a low red blood cell count in dogs?
- What are the top 10 causes of anemia in dogs?
- #1: Autoimmune conditions in dogs
- #2: Bleeding splenic masses in dogs
- #3: Cancer can cause anemia in dogs
- #4: Blood loss caused by parasites or due to diseases transmitted by parasites
- #5: Toxin exposure cause anemia in dogs
- #6: Blood loss due to trauma or surgery
- #7: Gastrointestinal (GI) bleeding in dogs
- #8: Bone marrow disease in dogs
- #9: Kidney disease
- #10: Chronic disease can cause a mild non-regenerative anemia in dogs
- Miscellaneous causes of anemia in dogs
- The benefit of understanding the causes of anemia in dogs
- What was the cause of your dog's anemia?
What is anemia in dogs?
The first order of business is to ensure you know what your veterinarian means if he or she reports that your dog is anemic. In short, the term “anemia” refers to a low red blood cell count. So if your dog is anemic, he or she has fewer red blood cells than he or she should.
Typically, you will find out your dog has a low red blood cell count after your vet performs a complete blood count (CBC). This test is an important component of screening blood tests for dogs. It reports the size and number of red blood cells, the number of platelets, and the numbers of several different types of white blood cells.
All of these blood components are vitally important for your dog’s health. But let’s focus in on the red blood cells for now. Their main job is to carry oxygen around the body. So without sufficient numbers of them, oxygen delivery can drop, sometimes to dangerous levels.
Like many blood work abnormalities, anemia can be mild, moderate, or severe depending on how low the red blood cell count is. Generally, your dog’s symptoms tend to mirror the severity of the drop, especially in cases of severe and sudden anemia.
What are the signs of a low red blood cell count in dogs?
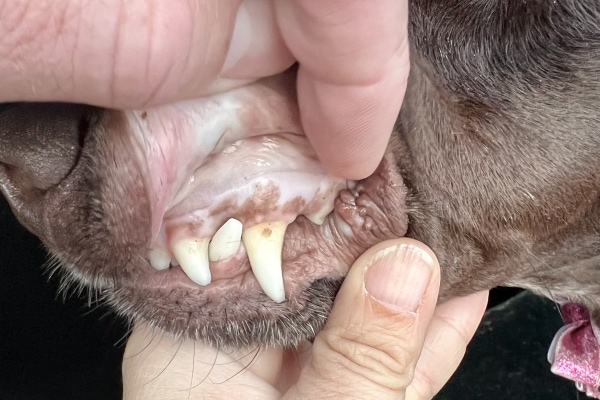
You may not even notice any signs of mild anemia. But as the red blood count drops further, dogs can become sluggish and tired. Their appetite may decrease, and they may become winded with even modest activity. You may also note that your dog has white or pale gums, eyes, or ears. Or, if you are checking your dog’s vital signs, you may notice a fast pulse or rapid breathing.
Should you notice any of those signs, make an appointment with your veterinarian ASAP (or take your dog in for an emergency vet visit if the signs are severe).
Mild anemia still indicates a need for more diagnostic digging but may be no big deal. Severely decreased red blood cells, on the other hand, requires immediate veterinary care. And unfortunately, even with aggressive treatment, severe anemia can sometimes be fatal.
What are the top 10 causes of anemia in dogs?
Once your vet diagnoses your dog with anemia, he or she will discuss how to figure out why your dog’s red blood cells numbers are so low. You see, anemia is actually a symptom of another medical problem, not a specific diagnosis. This means that the prognosis for an anemic dog depends largely on how easy or difficult the underlying cause of the anemia is to treat.
Let’s dive into the top 10 causes of anemia in dogs.
(If you want to become even more of an anemia expert, check out my article, Anemia in Dogs. There I cover the symptoms of anemia, the diagnostics your veterinarian might perform, and the broad types of anemia.)
#1: Autoimmune conditions in dogs
Two different immune-mediated diseases in dogs can cause anemia. Dogs with immune-mediated hemolytic anemia develop anemia as a direct result of the body targeting and destroying the red blood cells. On the other hand, dogs with immune-mediated thrombocytopenia can become anemic indirectly from spontaneous bleeding due to low platelets.
Both of these conditions tend to cause sudden anemia, and in some cases, severe anemia.
Immune-mediated hemolytic anemia
Immune-mediated hemolytic anemia, or IMHA in dogs, is both one of the most common immune-mediated diseases and one of the most common causes of anemia in dogs. As the name implies, in IMHA the dog’s immune system inappropriately attacks and destroys its own red blood cells.
Sometimes IMHA is secondary to something that has triggered the immune system to become overreactive. Common causes of hemolytic anemia in dogs can include:
- Certain types of antibiotic medications
- Tick-borne infectious diseases
- Certain types of cancers (which we will get to soon)
If a veterinarian performs the necessary diagnostics to rule out those potential triggers, then the IMHA is categorized as primary IMHA. This means that it happened without a definitive reason.
Dogs with IMHA typically have the normal signs of severe anemia like pale gums, a decreased appetite, and lethargy. Additionally, they may have a yellow tint to the gums and the whites of the eyes, and dark brown urine. These signs are caused by the build-up of bilirubin, a by-product of the red blood cell destruction going on in the body.
Veterinarians treat IMHA with blood transfusions and medications to suppress the immune system, such as prednisone for dogs. Many dogs with IMHA require hospitalization and aggressive supportive care. Then once dogs with IMHA stabilize, they often must continue taking medications for at least three to six months.
Unfortunately, roughly a third of dogs with IMHA who have gone into remission will eventually relapse. Thus, the prognosis for dogs with anemia caused by IMHA is somewhat guarded. However, remember that two-thirds of dogs with IMHA do well. So it is reasonable to remain hopeful that if your dog develops IMHA, he or she will fall into that group.
Immune-mediated thrombocytopenia
Immune-mediated thrombocytopenia, or ITP in dogs, is a condition where the immune system attacks and destroys the platelets. Platelets are tiny cell fragments in the blood that perform the very important task of clotting the blood. Dogs with ITP will have severely low platelets in dogs (i.e. thrombocytopenia) and consequently are at risk for life-threatening bleeding and anemia.
Dogs with ITP can bleed almost anywhere in their body. But most commonly their parents bring them to the vet clinic after noticing:
- Dark tarry stool
- Bleeding or bruising under the skin
- Bloody urine
- Dog nose bleeds
Many, but not all, dogs with ITP will also develop a low red blood cell count from their bleeding. If the anemia and low platelets are severe, they may need a blood transfusion to help stabilize them. This buys time for the medications that tamp down the inappropriate immune response to start working so the platelet numbers can return to normal.
Just like with IMHA, dogs with ITP need to remain on medications for months, and relapses are possible. But happily, the prognosis is somewhat better for dogs with ITP as compared to those diagnosed with IMHA.
#2: Bleeding splenic masses in dogs
Moving on from immune-mediated diseases, let’s head to another component of the immune system—the spleen. Normally, the spleen is a fist-sized organ that lives tucked behind the stomach and the liver. It works with the rest of the immune system to fight infections. And it filters out worn out or damaged red blood cells. These jobs mean that the spleen is full of many blood vessels.
As dogs get older, they can develop masses on their spleen, which can be either benign or cancerous. As the masses grow larger, they can sometimes rupture suddenly, leading to dangerous bleeding within the abdomen. The medical term for this situation is hemoabdomen, which just means blood within the abdomen.
Occasionally, masses from other abdominal organs like the liver or adrenal glands can cause a hemoabdomen too. But ruptured splenic masses in dogs are by far the most common cause.
Bleeding splenic masses and hemoabdomens are most common in large breed dogs like Labrador Retrievers or Golden Retrievers. But any breed can be affected. Some common signs of a hemoabdomen include:
- Pale gums
- An elevated heart rate
- Vomiting
- Labored breathing
- Collapse
Bleeding splenic masses are a medical emergency and can cause sudden severe blood loss anemia in dogs. If you suspect your dog may be suffering from a hemoabdomen, immediately head to your vet or the emergency vet.
Diagnosis and treatment for anemia and an enlarged spleen in dogs
The veterinarian will start by checking your dog’s vitals and performing a brief physical exam. If the vet remains concerned about a ruptured splenic mass, he or she will likely check a red blood cell count. Plus, he or she may perform either an abdominal X-ray or an abdominal ultrasound. And if there is free fluid in the abdomen, the vet may use a small needle to sample the fluid to determine if it is blood.

The vet may also perform screening chest X-rays. This is important because the most common type of cancerous splenic mass, hemangiosarcoma in dogs, likes to spread to the lungs. If X-rays show the cancer has already spread, dog parents may decide it is time to euthanize their dog with hemangiosarcoma rather than putting him or her through further treatments.
If the decision is made to move forward with treatment, the vet will discuss the plan. Many dogs with ruptured splenic masses are in a state of shock from blood loss. Therefore they will initially need to be stabilized with fluids or a blood transfusion. Then they can undergo emergency surgery to remove the splenic mass. Luckily, a dog can live without a spleen with no long-term negative consequences.
Prognosis for bleeding splenic tumors
Once the vet removes the spleen, he or she can send it to a diagnostic lab for a biopsy. The information from the biopsy, namely the tumor type and whether it was benign or cancerous, can significantly affect the prognosis.
If the mass is benign, then the great news is that surgery is curative. But if the mass is cancerous, the picture is not so rosy. Hemangiosarcoma survival times can range from two to six months, depending on whether the dog receives additional treatments like chemotherapy.
#3: Cancer can cause anemia in dogs
Hemangiosarcoma, as discussed above, is the cancer most frequently implicated in dogs with hemoabdomens. If you surveyed veterinarians, this is probably the type of cancer that they would most typically associate with anemia as well.
What kind of cancer causes anemia in dogs?
However, another set of cancers can also cause anemia in dogs. They include:
- Lymphoma in dogs
- Leukemia
- Histiocytic Sarcoma
- Multiple Myeloma
These cancers are all systemic cancers, meaning they are present throughout the body rather than being discreet masses. Also, they don’t cause anemia from blood loss like hemangiosarcoma. Rather, they cause anemia from increased red blood cell destruction or decreased red blood cell production.
Increased red blood cell destruction
Each of these cancers has the potential to trigger IMHA. As you remember from cause #1 of anemia in dogs, IMHA occurs when the body attacks and destroys the red blood cells. The end result is anemia.
Alternatively, in a specific type of histiocytic sarcoma, the cancerous cells themselves are responsible for gobbling up and destroying red blood cells.
Decreased red blood cell production
These types of cancers can also sometimes spread to the bone marrow. If that occurs, the cancerous cells can crowd out the normal bone marrow cells that are responsible for making new red blood cells.
As a result, the dog develops non-regenerative anemia. This type of anemia occurs when the body isn’t making new red blood cells in sufficient quantities.
Recognizing and addressing anemia due to cancer in dogs
Signs of each of these cancers are often relatively non-specific. They may include being a lethargic dog, lack of appetite, weight loss, or swollen dog lymph nodes. I don’t want this to scare you, though. There are also plenty of less dire diagnoses that can present with the same vague signs of not feeling well.
Depending on your dog’s signs, there are a variety of diagnostics your vet might recommend. This is a time when you can lean on your veterinarian’s education and expertise. He or she will be there to guide you on how best to proceed with your furry family member.
The exact prognostic information will depend heavily upon the stage of disease and whether chemotherapy or other therapy is pursued. In general, the prognosis for multiple myeloma with treatment can be good. However, the other listed cancers do not carry such favorable prognoses.
#4: Blood loss caused by parasites or due to diseases transmitted by parasites
After all these heavy topics, it is time for a bit of a reprieve! While they might be somewhat creepy, parasites are a “good” cause of anemia in dogs. This is because blood loss caused by parasites is both easily treatable and easily preventable.

Parasites are any organism that lives on or in another organism. Some of the most common parasites in dogs include fleas, ticks, and intestinal parasites. We will cover each of these parasites in turn and how they might cause anemia.
Can fleas cause anemia in dogs? Yes!
Fleas are small insects that survive by feeding on the blood of the host animal. If a dog has a severe flea infestation, the fleas can suck so much blood that the dog becomes anemic. Young puppies and very small breed dogs are most susceptible to developing severe flea anemia. This is the case because they have a lower blood volume than more mature or larger dogs.
However, even a moderate flea infestation can cause anemia if it lasts long enough. It does this by depleting the body of its iron stores. Since iron is an important component of red blood cells, the end result is another form of anemia, iron deficiency anemia in dogs.
Flea anemia symptoms and treatment
Moderate to severe flea infestations are generally fairly easy to spot. If you take a look at your dog’s coat, you can see flea dirt (i.e. flea feces, which often look like coffee grounds) and the fleas themselves. Plus, you may notice your dog licking the base of the tail or itching all over. On top of that, your dog may have pale gums, be lethargic, or show other signs of anemia.
Severe flea anemia is a serious medical condition that requires prompt attention. Very young puppies and other dogs with severe anemia may need aggressive care and a blood transfusion. It is also vital to kill the fleas by administering a topical or oral flea preventative medication. Finally, dog parents must take steps to ensure the environment is appropriately decontaminated. This will hopefully prevent the flea infestation from reoccurring once the puppy is recovered and back home.
Preventing flea anemia in dogs
After hearing how dangerous flea anemia is, you will be relieved to know that it is easy to prevent. You just need to ensure your dog reliably receives a veterinarian-prescribed oral or topical flea preventive medication. The two key aspects in this are “veterinarian-prescribed” and “reliably.”
Unfortunately, most holistic and over-the-counter flea preventive medications don’t work well. So it is important to use a prescription product that your veterinarian recommends for your dog’s particular situation. Also, keep in mind that missing doses can lead to a flea outbreak. Therefore, it is a good idea to keep administering your flea preventive all year round, even in cold climates.
If your dog isn’t already on a veterinary-prescribed flea preventive, please talk to your vet about which medication might be best for your pup. That way you can cross this cause of anemia off your list of things to worry about.
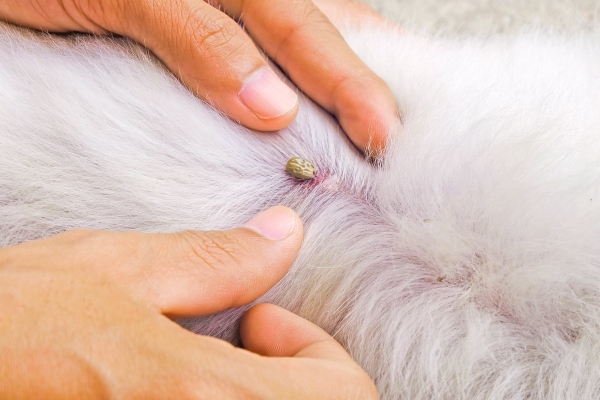
Can ticks cause anemia in dogs? Yes!
As it turns out, ticks can also cause anemia. However, they don’t do it the same way as fleas. Ticks tend to not suck enough blood to directly cause anemia. Instead, they spread several infectious diseases such as Babesiosis, Ehrlichiosis, and Anaplasmosis, which can cause a variety of different types of anemia.
The good news is that most tick-borne diseases in dogs that cause anemia can be treated readily with oral antibiotic. And the prognosis is good if caught early.
Similar to anemia caused by fleas, anemia from tick-borne diseases is preventable. It is important to keep your dog on a year-round veterinary-prescribed tick preventive. And to be extra safe, check him or her for ticks when you come inside, especially if you spent time in an area with tall grass or brush.
Can worms cause anemia in dogs? Yes!
You may be sensing a theme by now—worms can also cause anemia. There are a few common types of intestinal worms than can affect dogs: tapeworms, roundworms, whipworms, and hookworms.

But if worms are causing anemia, the culprit is almost always hookworms. These parasites live in the small intestines. And they are named after their hook-like mouth parts, which they use to attach to the small intestinal lining and feed on your dog’s blood.
Hookworms, though small, are mighty with regard to the amount of blood they can consume. Just as with flea anemia, young puppies are particularly susceptible to developing severe anemia from hookworms.
In addition to the typical signs of anemia, affected dogs may experience dark tarry stool, vomiting, or weight loss. Thankfully, your veterinarian can easily diagnose hookworms by finding the eggs on a fecal test for dogs.
If the dog with hookworms isn’t outwardly sick, the vet can prescribe a simple regimen of oral deworming medication. However, puppies or dogs with severe hookworm anemia may require aggressive treatment and blood transfusions in addition to deworming.
This is another scenario where an ounce of prevention is worth a pound of cure. Hookworms can be passed to puppies from their mothers. And puppies and older dogs can also acquire hookworms from a contaminated environment. Therefore, routinely deworming your dog according to your veterinarian’s instructions can go far in preventing anemia from hookworms. And it can help keep your dog free of other internal parasites too.
#5: Toxin exposure cause anemia in dogs
While we are on the topic of preventable types of anemia in dogs, it makes sense to also mention that anemia can occur due to toxin exposure. Educating yourself about toxins, including the ones below, can help you be more prepared to keep your pup safe.
Onions and garlic
Onions and garlic, while delicious in foods like soup and pasta, should be reserved only for human members of the household. In dogs, eating onions and garlic can cause a specific type of anemia known as Heinz-body anemia. These toxic foods, eaten in large enough quantities, cause oxidative damage and the subsequent build-up of abnormal “Heinz-bodies” inside red cells. Then the immune system destroys the damaged red cells, which leads to hemolytic anemia.
This toxicity is dose-dependent, meaning the more onions or garlic your pup consumes, the higher the risk of serious anemia. Overall, it is still safest to keep these foods away from dogs. But being dose-dependent does mean that if dogs accidentally get a bite or two of a dish that was seasoned with garlic or onions, they should be in the clear. However, if you are ever worried, call your veterinarian to find out if there is cause for concern.

Zinc
Zinc might help shorten the duration of your cold, but it isn’t any good for your dog. Interestingly, the most common cause of zinc toxicity in dogs is ingestion of objects made of zinc, specifically pennies made after 1982. However, vitamins and zinc lozenges, while typically low risk, can occasionally also cause problems.
Zinc toxicity often causes GI upset initially. Then several days later it may cause anemia and damage to other organs. If you suspect that your dog may have eaten something containing zinc (or really any foreign object), a prompt vet visit is in order. Severe zinc toxicity can be fatal if left untreated. But if it is caught early and treated appropriately, a good outcome is possible.
Acetaminophen
A common medicine cabinet staple in most households, acetaminophen is found in brand-name medications such as Tylenol®, Excedrin®, Goody’s®, NyQuil® and DayQuil®, Alka-Seltzer Plus®, and many more. In fact, more than 600 over-the-counter and prescription medications contain acetaminophen, according to the FDA.
While acetaminophen is a safe and effective pain-reliever in people, it can be toxic to dogs. It causes a multitude of issues that can develop within hours of ingestion. Specific risks can include liver damage, facial swelling, and red blood cell issues. Plus, acetaminophen can decrease the blood’s ability to carry vital oxygen, leading to chocolate-brown or bluish gums. It can also cause red blood cell destruction and anemia in dogs.
It is best to keep all acetaminophen-containing products locked safely away from pets to prevent these highly concerning complications. And if your canine companion does accidentally ingest acetaminophen, time is of the essence. Quick treatment can significantly improve the prognosis for this toxicity.
Anticoagulant rodenticide
There are several types of rat poison, each with a different mechanism of action. But all of them are dangerous for dogs and other household pets. One type of rat poison (i.e. rodenticide) works by causing fatal bleeding in its target pests. This type, known as anticoagulant rodenticide, exerts these same effects on dogs.

Dogs who have ingested anticoagulant rodenticide can’t clot their blood. This may cause severe bleeding, which is often internal, making it harder to notice. Signs you might observe include:
- Pale gums
- Weakness
- Difficulty breathing or a dog who is breathing fast
- A distended abdomen (i.e. the appearance of a pot-bellied dog)
- Bruising
- Neurologic signs like seizures in dogs
- Bloody nose (epistaxis)
- Blood in the stool, urine, or vomit
- Swollen and painful joints
As with most toxicities, the sooner you pursue treatment for your dog, the better chance of recovery. Without treatment, anticoagulant rodenticide toxicity can be fatal. However, if the dog is rapidly brought to a veterinarian and treated appropriately, it is possible that he or she may recover.
#6: Blood loss due to trauma or surgery
While we are on the topic of bleeding, it is also important to remember that any major injury that causes significant external or internal bleeding can lead to anemia in dogs. Cuts or injuries that affect large arteries or veins on the outside of the body, such as those from dog fights, may cause anemia due to rapid external blood loss.
Alternatively, blunt force trauma, like being hit by a car, can lead to internal bleeding, which can also cause severe and sudden anemia in dogs. And certain snake bites on dogs can also cause bleeding and anemia.
These types of injuries are accidental and not always preventable. However, you can do your best to guard against them by keeping your dog on a leash or inside a fenced-in area.
While planned surgery isn’t the same thing as an injury, anemia in dogs after surgery can occur during procedures where a dog loses significant amounts of blood. This happens more often after the major surgeries: dog leg amputation, removal of the spleen (i.e. splenectomy), or removal of part of the liver (i.e. liver lobectomy for liver cancer in dogs).
If your pup ends up in this situation, your veterinarian will monitor the red blood cell count closely after surgery. That way he or she can ensure your dog doesn’t need a blood transfusion. Happily, an otherwise healthy dog will almost immediately start to make new red blood cells to make up for those lost. Consequently, the red blood cell count should return to normal within one to two weeks.
#7: Gastrointestinal (GI) bleeding in dogs
Continuing on with the topic of bleeding, there is one more type of bleeding we need to discuss—GI bleeding. If the bleeding occurs higher in the intestinal tract, like in the stomach or small intestine, the digested blood turns the stool black. This dark, tarry stool is called melena. On the other hand, if the bleeding happens further down in the large intestine or rectum, then the blood either will be dark or bright red.
Regardless of the location, if the bleeding is severe or continues for long enough, your dog will become anemic. Aside from bleeding due to low platelets (i.e. thrombocytopenia), there are two main causes anemia in dogs from GI bleeding—GI ulcers and GI masses.
Stomach or intestinal ulcers
Ulcers are areas where the normal lining (i.e. mucosa) of the stomach or small intestines becomes damaged and worn away. This tends to happen when something goes wrong with the body’s natural protective mechanisms.
Normally, food is broken down by stomach acid. Then it is absorbed by the layer of tissue under the mucosa, which is full of many blood vessels. There are numerous safety mechanisms in place that keep the caustic stomach acid from damaging the normal, healthy mucosa lining the GI tract. However, when these mechanisms go awry, stomach acid can erode into the underlying blood vessels. This can cause anything from mild to severe bleeding.
Some possible predisposing factors or diseases that can increase the risk of stomach ulcers in dogs include:
- Non-steroidal anti-inflammatory drug (NSAID) administration
- Coadministration of NSAIDs and steroids
- Liver disease in dogs
- Kidney disease in dogs
- Inflammatory bowel disease (IBD in dogs)
- Addison’s disease in dogs (i.e. hypoadrenocorticism)
- Gastrointestinal foreign bodies
- Pancreatitis in dogs
- Mast cell tumors in dogs
- Gastrinomas (i.e. tumors of the acid-producing cells in the stomach)
- Spinal disease
- Sepsis
In addition to dark tarry stool, you may notice a decreased appetite, vomiting, or signs of abdominal pain if your dog has an ulcer. And if the ulcer causes significant enough bleeding, you will also see any combination of the normal signs of anemia.

Diagnosis and treatment of ulcers
The vet may be suspicious that your dog has an ulcer based on these symptoms. However, the definitive way to identify an ulcer is endoscopy. This scoping procedure, performed under general anesthesia, allows the vet to visualize the lining of the stomach and first part of the small intestine.
Additionally, the veterinarian may want to perform bloodwork. And if an obvious predisposing cause, like a history of being on NSAIDs, isn’t readily evident, he or she may also recommend an abdominal ultrasound to investigate further.
Treatment involves administering antacids (such as omeprazole for dogs) and stomach coating medications while trying to determine and address the underlying predisposing factor. Some dogs occasionally require blood transfusions. And rarely, dogs may need surgery to excise the ulcer and halt the bleeding. To help prevent recurrence of ulcers, the vet may recommend continuing antacid medications long term.
The prognosis, as for many things on this list, depends on whether the underlying cause is treatable. For example, the prognosis for ulcers from NSAID administration can be good if caught early. But the prognosis for ulcers secondary to severe liver or kidney disease is poor.
GI masses
Any abnormal growths or cancers affecting the gastrointestinal tract can also disrupt the protective mechanisms and lead to ulcers and/or GI bleeding. The two most common types of cancers of the GI tract are gastric lymphoma and gastric carcinoma. Both can cause anemia in dogs from GI bleeding in addition to a decreased appetite, vomiting, weight loss, and diarrhea. These cancers are typically treated with surgery and/or chemotherapy, and the prognosis for both is guarded.
Rectal polyps
There is one final, less nefarious cause of GI bleeding in dogs—rectal polyps. Rectal polyps are benign growths in the rectum that bleed easily. If rectal polyps are the cause of GI bleeding, the blood you would see is typically bright red. Thankfully, while it can look scary, most of the time there is not enough blood loss to lead to anemia.
The veterinarian can surgically remove rectal polyps, and the prognosis after surgical excision of benign rectal polyps is generally excellent.
#8: Bone marrow disease in dogs
Finally, let’s switch gears to talk about some causes of aplastic or non-regenerative anemia in dogs. We already briefly mentioned this type of anemia when discussing cancer, but as a reminder, non-regenerative anemia means that the body is not producing new immature red cells (i.e. reticulocytes). As a result, the anemia does not improve over time. This can occur for a variety of reasons, including problems with your dog’s bone marrow.
We normally think about bones as they relate to our furry family member’s ability to run, jump, and play. However, the spongy core at the center of your dog’s bones, the bone marrow, is a cell-making powerhouse. Most of your dog’s red and white blood cells and platelets are manufactured in the bone marrow.
Consequently, any disease or problem that affects the bone marrow can lead to decreased production of red cells and cause a non-regenerative anemia. Some common causes of bone marrow disease include:
- The administration of certain medications such as chemotherapy drugs (thankfully, this is a rare side effect)
- Cancers like leukemia and multiple myeloma
- Certain tick-borne infections in dogs that can set up shop in the bone marrow
- Immune-mediated disease that occurs at the level of the bone marrow
- Scarring of the bone marrow (i.e. myelofibrosis)
Ultimately, to determine which of these issues might be at play, your dog may need bone marrow testing in the form of a bone marrow aspirate or bone marrow biopsy.
Once your vet determines the underlying cause, he or she will go through the prognostic information. In general, the prognosis for immune-mediated and infectious causes listed above can be good to guarded. But the prognosis for the remainder of the causes is generally poor.
#9: Kidney disease
In addition to problems with the bone marrow itself, the dog may also become anemic because the bone marrow isn’t getting the signal to make more red blood cells. Such is the case in some dogs with severe or advanced kidney disease.

Normally, the kidneys make the hormone erythropoietin, which is what tells the bone marrow when it needs to make new red blood cells. However, since older dogs with moderate to severe chronic kidney failure in dogs have fewer functional kidney cells, they make less of this important hormone. The lack of erythropoietin can cause a non-regenerative anemia in dogs that can range from mild to severe.
Thankfully though, there is a synthetic form of erythropoietin that your vet can administer as a weekly injection until the anemia improves.
Overall, the prognosis for this type of anemia in dogs is related more to the degree of kidney disease than to the anemia itself. In other words, anemia generally occurs in the later stages of kidney disease in dogs. Therefore, these dogs may have a more guarded prognosis because of the severity of their kidney failure.
If your dog is struggling with kidney disease (with or without anemia), it is important to note that there are options to help him or her feel better. I encourage you to work closely with your veterinarian to find the right treatment regimen that will maximize your dog’s quality of life until it becomes time to euthanize your dog with kidney failure.
#10: Chronic disease can cause a mild non-regenerative anemia in dogs
This last cause of anemia in dogs is a bit of a catch-all, as any significant chronic disease can cause a mild non-regenerative anemia. In fact, this broad category, “anemia of chronic disease,” is actually the most common cause of anemia in dogs.
You see, making new red blood cells requires energy, and sometimes a dog’s body has bigger fish to fry. There are situations where some of the energy that would have gone into making new red blood cells is instead put toward dealing with whatever illness is at hand. As a result, the dog becomes mildly anemic.
Some examples of chronic diseases that might cause this type of anemia in dogs include:
- Cancers not listed above
- Chronic inflammation
- Chronic infections
- Liver disease
- Hypothyroidism in dogs
- Cushing’s disease in dogs (i.e. hyperadrenocorticism)
- Addison’s disease in dogs (i.e. hypoadrenocorticism)
It is important to note that this kind of anemia won’t ever be severe. So if an older dog has severe anemia, the vet will be looking elsewhere for the cause of the anemia.
In the case of anemia of chronic disease, the focus should be on diagnosing and addressing the primary chronic disease. Then the body can once again devote the appropriate energy toward resolving the anemia.
Miscellaneous causes of anemia in dogs
In addition to the “Top 10” list, there are a few other less common causes of anemia in dogs that still bear mentioning. They include:
- Infectious diseases including distemper or parvo
- Severe nutritional deficiencies (i.e. poor nutrition)
- Bleeding from the urogenital tract
- Heartworm disease in dogs
- Disseminated intravascular coagulation (DIC)
- Inherited disorders that affect red blood cell shape or function
- Diabetic ketoacidosis (DKA in dogs)
The benefit of understanding the causes of anemia in dogs
Whew! That was quite the journey, huh? If you made it through all 10 causes of anemia in dogs, then you and your pup likely got in some high-quality cuddle time. And this virtual “trip” around the body—from the immune system to the spleen, GI tract, bone marrow, kidneys, and liver—probably gave you a greater appreciation of the many possible causes of anemia.
Hopefully, you and your canine companion never have to put this newfound knowledge to use. But if you do find yourself dealing with a diagnosis of anemia, I hope you can feel confident that you have the background information you need to advocate for your furry family member. And even better yet, you have a knowledgeable co-pilot with superb navigation skills—your veterinarian. Together, you can tackle whatever life throws at your dog.
What was the cause of your dog’s anemia?
Please share his or her story in the comments.


My healthy 9 year old has just come back from the vet after undergoing a several tests and X-rays. He has lost about 10% of his body weight in the last few weeks and has been a bit off his food. The vet tested urine, which was fine and bloods. He is severely anemic (RBC is 17).. He has given him a 14 day course of antibiotics to kill any possible parasites. The vet is running more blood tests, results and will only be available tomorrow. After reading your very informative article, I am absolutely terrified!
Hi Christy,
I am sorry you are going through this scary situation with your pup. I am glad your vet is being very proactive and continuing to investigate and run tests. How are things today? Have you been able to get any answers? Don’t forget you can ask for a referral to talk with a specialist if needed. Praying for healing and a clear path forward. Feel free to leave an update if you have a chance.
Jack started symptoms of limping (back left leg) a week or so before he started breathing faster. On a Friday I first googled “why is my dog breathing faster?” But I wasn’t yet alarmed. I had noticed that say day he needed to gain some weight (he has always been lean). Since it’s very hot out and also because of the pain of the lamp, I thought the breathing might be related. On Sunday night I became more concerned since he was now sleeping more and breathing was faster. I got him into a vet appointment Tuesday. She did an ultrasound, and did not find any masses but his regenerative anemia was very severe.
He died on Thursday (7/20/23). He was 3 weeks shy of his 14th birthday. When he died he collapsed (heart attack?) while trying to lift his leg to pee on the puppy pad. He fell once and got back up. I went over to help him and he fell again and then while I was supporting him he peed and collapsed doing so.
I laid him down and saw he wasn’t breathing and then he started agonal breathing at which point blood and a watery fluid was coming from his throat. For hours after death he bled that fluid blood from his nose and mouth.
In all these years, I had never seen him sick before. Even the day before he was able to jump up and down from the couch and the bed. He was on steroids and pain medication and I thought he was coming through. I read that only certain conditions have leading at the mouth, but I can’t understand how it relates to the lamp either. Any ideas or things that I can rule out? I have another dog at home (his littermate).
Hi Angela,
I’m so sorry for the loss of your dog. Watching him decline and then die suddenly would be beyond scary and heartbreaking, and I understand your concern for your other dog. Unfortunately, without a necropsy, it is very hard to know for sure how the limp, regenerative anemia, bloody fluid, and sudden death are all connected (or if they even are). I’m sorry that I can’t offer you a more definitive answer to ease your mind a bit. Thinking about you as you process his sudden loss. ❤️
We almost lost our 11 year old yellow lab to IMHA August 2021. My husband was suppose to take our dog to our cabin for his annual boys weekend, but my gut said otherwise. For about a week prior I had noticed a change in Becker’s behavior. We had gone away with another family and he was unusually intolerant of their little boxer puppy who was wanting to play with Becker. (He’s usually SO PATIENT with puppies) That combined with a big change in his energy level made me feel like something wasn’t right. He normally walks with me to take my kids to school and this particular day he was walking so slow that he almost wasn’t moving. That night I noticed he was standing, just staring outside and I got a flash of his gums, they were almost white. My stomach dropped because I remember reading somewhere that white gums are a dangerous sign and he should be rushed to a vet. That’s where his brush with death started. They admitted him immediately into the emergency vet where the vet told me he most likely won’t make it through the night. I was gutted. How could this be happening over night. To make a VERY long story short, Becker is a fighter and I just happened to check him into one of the best vets in the Chicagoland area. (I had no idea). He proceeded to be on an iv, given high doses of med and was on the brink of needing a blood transfusion at any moment. After deciding that we’d take any measures to save him (meaning a VERY PRICEY blood transfusion) he ended up pulling through after 5 nights in the hospital. Although he never ended up needing the transfusion (the Vet said it’s worst case scenario and if his blood cell count dropped another mark or two, it would happen, he avoided it) each day was touch and go. To say he was weak would be an understatement. He dropped over 15 pounds in those few days and getting him to eat was so hard. But our Becker made it! After joking that my kids won’t go to college because of the cost (j/k…but it was over $7,000, not including the meds for the following months that were close to $500 a month) we have now had Becker for over a year after the incident and he’s still with us today at 12.5 years old). Before his bout with IMHA he would walk 2 miles a day and never showed obvious signs of aging. IMHA took a toll on him. His back legs don’t like to work like they used to, but his spirit is still that of a young dog. His walks now are about a block long, but the highlight of his day. I said at the time, “if I get 6 months more with becker then it would all be worth it.” at over a year later I feel blessed. The vet never could figure out what caused his IMHA. At first they thought it was cancer, or tumor, but nothing was found. He was on HEAVTY and very expensive meds for about 6 months, but now is off them all. The vet doesn’t want to risk any immunizations that may trigger it again, so he gets his senior panels and regular visits to check his condition. He keeps passing with flying colors! We’ve been so fortunate to have a very healthy 115 lb yellow lab this long. This has been his ONLY medical issue his whole life. It was beyond scary and I know our days with Becker are numbered so we spoil him with love and savor each moment with him.
Thank you Dr Buzby for this article.
Hi Emily,
Thank you so much for sharing your experience with our readers. What a blessing to still have Becker in your life and that he is able to find joy each day! I am glad you are making the most of this extra time you have been gifted. Hoping you have many more happy days ahead to continue making memories. Bless you and give your big guy a hug for me! ♥
Is the first symptom of anemia that a dog becomes tired early and frequently drops breath due to a faster heart rate?
Hi Sarwar,
Each dog is different, and they may not all show the same symptoms. But generally, yes lethargy and increased respiratory effort can be signs of anemia.
Thanks Julie
My dad’s 5 year old Pekingese had diarhee and by day 2 dad took her to n the vet who out her on a drip. her gums were white and stools yellow. Blood tests indicated low redblood count. After a day she deteriorated so badly that the vet called my dad and said something must have happened because she’s not going to make it. She was really struggling to breath.
Dad did what he thought was best and they put her to sleep. He asked permission to do an autopsy which came back a bloodclot thru the heart. We still have many questions. she was a healthy playful little dog. the only thing she suffered with was she scratched all the time, something seem to work and the vet did give her some injection which only brought her relief for a few weeks then it was back.
Dear Estelle,
I am sorry your dad had to say goodbye to his young pup. I understand how hard it can be when we are left with more questions than answers. Take comfort in knowing he made a loving decision to offer his girl peace and freedom from her suffering. May her memory stay with you both and be a source of joy in your lives. Bless you. ♥